Conditions Shingles
ICD codes: B02 What are ICD codes?
Shingles (herpes zoster) occurs through infection by the varicella-zoster virus. Older people and people with immune deficiency are most commonly affected. The condition is characterized by severe pains and a typical skin rash. Both always occur on one side of the body. All cases of shingles must be medically treated.
At a glance
- Shingles is a condition caused by varicella-zoster viruses lying dormant in the body.
- Anybody can catch it. Older people and people with immune deficiency are particularly affected.
- Shingles may occur anywhere on the body. Often, only one area is affected, for example the chest or torso.
- 80 percent of sufferers have pain that is very much limited to one side of their body. Later, a skin rash typically breaks out where the pain occurs.
- It is important to immediately get medical treatment with painkillers and antiviral drugs.
- People over the age of 60, and those with a greater risk of a severe progression are advised to get vaccinated.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is shingles?
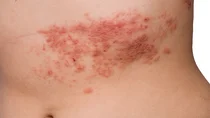
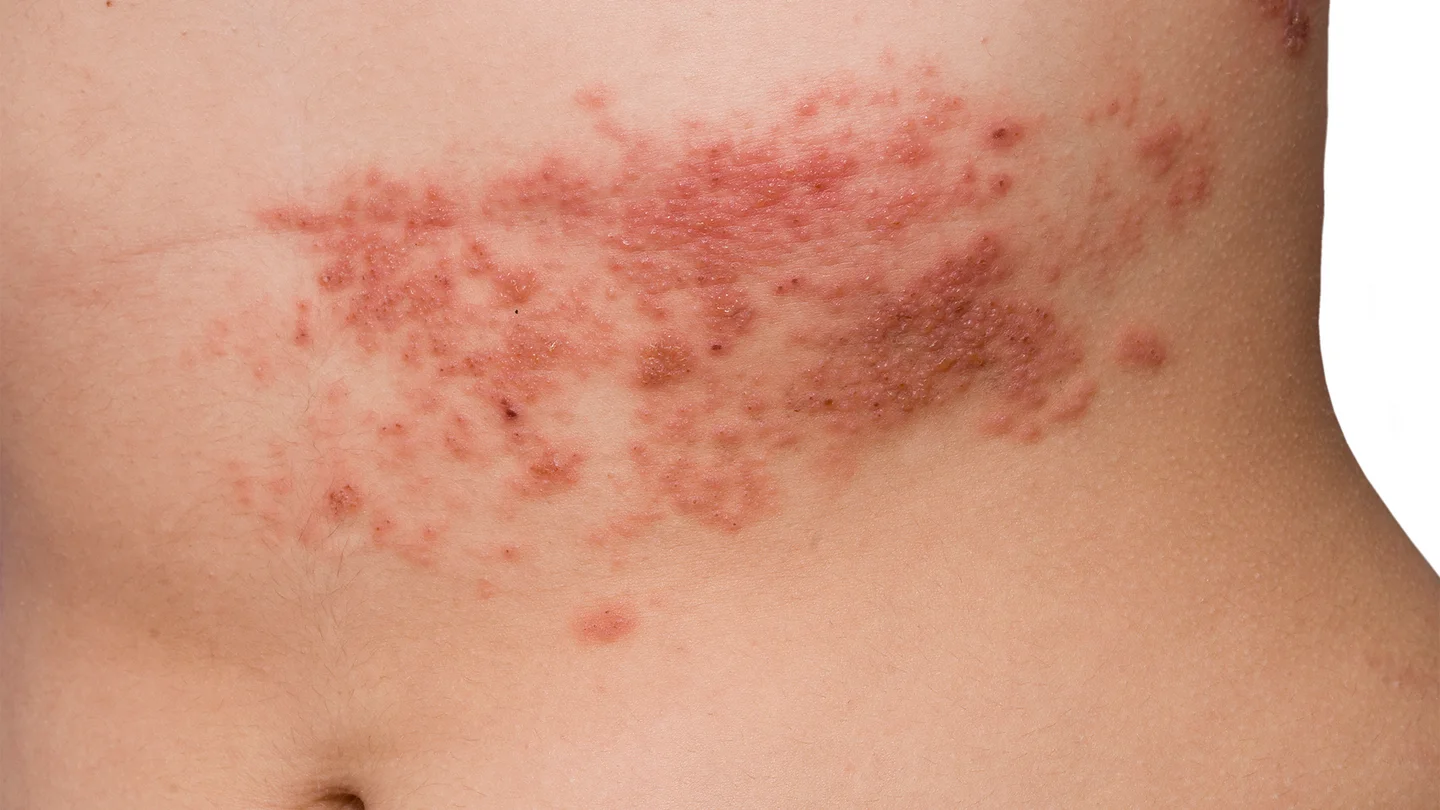
Shingles is the most common acute skin infection. It is important that it is identified and treated at an early stage. In 80 percent of cases the condition first makes itself known through severe pain. Later on, a blister-type skin rash that can spread like a belt develops where the pain is. It is significant that the symptoms always occur on one side of the body, i.e. they never spread across the mid-line of the body.
Essentially, shingles can occur anywhere on the body. The chest or torso are often affected. Typically only one part of the body is affected.
Shingles is triggered by dormant varicella-zoster viruses being reactivated in the body. The first time the person is infected, these viruses cause chickenpox. So shingles can develop in anyone who has had chickenpox at any time.
Older people and people with immune deficiency have a greater risk of suffering from shingles.
What causes shingles?
When a person is infected by the varicella-zoster virus for the first time and papules and blisters then develop over the entire body, we talk of chickenpox (varicella). Before the general chickenpox vaccine recommendation in 2004, most school-age children were carriers of the virus and went through chickenpox.
Once the chickenpox is over, the virus nests in the nerve cells of the brain and spinal cord. It remains there, inactive throughout the person's life. However, if the immune system weakens – for example due to stress, too little sunlight, or taking drugs like cortisone – the virus may be reactivated. It then moves through the nerve system to the skin, where the painful inflammations and typical skin rash occur. At this point it is no longer chickenpox, but shingles.
Video What causes shingles?
This video explains how shingles develops and what symptoms it may cause.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
How does the infection occur?
Shingles is not as easily transmitted as chickenpox. Only the fluid in the skin blisters is infectious, because it contains the viruses. This means that people that have not had chickenpox and who are not vaccinated against it can be infected if they come into contact with the blisters. These people then suffer from chickenpox, not shingles.
Important: Patients with shingles can substantially reduce the risk of infecting others by covering the areas affected, providing that a crust has not yet formed.
What symptoms does shingles cause?
Typically there is a skin rash limited to one side of the body, with small, reddish nodules or blisters, usually in the chest and torso area. However the eye, ear, oral cavity, and genital area can also be affected. The rash is always limited to one side of the body. The areas affected tingle sometimes and they are often very painful.
Once the rash has healed the pains, caused by nerve inflammations, may continue for some time (so-called post-herpetic neuralgia). In rare cases the pain persists over the long term.
Sometimes the typical skin rash fails to occur. Then medical practitioners speak of shingles without a rash (Zoster sine herpete). In these cases there is only the characteristic pain which does not cross the mid-line of the body.
Who can become affected and how common is shingles?
Shingles particularly affects people over the age of 50. 6 out of every 1,000 people in their 50s and 13 out of every 1,000 people over 90 develop shingles. So the risk increases with age. People with immune deficiency are more frequently affected. But healthy people and young adults may also catch shingles.
Who should be vaccinated?
The Standing Committee on Vaccination (STIKO) at the Robert Koch Institute recommends the vaccination with the Herpes-zoster inactivated vaccine for everyone over the age of 60 and for people over 50 if they are particularly at risk due to an existing underlying condition. This includes people who are receiving immunosuppressive drugs.
This applies, for example, to patients with:
- HIV/Aids
- rheumatoid arthritis
- systemic lupus erythematodes (SLE)
- chronic inflammatory bowel diseases such as ulcerative colitis
- chronic lung diseases such as COPD and bronchial asthma
- chronic kidney disease
- diabetes mellitus
The statutory health insurance scheme covers the cost of vaccination for these groups.
The vaccine is given twice at an interval of at least two and at most six months. These take the form of an injection into the muscle.
Important: The shingles vaccine is different to the one for preventing chickenpox. Before the shingles vaccine there is no need to test the blood count to find out whether the person is a carrier of the virus because they have had chickenpox. Since the chickenpox vaccine has only been available since 2004 it may be assumed that most people aged over 50 today had the illness as a child.
You will find answers to the questions most frequently asked about the shingles vaccine on the Robert Koch Institute website.
There is also information about recommended vaccines on impfen-info.de – a website run by the Bundeszentrale für gesundheitliche Aufklärung (Federal Centre for Health Education).
How is shingles diagnosed?
If a patient complains of severe pain on one side of the body, not crossing the mid-line, for example at chest height, a doctor should always consider shingles. This is the only way to prevent the pain being attributed to other conditions and being treated incorrectly. Because with shingles, in particular, it is important to provide treatment at an early stage to avoid chronic pain and complications.
If the skin rash has broken out, the doctor will usually recognize that it is shingles, from its appearance and the fact that it is only on one half of the body. If shingles is suspected with no symptoms, a specific test is carried out in the laboratory. This applies, for example, if the rash is not only on one half of the body, or if the person has already had shingles.
Fluid from the skin blisters and a blood test are used for the laboratory tests. In the case of pregnant women, the amniotic fluid is also tested.
How does shingles progress?
Before a visible skin rash with nodules occurs, there is usually severe pain. There are also usually symptoms such as fatigue and a mild fever. The changes in the skin are observed around one to two days after the pain occurs: at the place where it hurts.
Within hours the skin rash nodules turn into itchy blisters. After around five days these burst and dry out. The skin rash can be extremely painful, especially in adults. The pain can persist for months or even years, even when the skin rash has healed. Medical practitioners call this post-zoster neuralgia or post-herpetic neuralgia.
It usually takes two to four weeks for the illness to go. Sometimes the areas of skin affected remain slightly darker or lighter than the surrounding skin.
In severe cases the brain and nervous system, and lungs or liver, can also be affected. The progression sometimes becomes life-threatening. Patients with immune deficiency have a greater risk of complications and the progression of the illness is severe. In children, the illness is generally benign.
How is shingles treated?
Shingles should always be treated medically. The shingles therapy always uses painkillers and antiviral drugs at the same time. Symptoms such as a high temperature can also be alleviated using fever reducers.
Medical treatment with painkillers
Shingles is very painful. The pain therapy aims to alleviate this and prevent the pain from becoming chronic. The more quickly the pain therapy begins, the better.
Medical treatment with antiviral drugs
Antivirals target the virus directly. The products used have active ingredients like aciclovir, valaciclovir, famciclovir and brivudine. Selecting a suitable product can speed up the healing of the rash and shorten the time with pain. The doctor decides which product is to be used. For an effective antiviral therapy it is important that it is started within 72 hours.
Older people and people with weak immune defense are usually given the antiviral drugs in the vein. They are in most cases admitted to hospital and monitored. If the illness develops complications such as eye problems, doctors administer the antiviral (in this case, aciclovir) intravenously.
Therapy with antivirals must be considered in these cases:
- people aged over 50
- shingles in the head-neck area
- severe pain
- a weak immune system
- a kidney weakness
- severe progression or a heightened risk of complications
Skincare
With shingles, careful skincare is also recommended. This can help alleviate the itching and to dry out the blisters. Zinc paste may be suitable, for example. It also acts as a disinfectant.
If blisters have formed already cooling, moist (drying) compresses can be applied. There is no scientific evidence that they help, however.
- Deutsche Dermatologische Gesellschaft (DDG). Diagnostik und Therapie des Zoster und der Postzosterneuralgie. S2k-Leitlinie. AWMF-Registernummer 013 – 023. 05.2019. Aufgerufen am 19.11.2020.
- gesundheitsinformation.de. Gürtelrose. Aufgerufen am 19.03.2020.
- Robert Koch-Institut (RKI). Gürtelrose (Herpes zoster): Antworten auf häufig gestellte Fragen zu Erkrankung und Impfung. Aufgerufen am 19.11.2020.
- Robert Koch-Institut (RKI). Infektionsepidemiologisches Jahrbuch meldepflichtiger Krankheiten für 2018. Berlin 2019. Aufgerufen am 19.11.2020.
- Robert Koch-Institut (RKI). RKI-Ratgeber. Windpocken (Varizellen), Gürtelrose (Herpes zoster). Aufgerufen am 19.11.2020.
Reviewed by the German Dermatological Society (Deutsche Dermatologische Gesellschaft e.V.).
As at:


