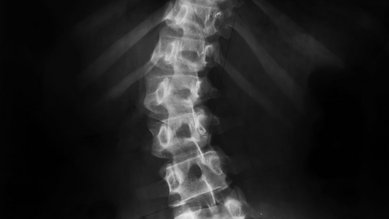
Conditions Spinal fractures
ICD codes: T08 What are ICD codes?
Spinal fractures often occur as a result of osteoporosis. Less frequently, this type of fracture is caused by serious traffic accidents or sports injuries. This article explains the symptoms of spinal fractures, how they can be prevented and what is involved in treatment and rehabilitation.
At a glance
- A spinal fracture can occur at any point along the spine. The thoracic spine (middle section) and lumbar spine (lower back) are often affected.
- Most spinal fractures occur as a result of osteoporosis. Less frequently, they are caused by traffic accidents or injuries sustained while playing sports.
- If the spinal cord is damaged or compressed, this can cause neurological deficits, including paralysis of the lower part of the body (paraplegia).
- The spine must be stabilized to avoid nerve damage.
- Fractures require rapid surgical intervention if the spinal cord is also involved. Pain medication and exercise therapy are usually sufficient to treat less severe fractures.
- Treatment aims to restore movement as fully as possible and to prevent chronic pain.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What are spinal fractures?
The spine consists of 33 small bones called vertebrae. They are divided into five groups – from top to bottom. These are the cervical vertebrae (neck), thoracic vertebrae (chest), lumbar vertebrae (lower back), sacral vertebrae (sacrum) and coccygeal vertebrae (coccyx or tailbone).
With the exception of the first two vertebrae in the neck and those in the sacrum and tailbone, all of these vertebrae consist of a vertebral body, vertebral arch, a number of articular and transverse processes and one spinous process.
At the center of these various parts of the vertebra is an opening called the vertebral foramen. All of the openings in the spinal vertebrae stacked one on top of the other form the spinal canal, which contains the spinal cord. The spinal cord is part of the central nervous system consisting of nerve fibers and blood vessels. It allows nerve impulses to travel between the brain and body.
Most spinal fractures occur due to conditions such as osteoporosis (bone atrophy). Less frequently, they result from serious falls, traffic accidents or sport-related injuries.
A fracture is considered stable if the spinal canal is not constricted as a result of the fracture and the spinal cord is not damaged. In such cases, there is no risk of the person suffering neurological damage. If the spinal cord is damaged or if there is a risk of neurological deficits, this is known as an unstable fracture.
Doctors treat spinal fractures based on the type and severity of the fracture in each case. The most important consideration is the stability of the fractured vertebra and whether the spinal canal is constricted in such a way that there is a risk of damage to the spinal cord.
Important: After a serious traffic accident or injury sustained while playing sports, the injured person should not be moved or only moved with the utmost care and caution until a spinal cord injury can be excluded.
What are symptoms of a spinal fracture?
In people with osteoporosis, the bones become weak, which can lead to spinal fractures. Around half of those affected in this way have no symptoms. However, acute or chronic back pain can occur. This pain is more severe when standing up or walking than when lying down. It is difficult to maintain muscle tension and balance when standing. If several vertebrae are affected, the spinal column becomes packed together and the person loses height.
Depending on their severity, fractures of the cervical vertebrae in the neck may be externally visible – for example, if bones have been displaced. Bruising or swelling may also occur. Severe neck pain and neurological symptoms, such as numbness or paralysis, may indicate damage to the spinal cord.
What causes spinal fractures?
The most common cause of a spinal fracture is bone atrophy (osteoporosis). In this condition, the body increasingly breaks down bone mass, making bones weaker and more likely to break. With osteoporosis, spinal fractures occur spontaneously – usually following compression of a disk or vertebra. For this reason, these fractures are also known as compression fractures.
However, spinal fractures can also be caused by a forceful impact – for example, in a car crash. Jumping from a height significant enough to put strong pressure on the spine so that it becomes compressed or twisted can also lead to a spinal fracture.
The most common accidents that cause spinal fractures include:
- car crashes or vehicles overturning
- falls from motorbikes or bicycles
- sport-related accidents, e.g. when skiing, horse riding or climbing
- work-related accidents, e.g. falling off scaffolding
What factors increase the risk of spinal fractures?
People who play contact or combat sports like wrestling or ice hockey are at an increased risk of suffering spinal fractures.
The risk of spinal fracture also increases with age. The older we get, the more our bone mass declines as part of the natural aging process. As a result, people over the age of 50 are more likely to suffer bone fractures in general.
Bone mass declines more than normal in people with osteoporosis. This means that their bones become porous and are easily broken in the event of a fall.
Other factors contribute to bones becoming weaker and more fragile. These include:
- previous bone fractures
- bone cancer
- bone inflammation (osteomyelitis)
- overactive thyroid (hyperthyroidism)
- in women: a low level of estrogen after the menopause
- smoking and high levels of alcohol consumption
- vitamin D deficiency
- long-term use of anti-inflammatory corticosteroids, such as cortisone
- chemotherapy and radiotherapy
How common are spinal fractures?
Compression fractures are common. This type of spinal fracture is mainly caused by illnesses such as osteoporosis.
Spinal fractures due to falls and accidents are less common. In as many as half of these cases, the section of spine between the chest and lower back is affected. Approximately one quarter of people who suffer this type of fracture have other fractures also – usually in the cervical spine in the neck.
What is the outlook for people who suffer spinal fractures?
Stable spinal fractures without compression of the spinal canal or injury of the spinal cord usually heal by themselves. In other words, they don’t require surgery.
Up to 40 percent of people who suffer a spinal fracture leading to serious spinal cord injury will develop chronic nerve damage.
The extent of neurological deficits occurring as a result depends on the severity of the injury. For mild problems, early treatment can help with the healing process.
Even if there are signs of partial paralysis due to spinal cord damage, the chances of recovery from symptoms such as muscle weakness or impaired sensitivity are good. Around 60 to 80 percent of patients make a full or partial recovery.
If the deficits are significant, the person may be unable to return to their previous job.
If the spinal fracture occurs in the cervical spine (neck), 5 to 10 percent of those injured will die – in particular if the injury is suffered in a motorcycle crash or car crash.
What can be done to prevent spinal fractures?
Spinal injuries can be avoided by taking certain safety and protective measures when playing sports, as a road user and at work. These include:
- ensuring that the driver and all passengers in the car are wearing their seat belts
- wearing a helmet and protectors when riding bikes and playing high-risk sports
- ensuring that proper safety equipment is used when working on scaffolding and ladders
- wearing a safety harness when climbing trees or mountains
Regular movement and exercises to build muscles also strengthen the bones. It is also beneficial to eat a balanced diet and to avoid cigarettes and alcohol.
In the case of osteoporosis, certain medication can reduce the risk of suffering further spinal fractures in the future. For example, bisphosphonates inhibit bone degradation.
Older people can also take measures to avoid falls – for example, by removing trip hazards or installing grab rails in their homes. Exercise programs and walking aids are also beneficial. Another important consideration is the side-effects and interactions of medications. This can help older people avoid becoming dizzy and light-headed, which can lead to falls.
How are spinal fractures diagnosed?
Doctors begin with a physical examination in which they palpate the spine to determine which parts of the spine are affected.
Imaging techniques are used to provide a reliable diagnosis of a spinal fracture. A computed tomography (CT) scan provides images of the spine at three levels to pinpoint the precise location and severity of the fracture. A magnetic resonance imagery (MRI) scan allows doctors to see injuries to the spinal cord, vertebral disks and ligaments.
Additionally, extensive neurological tests are conducted to determine whether and to what extent the spinal cord is damaged.
How are spinal fractures treated?
If a spinal injury is suspected following a serious accident, it is important to call an ambulance as quickly as possible by dialing 112. Until an emergency doctor arrives, the injured person should lie still, should not be moved if at all possible and must under no circumstances be carried or dragged to a different location.
Treatment of a spinal fracture seeks to restore the stability of the spine and preserve the functioning of the nerves and spinal cord.
Bed rest and pain therapy are initially indicated to promote the healing process.
Pain therapy in particular seeks to prevent chronic back pain. With less severe spinal fractures, a combination of medication, physiotherapy, occupational therapy and behavioral therapy is used. This helps the patient to begin moving again as soon as possible after a spinal fracture.
If these measures aren’t sufficient to restore the ability of move without pain, surgery may be required. If the fracture is so severe that the spinal canal is compressed or the spinal cord is damaged, surgery is required without delay.
Important: People who have suffered a spinal fracture causing damage to the spinal cord require intensive care. Severe spinal cord injuries often cannot be cured, so that the person is left with permanent physical or neurological limitations.
What is involved in rehabilitation following surgery for a spinal fracture?
After a stable fracture, i.e. where there are no neurological deficits, early rehabilitation helps people to return to their daily lives as quickly as possible. Rehabilitation ideally begins while treatment is still ongoing.
Depending on the patient’s level of mobility after a spinal fracture and the severity of their injuries, rehabilitation may take place on an inpatient or outpatient basis.
The main focus of rehabilitation is to restore the person’s normal posture and range of movement as far as possible. One important component of rehabilitation is therefore movement, which can include sports, physical therapy and occupational therapy. Psychological support can also be beneficial. Rehabilitation also explains how movement training can be incorporated into daily life and what measures can be taken in the workplace to strengthen the back.
In the case of severe spinal fractures with neurological deficits up to and including paraplegia (paralysis of the lower half of the body), it is important for patients to receive further treatment and rehabilitation in specialized centers as soon as possible.
What aftercare is required for spinal fractures?
To promote the healing process, extreme exercise and physical strain should be avoided after spinal surgery. More strain can be put on the spine once the bones have healed.
Special outpatient aftercare programs are offered to help make it easier for people to return to work and everyday life following surgery. People normally begin to return to work three months after an accident.
The programs teach strategies for making lifestyle and behavioral adjustments to make it easier to manage everyday life and ensure successful treatment outcomes.
The social services at the hospital and rehabilitation center provide advice about a patient’s entitlement to benefits and which measures are best suited to them. They also provide information about which costs are covered by health insurance providers.
- Deutsche Gesellschaft für Orthopädie und Orthopädische Chirurgie e.V. (DGOOC). Rehabilitation nach traumatischen Frakturen der Brust- und Lendenwirbelsäule ohne neurologische Ausfälle. S2k-Leitlinie. AWMF-Registernummer 033-043. 03.2016.
- Deutsche Gesellschaft für Unfallchirurgie e.V. (DGU). Verletzungen der thorakolumbalen Wirbelsäule. S1-Leitlinie. AWMF-Registernummer 012-028. 07.2018.
- DynaMed (Internet), Ipswich (MA): Cervical Spine Injury. EBSCO Information Services. Record No. T114826. 2018 (1995). Aufgerufen am 21.02.2022.
- Fernandez-de Thomas R, De Jesus O. Thoracolumbar Spine Fracture. [Updated 2021 Aug 30]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Aufgerufen am 21.02.2022.
- McMordie JH, Viswanathan VK, Gillis CC. Cervical Spine Fractures Overview. [Updated 2021 July 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Aufgerufen am 21.02.2022.
- National Institute for Health an Care Excellence (NICE). Spinal injury: assessment and initial management. NICE clinical guidelines, Band 41. 02.2016. Aufgerufen am 21.02.2022.
- Whitney E, Alastra AJ. Vertebral Fracture. [Updated 2021 Aug 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Aufgerufen am 21.02.2022.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: