Conditions Animal allergy
ICD codes: T78.4 What are ICD codes?
A runny or stuffy nose and sneezing when in contact with an animal can be signs of an allergy. It isn’t the fur that triggers an allergic reaction, it’s proteins that are found in the animal’s dander (flakes of skin), sweat or saliva.
At a glance
- It isn’t the animal’s fur that triggers an allergic reaction, it’s proteins that are found in an animal’s dander (flakes of skin) or saliva, for instance.
- The allergens enter the body through the airways or through direct physical contact.
- This usually causes allergic rhinitis with a runny or stuffy nose and sneezing.
- After some years, this can possibly develop into asthma.
- Even people who don’t have pets can develop an animal allergy.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is an animal allergy?
When people start sneezing or get a runny nose when they’re around cats or dogs, they often say that they’re allergic to the animal’s fur. But it isn’t the fur that triggers an allergic reaction. Instead, it’s proteins that are found in the animal’s dander (flakes of skin), sweat, skin oil, saliva (spit), urine and feces that trigger the allergy, known as allergens.
They stick to the animal’s fur and end up on objects like carpets or upholstered furniture. But particles with the protein on them also float through the air and spread in that way. The allergens enter the body through the airways or through direct physical contact.
Video What is an allergy?
The video below explains what can trigger an allergy and what symptoms can occur.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What are the symptoms of an animal allergy?
Most people usually develop the typical allergy symptoms immediately after coming into contact with the allergen. Respiratory symptoms (affecting the airways) are the most common. They occur when people breathe in small particles containing the allergen. This usually causes a runny or stuffy nose and sneezing. After several years, allergic rhinitis can develop into asthma.
Animal allergens can also make people’s eyes water and itch. Hives (nettle rash) and skin rashes may occur too, but they are less common.
Which animals cause allergies?


Many different animals are known to cause allergies when people come into contact with them. The ways in which the allergens spread also vary. These are the animals that are most likely to cause allergies, and how the allergens are spread:
- Cats: fur, saliva
- Dogs: fur, saliva
- Guinea pigs: urine
- Horses: hair
- Birds: feathers, excretions
Farm animals such as cattle, sheep and chickens can cause allergies too.
The allergens can also be spread through animal fur or tiny particles in the air on objects like mattresses, upholstered furniture, carpets, rugs and clothes.
This means that allergic symptoms can also occur when there are no animals around. This is particularly true for cat allergens that remain intact for a very long time, and can still trigger allergies months or years later. So, before moving into a new home, it’s a good idea for people to find out whether the people who lived there before them had cats.
How can an animal allergy be prevented?
Important: Even those who do not have pets can develop an animal allergy. Some people have a cat allergy, for instance, even though they have never had any cats as pets. But for people at higher risk of developing allergies to animals, getting a pet could make them have pet allergy symptoms for the first time.
On the other hand, though, it is believed that living with animals may actually prevent allergies. This could have something to do with the fact that regular close contact with allergens and microbes helps the immune system to learn how to tell the difference between harmless and harmful substances.
But so far research has not been able to clearly clarify how living with animals affects the risk of allergy long-term. The risk of becoming allergic to an animal you live with can for instance depend on what kind of animal it is and how much contact you have with it.
How is an animal allergy diagnosed?
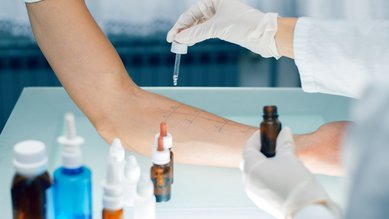
Allergy symptoms can have a range of causes including dust mites, animals and more. A medical examination helps to identify the allergen. Skin tests and blood tests are performed to see whether various allergens trigger a reaction. In a skin prick test, various potential allergens are placed on the forearm, spaced out at regular intervals. The skin is then scratched lightly at these points to allow the substances to enter the skin. If the skin turns red or itchy, the allergen has been found. In blood tests, the doctor checks whether there are antibodies to animal allergens in the blood.
In some cases, what is known as a provocation test under medical supervision might also be necessary. During this test, the membranes lining the nose or eyes (conjunctiva) are exposed to the potential allergen. The doctor then observes how the immune system responds.
How is an animal allergy treated?
The allergy symptoms can be relieved with medication. Nasal sprays and tablets for allergies can be used to treat the symptoms of allergic rhinitis. Rashes can be treated with steroid medications such as steroid creams.
For more detailed information, such as which drug treatment can be used for allergic rhinitis, visit gesundheitsinformation.de.
Allergen-specific immunotherapy (desensitization) is a treatment option also for cat allergies, among others. Immunotherapy may be considered if the symptoms are particularly severe and if contact with the animal can’t be avoided.
Those who are allergic to a certain type of animal should avoid contact with these animals. It can also be a good idea to thoroughly clean clothes and pieces of furniture or remove them. If it is the allergy sufferer’s own pet, they must consider giving up the animal. The severity of the symptoms and the treatment options play a role in the decision-making, but also their own relationship with the animal.
What else should I know?
Further information about the animal allergy condition can also be found at allergieinformationsdienst.de.
- Biedermann T, Heppt W, Renz H, Röcken M (Ed). Allergologie. Berlin: Springer; 2016.
- Brozek JL, Bousquet J, Agache I, Agarwal A, Bachert C, Bosnic-Anticevich S et al. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines – 2016 revision. J Allergy Clin Immunol 2017; 140(4): 950-958. Aufgerufen am 17.10.2024.
- Deutsche Gesellschaft für Allergologie und klinische Immunologie (DGAKI), Deutsche Gesellschaft für Kinder- und Jugendmedizin (DGKJ). Allergieprävention. S3-Leitlinie. AWMF-Registernummer 061-016. 2021. Aufgerufen am 17.10.2024.
- Trautmann A, Kleine-Tebbe J. Allergologie in Klinik und Praxis. Stuttgart: Thieme; 2022.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: