Conditions Polyneuropathy
ICD codes: G62 What are ICD codes?
Nerves located outside of the spinal cord and brain are known as peripheral nerves. If several of these nerves are damaged, a person may experience pain and prickling sensations known as paresthesia. Doctors refer to this condition as polyneuropathy.
At a glance
- The peripheral nervous system comprises all nerves located outside of the brain and spinal cord.
- These nerves are important for perceiving stimuli, moving muscles and controlling organs.
- The term “polyneuropathy” is used if damage occurs to several of these nerves, causing symptoms to occur.
- There are many different causes. Diseases such as diabetes are often a trigger.
- Typical symptoms include pain and prickling sensations (paresthesia). An unsteady gait or muscle weakness are other possible signs.
- Pain therapy can help relieve symptoms.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
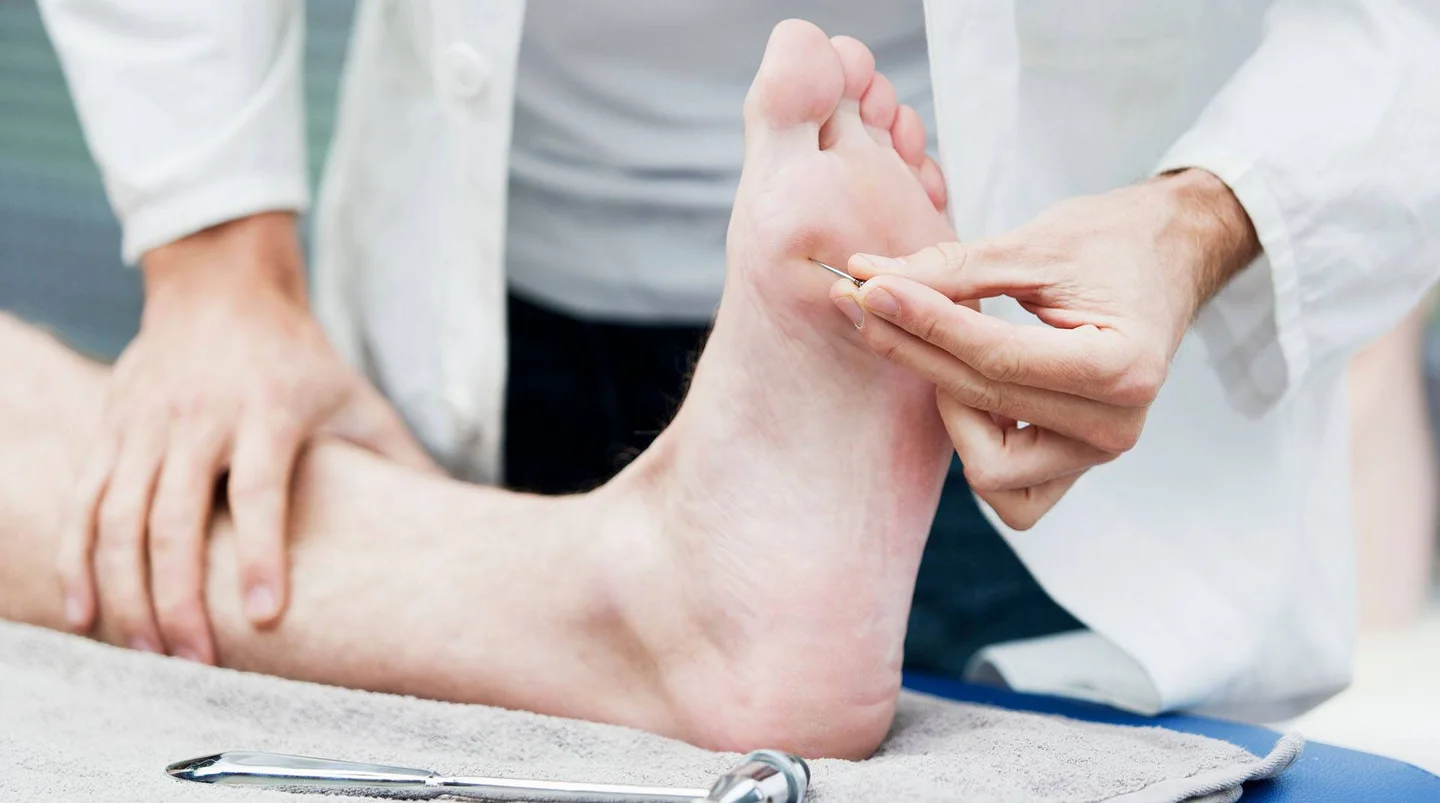
What is polyneuropathy?
Nerves located outside of the spinal cord and brain are known as peripheral nerves. These have many different functions. For example, they control muscle movement and transmit stimuli such as touch, heat or pressure to the brain.
Conditions caused by damage to these nerves are referred to as polyneuropathy or peripheral neuropathy.
The causes may be very varied and are not always known. Nerve damage is often caused by poorly managed diabetes (diabetic neuropathy) or heavy alcohol consumption (alcoholic neuropathy).
Pain and prickling sensations called paresthesia – particularly in the feet – are common symptoms. Muscle weakness and an unsteady gait may also be indicators of polyneuropathy.
Treatment aims to identify and eliminate the cause as far as possible.
What are the signs of polyneuropathy?
There is a wide range of symptoms, which differ depending on which nerves are affected.
Examples of symptoms caused by damage to sensory nerves controlling sensitivity are listed below:
- paresthesia, for example, prickling sensations, formication (a sensation of insects crawling on the skin) or the feeling of being pricked by a needle
- itching, numbness
- stabbing or burning pain – occurring spontaneously or due to light touch (e.g. through clothing)
- a feeling of being cramped, unpleasant feelings of pressure or a sensation of walking “on cotton wool”
- decreased sensitivity or lack of sensitivity to temperature changes
- unsteady gait, particularly in the dark
- painless wounds
If motor nerve fibers – the nerves that are important to movement – are affected, the person usually experiences symptoms such as:
- muscle weakness and pain
- muscle twitches and cramps
If nerve damage occurs in the organs, the following symptoms may occur, depending on which organ system is involved:
- heart palpitations when at rest
- feeling dizzy and faint, especially after standing up
- constipation, bloating, diarrhea
- difficulty urinating or bladder weakness (incontinence)
- decreased or increased sweating
- erectile dysfunction in men
What causes polyneuropathy?
The peripheral nerves are sensitive to inflammatory processes in the body, which can be caused, for example, by infections or exposure to toxic substances (cytotoxins) such as alcohol.
This can cause damage to the protective sheath surrounding the nerve fibers (the myelin sheath) or to the nerve fibers themselves.
Hereditary factors or diseases such as diabetes can also cause nerve damage.
Other possible causes are:
- an HIV infection that has been present for some time
- kidney diseases at an advanced stage
- cancer
- autoimmune diseases like Guillain-Barré syndrome
- bacterial infections, such as Lyme disease
- an underactive thyroid
- certain antibiotics and drugs used to treat cancer
- a vitamin B12 deficiency, for example, due to rapid weight loss or surgery to treat obesity
- excessive consumption of alcohol and drugs
In very many people with polyneuropathy – especially those in older age – the exact cause remains unknown.
How common is polyneuropathy?
Around 3% of the population will develop polyneuropathy at some point in their lives.
The most common cause is diabetes – almost half of all people with diabetes will develop nerve damage.
Polyneuropathy is similarly common among people with an alcohol dependency.
What is the outlook for polyneuropathy?
How polyneuropathy develops varies considerably between individuals.
Damage to sensory nerves (for example, due to poorly managed blood sugar levels) usually develops slowly. Often, the legs are the first to be affected by impaired sensitivity, followed by the hands.
If polyneuropathy is caused by cytotoxins (toxins that kill cells) such as alcohol, progression of the disease depends on how much of the cytotoxin has entered the body – sensory impairment will increase in tandem with alcohol consumption.
If polyneuropathy is caused by inflammatory or inherited conditions, the nerve damage usually progresses on a continuous basis. Depending on the severity of the condition, episodes of rapid progression may be interspersed with stable phases.
How is polyneuropathy diagnosed?
To determine what is causing the polyneuropathy, an in-depth consultation with a doctor is required.
The doctor will ask, for example, about:
- which symptoms the patient is experiencing
- when and where these first occurred
- whether it is only the feet and hands that are affected or other parts of the body also
- whether the symptoms are increasing or changing
- whether the patient has any pre-existing conditions
- which medication the patient is taking
- how much alcohol or drugs they consume
- details of their sexual life and whether they have any sexually transmitted infections
A physical examination may also be necessary. This serves to check:
- the patient’s sensitivity to stimuli
- how well they can walk and stand
- whether any muscles are weakened or paralyzed
- how well the reflexes are working
The following methods are used to determine which nerves are damaged and to what extent:
- Electroneurography (ENoG) is a method doctors use to determine how nerve impulses are transmitted and distributed in the body.
- They use electromyography (EMG) to ascertain how well the muscles respond to nerve impulses.
To obtain more information to help track down the cause, they may also test the patient’s urine, blood or cerebrospinal fluid (liquor), take tissue samples or perform genetic testing and use imaging techniques, such as ultrasound and magnetic resonance imaging (MRI).
How is polyneuropathy treated?
If polyneuropathy is caused by other conditions, these must be treated first.
Important: Treating the condition may improve the symptoms but will not completely cure the polyneuropathy.
Accompanying pain therapy is also important. This usually consists of treatment with antidepressants or anticonvulsants.
Doctors predominantly use antidepressants to treat depression. They cause the body to increase its production of chemical messengers that block the transmission of pain signals. As a result, the perception of pain is weakened. This can also benefit people with polyneuropathy.
Anticonvulsants are drugs used mainly to treat seizures in epilepsy. These drugs inhibit the sensitivity of nerves, reducing pain as a result.
If these do not adequately relieve the pain of polyneuropathy, opioid painkillers may prove effective. However, these should normally be used for short periods only, as they can be addictive.
- Bodman MA, Varacallo M. Peripheral Diabetic Neuropathy. [Updated 2022 Feb 12]. In: StatPearls [Internet]. Treasure Island (FL). StatPearls Publishing; 2022 Jan-. Aufgerufen am 14.03.2022.
- Deutsche Gesellschaft für Neurologie e.V. (DGN). Diagnostik bei Polyneuropathien. S1-Leitlinie. AWMF-Registernummer 030-067. 03.2019.
- DynaMed (Internet), Ipswich (MA). Peripheral Neuropathy. EBSCO Information Services. Record No. T474253. 2020 (1995). Aufgerufen am 14.03.2022.
- UpToDate (Internet). Overview of polyneuropathy. Wolters Kluwer 2020. Aufgerufen am 14.03.2022.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at:


