Conditions Lyme disease
ICD codes: A69.2 What are ICD codes?
Lyme disease is an infectious disease that is triggered by bacteria. It can be transmitted by ticks. Around three out of every 10,000 people contract Lyme disease every year in Germany.
At a glance
- Lyme disease is an infectious disease caused by bacteria.
- It can be transferred to humans by tick bites.
- An infection is less likely if the tick is removed in time.
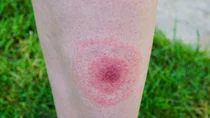
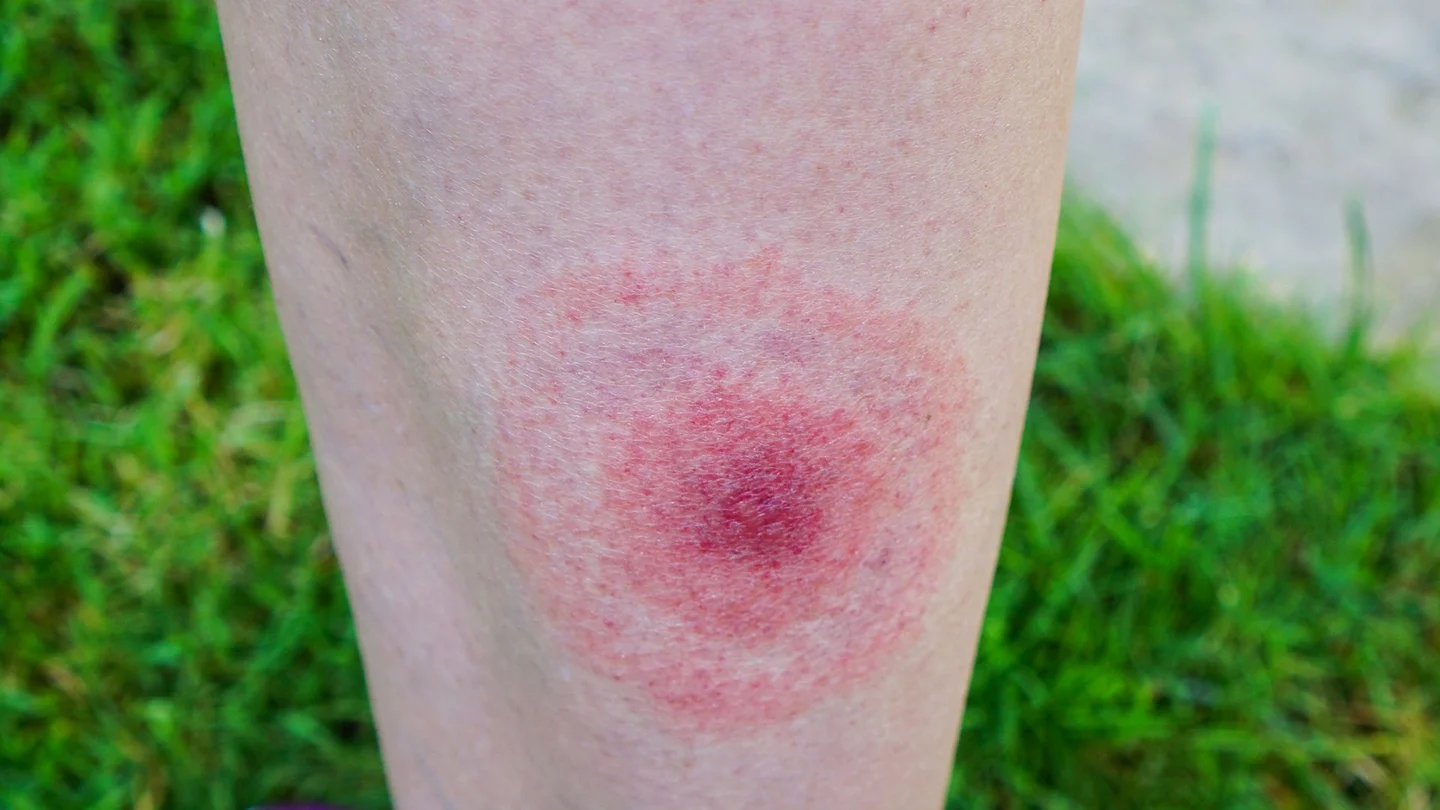
- Lyme disease can cause a rash with a ring-like appearance on the skin around the bite or flu-like symptoms.
- It is usually treated with antibiotics.
- In Germany, around three people out of every 10,000 develop Lyme disease each year.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is Lyme disease?
Anyone who spends time in the countryside is at risk of getting bitten by a tick. Some ticks transmit diseases such as Lyme disease. Lyme disease is an infectious disease that is triggered by bacteria. Lyme disease is also known as Lyme borreliosis.
The first sign of Lyme disease is inflamed skin near the bite. The bacteria that cause the infection – called Borrelia bacteria – may later go on to attack joints or various organs. However, the infection doesn’t usually cause any serious problems.
Video What are the signs of Lyme disease (borreliosis)?
The video below explains more about how you can become infected with Lyme disease as well as the symptoms and treatment options.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What are the signs of Lyme disease?
The skin around a tick bite usually turns red and becomes itchy. This inflammatory reaction is normal and has nothing to do with Lyme disease.
However, if the skin near the bite is red a few days or weeks after the person was bitten, this could be a sign of Lyme disease. A Lyme disease rash typically spreads outwards with a ring-like appearance until it reaches a diameter of more than five centimeters. This rash is called erythema migrans (Latin for “migrating redness”), or EM rash for short.
Flu-like symptoms such as fever, headache, drowsiness or aching muscles can also develop within six weeks of being bitten. These symptoms may also be signs of Lyme disease, even if there is no EM rash.
Flu-like symptoms appearing after one or two weeks may indicate tick-borne encephalitis (TBE), but that is rare.
Post-Lyme syndrome / “Chronic Lyme disease” – what does it mean?
Some people experience symptoms like achy muscles and joints, severe exhaustion or memory problems months or even years after being bitten by a tick. Some of these people and some doctors believe that the symptoms are a delayed complication of a Borrelia bacteria infection. This group of symptoms is sometimes referred to as post-treatment Lyme disease syndrome or “chronic Lyme disease” – although the latter is not generally accepted as a diagnosis.
These symptoms are sometimes linked to Lyme disease even if the person is not known to have been bitten by a tick and the blood tests fail to show any evidence of infection. In such cases, it is unlikely that the symptoms are actually connected to an infection with Lyme disease, as similar symptoms also occur as part of many other health conditions.
What increases the risk of developing Lyme disease?
The risk of a tick bite causing Lyme disease will mainly depend on
- how long the tick was attached to the skin, and
- the age and size of the tick.
Large ticks are more likely to be infected with Lyme disease than small ones because they are older and will generally have fed on more host animals.
Borrelia bacteria are found in all parts of Germany, but the proportion of infected ticks varies greatly from region to region.
Even if someone is bitten by an infected tick, they will not necessarily get Lyme disease. The Borrelia bacteria live in the bowel of the tick. This means that the host will only become infected – if at all – after the tick has fed for quite a long time.
That is why checking the body soon after spending time outdoors, and removing any ticks within 24 hours, is an effective way to prevent Lyme disease.
How common is Lyme disease?
It is estimated that about one percent of people who are bitten by a tick develop Lyme disease. In Germany, around three out of every 10,000 people develop the disease each year.
How can Lyme disease be prevented?
The risk of tick bites will depend among other things on the region and a person’s general behavior in nature.
One way of protecting oneself is to wear closed shoes when in tall grass or bushes. Clothing which covers as large an area of the body as possible – for example long trousers and long-sleeved T-shirts – is also recommended. This makes it harder for ticks to attach themselves.
Light clothing can also be a good idea, as it is easier to identify ticks than on darker clothes.
Before ticks bite, they sometimes crawl around on the body for hours. Checking one’s body soon after spending time in the woods or in the garden and removing any ticks can stop a bite from happening and reduces the risk of developing Lyme disease.
Children often forget to do this so it is important to remind them. Both children and adults should get help from another person when checking their bodies – especially in places that are difficult to check on their own.
Anyone bitten by a tick should watch to see if any symptoms develop which indicate an infection. If there is indeed an infection, it is necessary to see a doctor.
Important: According to the Robert Koch Institute, tick sprays (repellents) can offer a certain amount of protection from ticks for about two to four hours. However, the effect then wears off. As a result, these sprays have to be used repeatedly if staying outside for a longer period of time.
How is Lyme disease diagnosed?
If a typical rash has developed, Lyme disease can be diagnosed just by looking at it. It is important to tell the doctor about the tick bite.
If the physical examination is not sufficient, the blood may be tested for borrelia bacteria.
How is Lyme disease treated?
Lyme disease is treated with antibiotics over a period of two to three weeks, depending on the symptoms. The disease then usually goes away without any complications. Sometimes, though, initial treatment with antibiotics isn’t effective enough, and you might need to use different antibiotics.
The symptoms of Lyme disease may also get better by themselves without taking antibiotics, but then the disease is more likely to lead to more serious complications.
What are the possible long-term effects?
If the bacteria spread within the body, the first symptom is a burning pain near the tick bite.
Around three percent of people develop a disease called neuroborreliosis. When this happens, the infection spreads to the brain and nerves. This can lead to paralysis (often affecting the face), painful nerve inflammations, or meningitis.
Another complication that can develop months or even years after someone is infected is called Lyme arthritis. This affects about two percent of people. Lyme arthritis arises if the infection spreads to the joints, causing painful inflammations and swelling.
Very rare complications include heart problems and chronic inflammation of the skin.
Both neuroborreliosis and Lyme arthritis can be treated effectively with antibiotics and usually don’t have any long-term effects.
How can ticks be removed?
When a tick attaches itself to the skin, it is important to remove it as soon as possible.
Special tick removal tools can be used:
- tick tweezers
- tick-removal cards
- tick hooks
These tools are shaped to make it easy to slide them between the tick and the skin without squeezing the tick. These kinds of aids are available in pharmacies, for example.
Normal tweezers can also be used, as long as the tips of the tweezers bend inwards.
But if the tips are flat, the tick will be automatically squeezed when trying to get hold of it. This should be avoided because pathogens could be squeezed out of the tick and into the body in this way.
More detailed information about removing ticks can be found at gesundheitsinformation.de.
Where can I find support for Lyme disease?
Self-help groups offer people with Lyme disease and their relatives a way of obtaining information and advice, and sharing personal experiences.
You can find suitable self-help via a database on the National Contact and Information Point For Encouraging and Supporting Self-Help Groups (NAKOS) website.
- Cadavid D, Auwaerter PG, Rumbaugh J et al. Antibiotics for the neurological complications of Lyme disease. Cochrane Database Syst Rev. 2016 Dec 8;12(12):CD006978. doi: 10.1002/14651858.CD006978.pub2.
- Deutsche Gesellschaft für Neurologie e.V. (DGN). Neuroborreliose. S3-Leitlinie. AWMF-Registernummer 030-071. 11.2020.
- Enkelmann J, Bohmer M, Fingerle V et al. Incidence of notified Lyme borreliosis in Germany, 2013-2017. Sci Rep. 2018 Oct 8;8(1):14976. doi: 10.1038/s41598-018-33136-0.
- Richardson M, Khouja C, Sutcliffe K. Interventions to prevent Lyme disease in humans: A systematic review. Prev Med Rep. 2018 Nov 13;13:16-22. doi: 10.1016/j.pmedr.2018.11.004.
- Robert Koch-Institut (RKI). FSME: Antworten auf häufig gestellte Fragen zu Zecken, Zeckenstich, Infektion. 09.2020.
- Robert Koch-Institut (RKI). RKI-Ratgeber. Frühsommer-Meningoenzephalitis (FSME) und verwandte Virusenzephalitiden (TBE, tick-borne encephalitis). 04.2022.
- Warshafsky S, Lee DH, Francois LK et al. Efficacy of antibiotic prophylaxis for the prevention of Lyme disease: an updated systematic review and meta-analysis. Antimicrob Chemother. 2010 Jun;65(6):1137-44. doi: 10.1093/jac/dkq097.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at:


