Conditions Gestational diabetes
ICD codes: O24 What are ICD codes?
Gestational diabetes, i.e. diabetes during pregnancy, increases the risk of certain rare birth complications. However, this risk can usually be reduced by a change in diet. In most cases, the pregnancy is otherwise normal.
At a glance
- Women with gestational diabetes have a higher risk of rare birth complications.
- However, this risk can usually be reduced by a change in diet.
- A slightly elevated blood glucose level can easily become gestational diabetes.
- The vast majority of women with gestational diabetes have a normal pregnancy and give birth to a healthy baby.
- Having gestational diabetes is not the same as having diabetes mellitus, which is a chronic disease.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is gestational diabetes?
In most women, blood glucose levels remain normal during pregnancy. However, if the blood glucose level exceeds a certain limit, doctors call this gestational diabetes. Around 5 in every 100 pregnant women have gestational diabetes.
A slightly elevated blood glucose level can easily become gestational diabetes. This is because the metabolism changes during pregnancy.
After eating, sugar is absorbed more slowly from the blood into the body’s cells. Therefore, elevated blood glucose levels are not uncommon in many pregnant women. After the birth, these levels usually return to normal. Having gestational diabetes is not the same as having diabetes mellitus, which is a chronic disease.
Gestational diabetes slightly increases the risk of certain rare birth complications. However, if those affected change their diet, this risk can usually be reduced.
The vast majority of women with gestational diabetes have a normal pregnancy and give birth to a healthy baby.
What symptoms can occur with gestational diabetes?
In most cases, gestational diabetes does not cause any symptoms. However, if the blood glucose level rises very sharply, symptoms such as fatigue, weakness, or an increased feeling of thirst may occur, similar to other types of diabetes. Usually, the symptoms are rather mild and are often interpreted as common pregnancy symptoms.
What causes gestational diabetes?
A woman’s metabolism changes under the influence of pregnancy hormones. Body cells absorb the sugar dissolved in the blood from food more slowly. As a result, the blood sugar level increases. If certain values are consistently exceeded, this is referred to as gestational diabetes.
What increases the risk of gestational diabetes?
Elevated blood glucose levels are more common in women who:
- are severely overweight
- have had gestational diabetes before
- have close relatives with diabetes
The risk of gestational diabetes is also higher for pregnant women of a more advanced age.
What is the outlook for gestational diabetes?
Gestational diabetes usually has no consequences for the mother or child. On average, the children of women with gestational diabetes are somewhat heavier at birth. However, women with gestational diabetes should not become concerned by this fact alone.
When larger children are born, there is more often a delay after the baby’s head is delivered. If the child’s shoulder gets stuck in the mother’s pelvis (known as shoulder dystocia), there is a risk that the child will not get enough oxygen. As a precaution, midwives or doctors will take quick countermeasures if this happens.
Shoulder dystocia occurs in about 4 out of 100 children whose mothers do not treat their gestational diabetes. However, more severe injuries and emergency situations are rare.
Women with gestational diabetes are also at a higher risk of developing a condition known as pre-eclampsia. In this rare pregnancy condition, increased protein is excreted into the urine and blood pressure rises. Pre-eclampsia also leads to water retention in the body. If pre-eclampsia is not treated, it can harm both mother and child.
Women who have had gestational diabetes are more likely to develop type 2 diabetes mellitus later in life.
How can gestational diabetes be prevented?
Pregnant women who eat a diet high in carbohydrates or are overweight are more likely to have gestational diabetes than expectant mothers who exercise regularly and eat a balanced diet. However, since the metabolism of every pregnant woman changes, blood glucose levels can, in principle, become elevated in any expectant mother.
How is gestational diabetes diagnosed?
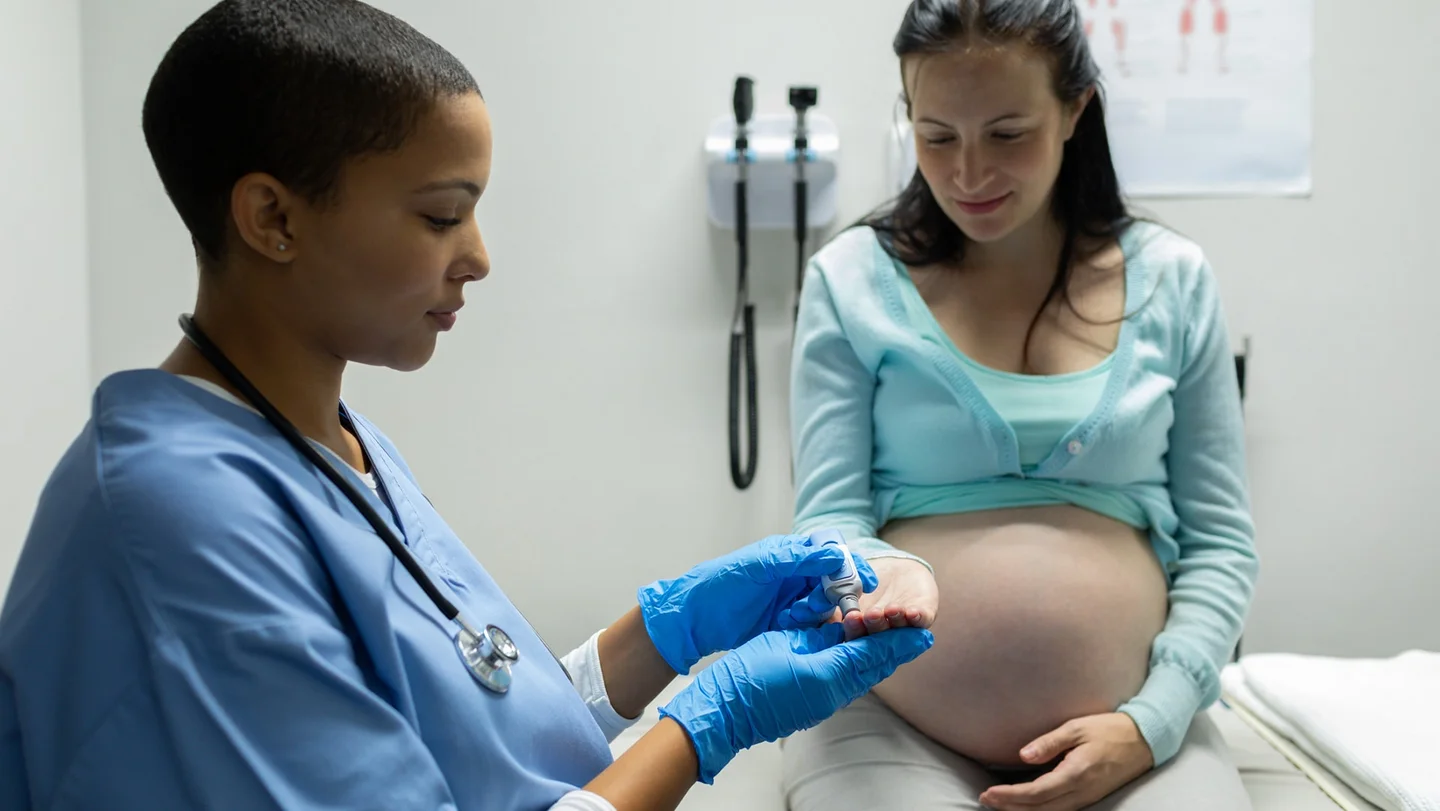
Gestational diabetes is best detected with a sugar test (glucose tolerance test). It looks at how the body reacts to a large amount of glucose. The test is offered to women in the 24th to 27th week of pregnancy. It consists of a screening test (glucose challenge test) and a diagnostic test.


In the screening test, the woman drinks a glass of sugar water. Blood is then taken from a vein in the arm and the blood glucose level is determined. If the value is elevated, a second test is performed. This test is similar, but a little more complex. For example, it requires the woman to have fasted beforehand.
For more detailed information, for example on how gestational diabetes is diagnosed, visit gesundheitsinformation.de.
How is gestational diabetes treated?
The elevated blood glucose levels associated with gestational diabetes can usually be reduced sufficiently by a change in diet. Those affected can seek advice from their doctor. In addition, special nutritional advice and exercise may also be beneficial.
For some pregnant women, blood glucose levels are consistently so high that they need to inject insulin or, in exceptional cases, take diabetes medication.
Once the baby is born, the doctor offers the mother another blood glucose test. If it indicates that the values are normal again, no further treatment is necessary. All women with gestational diabetes should obtain medical advice following the birth as to whether further examinations or a change of lifestyle are advisable.
What else should women know about gestational diabetes?
Gestational diabetes does not usually cause any symptoms. For those affected, the diagnosis is therefore often unexpected. Many women with gestational diabetes then wonder whether their child will develop healthily and are afraid of birth complications. Some also fear that the diabetes could continue after birth. Such fears can be stressful for expectant mothers. They should therefore note that the majority of children are born healthy despite gestational diabetes.
For some affected, changes that are part of the treatment may take some time to get used to. However, after a short time, a more balanced diet and more exercise can become part of everyday life. In addition, these changes also help the mother to stay healthy after the birth of the child.
- Bennett CJ, Walker RE, Blumfield ML et al. Interventions designed to reduce excessive gestational weight gain can reduce the incidence of gestational diabetes mellitus: A systematic review and meta-analysis of randomised controlled trials. Diabetes Res Clin Pract 2018; 141: 69-79. Aufgerufen am 17.10.2024.
- Craig L, Sims R, Glasziou P, Thomas R. Women's experiences of a diagnosis of gestational diabetes mellitus: a systematic review. BMC Pregnancy Childbirth 2020; 20(1): 76. Aufgerufen am 17.10.2024.
- Deutsche Diabetes Gesellschaft (DDG), Deutsche Gesellschaft für Gynäkologie und Geburtshilfe (DGGG). Gestationsdiabetes mellitus (GDM): Diagnostik, Therapie und Nachsorge (S3-Leitlinie, in Überarbeitung). AWMF-Registernr.: 057-008. 2018. Aufgerufen am 17.10.2024.
- Farrar D, Simmonds M, Bryant M et al. Treatments for gestational diabetes: a systematic review and meta-analysis. BMJ Open 2017; 7(6): e015557. Aufgerufen am 17.10.2024.
- Gemeinsamer Bundesausschuss (G‑BA). Richtlinien über die ärztliche Betreuung während der Schwangerschaft und nach der Entbindung. 2023. Aufgerufen am 17.10.2024.
- Guo XY, Shu J, Fu XH et al. Improving the effectiveness of lifestyle interventions for gestational diabetes prevention: a meta-analysis and meta-regression. BJOG 2019; 126(3): 311-320. Aufgerufen am 17.10.2024.
- Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen (IQWiG). Screening auf Gestationsdiabetes: Abschlussbericht; Auftrag S07-01; 2009. Aufgerufen am 17.10.2024.
- Rayanagoudar G, Hashi AA, Zamora J, Khan KS, Hitman GA, Thangaratinam S. Quantification of the type 2 diabetes risk in women with gestational diabetes: a systematic review and meta-analysis of 95,750 women. Diabetologia 2016; 59(7): 1403-1411. Aufgerufen am 17.10.2024.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at:


