Conditions Aortic dissection
ICD codes: I71.0 What are ICD codes?
If a tear occurs in the inner lining of the body’s main artery (the aorta), blood enters the wall of the aorta, causing an aortic dissection. If this occurs close to the heart where the aorta starts, surgery must be performed as soon as possible.
At a glance
- An aortic dissection occurs when blood surges into the wall of the aorta through a tear, causing the lining of the aorta to split.
- Typical symptoms are sudden, severe pain in the chest or back, often experienced as a ripping or tearing sensation.
- Aortic dissection is rare. Two-thirds of those affected are men of middle or older age.
- If the aortic lining splits close to the heart, urgent surgery is essential.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is an aortic dissection?
If blood surges into the wall of the body’s main artery (aorta) causing the lining of the aorta to split apart, doctors refer to this as an aortic dissection or aneurysm dissecans aortae.
The wall of the aorta consists of three layers of tissue. If a tear occurs in the innermost layer, the blood may penetrate the vessel wall and cause the layers to split apart. This split (dissection) is typically associated with the sudden onset of severe pain in the chest or back.
Aortic dissection is rare but, when it occurs, it is often a life-threatening emergency. If a dissection occurs close to the heart where the aorta begins, it is particularly important that surgery be performed as soon as possible.
What are the symptoms of an aortic dissection?
An aortic dissection is typically associated with the sudden onset of severe pain in the chest or back, and occasionally in the stomach. The pain is often described as a tearing or stabbing sensation.
Other symptoms depend on the location where the dissection occurs. All possible symptoms are listed below:
- weak pulse, for example in an arm, in one of the carotid arteries in the side of the neck, or in the legs
- loss of consciousness (fainting) or impaired consciousness
- tingling, pain, or paralysis in the limbs
- hoarseness
- drooping eyelid and contracted pupils
- dyspnea (breathlessness)
What causes an aortic dissection?
An aortic dissection begins when a tear occurs in the innermost layer of the lining of the aorta. The wall of the aorta is subjected to a large amount of stress due to the fast-flowing blood and high pressure within the aorta. If the lining of the wall tears open, blood surges into it, much like a river that is diverted from its natural course.
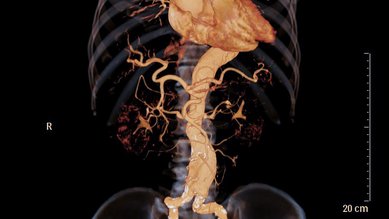
The aorta – the main artery in the body – has a shape like a wooden walking stick. It originates in the left ventricle of the heart, climbs slightly upwards and then curves in an arch before continuing downwards through the chest into the upper pelvic region.
If a rip occurs in the initial section of the aorta close to the heart or in the ascending portion, this is known as a type A aortic dissection. In this case, the surge of blood may continue into the descending portion of the blood vessel, which can cause a split along a longer section. If lining is ripped in the descending portion of the aorta only, this is known as a type B dissection.
Important: Around two-third of people who experience an aortic dissection have a type A dissection, which is the more dangerous variant.
What factors contribute to an aortic dissection?
Aortic dissection is rare. Two-thirds of those affected are men. Aortic dissection is often associated with wear and tear of the arterial wall, and mostly occurs in middle or older age. However, young adults may also experience an aortic dissection, for example if they have a genetic condition that causes changes to connective tissue.
The following underlying conditions and risk factors increase the likelihood of the lining of the aorta being damaged:
- high blood pressure and arteriosclerosis (also known as vascular calcification or hardening of the arteries)
- a sudden increase in blood pressure, e.g., when weightlifting or consuming drugs like ecstasy or cocaine
- genetic connective tissue disorders, such as Marfan syndrome or Ehlers-Danlos syndrome
- congenital heart valve defects (bicuspid aortic valve)
- a pre-existing aortic aneurysm
- previous heart surgery or catheter-based treatments
- vascular inflammation (vasculitides)
- pregnancy and birth – although the exact connection is not well understood
How does an aortic dissection progress?
In most cases, aortic dissection is an acute emergency that requires immediate action. However, there are also protracted or even chronic forms, which are less life-threatening.
The progression of this condition depends, above all, on the site and extent of the dissection and on the complications that may arise within the first couple of weeks after it occurs. An aortic rupture may occur if all layers of the aorta are torn through. This is always an emergency, which causes internal hemorrhage and, in many cases, circulatory shock.
If a type A dissection occurs close to the heart, blood may pour into the outer sac surrounding the heart (the pericardium) and put pressure on the heart muscle itself. This is referred to as cardiac tamponade (or pericardial tamponade). The aortic valve may also stop closing properly, so that blood flows back into the left ventricle of the heart. In addition, the coronary arteries may become blocked. This can result in a heart attack.
If a dissection occurs along the aorta, major side branches of the aorta may also be involved. If this causes a blockage in the carotid arteries in the neck, the patient may have a stroke. If blood flow to the renal arteries is impaired, this can result in kidney failure. In addition, blood flow to other internal organs, to the spinal cord, or to the arms and legs can be impacted.
Due to these potential complications, a type A dissection in particular is associated with a high risk, with around 50% of all patients who don’t have surgery dying as a result. However, if the aortic dissection is detected and treated quickly, around 80% of people who experience a type A dissection will survive.
How is an aortic dissection diagnosed?
Typical symptoms, such as the sudden onset of severe chest pain, provide a good indication to doctors that an aortic dissection may have occurred. The known risk factors provide further indications. If an aortic dissection is suspected, the patient must be examined in a hospital as soon as possible.
As a heart attack, which is a much more common occurrence, causes very similar pains, it must be excluded first. Most doctors will perform an electrocardiogram (ECG) for this purpose.
An aortic dissection can be diagnosed using various scanning procedures. These include:
- echocardiography: an echocardiogram is an ultrasonic technique used to examine the heart and aorta. The ultrasonic probe is often inserted into the esophagus.
- computed tomography (CT): this high-resolution x-ray procedure provides a detailed view of the heart, aorta and organs. A contrast medium can be administered in combination with the CT scan to enable a clearer view of the blood vessels. This is known as CT angiography.
- magnetic resonance imaging (MRI): this procedure is occasionally used as an alternative to computed tomography.
How is an aortic dissection treated?
If an aortic dissection occurs, doctors always administer medication immediately to relieve the pain and to bring down blood pressure and pulse rate. This relieves the pressure on the damaged arterial wall.
Further treatment then depends on the type and extent of the dissection involved:
Treatment of a type A aortic dissection
If the lining of the arterial wall splits close to where the aorta exits the heart, emergency surgery is required – and the sooner this can be done, the better the chances the patient has of surviving.
The procedure is performed as open-heart surgery, whereby the surgical team replaces the damaged section of the aorta with a vascular prosthesis, also known as a vascular implant. If the aortic valve is also affected, they replace this with a prosthetic valve.
Treatment of a type B aortic dissection
If only the descending portion of the aorta is damaged, medication is used to treat milder cases. The patient is kept in hospital to monitor the success of the treatment. In this case, an operation is only necessary if the pain and blood pressure cannot be sufficiently regulated, if the aorta is significantly enlarged and at risk of rupture, or if other complications develop. During surgery, an incision is usually made in the groin and an aortic stent graft is fed through a narrow tube called a catheter until it reaches the correct position in the aorta.
What aftercare is provided for an aortic dissection?
Following an aortic dissection, it is important to monitor blood pressure on an ongoing basis and to use suitable medication to manage blood pressure if necessary.
It is also recommended that regular checks be performed to detect late complications or, in chronic cases, to determine whether the dissection is likely to spread. It is essential to attend follow-up checks where computed tomography (CT), resonance imaging (MRI), or heart ultrasound (echocardiography) techniques are used for this purpose. These checks are initially performed at intervals of 3 to 6 months, and subsequently once a year.
- Deutsche Gesellschaft für Gefäßchirurgie und Gefäßmedizin e.V. Typ B Aortendissektion. S2k-Leitlinie. AWMF-Registernummer 004-034. 05.2018.
- DynaMed (Internet), Ipswich (MA). Thoracic Aortic Dissection. EBSCO Information Services. Record No. T113709. 2018 (1995). Aufgerufen am 27.05.2021.
- Levy D, Goyal A, Grigorova Y et al. Aortic Dissection. [Updated 2020 Dec 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Aufgerufen am 27.05.2021.
- Matthews CR, Madison M, Timsina LR et al. Impact of time between diagnosis to treatment in Acute Type A Aortic Dissection. Sci Rep. 2021 Feb 10;11(1):3519. doi: 10.1038/s41598-021-83180-6. PMID: 33568755; PMCID: PMC7876041.
- UpToDate (Internet). Clinical features and diagnosis of acute aortic dissection. Wolters Kluwer 2020. Aufgerufen am 27.05.2021.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at: