Conditions Polycystic ovarian syndrome
ICD codes: E28.2 What are ICD codes?
Polycystic ovarian syndrome (PCOS) is a hormone disorder that mainly occurs in women of child-bearing age. Read on to find out how PCOS is recognized, how it progresses, which factors favor it, and how it can be treated.
At a glance
- Polycystic ovarian syndrome (PCOS) can affect the function of the ovaries.
- Indications of PCOS are irregular or missed menstrual periods, and male hair growth (hirsutism).
- There are also small blisters resembling cysts on the ovaries.
- PCOS can be treated by a change in lifestyle and with medication.
- Pregnancy is also possible after treatment.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is polycystic ovarian syndrome?
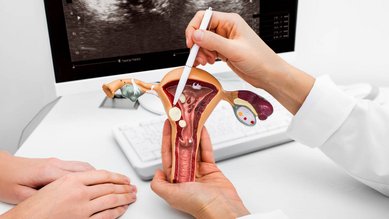
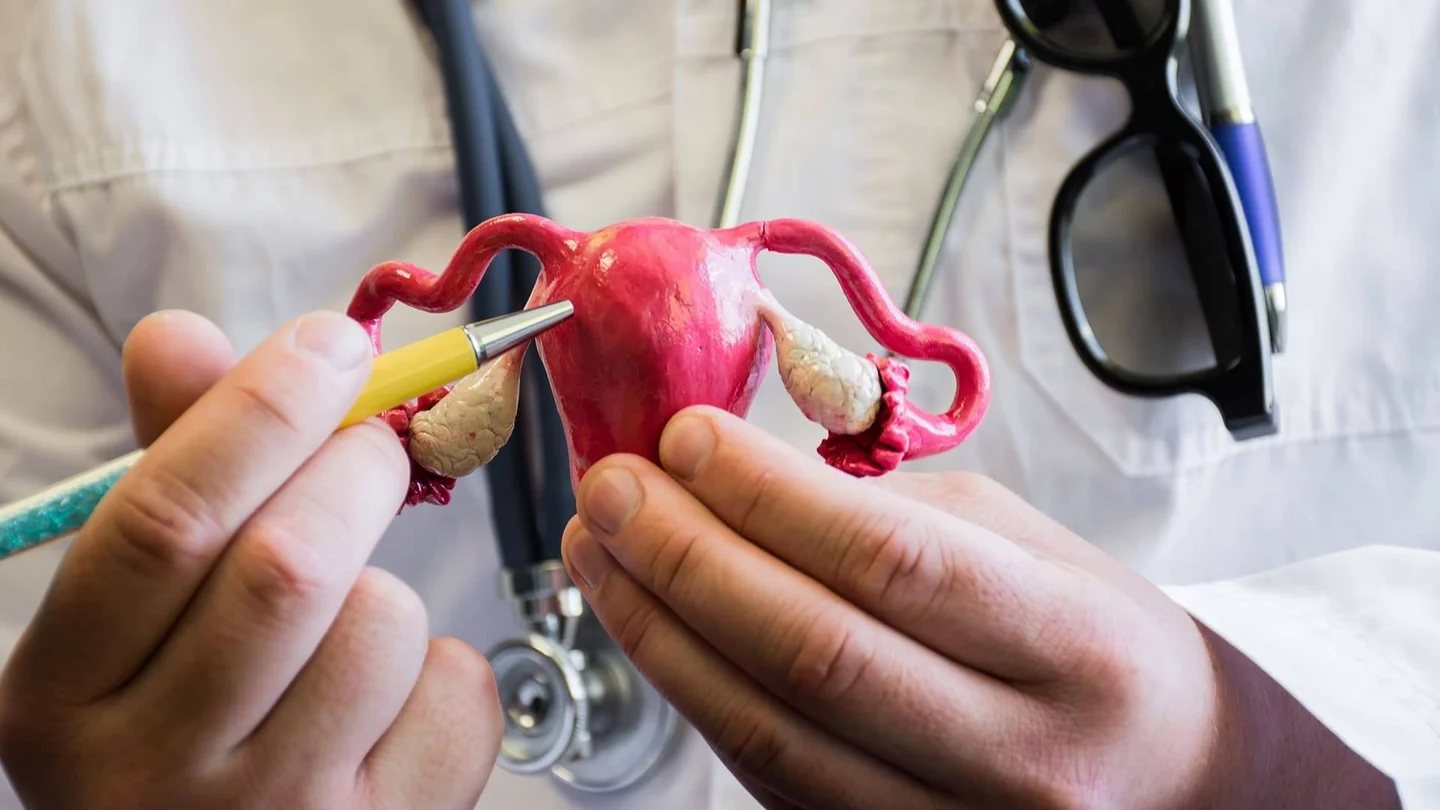
Polycystic ovarian syndrome (PCOS) – formerly known as Stein-Leventhal syndrome – is a woman’s hormone disorder and often causes the function of the ovaries to partly or completely fail.
The egg cells mature for reproduction in the ovaries. They also produce the female sexual hormones progesterone and estrogen. With PCOS, however, a woman’s ovaries produce too many male sexual hormones such as testosterone. This results in a hormonal imbalance which can cause infertility. Small, cyst-like blisters also form on the ovaries.
What are the symptoms of polycystic ovarian syndrome?
Women with polycystic ovarian syndrome (PCOS) have more male sexual hormones and often only get their menstrual period irregularly. Some women miss ovulation and their period entirely.
A woman with PCOS might find that her body hair changes and becomes more like that of a man: a lot of thick hair grows on the upper lip, chin, back, and pubic area. Doctors call this hirsutism.
Other indications of PCOS include:
Occasionally, also the hair on the head may fall out, the voice may become deeper, and the clitoris may get larger. These symptoms can occur on their own or in combination, but sometimes not at all.
What causes polycystic ovarian syndrome?
The causes of polycystic ovarian syndrome (PCOS) are not yet understood. It is thought that the tendency to PCOS is at least partly inherited because it occurs more frequently in some families.
Which factors favor polycystic ovarian syndrome?
Between 50 and 80 percent of all women with polycystic ovarian syndrome (PCOS) are overweight. Many also show a resistance to insulin: their body reacts less sensitively to insulin. The body can then not control the blood sugar level very well, and a so-called diabetic metabolic state develops. This further increases the production of male sexual hormones, which intensify the PCOS symptoms.
How common is polycystic ovarian syndrome?
Worldwide, polycystic ovarian syndrome occurs in around 8 to 13 percent of all women of childbearing age. The PCOS remains undetected in up to 70 percent of women.
Which are the consequences of polycystic ovarian syndrome?
Polycystic ovarian syndrome (PCOS) and a resulting malfunction of the ovaries can cause both physical and mental symptoms. Women with PCOS can struggle with their physical changes, and depression, anxiety and eating disorders may occur.
As the syndrome progresses, women may find it more difficult to get pregnant. They are at an increased risk of cardiovascular diseases and type 2 diabetes, and they may have problems during pregnancy.
How is polycystic ovarian syndrome diagnosed?
Polycystic ovarian syndrome (PCOS) is identified by:
- malfunctions of the ovaries (ovarian insufficiency): long-term irregular or missed periods
- an increased concentration of male sexual hormone in the blood, and increased male hair growth (hirsutism)
- cyst-like blisters on the ovaries
A high concentration of certain hormones can be identified in the blood. Doctors can identify polycystic ovaries – i.e. the hollows or blisters on the ovaries – using ultrasound.
How is polycystic ovarian syndrome treated?
Polycystic ovarian syndrome (PCOS) cannot be linked to a single cause. So doctors treat the individual symptoms. These can be alleviated or eliminated.
Women with PCOS can do certain things themselves: they can lose weight if they are overweight. Exercise and changes to their diet can also help to alleviate the symptoms and to restore a regular cycle. With some women, just a slight change in the Body Mass Index (BMI) is enough to improve the symptoms.
Other PCOS treatment varies according to whether the woman wishes to get pregnant or not.
Women not trying for a baby
Women with PCOS who do not want to get pregnant are prescribed contraceptives such as the pill by doctors. This enables their cycle to be stabilized. The pill also reduces production of male hormone so that hair growth can be reversed.
Women who are not getting any menstrual periods are at increased risk of endometrial cancer. The contraceptive pill can reduce this risk because it stabilizes the cycle. Alternatively, for instance if the woman does not tolerate the pill, doctors prescribe metformin: a drug that reduces insulin resistance, decreases the blood sugar level, and reduces male hormones.
Women trying for a baby
Women with PCOS who want to get pregnant are given drugs that promote ovulation. This makes pregnancy possible. Overweight women who lose weight before taking the drugs increase the probability that they will get pregnant.
Where can I find support in everyday life?
Self-help groups offer people with polycystic ovarian syndrome (PCOS) and their loved ones the opportunity to get information and advice, and to share personal experiences.
You can find suitable self-help via a database on the National Contact and Information Point For Encouraging and Supporting Self-Help Groups (NAKOS) website.
- DynaMed (Internet), Ipswich (MA). Evaluation of Polycystic Ovary Syndrome (PCOS). EBSCO Information Services. Record No. T917041. 2018 (1995). Aufgerufen am 28.05.2021.
- Monash University on behalf of the NHMRC, Centre for Research Excellence in PCOS and the Australian PCOS Alliance. International evidence-based guideline for the assessment and management of polycystic ovary syndrome. 02.2018.
- UpToDate (Internet). Evaluation of female infertility. Wolters Kluwer 2021. Aufgerufen am 28.05.2021.
- UpToDate (Internet). Treatment of polycystic ovary syndrome in adults. Wolters Kluwer 2020. Aufgerufen am 28.05.2021.
- Weyerstahl T, Stauber M. Duale Reihe Gynäkologie und Geburtshilfe. Thieme: Stuttgart 2013.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at: