Conditions CUP syndrome (cancer of unknown primary)
ICD codes: C76 C80 What are ICD codes?
CUP syndrome is an unusual form of cancer, in which doctors detect secondary tumors around the body, known as metastases. However they do not find the tumor of origin. This is why it’s called CUP or cancer of unknown primary.
At a glance
- In CUP syndrome metastases are found in the body but the primary tumor is not.
- This is an advanced form of cancer where the cancer has already spread (“metastasized”).
- The causes and risk factors for CUP syndrome are largely unknown.
- The symptoms and progression depend on where the cancer cells originated and where they have metastasized to.
- One diagnostic approach involves histological examinations of tissue to identify the primary tumor.
- In most cases, CUP syndrome cannot be cured; treatment is on an individual basis and is aimed at alleviating symptoms and maintaining quality of life.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
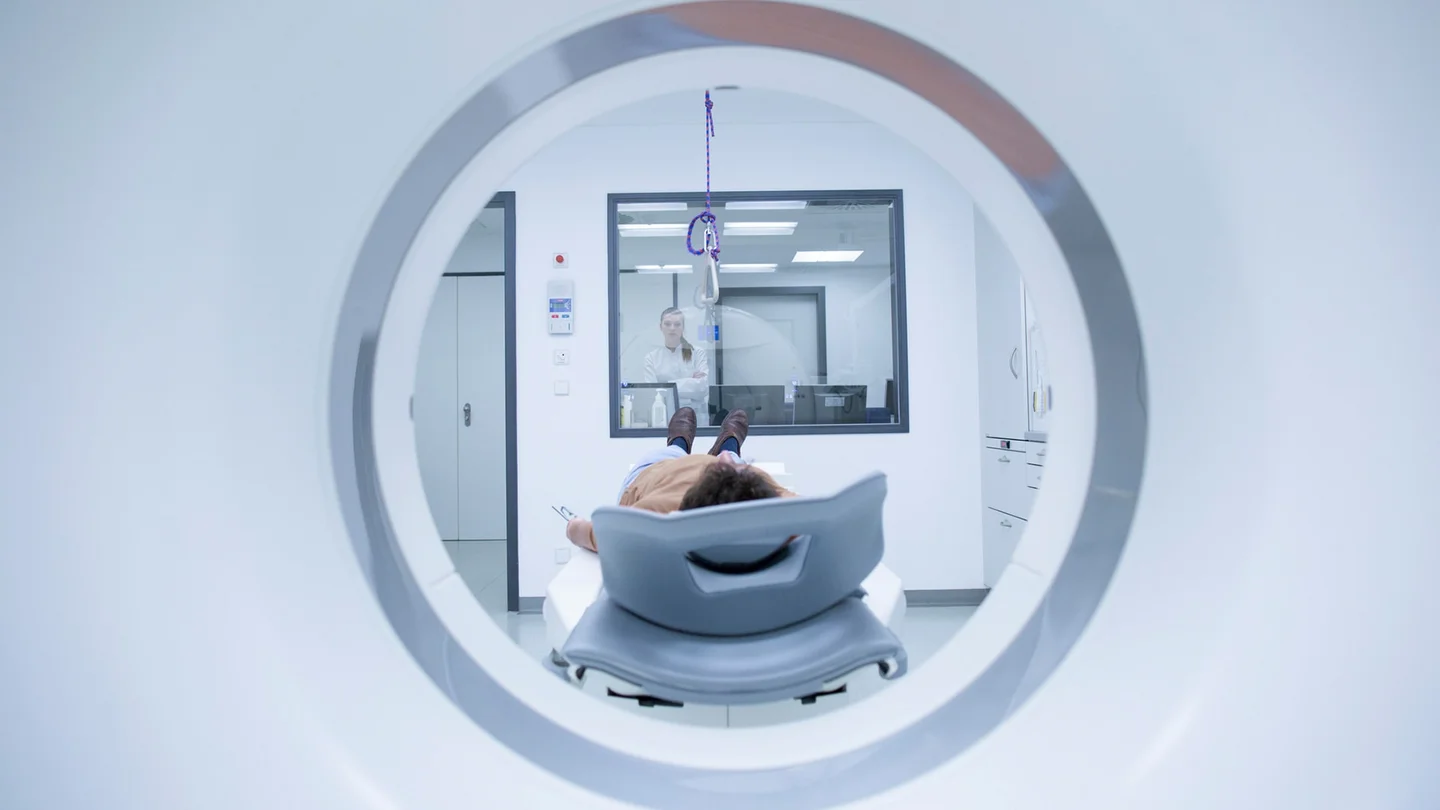
What is CUP syndrome?
In “normal” tumors, the cancer originates in a specific organ and then spreads or “metastasizes” to other parts of the body in the form of secondary or metastatic tumors, also known as metastases. CUP syndrome, in contrast, is an unusual type of cancer, in which doctors detect metastases in the body but are unable to pinpoint the tumor of origin. This is why it’s called CUP or cancer of unknown primary.
In CUP syndrome, cancer cells have detached themselves from an unknown tumor of origin and migrated to other tissues or organs, making this an advanced form of cancer that often grows aggressively.
Many tumors form metastases in the liver, lung, bones and/or lymph nodes in particular. But growths can also occur in the brain or the skin. Moreover, in patients with CUP syndrome, metastases also migrate to sites in the body where tumors would not usually spread. Metastases can occasionally occur simultaneously in several different organs.
Where does the cancer originate?
In patients with CUP syndrome, doctors search for the “primary tumor”, the tumor where the cancer originated. If they find the tumor of origin, the cancer is assigned to the specific organ or tissue. If the search is unsuccessful the diagnosis of CUP syndrome is retained.
What are the symptoms of CUP syndrome?
The symptoms of CUP syndrome, like its potential origin and presentation, can vary widely from patient to patient. The specific symptoms depend in particular on the organ or tissue to which the metastases migrate.
So there are no typical symptoms of CUP syndrome. However, in most cases they will be symptoms of any advanced cancer such as:
- swollen lymph nodes that are firm to the touch, do not move and are not painful
- enlarged abdominal girth, swelling or hard masses in the chest or abdomen
- unusual shortness of breath (dyspnea) or pain in the chest or abdomen
- pain in the bones
- persistent fatigue, exhaustion or loss of appetite
- involuntary weight loss
Anyone with these symptoms should consult a doctor. This is particularly important if they are not caused by an infection and last longer than a few days or even weeks.
What causes CUP syndrome?
The causes of CUP syndrome are still largely unknown. However, it is known that the metastases in the body must have come from an original cancer site.
Cancers are based on genetic mutations that convert normal cells in the body into malignant cancer cells. These cancer cells start to grow uncontrollably into surrounding tissue, destroying it. Cancer cells are also capable of detaching themselves from the primary site, spreading around the body through the lymph system and/or bloodstream and migrating into other organs to form metastases.
Video What is cancer?
The video below explains when doctors talk about cancer and how cancer occurs.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
But why is it that the metastases can be detected but not the tumor of origin? Experts believe that some of the cancer cells’ properties act in favor of CUP syndrome. Various theories have been put forward, for example:
- One theory is that the metastases in CUP syndrome migrate very quickly after the original cancer occurs without actually forming any primary tumor at all. Or the primary tumor is so small that it does not cause any symptoms and goes undetected by the usual tests.
- Another theory is that the body’s immune system has managed to deal with the tumor of origin but not with the metastases that form in the meantime.
How common is CUP syndrome?
The medical literature has a number of different estimates of the prevalence of CUP syndrome. The Center for Cancer Registry Data (Zentrum für Krebsregisterdaten) estimates that around 10,500 people get CUP syndrome in Germany each year. This means that CUP syndrome accounts for approximately 2 percent of cancer cases. Most people affected are over 60 years of age, and CUP syndrome occurs with more or less the same frequency in women and men.
The number of CUP diagnoses has declined in recent years. This may be because the tumor of origin is actually being detected in an increasing number of cases, or doctors have at least been able to clarify the tissue from which the cancer cells have originated. In these cases, the diagnosis of CUP syndrome is changed to the relevant type of cancer.
How does CUP syndrome progress?
Like its symptoms and presentation, the progression of CUP can vary significantly from one patient to another. Decisive factors include the origin of the cancer cells, how aggressively they grow and the tissue to which they have migrated. So no overall prognosis can be provided. However, a cure is unlikely for most patients with CUP, as the cancer advances rapidly in most cases.
The prognosis is better for around one in five patients. For these, the biological properties of the cancer cells, for example, may indicate a specific tumor of origin. Doctors can then begin organ-specific treatment. As a result, these patients generally have a prognosis that is similar to that of cancer patients with a corresponding primary tumor at the same stage.
How is CUP syndrome diagnosed?
If doctors detect cancer cells expressed as metastases in a patient, they initially focus on determining how many metastases there are, how large they are and where precisely they are situated.
They also try to identify the tumor of origin. For patients, this often means that testing can take longer to complete, which generally requires a great deal of patience and endurance.
Doctors begin by determining the patient’s general health status (medical history). This is followed by a physical examination and laboratory testing of blood, urine and stool samples. However, imaging scans are the main diagnostic tool used. These mostly involve a computed tomography (CT) scan of the chest, abdomen and pelvic cavity. But they may also include:
- positron emission tomography (PET)
- magnetic resonance imaging (MRI)
- endoscopy of various organs, as suggested by the patient’s symptoms
- ultrasound breast scan and mammography
- transvaginal ultrasound in women
- scintigraphy
The most important diagnostic goal is to exclude specific cancers such as lymphomas or germ cell tumors. These may present a clinical picture similar to that of CUP syndrome but generally respond well to chemotherapy and are potentially curable.
Doctors also try to identify whether the tumor of origin could be a sex-specific form of cancer such as prostate cancer or breast cancer. For this purpose, they sometimes determine endogenous (from your own body) substances in the blood that indicate cancer (tumor markers).
However, the tumor of origin may never be identified, even after rigorous investigation. If that is the case, doctors use histological examinations of tissue to try to identify the origin of the cancer cells.
Histological examinations
Histological examinations of CUP syndrome metastases are particularly important. In these analyses, tissue samples are treated with a special stain and examined under the microscope. They are also subjected to microbiological testing. This involves searching for the typical characteristics of certain types of cancer for the purpose of identifying, or at least narrowing down, the location of the tumor of origin.
The examinations are intended to help determine:
- whether the cells can be assigned to a specific organ of origin such as the prostate, lung, breast or bowel
- the type of cancer involved – for example, carcinoma, melanoma, sarcoma or lymphoma
- the sub-type of the cancer – for example, adenocarcinoma or squamous cell carcinoma
The diagnostic goal is always to exclude certain types of cancer and to identify the tumor of origin – or, at least, to find biological properties that are important for treatment planning. However, doctors do not continue searching for the tumor of origin forever. They also need to start treatment as soon as possible. If diagnostic testing is unable to identify a tumor of origin, CUP syndrome is diagnosed.
How is CUP syndrome treated?
Most patients with CUP syndrome receive palliative treatment. Curative treatment is only possible in rare cases. The overall goal of treatment is to slow the growth of the metastases, alleviate symptoms and maintain quality of life as far as possible. Generally, treatment should be personalized and take the following into account:
- overall health
- likely progression of the disease
- patient’s individual requests
The crucial factor in the treatment of cancer of unknown primary is whether the organ of origin can be determined from examination of the cancer cells. Treatment can be targeted far more precisely if the features of the tumor can be precisely assigned to a specific suspected origin.
So treatment varies depending on whether the primary tumor:
- is located. If so, it is by definition no longer a CUP syndrome. The cancer is instead assigned to the relevant organ or tissue. In most cases, prognosis is more favorable. Patients are treated in accordance with the treatment guidelines for the specific type of cancer. Their treatment usually follows the recommendations for patients with the advanced, metastasized form of the cancer.
- is suspected. Here too, patients often have a better prognosis and are also treated in accordance with the treatment guidelines for the specific type of cancer.
- cannot be identified. In most cases, metastases have already spread to the internal organs. So the prognosis is worse. However, treatment is still possible – in most cases, this will be palliative and involve chemotherapy with the minimum of adverse side effects, causing the least amount of discomfort to patients.
But it’s not just the origin of the tumor that is important here. Another important factor is the extent to which the CUP syndrome metastases have already spread. Are they just located at a single site, or have they already infected several organs?
Localized metastases
Doctors can remove localized metastases by surgery or targeted radiotherapy, sometimes using a combination of the two. However surgery is only appropriate if there is a chance of curing the cancer or alleviating symptoms. Targeted radiotherapy is designed to reduce the size of metastases and prevent them from growing, and in the case of bone metastases to alleviate pain.
Systemic therapies
However, since most CUP syndromes have already metastasized into multiple organs, treatments that act on the whole body (“systemic therapies”) are more important for many people with CUP syndrome. For most of these patients, chemotherapies with low adverse side effects are the treatment of choice. However, immunotherapy or antihormone therapy are also possible if the cancer cells exhibit the necessary properties.
Targeted drugs are also suitable for systemic treatment as they block biological mechanisms that are important for cancer growth but not for healthy tissue. However these drugs are only available for patients with tumor tissue that exhibits specific biological properties.
What are the procedures for the various cancer treatments and what side effects do they have? You can find detailed information on the different treatments on the German Cancer Research Center’s Cancer Information Service website (in German).
What happens after CUP syndrome treatment?
Receiving treatment for CUP syndrome can be physically and mentally exhausting. Medical rehabilitation (rehab) aims to help patients regain their strength. It is also designed to help them cope with the consequences of the disease and its treatment as best as possible.
Rehab focuses on the patient’s personal history with the disease and individual limitations. Psycho-oncological counseling to help people deal with worries and fears can be particularly helpful to those with CUP syndrome.
Aftercare
Whether CUP patients require aftercare will depend on the specifics of the disease. If the aim of the treatment was to effect a cure, the CUP patient should receive intensive aftercare. However this is rarely the case.
Is the cancer incurable? If so, check-ups and regular ancillary care can help to identify and alleviate distressing symptoms. The aim is to maintain the patient’s quality of life for as long as possible.
What changes following a CUP syndrome diagnosis?
Suddenly facing a diagnosis of cancer is usually extremely distressing for most people. This applies particularly if the disease is already at an advanced stage. The nature of CUP syndrome itself also exacerbates the situation – despite numerous examinations and diagnostic tests, doctors may never be able to identify the origin of the cancer in most cases.
What’s more, the disease develops very rapidly in many people, leaving very little time for them to adjust to the new situation. They have to weigh up the risks and benefits of treatment options over and over with their doctors. Patients with CUP syndrome therefore usually require intensive care and monitoring.
But that doesn’t mean patients have to spend the whole time hospitalized or regularly go to hospital for in-patient treatment: many treatments or checkups can be provided by specialists in medical practices or specialist outpatient clinics.
Frequent contact with medical staff is also important as metastasized cancers can lead to conditions that can change very rapidly. The regular checkups are a chance to discuss pain, nausea, dietary or weight problems as well as any other distressing symptoms. There is usually something that can be done to help with these problems.
Who are the best contacts for people with CUP syndrome?
There is no official list in Germany of clinics that treat patients with CUP syndrome. Certified organ centers exist for other types of cancer but not for CUP syndrome. The individual circumstances of the patients’ health will determine the treatment they receive. An interdisciplinary approach is often required for both diagnosis and treatment of patients with CUP.
University hospitals or other large clinics generally have specialist departments that work together on an interdisciplinary basis. Some of the large cancer centers also provide dedicated clinics for patients with CUP syndrome as part of their interdisciplinary outpatient cancer service.
You can find information on how to find the right clinic on the German Cancer Research Center’s Cancer Information Service website (in German).
Or you can contact professional associations to identify specialist centers. One of these in Germany is the CUP Syndrome sub-group of the Working Group on Internal Oncology (AIO).
Do you have further questions about dealing with the condition in everyday life and additional support options? You can find information about this on the German Cancer Research Center’s Cancer Information Service website (in German).
For all questions about CUP syndrome, you can also make direct contact with Cancer Information Service doctors by dialing the freephone number (0800) 420 30 40 or by sending an e-mail to krebsinformationsdienst@dkfz.de.
- Europäische Gesellschaft für medizinische Onkologie (European Society for Medical Oncology, ESMO). Cancers of unknown primary site: ESMO Clinical Practice Guidelines. Aufgerufen am 08.12.2023.
- Hübner G, Borner M, Stöger H, Neben K. CUP Syndrom – Krebserkrankungen mit unbekanntem Primärtumor. Leitlinie der Deutschen Gesellschaft für Hämatologie und Onkologie (DGHO). Juni 2023. Aufgerufen am 08.12.2023.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at: