Conditions Diabetic foot
ICD codes: E11 What are ICD codes?
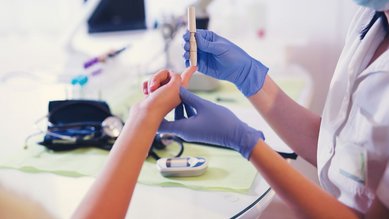
A diabetic foot can develop as a result of permanently elevated blood glucose levels. This article explains how people with diabetes can prevent it and how poorly healing wounds on the foot are treated.
At a glance
- Diabetic foot is a possible consequence of untreated or poorly monitored diabetes mellitus.
- Permanently elevated blood glucose levels can cause nerve and tissue damage.
- The first signs of a diabetic foot are dry feet and increased callus formation.
- Complications can be prevented by taking prevention measures.
- It is particularly important to care for the feet properly, wear suitable shoes, and avoid injuries.
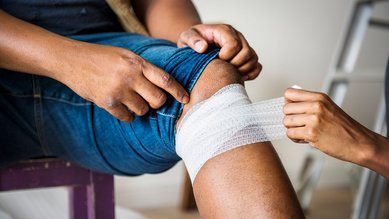
- Even minor injuries should be treated to prevent the development of chronic wounds.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is diabetic foot?
Untreated or poorly monitored diabetes mellitus can lead to permanent diabetic foot, also called “diabetic foot syndrome”. The first warning signs are dry feet and increased callus formation. Over time, this can lead to open wounds on the foot or toes that do not heal properly.
About 20 to 30 percent of people with diabetes develop a diabetic foot during their lifetime.
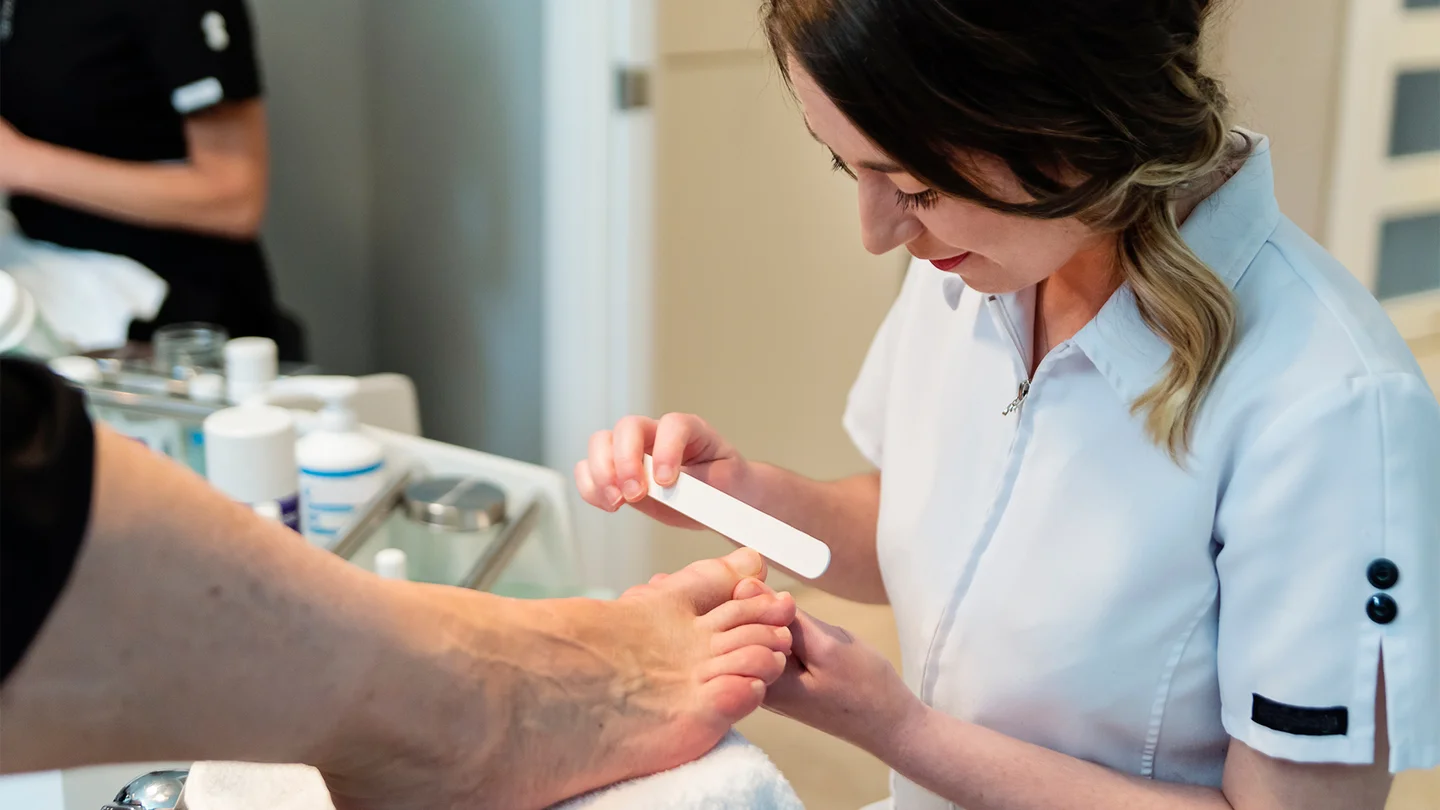
However, this does not have to happen. Good diabetes management and thorough foot care can prevent the development of chronic wounds on the feet. Doctors, relatives, caregivers, or regular medical foot care (podological treatment) can help.
What are the indications of diabetic foot?
Dry feet and increased callus formation can be the first signs of a diabetic foot. Further symptoms depend on whether nerve or vascular damage is the cause.
In the case of nerve damage, the following foot symptoms can arise:
- insensitivity to pain, pressure, cold, and heat
- numbness
- tingling
- very dry and warm skin
- wounds that heal poorly, mainly on the sole of the foot
The following symptoms are typical in the case of vascular damage:
- foot feels cool
- pale or blue skin
- extremely weak pulse
- open wounds mainly in the toes or heel
- pain in the calves when walking
What causes diabetic foot?
People with diabetes have blood glucose levels that are too high. If the blood glucose level is permanently elevated, damage to the nerves (neuropathies) and the vessels (macroangiopathies) occurs more frequently.
As a result of nerve damage, the sensation of pain is partially or completely lost. This can result in a loss of feeling of pressure points and small injuries on the feet. Often the affected areas are not spared and also not treated in time. Foot injuries can sometimes be caused by shoes that are too tight, calluses, and pressure points due to foot malpositions.
Damage to the vessels leads to poorer blood circulation in the feet. As a result, wounds heal very slowly.
What increases the risk of diabetic foot?
Some factors can cause additional damage to the vessels, and thus further worsen blood circulation in the feet and impair healing of the wound.
Risk factors are:
What are the effects of diabetic foot?
It is important to recognize and treat a diabetic foot early on. If this does not happen, a chronic wound can develop. In particular, the toes, the sole of the foot, the heel, or the ankles are often affected. This type of wound can become very deep and inflamed. Black spots in the wound indicate dead tissue. Very severe wounds may require amputation of the affected toe or part of the foot.
How can diabetic foot be prevented?
People with diabetes can do a lot to keep feet healthy. The most important factors are:
- blood sugar that is well-monitored
- shoes that fit well and do not pinch under any circumstances
- avoiding injuries and not walking barefoot
- daily foot care
- regular medical check-ups
- treatment of high blood fat values and high blood pressure
- not smoking
Pressure points and injuries to the feet can be avoided by:
- shoes that offer sufficient room
- a soft footbed
- no seams or straps that can chafe
- orthopedic custom-made shoes and adapted insoles
- repairing or replacing worn-out shoes
- shoe checks before putting them on: for example whether there is sand or stones in the shoe
In the case of pronounced foot deformities, surgery may be possible to reduce the pressure on certain areas.
Even if a wound has already formed, it is possible to prevent it from becoming chronic. And even if wounds have been present for some time already, they can be healed with careful treatment.
You can find more information about how to ensure good foot care and how to prevent wounds at gesundheitsinformation.de.
How can diabetic foot be recognized early?
People with diabetes should check their feet themselves as much as possible. A hand mirror can help to examine the soles of the feet. Minor injuries and pressure points should also be taken seriously and checked by a doctor.
If it is difficult for someone to recognize their foot problems themselves, it is important to have feet examined regularly by a doctor or at a medical foot care center. Relatives or caregivers can also look at the feet regularly and check for injuries and pressure points.
How is diabetic foot diagnosed?
To determine whether diabetic foot has developed, the doctor examines the skin. They check the temperature and the blood circulation of the foot. The sensitivity of the nerves is tested by touching the feet with a tuning fork or plastic thread. They also look for wounds, pressure points, or deformities. If a wound is discovered, the doctor examines how deep it is and whether it has become infected.
An ultrasound or imaging of the vessels (angiography) may be useful to assess the blood flow to the legs. In addition, imaging techniques such as X-ray, computed tomography (CT), or magnetic resonance imaging (MRI) may be used to detect possible bone damage.
How is diabetic foot treated?
Timely treatment of wounds is important to prevent severe tissue damage. This often prevents chronic wounds and also reduces the risk of amputation. Wounds must be completely relieved of any pressure and inflammation must be treated. It is also important to improve circulation in the leg. If there is a circulatory disorder, it can be eliminated through surgery, such as vascular dilatation or a new vessel (bypass).
The amount of time needed for a wound to heal depends on how large and how deep the wound is. Small wounds often take only a few weeks, while large or deep wounds can take months to heal. To promote healing, a skin or tissue transplant may be possible.
Sometimes amputation of toes or parts of the foot or lower leg is unavoidable. This is the case if:
- the affected area can no longer be preserved,
- the wound will never heal,
- the infection in the leg has spread, or
- pain is extreme.
Important: If amputation is recommended, it is good to be well informed and obtain a second opinion.
The decision aid from gesundheitsinformation.de can help you choose an appropriate treatment for diabetic foot.
- Bundesärztekammer. Kassenärztliche Bundesvereinigung. Arbeitsgemeinschaft der Wissenschaftlichen Medizinischen Fachgesellschaften. Nationale VersorgungsLeitlinie "Therapie des Typ-2-Diabetes". Konsequenzen für die Praxis. MMW Fortschr Med. 2014 Mar 27;156 Spec No 1(1):76-8. German. PMID: 24930352.
- Coffey L, Mahon C, Gallagher P. Perceptions and experiences of diabetic foot ulceration and foot care in people with diabetes: A qualitative meta-synthesis. Int Wound J. 2019 Feb;16(1):183-210. doi: 10.1111/iwj.13010. Epub 2018 Nov 4. PMID: 30393976.
- Elraiyah T, Prutsky G, Domecq JP, Tsapas A, Nabhan M, Frykberg RG, Firwana B, Hasan R, Prokop LJ, Murad MH. A systematic review and meta-analysis of off-loading methods for diabetic foot ulcers. J Vasc Surg. 2016 Feb;63(2 Suppl):59S-68S.e1-2. doi: 10.1016/j.jvs.2015.10.006. PMID: 26804369.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at: