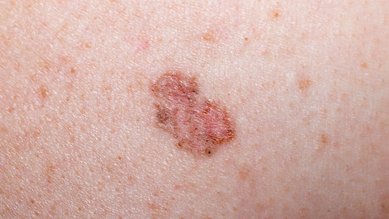
Conditions Melanoma skin cancer
ICD codes: C43 What are ICD codes?
Melanoma skin cancer is a malignant tumor that originates in the skin. Medical practitioners often refer to it as malignant melanoma. If detected early, melanoma skin cancer usually responds well to treatment. This article offers an overview of risk factors, symptoms, diagnosis, and treatment options.
At a glance
- Melanoma skin cancer is also known as malignant melanoma or simply melanoma.
- Excessive exposure to sunlight or ultraviolet (UV) light can increase the risk of developing melanoma.
- People with fair skin or a very large number of moles on their skin are at an increased risk of developing the disease.
- New or changed pigmented moles may indicate the presence of melanoma.
- Melanoma skin cancer usually responds well to treatment if detected early.
- The main objective of treatment is to remove the tumor entirely.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is melanoma?
Medical practitioners use the term melanoma skin cancer to describe a malignant skin tumor that originates in the skin cells that produce pigment. The medical term for these cells is “melanocytes”. Melanocytes give skin its color. Melanoma skin cancer is also known as malignant melanoma.
In very rare cases, melanoma can also develop in other areas of the body, such as the eyeball or the mucous membranes lining the mouth or anus.
Melanoma skin cancer metastasizes (i.e., spreads to other parts of the body) much more frequently than non-melanoma skin cancer.
What are the symptoms of melanoma?
Melanoma skin cancer can vary greatly in its appearance. In most cases, it is indicated by the occurrence of a new pigmented mole (liver spot or mole) or a change in the appearance of an existing one. A melanoma mole appears as an irregular patch of changed skin, which may have shades of brown, red, blue, or black. Some parts of the melanoma may also be colorless (non-pigmented). There are also some melanomas that completely lack any pigment.
Melanoma skin cancer may grow slowly in the surface layers of the skin but may also grow very rapidly and down into the deeper skin layers.
Signs that may indicate the presence of melanoma:
- a new pigmented mole
- changes in an existing pigmented mole (e.g. changes in size or color)
- a pigmented mole with an irregular shape or a blurred, scalloped, or notched edge
- a pigmented mole that itches or bleeds
- swollen or red skin surrounding a pigmented mole
- a pigmented mole that has a different appearance to all other moles on the body may also be a melanoma
Melanoma skin cancer can develop on any part of the skin, including the scalp, mucous membranes, and the skin under the finger- and toenails. Malignant melanoma can also occur on parts of the body that are not overly exposed to the sun.
This type of skin cancer does not initially cause symptoms such as pain. However, such symptoms may occur if the skin tumor metastasizes. A wide range of symptoms may occur, depending on the part of the body to which the cancer has spread.
What increases the risk of developing melanoma skin cancer?
The most important controllable risk factor for developing melanoma is exposure to ultraviolet (UV) radiation. This UV light may come from the sun or from a tanning lamp or tanning bed.
In particular, exposure to an extremely high dose of UV radiation for a short period of time increases the risk of developing melanoma. This includes, for example, sunburns during childhood and adolescence. In other words, melanoma skin cancer is more likely to occur in people who have been exposed to strong UV radiation for short periods as a child or teen and suffered severe sunburn as a result.
The risk of developing melanoma skin cancer may be increased in individuals who have:
- fair skin
- a large number of moles
- close family members with melanoma
If an individual has already had melanoma skin cancer, the risk of developing another melanoma is increased.
How common is melanoma skin cancer?
In 2016, around 23,000 people were newly diagnosed with melanoma skin cancer in Germany. Roughly speaking, equal numbers of women and men are affected.
The number of patients with melanoma skin cancer has been steadily rising over recent years. This may be due to the fact that more people with fair skin are being exposed to intense sunlight without protection. On the other hand, malignant melanoma is being increasingly detected at an early stage – possibly due to the skin cancer screening program.
What is the outlook for melanoma skin cancer?
Ein Melanoma in situ entspricht dem Tumorstadium 0. In diesem Stadium sind die entarteten pigmentbildendenden Zellen (Melanozyten) noch auf die Oberhaut (Epidermis) begrenzt. Sie können sich zu Krebs entwickeln und in das umgebende Gewebe ausbreiten.
Melanoma skin cancer can occur in various forms, which differ in terms of the rate at which they grow. Some melanomas grow slowly in the surface layers of the skin, while others spread very rapidly, and may grow into the deep skin layers.
As long as the altered cells grow only on the outer layer of the skin (epidermis), this is referred to as a melanoma in situ. A melanoma in situ does not metastasize, i.e., spread to other parts of the body. However, it can become an invasive melanoma that grows into the deep skin layers.
Once it invades these deeper layers, it can also metastasize. Tumor cells can spread throughout the body by means of the lymphatic system or blood vessels.
How can melanoma skin cancer be prevented?
Exposure to intense ultraviolet (UV) light increases the risk of developing melanoma skin cancer. Therefore, it is important to ensure adequate protection against overexposure to sunlight and UV radiation and avoid sunburn. This includes avoiding use of tanning beds.
As with all other types of cancer, there is no completely failsafe method of protecting oneself against melanoma. The disease can still develop in an individual who has avoided or minimized all known risk factors.
The following measures help to protect you against excessive UV radiation:
- During the summer in particular, avoid strong sunlight between the hours of 11 am and 3 pm.
- Move into the shade or under a parasol, especially around midday Note: Even in the shade, the skin is still exposed to a small amount of UV radiation.
- Wear UV-protective clothing and sunglasses as well as a hat.
- Use plenty of sunscreen on any uncovered areas of the body.
- Do not use solariums.
Parents should take care to protect their children particularly well. Furthermore, people who work outdoors should follow their company’s sun protection measures.
The Federal Office for Radiation Protection (Bundesamt für Strahlenschutz) provides a forecast of the intensity of the UV radiation to be expected from the sun in Germany over the coming days.
Would you like to know more about UV rays and how to protect yourself from them? You can find detailed information about UV radiation and sun protection on the website of the Cancer Information Service of the German Cancer Research Center (in German).
What screening options are available for skin cancer?
The earlier melanoma skin cancer is detected, the better the chances are that the patient will make a recovery.
In Germany, anyone aged 35 and over and covered by statutory health insurance is entitled to a skin cancer screening every 2 years. This skin cancer screening is part of the statutory cancer screening program.
During the screening, a specially trained doctor examines all of the individual’s skin and mucous membranes.
Everyone should also check their own skin on a regular basis. Any suspicious changes should be checked by a dermatologist.
The ABCDE rule helps you to detect suspicious pigmented moles during self-examination.
During a screening, the ABCDE rule is applied, whereby a skin change is considered to be of concern if it:
- A: is asymmetrical
- B: has an uneven border
- C: has a range of different colors
- D: has a diameter greater than 5 millimeters
- E: has evolved, i.e., the pigmented mole has changed in any way
Would you like to find out more about skin cancer screening? The website of the Cancer Information Service of the German Cancer Research Center provides more information (in German).
How is melanoma skin cancer detected?
In most cases, doctors detect melanoma skin cancer based on the external appearance of the skin when examined with the naked eye. A reflected-light microscope (dermatoscope) can help them to examine the affected area of the skin in greater detail.
If it is suspected that the patient has a melanoma, the suspicious area of the skin is usually removed in its entirety. Some of the tissue around the affected area is also removed. The sample is then examined under a microscope in the lab to determine whether melanoma skin cancer is present.
If malignant melanoma is diagnosed, the doctor can use further tests to determine whether the cancer has already spread. For example, nearby lymph nodes are often removed and tested for the presence of cancer cells (sentinel lymph node biopsy). An ultrasound scan and a magnetic resonance imaging (MRI) or computed tomography (CT) scan may also be required, in addition to laboratory testing.
Would you like to know more about testing methods, such as sentinel lymph node biopsy, ultrasound, or computed tomography? You can find detailed information about these on the German Cancer Research Center’s Cancer Information Service website.
How can melanoma skin cancer be treated?
With melanoma skin cancer, the main objective of treatment is to remove the tumor entirely. When doctors suspect that a patient has melanoma, they will remove the suspicious area of tissue in its entirety (biopsy). This will then be examined under a microscope to determine whether malignant melanoma is present. If it turns out that the skin change is indeed due to melanoma skin cancer, the doctor will perform a second operation to remove additional tissue around the site of the first operation.
For very small tumors, one operation is usually sufficient. In such cases, no further treatment is required.
If the tumor is at least 1 millimeter wide, the doctor will also remove the lymph nodes in the vicinity of the melanoma. These lymph nodes are examined to determine whether they contain tumor cells (sentinel lymph node biopsy). If the sentinel lymph nodes contain a certain number of tumor cells, the doctor will remove all lymph nodes in the affected area.
The tumor’s stage of growth will determine whether additional or different treatments are necessary. The tumor stage is determined by:
- the size of the tumor
- possible ulceration
- metastases in nearby lymph nodes or on adjacent areas of the skin
- metastases in distant organs
If an operation is not possible or if the skin cancer has already spread, radiation therapy may be useful.
Various drugs may also be considered, depending on the type and stage of the tumor. In some cases, these drugs are administered in addition to surgery at an early stage of the disease, for example, if the melanoma is large. Doctors refer to this treatment as adjuvant therapy. It objective is to improve the chances of recovery.
Video How is cancer treated?
The video below explains how cancer can be treated.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
Treatment of advanced melanoma skin cancer
Even if the skin cancer is at an advanced stage, special drugs are available to treat patients. This is the case, for example, if the tumor cannot be completely removed and has already spread to other organs. Treatment aims to stop the progression of the disease and alleviate symptoms.
The drugs that can be administered to a patient depends on the properties of the tumor and whether and how the tumor has been treated. Some drugs are only used in combination with others.
If the tumor cells have specific features, targeted therapy drugs can be used to treat melanoma skin cancer. These suppress the growth of tumor cells and can prevent the disease from progressing further.
Patients with melanoma skin cancer may also be treated with a type of immunotherapy known as immune checkpoint inhibitors. The medication binds to specific docking sites on the body’s own defense cells and stimulates these to fight the cancer cells directly.
If none of these drugs can be administered or if treatment with these drugs proved unsuccessful, chemotherapy is another option.
Video What are targeted cancer therapies?
The video below explains when targeted cancer therapies are used. How are these drugs used and how do they work?
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
In addition to the desired effects of the treatment options mentioned above, cancer treatments also have side-effects. Visit the Cancer Information Service of the German Cancer Research Center’s website for a detailed description of the treatment options described above, their side effects, and possible supportive measures (in German).
Rehabilitation following skin cancer treatment
Cancer treatment can be both mentally and physically exhausting. Medical rehabilitation (rehab) after cancer therapy aims to help patients return to their normal daily lives. Rehab is also designed to prevent or alleviate the effects of the illness and its treatment.
Rehab measures are tailored to the specific needs of patients with melanoma skin cancer.
On one hand, rehab should improve physical discomfort and impairments. Possible measures include physiotherapy exercises, muscle-building, lymph drainage, or compression bandages.
Other rehab measures assist patients with handling their cancer diagnosis and managing possible effects on their mental health, such as anxiety or depression.
Further information about rehabilitation after oncological illnesses can be found on the German Cancer Research Center’s Cancer Information Service website (in German).
Melanoma skin cancer: What happens after treatment?
Melanoma skin cancer may recur even after it has been treated successfully. Aftercare aims to detect and treat possible relapses at an early stage.
Experts recommend that patients with melanoma attend follow-up appointments on a regular basis for a period of 10 years. Those with tumors at a more advanced stage will need to be seen more frequently.
At each follow-up appointment, the doctor examines all of the patient’s skin, the site of the operation, lymphatic drainage areas, and adjacent lymph nodes. For patients with melanoma at a very early stage, this examination is sufficient. For all other patients, additional tests may be performed, such as a blood test or ultrasound scan.
Those who have recovered from melanoma skin cancer should also examine themselves regularly.
Living with melanoma skin cancer
Skin cancer patients – and indeed everyone else – should protect themselves from overexposure to the sun and examine themselves regularly. If an individual has already had melanoma skin cancer, the risk of developing another melanoma is increased. Those affected should also be sure to attend follow-up appointments with their doctor. This means that any new or recurring carcinomas can be detected at an early stage.
Points of contact for more information about melanoma skin cancer
Hospitals that are particularly experienced in treating patients with skin cancer can demonstrate this through certification. The German Cancer Society (DKG) regularly checks their compliance with certain professional requirements.
You can find the addresses of the certified centers on the OncoMAP website.
You can also search for dermatology clinics in Germany on the homepage of the German Dermatological Society.
Do you have further questions about dealing with the condition in everyday life and additional support options? You can find information about this on the website of the Cancer Information Service of the German Cancer Research Center (in German).
You can also contact the Cancer Information Service directly with any questions about melanoma skin cancer on freephone 0800 420 30 40 or by e-mail at krebsinformationsdienst@dkfz.de.
- Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF. Leitlinienprogramm Onkologie. Diagnostik, Therapie und Nachsorge des Melanoms. Langversion 3.2. S3-Leitlinie. AWMF-Registernummer 032/024OL. 10.2019.
- Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF. Prävention von Hautkrebs. Langversion 2.0. S3-Leitlinie. AWMF-Registernummer 032/052OL. 03.2021.
- Zentrum für Krebsregisterdaten (ZfKD) des Robert-Koch-Instituts (RKI). Malignes Melanom der Haut. Aufgerufen am 19.05.2020.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at: