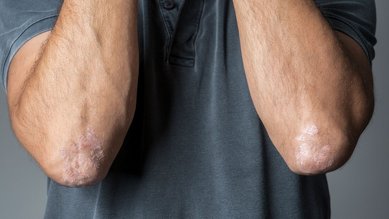
Conditions Vitiligo
ICD codes: L80 What are ICD codes?
Vitiligo is a skin pigmentation disorder. It appears as white patches on the skin. The causes remain unknown. This pigmentation disorder can be distressing from a cosmetic point of view, and many people with vitiligo feel stigmatized.
At a glance
- Vitiligo is a skin pigmentation disorder. It stops the production of pigments in certain areas of the body, causing white patches to appear on the skin.
- Vitiligo does not cause pain and is not contagious.
- Many people find the changes in their skin distressing, in many cases because they feel stigmatized by others.
- Treatment with medication and light can bring about a partial improvement in skin pigmentation.
- Skin patches can also be concealed with certain make-up products.
- It is important to protect the affected areas from external irritants, such as sunlight.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is vitiligo?
Vitiligo is a skin pigmentation disorder that causes a loss of the brown skin pigment melanin.
Pigments are normally produced by special skin cells called melanocytes. With vitiligo, it is likely that these skin cells are damaged by the skin’s immune response (autoimmune response) and stop producing pigments as a result. This causes the appearance of white patches on the skin.
Vitiligo usually begins between the ages of 10 and 30. Most of the white patches initially appear on the face, hands, and feet. If they appear in isolated parts of the body, this is referred to as “localized vitiligo”. If vitiligo appears on many parts of the body and usually in large patches, this is known as “generalized vitiligo”.
Certain treatments can help partially restore pigment production.
What are the typical symptoms of vitiligo?
This skin pigmentation disorder does not normally cause any pain or discomfort. However, some people with vitiligo report experiencing itchiness when new patches of unpigmented skin are developing.
The patches of lightly pigmented or white skin stand out clearly against the remaining normally pigmented skin, in particular in people with dark skin tones. The patches are initially several millimeters to centimeters in size and oval, round, or linear in form. As the disorder progresses, individual patches may blend together to form larger areas of depigmented skin.
The white patches can appear anywhere on the body. They most commonly occur on the face (especially around the mouth and eyes) and on the hands, feet, and genital areas.
Friction may also trigger the development of patches on the neck, elbows, and ankles. Doctors refer to this effect as the Koebner phenomenon or isomorphic response.
What causes vitiligo?
The precise cause of vitiligo is unknown. A genetic predisposition may play a role, as approximately 25% to 50% of people with vitiligo have relatives with the same disorder.
How common is vitiligo?
Vitiligo is one of the most common pigment disorders. It occurs across all population groups, and affects up to 2 percent of people across the globe.
How does vitiligo progress?
Vitiligo is a chronic condition that can progress in very different ways depending on the individual case. If it begins at an early age, the disorder usually progresses more rapidly and the area affected by depigmentation spreads.
Many people with vitiligo experience inactive phases without any loss of pigmentation interspersed with active cycles of further pigmentation loss. In some people, pigment production resumes spontaneously in some areas of the skin.
Treatments can improve the pigmentation of the skin but vitiligo cannot be cured.
How is vitiligo diagnosed?
Patches of white or lightly pigmented skin are typical of vitiligo.
An in-depth consultation with a doctor will help assess the severity of the disorder. This assessment takes account of factors such as:
- age of onset (i.e., when did the symptoms first appear?)
- the spread of patches and changes in patches
- other conditions, such as autoimmune diseases
- contact with chemicals or radiation
- any medication the patient is taking
- vitiligo and other autoimmune diseases in the family
Doctors use a Wood’s lamp/light to detect vitiligo. This instrument emits a certain type of UVA light that enables the detection of otherwise invisible changes in skin pigmentation.
How is vitiligo treated?
If the pigmentation disorder progresses rapidly, anti-inflammatory steroids are normally used to treat it. These are intended to slow the spread of the patches and can be used on their own or in combination with light therapy using UVB rays.
Unpigmented skin is very sensitive to sunlight and does not tan, which means that it cannot protect itself from burning. Creams or spray with a high UVA and UVB light protection factor can replace the skin’s own self-protection, while also preventing skin cancer. The skin can also be protected from excessive exposure to sunlight by wearing long clothing or special clothing with UV protection during the summer.
Important: If there are any accompanying diseases (co-morbidities), such as a chronic inflammation of the thyroid gland (known as Hashimoto’s disease or Hashimoto’s thyroiditis), these must be treated also.
How to cope better with everyday life – what can help?
People with vitiligo often feel stigmatized. Some children are teased or even bullied in school because of their appearance. These experiences can damage self-esteem, affect quality of life, and, in some cases, lead to psychological problems. Psychological counseling and support can be beneficial in such cases.
Some people also find it helpful to use camouflage make-up products to conceal their patches – especially on the face.
- Ahmed jan N, Masood S. Vitiligo. 2020 Aug 10. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan–. PMID: 32644575. Aufgerufen am 23.01.2021.
- DynaMed (Internet), Ipswich (MA). Vitiligo. EBSCO Information Services. 2018 (1995). Record No. T116389. Aufgerufen am 23.01.2021.
- UpToDate (Internet). Vitiligo: Management and Prognosis. Wolters Kluwer 2020. Aufgerufen am 23.01.2021.
- UpToDate (Internet). Vitiligo: Pathogenesis, clinical features, and diagnosis. Wolters Kluwer 2020. Aufgerufen am 23.01.2021.
- Whitton ME, Pinart M, Batchelor J et al. Interventions for vitiligo. Cochrane Database of Systematic Reviews 2015, Issue 2. Art. No.: CD003263. DOI: 10.1002/14651858.CD003263.pub5. Aufgerufen am 23.01.2021.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: