Conditions Cervical cancer
ICD codes: C53 What are ICD codes?
In the past, cervical cancer was a common type of cancer in women. As a result of screening and the timely treatment of its precursors, it has become significantly less prevalent. It is usually curable in the early stages. The HPV vaccine can prevent cervical cancer.
At a glance
- Doctors also refer to cervical cancer as cervical carcinoma.
- Since cervical cancer is typically caused by human papillomaviruses (HPV), this type of cancer can be prevented by an HPV vaccine.
- There is a national cervical cancer screening program in Germany.
- In the early stages, cervical cancer can usually be effectively treated by surgery.
- Doctors treat advanced cervical cancer with a combination of radiation and chemotherapy.
- Cancers of the genital area, like cervical cancer, often have a direct effect on sexuality.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is cervical cancer?
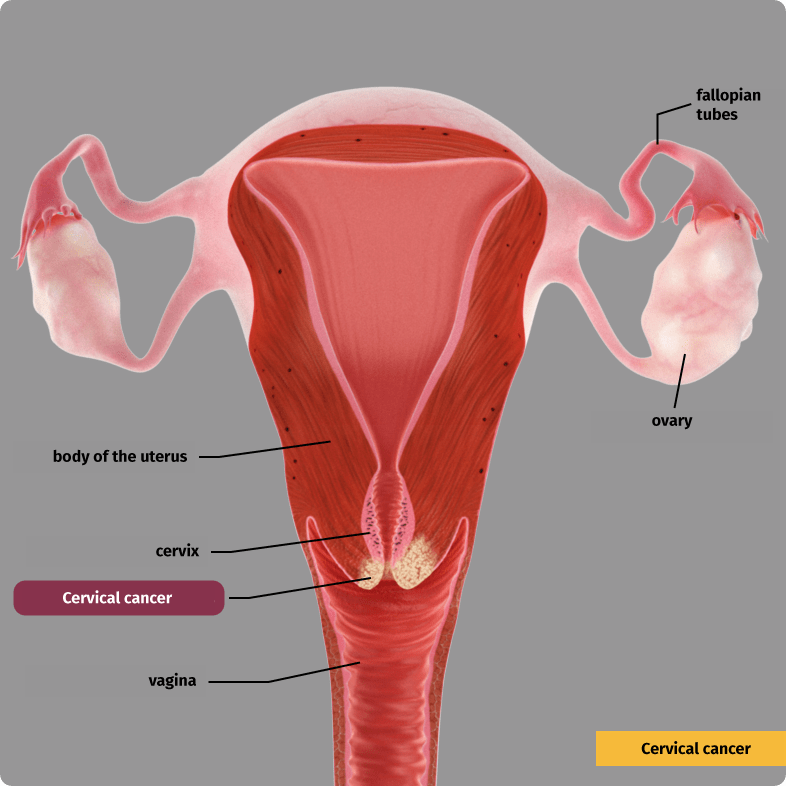
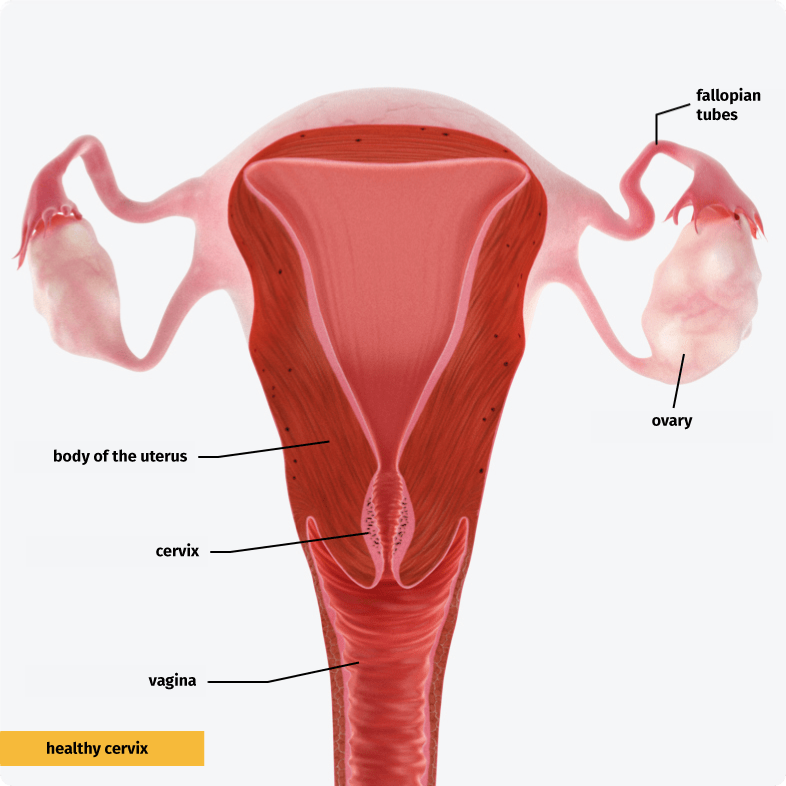
Doctors also refer to cervical cancer as cervical carcinoma. A cervical carcinoma is a malignant tumor in the lower portion of the uterus.
Cervical cancer is preceded by precursor lesions, which are primarily located in the transition zone. In the transition zone, the glandular mucosa of the cervical canal transitions into the mucous lining of the vagina. This means that the glandular cells and surface cells are adjacent in this zone.
لمحة عامة عن الأعضاء التناسلية الأنثوية الداخلية. في الدائرة، عنق رحم متضخم مصاب بالورم.
7 to 8 of 10 tumors of the cervix arise from the surface cells. These are referred to as squamous cell carcinomas. Cervical intraepithelial neoplasia (CIN) is a precursor to squamous cell carcinoma. Adenocarcinomas and their precursor (ACIS) are less common. They are comprised of abnormal glandular cells.
What are the symptoms of cervical cancer?
There are often no symptoms in the precursor stages and early stages of cervical cancer.
However, the following symptoms can indicate a cervical carcinoma:
- vaginal discharge
- bleeding after intercourse or outside of the normal menstrual cycle
In the case of advanced cervical cancer, pain in the small of the back and pelvis, pain during urination or defecation, and lymphostasis in the legs are possible.
Symptoms like vaginal discharge and pain during urination not only occur in cervical cancer but are also common symptoms of benign diseases. See a doctor if these symptoms persist for several weeks. Gynecologists can evaluate the cause of symptoms and initiate further diagnostic testing as needed.
What causes cervical cancer?
Cervical cancer is typically caused by infection with certain human papillomaviruses (HPV), i.e., the high-risk types, primarily HPV 16 and 18.
A persistent HPV infection can result in dysplasia, which is a precursor to cancer. If this dysplasia is not treated, it can develop into cervical cancer.
To learn more about the connection between human papillomaviruses and cancer, visit the website of the Cancer Information Service of the German Cancer Research Center for answers to frequently asked questions (in German).
What increases the risk for cervical cancer?
Certain risk factors can additionally increase the risk of disease. These include:
- smoking
- other sexually transmitted infections, e.g. chlamydia, herpes, and gonococcal infections
- numerous pregnancies and births
- use of birth control pills for more than 5 years
- a significantly compromised immune system
How common is cervical cancer?
In Germany, cervical cancer is the thirteenth most frequent new cancer diagnosis in women. Approximately 2 of every 100 cases of cancer in women are cervical cancer. Each year, approximately 4,400 women are diagnosed with cervical cancer.
The precursors of cervical cancer are approximately 100 times more prevalent.
Can cervical cancer be prevented?
A vaccine against human papillomaviruses (HPV vaccine) can prevent HPV infection and thus the precursors of cervical cancer. The Standing Committee on Vaccination (Ständige Impfkommission – STIKO) of the Robert Koch Institute (RKI) recommends the vaccine for girls (and boys) between the ages of 9 and 14. Statutory health insurance providers assume the cost of catch-up vaccinations to the age of 17.
Vaccination intervals for HPV vaccine: the official recommendation is to vaccinate boys and girls between 9 and 14 with two doses of the vaccine at 5 to 13-month intervals. Adolescents aged 15 to 17 inclusive need three vaccinations: the initial dose, a second dose preferably after one to two months and the third dose after 6 to 12 months.
Since the vaccine does not protect against all cancer-causing types of HPV, vaccinated women should continue to participate in the cervical cancer screening program.
Do you want to know more about the HPV vaccine? On the website of the Cancer Information Service of the German Cancer Research Center you will find answers to frequently asked questions as well as in-depth background information (in German).
How does cervical cancer progress?
If the precursors of cervical cancer are not treated, cancer can develop. The cancer cells on the surface of the cervix can infiltrate the surrounding tissue (invasive carcinoma).
In most patients, cervical cancer only spreads in the pelvis for a long time. Later, spread to neighboring lymph nodes (lymph node metastases) and other organs (distant metastases) can also occur.
Recurrence can occur as a local recurrence in the pelvis, as lymph node metastases, or as distant metastases. The rate of recurrence varies depending on prior treatment.
Is it possible to screen for cervical cancer?
In Germany, every woman over the age of 20 is eligible for free cervical cancer screening as part of the national cancer screening program.
The Pap smear is an important part of the examination. During the Pap smear, the gynecologist scrapes cells from the cervix and sends them to a laboratory. The laboratory stains the cells and examines them under a microscope.
In 2020, the screening program began offering women over the age of 35 a combined HPV test and Pap smear every 3 years instead of an annual Pap smear.
Treatment of precursors
Abnormal screening findings are sometimes clarified with additional testing, including a colposcopy examination in which a tissue sample is taken. If this test confirms the abnormal finding, the doctor can treat the dysplasia. They typically perform cervical conization, which involves the removal of a cone-shaped piece of tissue containing the dysplasia.
The website of the Cancer Information Service
of the German Cancer Research Center provides information about cervical cancer screening examinations, the advantages for patients, and any possible disadvantages (in German).
Comprehensive information about screening for cervical cancer is also provided in the patient brochure published by the Joint Federal Committee (G-BA).
How is cervical cancer diagnosed?
The gynecological examination is the first step in the diagnosis of cervical cancer. The doctor examines the lower portion of the cervix that protrudes into the vagina (ostium of uterus) and the vagina.
A spatula is used to scrape cells from the cervix and a brush is used to collect cells from the cervical canal. The doctor also palpates the vagina, uterus, and the rectum.
Depending on the finding, it may be necessary to closely examine the mucous lining of the ostium of the uterus and the vagina with a special magnifying glass (colposcopy). In the case of abnormalities, the doctor takes tissue samples (biopsy) during the colposcopy examination and/or scrapes the inside of the cervix.
A pap test involves a doctor using a spatula to scrape cells from the ostium uteri (mouth of the womb) or a small brush to scrape cells from the cervical canal.
Ultrasound examination of the internal reproductive organs via the vagina (vaginal ultrasound) and ultrasound of the kidneys are often also performed.
Additional imaging methods may be helpful to evaluate tumor spread. Magnetic resonance imaging (MRI) in particular allows the doctor to effectively evaluate the extent to which the tumor has already spread. If MRI is not an option, patients will be examined using computed tomography (CT).
The diagnosis of cervical cancer is confirmed by histological examination of tissue samples from the tumor.
How is cervical cancer treated?
When selecting the best treatment option, doctors primarily take 3 factors into account:
- Tumor stage: how advanced is the cervical cancer?
- General medical condition and life situation of the patient: does the patient have a desire to conceive? Is the patient premenopausal or postmenopausal, i.e., no longer menstruates?
- Histopathological properties of the tumor
Prior to the start of treatment, experts often recommend surgical staging to evaluate the extent to which the tumor has spread in the pelvis and whether the lymph nodes have already been affected. This surgery is usually performed on a laparoscopic basis.
Treatment options
Initial treatment of cervical cancer entails either surgery or a combination of radiation and chemotherapy, referred to as radiochemotherapy.
In the case of a tumor of the cervix, radiation therapy is performed both externally and internally (brachytherapy). For brachytherapy, the doctor inserts a stent into the cervix. During treatment, the stent is filled with radioactive material, which is then removed after the treatment session. Radiation therapy is performed externally for lymph node stations.
In the early stage
In the early stages of the disease, the tumor is limited to the uterus (and the upper portion of the vagina). In this case, doctors typically recommend surgery as the primary treatment.
- In premenopausal patients, it is possible for doctors to remove only part of the cervix in the early stages of the disease in order to preserve fertility.
- In postmenopausal women or women with no desire to conceive, doctors typically remove the uterus along with its supporting structures and parts of the vagina in the early stages. In postmenopausal women, the fallopian tubes and the ovaries are also removed.
- In younger women (premenopausal), it is possible to leave the ovaries for hormone production.
During surgery, doctors typically also remove the pelvic lymph nodes and sometimes also the lymph nodes along the aorta.
Some patients undergo supportive (adjuvant) therapy after surgery, for example, when the tumor has spread to the smallest lymphatic and blood vessels or is very large. Doctors typically use adjuvant radiochemotherapy for this purpose.
Video How is cancer treated?
The video below explains how cancer can be treated.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
If the cancer is advanced
Experts recommend combined radiochemotherapy as the primary treatment.
If the tumor has spread further into the pelvis and metastases have also developed in other distant organs (distant metastases), doctors select treatment on an individual basis depending on the particular disease situation. Usually radiochemotherapy, sometimes only chemotherapy, and more rarely complete or partial removal of the pelvic organs are considered.
To learn more about conventional treatments of cervical cancer and possible side effects and about the available treatment options in the case of advanced incurable cervical cancer, visit the website of the Cancer Information Service of the German Cancer Research Center for detailed descriptions of the various types of treatment (in German).
What is the aftercare for cervical cancer?
The goal of aftercare in women with cervical cancer is the early detection and treatment of a possible recurrence as well as aftereffects of the disease and of the treatment. A further goal is to maintain or restore the quality of life of patients.
After the end of treatment, the women are examined regularly, initially at short intervals, then at longer ones.
In the follow-up, the gynecologist asks patients about symptoms and performs a Pap smear of the vagina and cervix (if still present). Additional examinations can be performed as needed, e.g., a human papillomavirus (HPV) test or colposcopy.
How to cope with the effects of cervical cancer and its treatment?
Many patients with cervical cancer want to actively participate in their recovery. There are a number of ways they can do this. The appropriate supportive measures for coping with the disease and the treatment effects are determined on an individual basis.
- Psycho-oncological counseling can help if worry and anxiety become overwhelming.
- Removal of the uterus and the ovaries makes women infertile: consultation with the treating doctor may make it possible for younger women to conceive in spite of cancer treatment.
- Removal of the ovaries causes early menopause in younger women: supportive measures can minimize the associated symptoms.
How is sexuality affected?
Cancers in the genital area, like cervical cancer, often have a direct effect on sexuality. The disease and the necessary treatment can interfere with sexual sensation and limit sexual function.
Depending on the life situation, this can put a significant strain on the woman and her partner.
In addition to treating physicians, psycho-oncologists offering sexual therapy can provide valuable professional help. There are also health centers that offer advice.
Contacts for cervical cancer
Physicians from various disciplines work closely together to treat cervical cancer. Hospitals with significant experience treating patients with gynecological cancers like cervical cancer can become certified treatment centers. The German Cancer Society (DKG) regularly checks their compliance with certain professional requirements.
You can find the addresses of the certified centers on the OncoMAP website. Select “gynecological cancer center” under “center”.
Do you have further questions about dealing with the condition in everyday life and additional support options? Visit the website of the Cancer Information Service of the German Cancer Research Center (in German).
Contact the Cancer Information Service with any questions regarding cervical cancer under the toll-free number 0800 - 420 30 40 or per e-mail: krebsinformationsdienst@dkfz.de.
- Cibula D et al. (2018). The European Society of Gynaecological Oncology/European Society for Radiotherapy and Oncology/European Society of Pathology. Guidelines for the Management of Patients with Cervical Cancer. Virchows Arch. 2018. 472(6): 919-936. doi: 10.1007/s00428-018-2362-9. Aufgerufen am 26.06.2020.
- Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF: Diagnostik, Therapie und Nachsorge der Patientin mit Zervixkarzinom. S3-Leitlinie. Langversion 2.0. AWMF-Registernummer 032/033OL. 03.2021. Aufgerufen am 21.04.2021.
- Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF. Prävention des Zervixkarzinoms. S3-Leitlinie. Langversion 1.1. AWMF-Registernummer 015/027OL. 03.2020. Aufgerufen am 21.04.2021.
- Zentrum für Krebsregisterdaten (ZfKD) des Robert Koch-Instituts (RKI). Gebärmutterhalskrebs (Zervixkarzinom). Aufgerufen am 21.04.2021.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at: