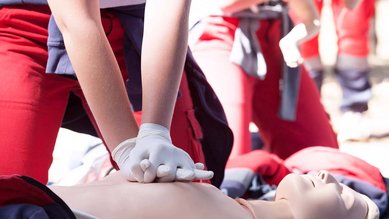
Healthy living First aid for children
Falls, burns, choking, poisoning, insect bites – whenever a child has an accident or emergency incident, adults are obliged to help them. First aid for children is pretty much the same as first aid for adults. However, there are a few differences to keep in mind.
At a glance
- Don’t be afraid of doing something wrong – your help can save lives.
- In an emergency, call emergency services on 112.
- If the child is unconscious but still breathing, place them in the recovery position.
- If they have stopped breathing, give them 5 rescue breaths (mouth-to-mouth) followed by 30 chest compressions and repeat this cycle until an ambulance arrives. For babies, use two fingers instead of the ball of the hand for chest compressions.
- Avoid moving injured children if possible and protect wounds from becoming contaminated.
- Stay with the child to calm and comfort them.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
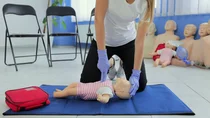

What to do in an emergency involving a child
Children require first aid if they find themselves in an emergency situation due to an accident or illness. Adults are legally obliged to provide this assistance. This applies even if emergency services have already been notified.
Don’t be afraid of doing something wrong – first aid for babies and children only differs in a few small respects from first aid for adults.
However, it is important to take account of the age and size of the child involved. This is essential when giving rescue breaths and resuscitating a child, for example. A distinction is made between the following age groups:
- Babies: infants up to 1 year of age
- Small children: toddlers and pre-schoolers from age 1 up to school-going age
- Children: children from their first year of school until they reach puberty
The first aid recommendations for adults apply in the case of older children and adolescents.
It is important to stay with the child to calm and comfort them and ensure that they are not left alone. Fuss and panic will upset the child and make them anxious.
How to provide first aid to babies and children
First, get an overview of whether the child is:
- conscious and responsive
- injured
- in an area of risk and needs to be brought to safety
Alert the emergency services as soon as possible by dialing 112. This number can be used free of charge nationwide from both cell phones and land lines. For more information about emergency calls, see the article on the topic of first aid.
Begin essential first aid measures without delay.
What to do if a child is unconscious
When a person loses consciousness, all of their muscles go limp. As a result, the tongue can potentially block the top of the throat and the airways. The cough reflex also stops working.
- Carefully turn unconscious children on their side to free their airways and prevent them from choking on saliva, blood or vomit. For more information about how to put someone into the recovery position, see the article on the topic of first aid.
- There’s no need to additionally extend the head for babies and small children.
- Place the child on something warm if possible and cover them, e.g., with an emergency blanket or jacket.
- The child needs to be covered up and kept warm.
- Try to get the child to respond to you by speaking to them, touching them or pinching the inside of their upper arm.
Important: Never shake a baby or small child, as this can cause a potentially fatal brain hemorrhage.
How to determine whether a child is breathing
It’s easiest to check whether the baby or child is breathing if they are lying on their back. If a baby’s head falls forward when they are in this position, it can be gently moved back into a neutral position. To find out whether a child is breathing:
- Hold your ear close to their nose and mouth. This will allow you to feel their breath on your cheek and hear breathing noises.
- While doing so, look at the child’s chest and stomach to detect any breathing movements.
- If, after 10 seconds, you haven’t detected any breathing or if their breathing is very irregular, immediately begin giving them CPR, i.e., rescue breaths and chest compressions.
What to do if a child or baby has stopped breathing
If you cannot detect any breathing, if the breathing detected is irregular or if you are unsure, begin immediately with rescue breaths and chest compressions:
- In children older than 1 year of age, begin by giving 5 rescue breaths. Pinch the child’s nose closed while doing so. In babies (younger than 1 year), deliver 5 rescue breaths into the mouth and nose at the same time. Always check to ensure that the chest is visibly rising and falling.
- If they don’t begin to breathe, place them on their back on a hard surface.
- Remove anything covering the child’s chest.
- If the baby is younger than 1, place two fingers on the center of the chest and press down towards the spine 30 times.
- If the child is older than one, you can use the ball of your hand for chest compressions and use an extended arm to exert pressure.
- Each compression should push the chest down by about one third.
- Press down twice per second.
- If you haven’t called the emergency services yet, take a short break from CPR after one minute to do so.
- Continue repeating cycles of 2 rescue breaths followed by 30 chest compressions until the ambulance arrives.
Important: Don’t be afraid of doing something wrong. Your help could save a life.
How to stop bleeding in a child
Small cuts and grazes can be carefully cleaned before being covered with a bandage or plaster. Heavy bleeding, including persistent nosebleeds, can lead to shock and place strain on the heart and circulation. Information about stopping bleeding is provided in the general article on the topic of first aid.
What are typical emergency situations for children?
Children need comfort and attention if they have had an accident or are feeling ill. Stay with the child at all times if possible and talk to them:
- Try to explain the situation to the child in an age-appropriate way.
- Explain to the child what you’re going to do.
- Ask the child for their help and praise them for it.
If the child is responsive, you can ask them what happened and how they are feeling. Bear in mind, however, that younger children are often unable to tell with certainty where they are feeling pain or injury. In this case, it can be helpful to talk to people who witnessed what happened and to carefully examine the child.
Of course, it would be best if accidents never happened in the first place. To find out how to identify potential hazards and avoid accidents involving children, see the article discussing accidents involving children.
What to do if a child has a fall
Almost all fall-related accidents, such as bone fractures, contusions, strains and sprains present with bruising and swelling.
What to do if a broken bone is suspected
- Avoid moving the baby or child if possible and lay them flat or in the position in which they were found
- For open fractures, cover the wound with a sterile wound dressing or cloth from a first-aid kit to prevent infection
- Gently support and immobilize the body part affected
- For closed fractures, carefully cool the swelling
- Cover the child and keep them warm
What to do if a contusion, strain or sprain is suspected
If a child has fallen, you can treat them according to the “RICE rule”:
- R – rest: immobilize the affected part of the body immediately
- I – ice: use cool packs or an ice pack to cool down the affected part of the body
- C – compression: use a compression bandage
- E – elevation: elevate the injured body part, ideally above heart height
Important: Before using cool packs and ice, place a cloth over the skin to protect the skin from frostbite.
How to tell if a child has concussion
A concussion can be caused by a knock or hard impact to the head. If the child is unconscious, it is essential to call the emergency services.
Typical signs of concussion are:
- a dazed feeling
- double vision
- vomiting
- lethargy or confusion
- lack of speech
- tiredness
- uncontrollable crying
What to do if a child swallows something and is at risk of suffocating
A foreign body in the windpipe or esophagus can cause an urge to cough, wheezing, inability to speak, an urge to vomit or difficulty breathing. The face often turns red or blue. If the foreign body is visible when you look into the mouth, you can try to remove it with your fingers. If you suspect that the child has swallowed or breathed in a foreign body but you are unable to see it, call the emergency services immediately. Encourage the child to cough.
If coughing fails to dislodge the foreign object and the child/baby is unable to breathe and becomes unconscious:
- Turn babies onto their back and give them five abrupt chest compressions by applying your fingertips to the middle of their chest.
- Abdominal thrusts can be used for children aged over 1 and for adolescents. Kneel or stand behind the child, place a fist on their upper abdomen below the breastbone and sharply pull your fist backwards and upwards 5 times in succession.
- Alternate back blows and abdominal thrusts until the foreign body is dislodged or until emergency services arrive.
- The aim of each action is to change the position of the foreign body so that the child can get some air.
Important: Do not lift small children up by their legs to give them back blows.
What to do if a child is drowning
As soon as the child has been rescued from the water, start giving them CPR, i.e., rescue breaths and chest compressions immediately. Ignore any water that may be in the lungs, as this cannot be removed. Attempting to do so would only cause an unnecessary delay to resuscitation efforts.
What to do if a child is bitten in the mouth or throat
Insect venom can cause the mucus membranes in the mouth and throat or the tongue to swell, making it difficult to breathe. Allergic shock (anaphylaxis) may also occur if the child has an insect venom allergy. In this case, dial 112 to notify the emergency services.
Until the emergency services arrive:
- Get the child to suck on ice-cream or ice cubes.
- Cool the throat on the outside using an ice pack or cold compress.
- If the child is unconscious, place them in the recovery position.
- Begin CPR, i.e., rescue breaths and chest compressions immediately if they stop breathing or their heart stops.
What to do if a child has heatstroke, sunburn or sunstroke
Babies and small children are more sensitive than adults to sunshine and heat. Their body’s temperature regulation is unable to cope with high temperatures. Sunstroke is caused by strong sunshine, while heatstroke is caused by high temperatures. Sunburn can also have serious consequences.
Signs of sunstroke or heatstroke:
- headache
- dizziness
- nausea and vomiting
- fast pulse
- increased body temperature (fever)
- a bright red face
- stiff neck
First aid for sunstroke and heatstroke:
- If the baby or child has a temperature of 40 degrees or higher, notify the emergency services.
- Bring the baby or child to a cool location in the shade.
- Lay the child down flat, but with a slightly elevated head.
- Remove any unnecessary clothing.
- Pour cool – but not ice-cold – water over their chest or place damp towels on the chest.
- Encourage the child to drink water but make sure it is not too cold.
Sunburn is a first-degree or second-degree burn. What to do if a child is sunburned:
- Ensure that the baby or child is not exposed to direct sunshine for at least one week.
- Cool the irritated skin with damp towels and use hydrating lotions.
- Consult a doctor immediately if fever and chills develop.
Important: Sunburn in childhood increases the risk of developing melanoma skin cancer later in life. To prevent sunburn, good sunscreen is important for children in particular. Put sunscreen with a sun protection factor (SPF) of 30 to 50 on your child in the morning and reapply over the course of the day if necessary.
What to do if poisoning is suspected
The term poisoning is used if a substance that is harmful to health enters the body via the airways, mouth, skin or eyes and causes harm. Household poisoning is common in children, for example, due to swallowing cleaning agents.
If poisoning is suspected, first call the emergency services and then the poison control center. They provide expert advice 24 hours a day. For more details of what to do if someone is poisoned, see the article about first aid for poisoning.
For a complete overview of emergency phone numbers for poison control centers, see the website of the Federal Office of Consumer Protection and Food Safety (Bundesamt für Verbraucherschutz und Lebensmittelsicherheit, BVL).
What is the child emergency app?
The child emergency app (“Kindernotfall-App”) is an app for smartphones. It contains guides and instructions for first aid measures for children and babies. It also offers:
- an emergency call function
- a search function for emergency ambulances and pharmacies
- timer for chest compressions with optical and acoustic signals
- tips for avoiding sunstroke and tick bites
- tips for everyday safety for children
The child emergency app is available free of charge for all standard smartphone operating systems.
Where to find training courses in first aid for children
Special training courses in first aid for children and babies are offered by various voluntary and emergency organizations. These courses usually comprise both theoretical and practical components.
For courses offered by St. John’s Ambulance (“die Johanniter”), see www.johanniter.de.
For courses offered by the Order of Malta (“die Malteser”), see www.malteser.de.
For courses offered by the German Red Cross (“Rotes Kreuz”), see www.drk.de.
For courses offered by the Workers’ Samaritan Federation (ASB), see www.asb.de.
Deutsche Gesetzliche Unfallversicherung e.V. (DGUV). Handbuch zur Ersten Hilfe in Bildungs- und Betreuungseinrichtungen für Kinder. Aufgerufen am 11.04.2022.
Kahl K. Kindernotfall-App: Erste Hilfe am Kind. Deutsches Ärzteblatt 2021. 118(17): A-896 / B-741.
Maltester Hilfsdienst e.V. Erste Hilfe für Babys und Kinder – das solltest du wissen. Aufgerufen am 11.04.2022.
Universitätsklinikum Bonn. Erste Hilfe am Kind. Verschlucken / Ersticken. Aufgerufen am 11.04.2022.
Universitätsklinikum Bonn. Wiederbelebung (Reanimation) bei Säuglingen/Babys. Aufgerufen am 16.04.2022.
Reviewed by the German Interdisciplinary Association for Intensive and Emergency Medicine (Deutsche Interdisziplinäre Vereinigung für Intensiv- und Notfallmedizin e.V. – DIVI).
As at: