Conditions Multiple myeloma
ICD codes: C90.0 What are ICD codes?
Multiple myeloma is a malignant disease that originates from plasma cells in the bone marrow. With modern therapies, the symptoms can usually be effectively treated. This article provides an overview of the symptoms, as well as the diagnostic and treatment options, of bone marrow cancer.
At a glance
- Multiple myeloma originates from plasma cells in the bone marrow.
- Therefore, it is also called plasmacytoma or bone marrow cancer.
- The myeloma cells displace healthy blood-building (hemopoietic) cells in the bone marrow and destroy the bone structure in many places.
- Anemia, frequent infections, bone pain, bone fractures, and kidney dysfunction are possible consequences of multiple myeloma.
- With appropriate treatment, symptoms of the disease often regress well.
- A permanent cure is most likely not possible with the treatments currently available.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is multiple myeloma?
Multiple myeloma is a cancer that originates from mutated plasma cells in the bone marrow. Therefore, it is also called plasmacytoma or bone marrow cancer.
Healthy plasma cells are important for immune defense because they produce antibodies that specifically target pathogens. Mutated plasma cells, on the other hand, usually produce large amounts of useless antibodies or antibody fragments. These are also called paraprotein or monoclonal immunoglobulin.
As the myeloma cells spread into the bones, they displace the normal hematopoietic cells in the bone marrow and destroy the bone structure in many places. The numerous (technical term: multiple) tumor foci in the bone marrow are typical of multiple myeloma.
Plasma cells are derived from certain white blood cells, known as B lymphocytes. For this reason, physicians classify multiple myeloma as a B-cell lymphoma.
What are the symptoms of multiple myeloma?
Onset of the disease is slow for most patients. Therefore, doctors often discover multiple myeloma as an incidental finding during a blood or urine test. Possible signs of the disease are:
- bone pain, often in the area of the spine
- fatigue, weakness, loss of performance, exhaustion
- frequent infections
- loss of appetite, nausea, unintentional weight loss
- foamy urine
- frequent urination
However, these symptoms can be present not only with multiple myeloma, but also with other diseases. If these symptoms persist over a long period of time, a visit to the doctor is recommended. General Practitioners can already narrow down what is causing the symptoms and, if necessary, initiate further diagnostic steps with specialists.
What causes multiple myeloma?
Multiple myeloma is caused by a single mutated plasma cell in the bone marrow. The exact trigger of this change is still largely unclear.
However, experts suspect that there are factors that can increase the risk of multiple myeloma. These include, for example:
- older age: the risk of developing multiple myeloma increases with age, with most patients between 70 and 80 years old.
- male sex: men are slightly more likely to develop the disease than women.
- a genetic disposition: multiple myeloma occurs more frequently in some families. However, multiple myeloma is not considered an inherited disease per se.
- other plasma cell disorders: individuals with certain other plasma cell abnormalities have a higher risk of developing the disease.
Experts discuss chronic infections, excess weight (obesity), ionizing radiation, and certain chemical substances as other risk factors.
How common is multiple myeloma?
Every year, about 7,000 people are newly diagnosed with multiple myeloma in Germany. Men are affected slightly more often than women.
Multiple myeloma primarily affects older people. Most patients are older than 70 years. Since life expectancy is increasing overall, a growing number of new cases of multiple myeloma can also be expected in the coming years.
How does multiple myeloma progress?
The course of the disease can vary greatly from patient to patient: some patients have few symptoms and live with the disease for many years, while in others it progresses rapidly. Important complications mainly affect blood formation, the bones, and the kidneys.
Blood formation disorder
If the myeloma cells spread in the bone marrow, they displace the normal blood-forming cells. This can lead to anemia, frequent infections, and an increased tendency to bleed.
Dissolution of bone
Myeloma cells destroy the bone structure. Bone pain and fractures are possible consequences. If the bone is dissolved, more calcium also enters the blood. This is called hypercalcemia and can lead to kidney problems, among other things.
Disorder of kidney function
The mutated plasma cells form useless proteins known as monoclonal immunoglobulins. They are excreted through the kidneys and can lead to kidney damage and kidney dysfunction.
As of today, multiple myeloma is not considered curable. However, with the therapies available today, the disease can often be effectively treated while maintaining a good quality of life for patients. The type of treatment and the response of the myeloma cells to treatment determine how the disease progresses.
Assessing the progression: prognostic markers
Prognostic markers help doctors distinguish between patients with a more favorable progression and patients with a more unfavorable progression. To this end, they check factors such as the
- protein levels in the blood serum (beta-2-microglobulin, albumin)
- lactate dehydrogenase (LDH) value in the blood serum
- myeloma cells, for certain genetic alterations
How is multiple myeloma diagnosed?
If multiple myeloma is suspected, the doctor will perform various tests. These include:
- a physical examination
- a blood and urine test
- taking a tissue sample from the bone marrow (biopsy)
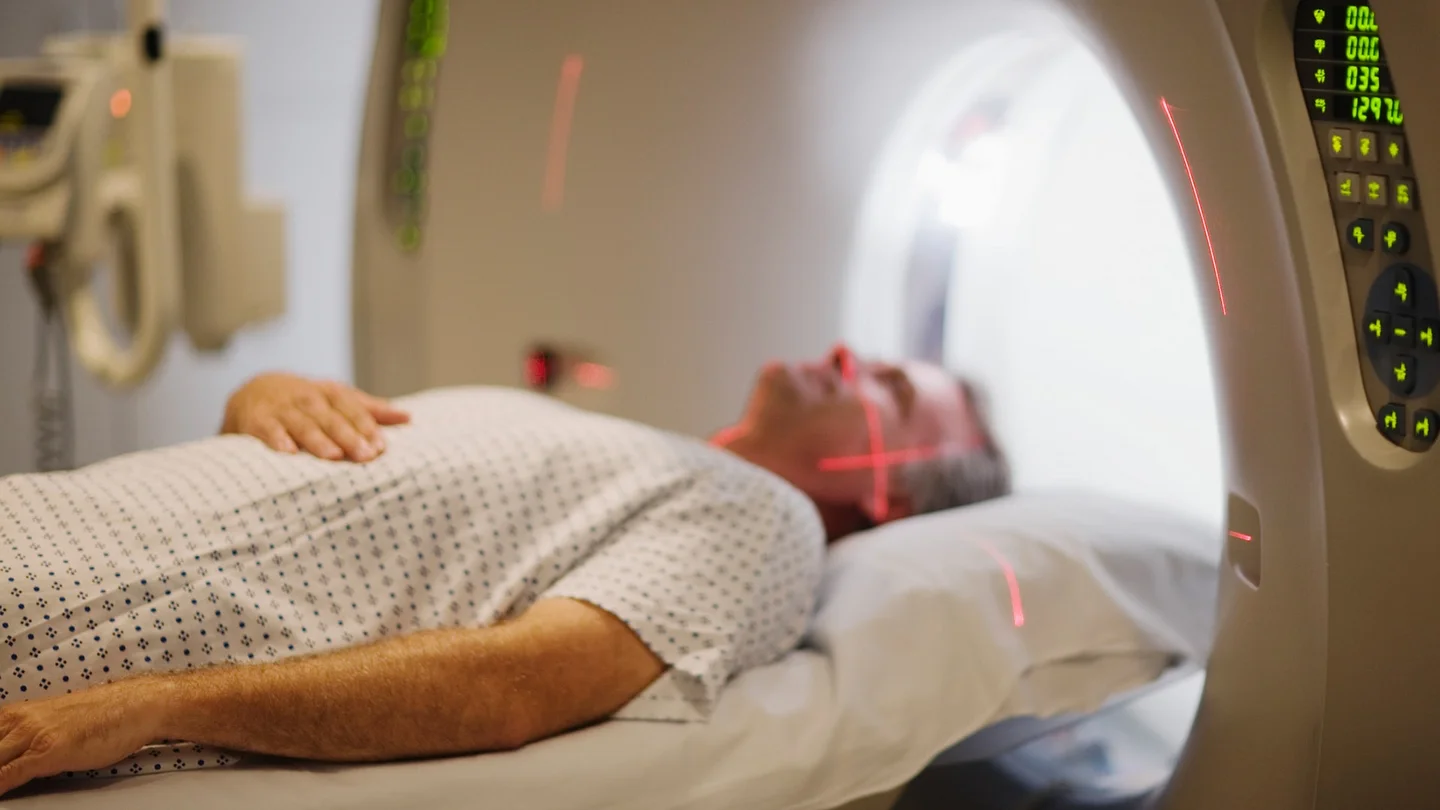
- imaging: full-body computed tomography (CT), full-body magnetic resonance imaging (MRI) and positron emission tomography (PET) if necessary
This allows physicians to make a diagnosis, assess the extent of the disease, and evaluate further disease progression.
Blood and urine tests
Doctors can detect characteristic antibodies known as paraproteins in the blood and urine. A blood test helps doctors determine the extent to which normal blood formation and kidney function are impaired. The concentration of certain proteins in the blood provides information about the further progression of the disease.
Biopsy
The percentage of mutated plasma cells is determined in the bone marrow sample, and plasma cells are examined for genetic alterations.
Imaging
Full-body computed tomography (full-body CT) provides information about the extent of the disease and the stability of the bones. Magnetic resonance imaging (full-body MRI) can help estimate to what extent bone marrow is affected.
How is multiple myeloma treated?
Experts recommend that treatment for multiple myeloma should always begin once organ damage is already present or imminent. Different treatment approaches are available for this purpose. Doctors consider three main factors when choosing the appropriate form of treatment:
- symptoms
- extent of the disease
- patient’s general state of health
Treatment is constantly changing due to new, highly effective medications. Patients with multiple myeloma should therefore seek treatment in clinical trials whenever possible.
Important: Multiple myeloma therapy requires special expertise. Treatment should therefore be carried out in close consultation with a specialized center or specialized physicians.
Drug therapy
Multiple myeloma usually affects several parts of the body. Therefore, treatment must target the entire body. Experts refer to this as systemic therapy.
Various drugs and drug combinations can be used for this purpose. In addition to chemotherapy, cortisone and immunomodulatory medication, doctors also use targeted drugs. A new form of therapy is treatment with the patient’s own genetically modified immune cells, known as CAR T-cell therapy.
Video What are targeted cancer therapies?
The video below explains when targeted cancer therapies are used. How are these drugs used and how do they work?
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
Stem cell transplant
A stem cell transplant is considered in patients with a good general state of health. High-dose chemotherapy is usually followed by the transplant of the patient’s own blood stem cells (autologous stem cell transplantation). This intensive treatment can cause a long-lasting regression of disease symptoms, known as remission.
In some cases, transplanting blood stem cells from another person is also possible (allogeneic stem cell transplantation).
Following the stem cell transplant, patients are generally administered further medication. Known as maintenance therapy, this aims to solidify the success of the treatment and slow the progression of the disease.
Local treatment
In certain situations, localized treatment may be useful for multiple myeloma. For example, this is the case when myeloma foci do not respond to systemic therapy and cause pain or threaten bone stability. In such cases, the myeloma foci are often targeted with radiation.
Supportive drugs
Myeloma cells produce substances that activate bone-degrading cells in the bone, so called osteoclasts. Bisphosphonates and the antibody denosumab reduce osteoclast activity and can stabilize the bone. They reduce the risk of bone fractures and bone pain.
What happens after treatment?
After treatment, regular check-ups serve to detect and treat side effects from the treatment and relapses as early on as possible. The attending physicians determine which check-ups are necessary and at what intervals.
Do you want to know more about the process and side effects of chemotherapy, blood stem cell transplants, or radiation? The website of the Cancer Information Service of the German Cancer Research Center provides interesting information about the effects and side effects of the above-mentioned treatment procedures (in German).
Who supports patients after a diagnosis of multiple myeloma?
After the diagnosis of multiple myeloma, patients and their relatives face the challenge of adjusting to a new life and dealing with impacts and worries.
Physical performance can often be improved with the help of rehabilitation.
Psycho-oncological support is available to patients and their relatives by contacting the psycho-oncological center in hospitals or from private practice psycho-oncologists.
For advice on socio-legal issues, such as living costs, rehabilitation or the occupational situation, those affected can also contact the hospital social services or the regional cancer counseling centers.
Support groups also offer extensive information and assistance.
Where is more information available?
Points of contact for clinical trials are the German Study Groups in the Competence Network Malignant Lymphomas (KML): the German Study Group for Multiple Myeloma (DSMM), and the German Speaking Myeloma Multicenter Group (GMMG). Contact details can be found on the internet at the Competence Network Malignant Lymphomas website.
Multiple myeloma should be treated by a team of experienced doctors from a number of different specialties. Hospitals that are particularly experienced in the treatment of patients with lymphomas such as multiple myeloma can become certified as oncology centers specializing in “hematological neoplasms”. The German Cancer Society (DKG) checks compliance with certain professional requirements.
You can find addresses of centers with this designation on the OncoMAP website. To do this, select “Hematological Neoplasms” in the search panel under “Centre”.
- Leitlinienprogramm Onkologie (Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF): Diagnostik, Therapie und Nachsorge für Patienten mit monoklonaler Gammopathie unklarer Signifikanz (MGUS) oder Multiplem Myelom, Langversion 1.0, 2022, AWMF-Registernummer: 018/035OL Aufgerufen am 10.03.2022.
- European Hematology Association (EHA) / European Society for Medical Oncology (ESMO): Dimopoulos MA et al. (2021) EHA-ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 32(3):309-322. doi: 10.1016/j.annonc.2020.11.014.
- Wörmann B, Driessen C, Einsele H, Goldschmidt H et al. Multiples Myelom. Leitlinie der Deutschen Gesellschaft für Hämatologie und Medizinische Onkologie e.V. (DGHO). 05.2018. Aufgerufen am 18.06.2020.
- Zentrum für Krebsregisterdaten (ZfKD) des Robert Koch-Instituts (RKI). Multiples Myelom. Aufgerufen am 20.04.2022.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at:

