Conditions Ringworm
ICD codes: B35.4 What are ICD codes?
Ringworm can normally be identified by the typical circular skin rash that it causes. It is triggered by an infection with filamentous skin fungi. The infection can be effectively treated by applying anti-fungal ointment to the skin.
At a glance
- Ringworm (tinea corporis) is an inflammatory skin condition.
- It is caused by an infection with filamentous fungi that live on the skin.
- It is transmitted by means of direct contact with an infected person or pet.
- Indirect transmission via unclean objects or clothing is also possible.
- A typical sign of ringworm is a ring-shaped skin rash that appears on the torso, arms, legs and face and is often itchy.
- In most cases, the infection can be effectively treated with ointments containing anti-fungal agents.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is ringworm?
Ringworm – also referred to by medical professionals as tinea corporis – is a moderately contagious fungal infection of the skin. It is caused by an infection with various types of filamentous skin fungi.
It typically causes a circular or ring-shaped rash that particularly appears on the torso, arms, legs and face and is often itchy.
Ringworm is usually treated by applying anti-fungal (antimycotic) ointment to the skin. Doctors refer to this type of external treatment as “topical application”.
What are the symptoms of ringworm?
After contracting an infection with skin fungi, it takes approximately 2 to 4 weeks before the first changes on the skin become noticeable.
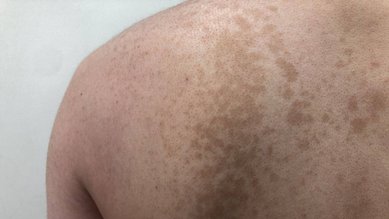
Ringworm is usually identified by the circular red patches it causes to develop on the skin, with paler patches toward their center. The edge of the circle is often slightly thickened and scaly. Smaller red patches and pimple-like sores also appear on the skin.
These skin changes are between 1 and 5 centimeters in size and are often itchy. The fungal infection frequently spreads across the stomach, back, arms, legs and face.
What causes ringworm?
Ringworm is caused by an infection of the skin with filamentous fungi. Medical professionals call these fungi dermatophytes.
Various types of skin fungi can trigger the skin rash that is typical of ringworm. They live on the outermost layer of the skin, where they feed on a horny substance called keratin.
Skin fungi can be spread by close contact with people or animals, such as cats and dogs.
It can also be picked up from unclean surfaces, gym mats, clothing, towels or bed linen.
A localized fungal skin infection can also spread from the feet, for example, to other parts of the body.
Skin fungi thrive in warm, moist environments. For this reason, infections are often picked up in swimming pools or changing rooms. Skin fungi also multiply very effectively on sweaty skin.
What factors increase the likelihood of catching ringworm?
Skin fungi find it particularly easy to multiply on the skin of someone with a pre-existing condition that affects the immune system.
Older people are also at an increased risk of developing a skin infection because their immune system no longer works as well as in younger people.
If people frequently visit gyms, swimming pools or communal changing rooms, their risk of infection is similarly higher.
How high is the risk of infection?
The risk of infection is only moderately high.
For example, if a child attending school is infected with ringworm, the risk of other children in the class becoming infected is less than 10 percent.
The risk of infection spreading within the family is around 10 to 30 percent.
How common is ringworm?
In industrialized western countries, around 10 to 20 percent of the population will develop a ringworm infection at some point in their lives.
What is the outlook for ringworm?
Ringworm can normally be treated effectively with external (topical) skin ointments.
In some cases, the condition worsens because the skin fungi become established deep in the hair follicles. If this happens, small nodules appear on the skin, either on their own or around the rash patches. This can occur, for example, in people whose immune system is suppressed due to medication they are taking.
If treated with an anti-inflammatory cream containing cortisone, the typical skin rash disappears but the skin fungi continue to spread. In this case, various atypical skin reactions may occur that are barely visible to the naked eye.
Sometimes, ringworm spreads to skin folds or other moist areas of the skin. Bacterial infections may occur there also.
Sometimes, a fungal skin infection causes an allergic reaction of the skin in a completely different part of the body. This is frequently accompanied by blisters and itching. Allergic skin reactions clear up once the fungal infection has been treated successfully.
How is ringworm diagnosed?
The symptoms that ringworm causes on the skin are often so typical that doctors can identify a fungal infection at a glance.
If the doctor wants to pinpoint which type of fungus is causing the infection, they can take a small scraping of skin from the edge of the rash. This sample can then be examined under a microscope or using a special laboratory test.
If there are atypical skin reactions or a persistent rash, it may be necessary to take a biopsy, i.e. a tissue sample.
How is ringworm treated?
In most cases, the infection clears up if the affected areas of the skin are treated with an anti-fungal ointment.
When applying the ointment, it’s important to also cover the surrounding healthy skin about 2 cm beyond the rash itself. Once the skin has regained its normal appearance, treatment should be continued for another week. Otherwise, the fungal infection may recur. The skin on which the rash appears should be kept as dry as possible.
Important: Ointments containing cortisone may make a fungal skin infection worse and should therefore not be used to treat a fungal infection. Anti-fungals containing the active ingredient nystatin are not effective against ringworm.
If the ringworm infection is particularly severe, affects several skin regions at the same time or has penetrated the deeper skin layers, doctors will prescribe anti-fungal tablets. If the skin becomes very scaly, keratolytic preparations can be applied locally to the affected areas to break down the outer layers.
How does ringworm impact everyday life?
As ringworm is only moderately contagious and can be effectively treated, infected children can continue to attend school and kindergarten/pre-school.
People with ringworm who play contact sports without protective clothing should avoid training with others for one week.
- DynaMed, Ipswich (MA). Tinea corporis. EBSCO Information Services. 2018 (1995). Aufgerufen am 23.11.2021.
- UpToDate. Dermatophyte (tinea) infections. Wolters Kluwer 2021. Aufgerufen am 23.11.2021.
Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: