Conditions Clotting (coagulation) disorders
ICD codes: D68 D69 What are ICD codes?
Clotting disorders have many causes and can lead to both bleeding and blood clots (thromboses). Some disorders are harmless, but others require special treatment. In some cases, treatment can even require the use of blood products.
At a glance
- Clotting (coagulation) disorders cause the blood to clot (coagulate) abnormally. This can result in increased bleeding, but also blood clots (thromboses).
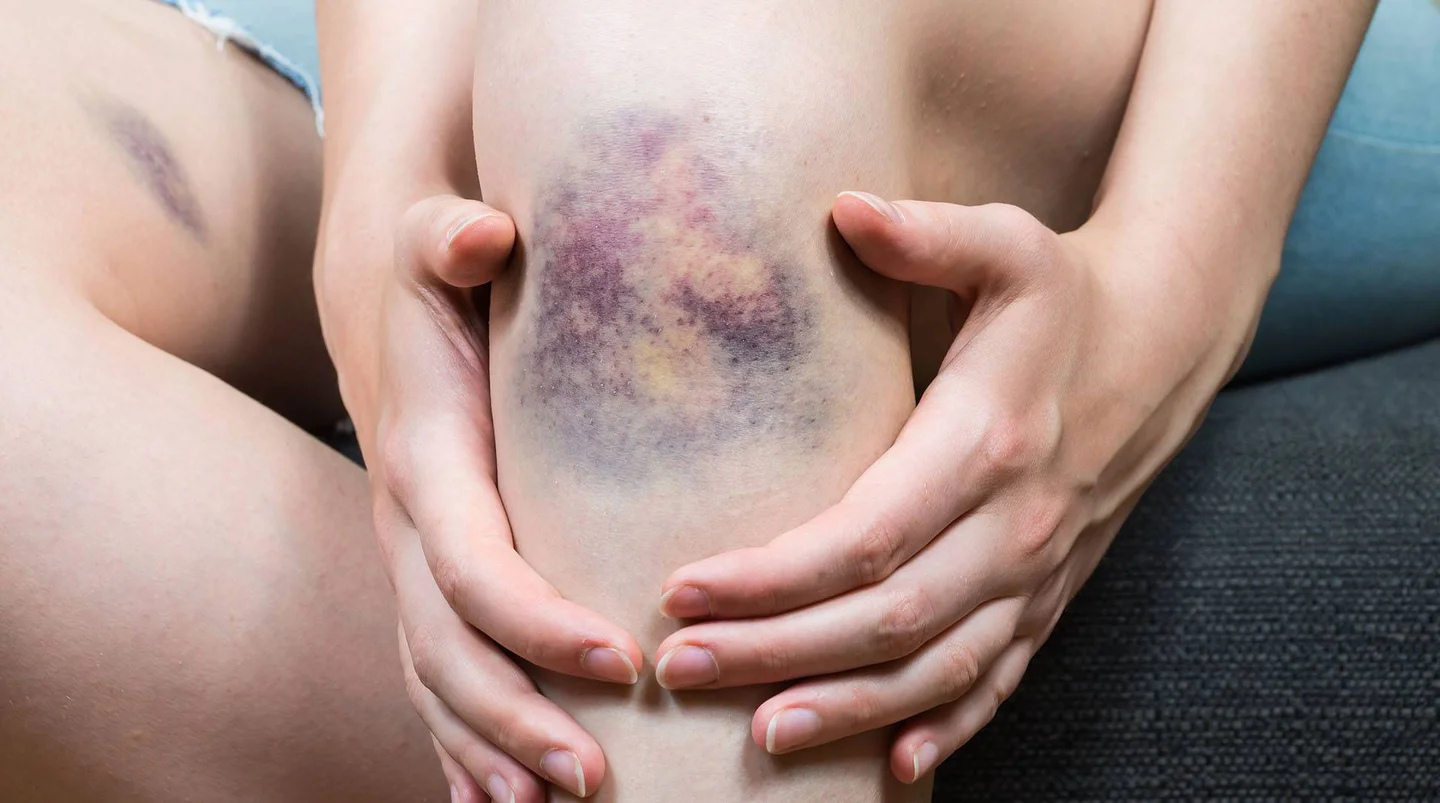
- Typical signs of a tendency to bleed include frequent nose bleeds, bruises or extremely heavy periods.
- If the blood clots more easily, this is often indicated by thromboses in the legs.
- Clotting disorders can be congenital or only develop over the course of a person’s life for various reasons.
- Mild cases do not usually require any special treatment. More severe disorders can generally be treated with medication or blood products.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What are clotting disorders?
With clotting disorders, the blood in the body does not clot properly. There are essentially two types of disorder: on the one hand, blood clotting can be delayed, causing a tendency to bleed. In such cases, seemingly unexplained bleeding occurs in the skin or mucous membranes, unusually large bruises appear or women can have particularly heavy periods (menstrual bleeding), for example.
On the other hand, some clotting disorders result in blood clots (thromboses) forming more easily and quickly (tendency to thrombosis).
Clotting disorders have multiple causes. Some are congenital, such as bleeder’s disease (hemophilia), where certain clotting factors in the blood are missing. In the case of newborns, clotting disorders are usually due to a vitamin K deficiency. In addition, medication, immune reactions and various health conditions, such as liver damage, can impair blood clotting.
Mild clotting disorders have little effect on people’s everyday lives and do not require any special treatment. In the event of more pronounced symptoms, a tendency to bleed or increased risk of thrombosis can often be controlled through the use of medication. Severe clotting disorders, on the other hand, can require hospital treatment and the use of blood products.
What are the symptoms of clotting disorders?
Clotting disorders can have multiple symptoms, including frequent or prolonged bleeding.
The typical symptoms include:
- unexplained nose bleeds that are hard to stop
- frequent mucous membrane bleeding, for example on the palate
- bruises that occur after only slight knocks
- pin-sized spots of bleeding (petechias), for example on the lower legs and ankles
- skin wounds that bleed for an excessively long time
- secondary bleeding as a result of minor surgery such as extracting a tooth
- heavy, persistent menstrual bleeding
- bruises in muscles or joints without prior injury
Some clotting disorders lead to increased blood clotting rather than decreased. These result in more frequent blood clots, a condition known in medical terms as “thrombophilia”. Such disorders are often indicated by venous thrombosis in the legs and are typically accompanied by lower leg pain and tightness.
What causes clotting disorders?
When the blood clots, several clotting factors interact with the platelets (thrombocytes) and the blood vessels’ wall cells.
The body’s finely tuned clotting system is required to not only keep the blood fluid and enable it to flow well, but also to quickly form blood clots in the event of injuries and prevent major blood losses.
In the event of clotting disorders, this balance is impaired. There are multiple causes for this:
- congenital influences
- taking certain medication
- immune reactions
- existence of other health conditions
- vitamin K deficiency
Congenital influences
Some clotting disorders are genetically determined. For example, the level of certain clotting factors required for normal blood clotting can be lower than usual.
There are also congenital clotting disorders where the blood clots more than usual, resulting in a higher risk of blood clots (thrombosis).
Medication
Blood-thinning drugs such as heparin or phenprocoumon inhibit the effect of various clotting factors or block their formation in the liver. The risk of bleeding thus increases.
Non-prescription painkillers containing the active ingredient acetylsalicylic acid (ASA) can also result in a tendency to bleed as they impair the normal function of platelets (thrombocytes).
Various other forms of medication also affect blood clotting. Many hormonal contraceptives are known to increase clotting and the risk of thrombosis.
Immune reactions
The immune system sometimes produces autoantibodies that damage thrombocytes or block their formation, for example. This reduces the number of thrombocytes and results in a tendency to bleed (referred to in medical terms as immune thrombocytopenia). The reason for the development of such autoantibodies is often unclear.
Other health conditions
Various clotting factors are formed in the liver. Chronic liver damage can therefore result in a tendency to bleed, for example. Likewise, various other health conditions such as kidney disease or cancer are frequently associated with increased bleeding and sometimes with an increased risk of thromboses.
Vitamin K deficiency
Vitamin K is important for the formation of several clotting factors in the liver. As newborns are only able to store small amounts of this vitamin, they can sometimes be at a far greater risk of bleeding. Babies are therefore preventively given vitamin K at birth (vitamin K prophylaxis). In adults, on the other hand, it is rare for a vitamin K deficiency to cause heavier bleeding.
How are clotting disorders diagnosed?
To diagnose a clotting disorder, doctors will start by asking patients about their medical history and the typical symptoms. This makes it possible to determine if the patient has a clotting disorder and, if so, its severity.
A blood sample is also required for an accurate diagnosis. Several laboratory tests are performed to see how long the blood takes to clot. The number and shape of the platelets (thrombocytes) are also checked.
Depending on the results, further laboratory tests may be needed, for example to determine the concentration of individual clotting factors or how well the thrombocytes are functioning. In some cases, genetic analyses are also revealing.
The further diagnosis is often carried out by hematology specialists, i.e. specialists in disorders of the blood and blood-forming organs. However, it is not always possible to definitively determine the cause of clotting disorders.
How are clotting disorders treated?
Some clotting disorders are very mild and have little effect on people’s everyday life. They do not need any special treatment. It generally suffices to avoid certain medications that impair or promote blood clotting.
If, on the other hand, clotting disorders result in more severe symptoms, various types of medication are used.
Treatment can include:
- administering the active substance tranexamic acid: this can stop or prevent bleeding in the case of various clotting disorders.
- injecting missing clotting factors: for example in the case of congenital bleeder’s disease (hemophilia).
- vitamin K: newborns are routinely given the vitamin at birth. Vitamin K products can also sometimes be useful for adults.
- blood-thinning medication and anti-thrombosis stockings (compression stockings): these are used for clotting disorders with a tendency to thrombosis in order to prevent deep vein thrombosis.
The risks and benefits of each form of medication should be carefully considered on a case-by-case basis. For example, it often suffices to temporarily treat a clotting disorder in relation to an impending operation or dental treatment.
In the case of prolonged or complicated bleeding, hospital treatment with blood products or platelet concentrates may be necessary.
- Doherty TM, Kelley A. Bleeding Disorders. [Updated 2021 Aug 12]. In: StatPearls (Internet). Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Aufgerufen am 10.01.2022.
- Eden RE, Coviello JM. Vitamin K Deficiency. [Updated 2021 July 26]. In: StatPearls (Internet). Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Aufgerufen am 10.01.2022.
- Kruse-Jarres R, Singleton TC, Leissinger CA. Identification and basic management of bleeding disorders in adults. J Am Board Fam Med 2014;27:549 –564. doi: 10.3122/jabfm.2014.04.130227.
- Rodeghiero F, Pabinger I, Ragni M, et al. Fundamentals for a Systematic Approach to Mild and Moderate Inherited Bleeding Disorders: An EHA Consensus Report. HemaSphere, 2019;3:5. doi: 10.1097/HS9.0000000000000286.
- Senst B, Tadi P, Goyal A, Jan A. Hypercoagulability. [Updated 2021 Sep 29]. In: StatPearls (Internet). Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Aufgerufen am 10.01.2022.
- UpToDate. Approach to the adult with a suspected bleeding disorder. Wolters Kluwer 2021. Aufgerufen am 10.01.2022
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at:


