Conditions Underactive thyroid
ICD codes: E03 What are ICD codes?
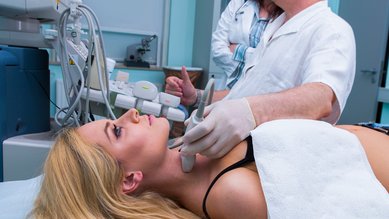
An underactive thyroid (hypothyroidism) occurs when the thyroid gland does not produce enough hormones. This slows down the metabolism. People affected by this condition often feel lethargic, have a low heart rate and suffer from constipation. A blood test is a reliable way to diagnose hypothyroidism.
At a glance
- If the thyroid gland does not produce enough hormones, this is referred to as an underactive thyroid (hypothyroidism).
- An underactive thyroid slows down the metabolism.
- Symptoms include, for example, fatigue, listlessness or constipation.
- The most common cause of underactive thyroid is a thyroid disease known as Hashimoto’s thyroiditis.
- In adults, an underactive thyroid often develops slowly and insidiously.
- In older people in particular, the disease may be mistaken for age-related changes.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
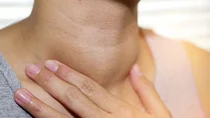
What is an underactive thyroid?
An underactive thyroid (hypothyroidism) occurs when the thyroid gland does not produce enough hormones. The thyroid gland is a vital organ. It produces hormones that regulate metabolic processes and keep them in balance. The thyroid hormones control a large number of processes in the human body.
An underactive thyroid slows down the metabolism. As a result, it can cause general symptoms such as tiredness, listlessness or constipation.
Most cases of underactive thyroid are caused by a chronically inflamed thyroid gland. An underactive thyroid can be rectified by taking tablets containing thyroid hormones daily. These hormone tablets usually cause the symptoms to disappear.
Video What are the common forms of thyroid disease?
This video explains what the most common forms of hypothyroidism and hyperthyroidism are, what causes them and how they are treated.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What symptoms indicate an underactive thyroid?
An underactive thyroid can affect many parts of the body and cause a wide range of symptoms.
General symptoms include:
- weakness
- tiredness
- low heart rate
Psychological problems may also occur, such as:
- concentration and memory problems
- lethargy
- depression or other mental health issues
Certain physical changes are also possible, including:
- mild to moderate weight gain
- constipation
- dry hair, hair loss
- low-pitched, hoarse voice
- enlarged tongue
- dry skin and puffiness, especially on the face
- enlarged thyroid, also referred to as goiter
- hearing impairment
- heavy or irregular periods, fertility problems
- erectile dysfunction
There are also symptoms that affect the body as a whole, such as:
- muscle pain or joint pain
- slower reflexes
- feeling cold and sensitivity to cold
- tingling and numbness
Many of these symptoms may have other causes too. In older people in particular, an underactive thyroid may be mistaken for age-related changes. This may happen, for example, with people in the initial stages of dementia. This means that blood tests are essential to confirm a suspected diagnosis of an underactive thyroid.
If the thyroid gland does not produce enough hormones this slows down the metabolism, which may affect many parts of the body and cause very specific problems. Potential symptoms include:
- exhaustion, weakness and fatigue
- low heart rate
- sensitivity to cold and decreased sweat production
- shortage of breath (dyspnea) during exertion
- mild to moderate weight gain
- difficulty concentrating or memory problems, slow thoughts or speech
- constipation
- dry skin and hair, hair loss
- yellowing of skin
- low-pitched, hoarse voice
- enlarged tongue
- puffy, swollen skin
- enlarged thyroid (also referred to as struma or goiter)
- hearing impairment
- muscle pain or joint pain
- slower reflexes
- heavy or irregular periods, fertility problems
- erectile dysfunctions
- lethargy
- depression or other mental abnormalities
Many of these symptoms may have other causes too. In older people in particular, an underactive thyroid may be mistaken for age-related changes. This may happen, for example, in people with incipient dementia. So blood tests are essential to confirm a suspected diagnosis of an underactive thyroid.
What causes an underactive thyroid?
An underactive thyroid may have a range of causes. Conditions and factors that can lead to a deficiency in thyroid hormones include:
- inflammation of the thyroid gland
- thyroid gland removal or radiotherapy
- severe iodine deficiency
- medication
- congenital hypothyroidism
Inflammation of the thyroid gland
In people with Hashimoto’s thyroiditis, the thyroid gland is chronically inflamed. This auto-immune disease is the most common cause of an underactive thyroid. It causes the body’s immune system to mistakenly identify thyroid cells as foreign bodies. In response, antibodies are produced that attack the thyroid gland and cause inflammation. The inflammation remains limited to the thyroid gland. An inflamed thyroid gland may also be caused by an infection.
Thyroid gland removal or radiotherapy
Treatment of some conditions, such as an overactive thyroid or thyroid cancer, involves exposing the thyroid gland to radiation or surgery to remove it entirely or in part. Parts of the thyroid gland are also surgically removed to treat an enlarged thyroid (goiter). Following these treatments, the thyroid gland produces insufficient amounts of hormones or none at all. Radiotherapy can lead to an underactive thyroid developing very slowly and only being detected several years later.
Severe iodine deficiency
Iodine is an important trace element. The body needs it to produce the thyroid hormones. As the body cannot produce iodine itself, it must absorb it from food. An underactive thyroid may develop if the body fails to get enough iodine from food over an extended period. However, this is very rarely the case in industrialized countries today.
Medication
Certain medications, such as antidepressants containing the active substance lithium, can inhibit the production of thyroid hormones. Some drugs used to treat an overactive thyroid can also inhibit the production of thyroid hormones. If the dosage is too high, this can cause an underactive thyroid.
Congenital hypothyroidism
An underactive thyroid is only genetically determined in rare cases. If a pregnant woman consumes very little iodine or if her immune system develops antibodies against the tissue of the thyroid gland, this can cause an underactive thyroid in her child.
In each of the cases described above, the thyroid gland itself is affected. This is known as primary hypothyroidism. However, an underactive thyroid can also be caused by conditions affecting the pituitary gland or the hypothalamus in the brain. The pituitary gland and hypothalamus produce hormones that control hormone production in the thyroid gland. This means that a thyroid gland may itself be healthy but may no longer be controlled correctly so that it fails to produce enough hormones. Doctors refer to this as secondary or central hypothyroidism.
Video What is autoimmune disease?
The video below provides basic information on the human immune system and typical autoimmune diseases.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
How common is an underactive thyroid?
In countries like Germany, around 5 percent of people have an underactive thyroid. It more commonly affects women and older people. Around 1 in every 3,400 babies is born with an underactive thyroid.
How does an underactive thyroid progress?
How an underactive thyroid progresses varies depending on what causes it. Most adults affected have an inflamed thyroid gland. This normally causes a gradual decomposition of the thyroid tissue. In these cases, an underactive thyroid often develops insidiously. For a certain period of time, the remaining thyroid tissue can compensate for the tissue that is lost by increasing its production of hormones so that the body still has an adequate supply. However, as the condition progresses, more and more tissue is lost, until the gland can no longer produce enough hormones. Symptoms then appear.
The missing thyroid hormones can easily be replaced by taking tablets. This restores normal metabolism and the symptoms disappear. Sometimes, the thyroid heals by itself – for example, when the inflammation clears up.
What can be done to prevent an underactive thyroid?
Iodine deficiency is now only very rarely the cause of an underactive thyroid in Germany. An underactive thyroid caused by an iodine deficiency can be prevented by ensuring an adequate intake of iodine. This can be done by consuming milk or dairy products daily and by regularly eating salt-water fish and using iodized salt. There are also certain food supplements that contain iodine.
Important: Excessive iodine levels are also a problem in the long term. They increase the risk of an overactive thyroid. However it is virtually impossible to overdose from food. The exception to this is dried algae, especially seaweed. It contains so much iodine that people could exceed the maximum daily recommended dose of 500 micrograms. Food supplements can also be problematic if the daily dose contains more than 100 micrograms of iodine.
Is early detection of an underactive thyroid possible?
A normally functioning thyroid gland is particularly important for babies and children. An underactive thyroid can have very adverse effects on physical and mental development.
All newborn babies undergo routine screening to measure their thyroid hormone levels so that any treatment needed can be started as soon as possible. The TSH reading is particularly important. TSH stands for “thyroid stimulating hormone”, a hormone that is produced and released by the pituitary gland to stimulate the production of hormones in the thyroid gland. An elevated TSH reading is an indicator of an underactive thyroid gland. If the TSH reading is elevated but there are no symptoms, this is known as latent hypothyroidism.
There is no scientific evidence of the benefits of measuring adult hormone levels for screening purposes. Therefore, adult screening is not recommended.
Important: TSH levels are not conclusive on their own. A relatively large number of people have slightly elevated TSH levels. However, this doesn’t automatically mean that their thyroid isn’t producing enough hormones. In any case, these levels often normalize by themselves. Which means that a routine test could lead to unnecessary treatment and worry.
How is an underactive thyroid treated?
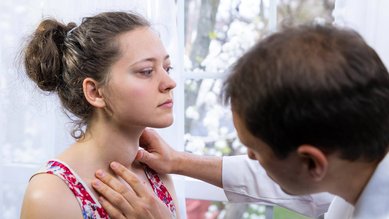
To diagnose underactive thyroid, the doctor begins by asking about the symptoms. This is followed by a physical exam (palpation) of the thyroid gland. If there are any indications of underactive thyroid, a blood test is required because many of the symptoms can also have alternative causes. The blood test measures thyroid hormone and TSH levels.
TSH is a hormone produced in the pituitary gland to stimulate the production of thyroid hormones. Slightly elevated TSH levels may be the first sign of an incipient underactive thyroid. This is because the pituitary gland responds to a weakening of the thyroid function by increasing its own production of TSH in an effort to further stimulate the thyroid gland. At a certain point, however, this is no longer sufficient and the thyroid gland no longer releases enough hormones into the bloodstream. This can also be detected in a blood test.
However, an elevated TSH reading doesn’t always mean that the person will be diagnosed as having underactive thyroid with symptoms. Every year, on average, only 2 to 5 out of every 100 people with elevated TSH levels develop symptoms that require treatment. If the TSH levels are very high, or the blood contains certain antibodies, the risk is higher. Women are at a higher risk than men.
How is underactive thyroid treated?
The treatment of underactive thyroid seeks to compensate for the hormone deficit. The missing thyroid hormone (thyroxine) is replaced by a drug that is identical to the hormone produced by the body. The active ingredient is also referred to as levothyroxine or L-thyroxine. The drug restores hormone levels to normal so that symptoms usually clear up entirely. Depending on the cause, treatment of an underactive thyroid is either temporary or lifelong.
There are virtually no side effects provided the right dose is given. The dosage is based on body weight. It can be adjusted after 2 to 3 months as required, which is the length of time it takes for hormones levels in the body to stabilize.
In the case of latent hypothyroidism, only the TSH reading is elevated but there are no symptoms. There is some disagreement among experts as to the point at which treatment should begin in such cases.
For more detailed information about whether and when an underactive thyroid should be treated, visit gesundheitsinformation.de.
- Bekkering GE, Agoritsas T, Lytvyn L et al. Thyroid hormones treatment for subclinical hypothyroidism: a clinical practice guideline. MJ. 2019 May 14;365:l2006. doi: 10.1136/bmj.l2006. PMID: 31088853.
- Bundesinstitut für Risikobewertung (BfR). Jodversorgung in Deutschland wieder rückläufig – Tipps für eine gute Jodversorgung. 09.02.2021.
- Bundesinstitut für Risikobewertung (BfR). Verwendung von Mineralstoffen in Lebensmitteln. BfR Wissenschaft: Berlin 2004.
- Chaker L, Bianco AC, Jonklaas J et al. Hypothyroidism. Lancet. 2017 Sep 23;390(10101):1550-1562. doi: 10.1016/S0140-6736(17)30703-1. Epub 2017 Mar 20. PMID: 28336049; PMCID: PMC6619426.
- Deutsche Gesellschaft für Kinder- und Jugendmedizin e.V. (DGKJ), Deutsche Gesellschaft für Endokrinologie e.V. (DGE). Angeborene primäre Hypothyreose: Diagnostik, Therapie und Verlaufskontrolle. S2K-Leitlinie. AWMF-Registernummer 027-017.
- Gesellschaft für Neonatologie und pädiatrische Intensivmedizin e.V. (GNPI). Neugeborenen-Screening auf angeborene Stoffwechselstörungen und Endokrinopathien, schwere kombinierte Immundefekte (SCID), Sichelzellkrankheit, 5q-assoziierte spinale Muskelatrophie (SMA) und Mukoviszidose. S2k-Leitlinie. AWMF-Registernummer 024-012.
- Jameson JL, Mandel SJ, Weetmann AP. Disorders of the Thyreoid Gland. In: Kaspers D. L., Hauser S. L., Jameson J. L. et al (Ed). Harrison's Principles of Internal Medicine. McGraw-Hill Education 2015.
- Pearce SH, Brabant G, Duntas LH et al. 2013 ETA Guideline: Management of Subclinical Hypothyroidism. Eur Thyroid J. 2013 Dec;2(4):215-28. doi: 10.1159/000356507. Epub 2013 Nov 27. PMID: 24783053; PMCID: PMC3923601.
- Persani L, Brabant G, Dattani M, Bonomi M, Feldt-Rasmussen U, Fliers E et al. 2018 European Thyroid Association (ETA) Guidelines on the Diagnosis and Management of Central Hypothyroidism. Eur Thyroid J. 2018 Oct;7(5):225-237. doi: 10.1159/000491388. Epub 2018 Jul 19. PMID: 30374425; PMCID: PMC6198777.
- Reyes Domingo F, Avey MT, Doull M. Screening for thyroid dysfunction and treatment of screen-detected thyroid dysfunction in asymptomatic, community-dwelling adults: a systematic review. Syst Rev. 2019 Nov 18;8(1):260. doi: 10.1186/s13643-019-1181-7. PMID: 31735166; PMCID: PMC6859607.
- Schübel J, Feldkamp J, Bergmann A et al. Latente Hypothyreose des Erwachsenen. Dtsch Arztebl Int 2017; 114(25): 430-438.
- UK National Screening Committee (UK NSC). Screening for thyroid dysfunction in adults. External review against programme appraisal criteria for the UK National Screening Committee (UK NSC). 06.2017.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: