Conditions Non-melanoma skin cancer
ICD codes: C44 What are ICD codes?
Non-melanoma skin cancer is a blanket term used to describe certain skin tumors that are unlike those that occur in melanoma skin cancer. If detected early, non-melanoma skin cancer responds well to treatment. This article explains who is most at risk of developing non-melanoma skin cancer and how it can be treated.
At a glance
- Within the category of non-melanoma skin cancer, doctors further distinguish between basal cell carcinoma (BCC) and squamous cell carcinoma (SCC).
- It is rare for non-melanoma skin cancer to metastasize, i.e. spread to other parts of the body. However, squamous cell carcinoma is somewhat more aggressive than basal cell carcinoma.
- Squamous cell carcinomas often develop as cancer precursors, for example actinic keratoses. BCC, in contrast, develops directly without any precursor growths.
- The main risk factor for non-melanoma skin cancer is exposure to sunlight, specifically UV radiation in sunlight.
- Non-melanoma skin cancer responds well to treatment, in particular if it is detected at an early stage.
- The main goal of treatment is complete removal of the tumor.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is non-melanoma skin cancer?
Non-melanoma skin cancer is a type of cancer involving skin tumors that differ from those that occur in melanoma skin cancer. When doctors speak of non-melanoma skin cancer, they are usually referring only to the two main sub-categories of basal cell carcinoma (also commonly called basal cell cancer or BCC) and squamous cell carcinoma (squamous cell cancer or SCC).
BCC and SCC each develop from different types of skin cell. SCC is somewhat more aggressive than BCC. Both forms of non-melanoma skin cancer only rarely metastasize, i.e. spread to other parts of the body.
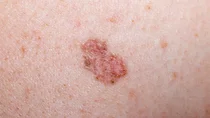
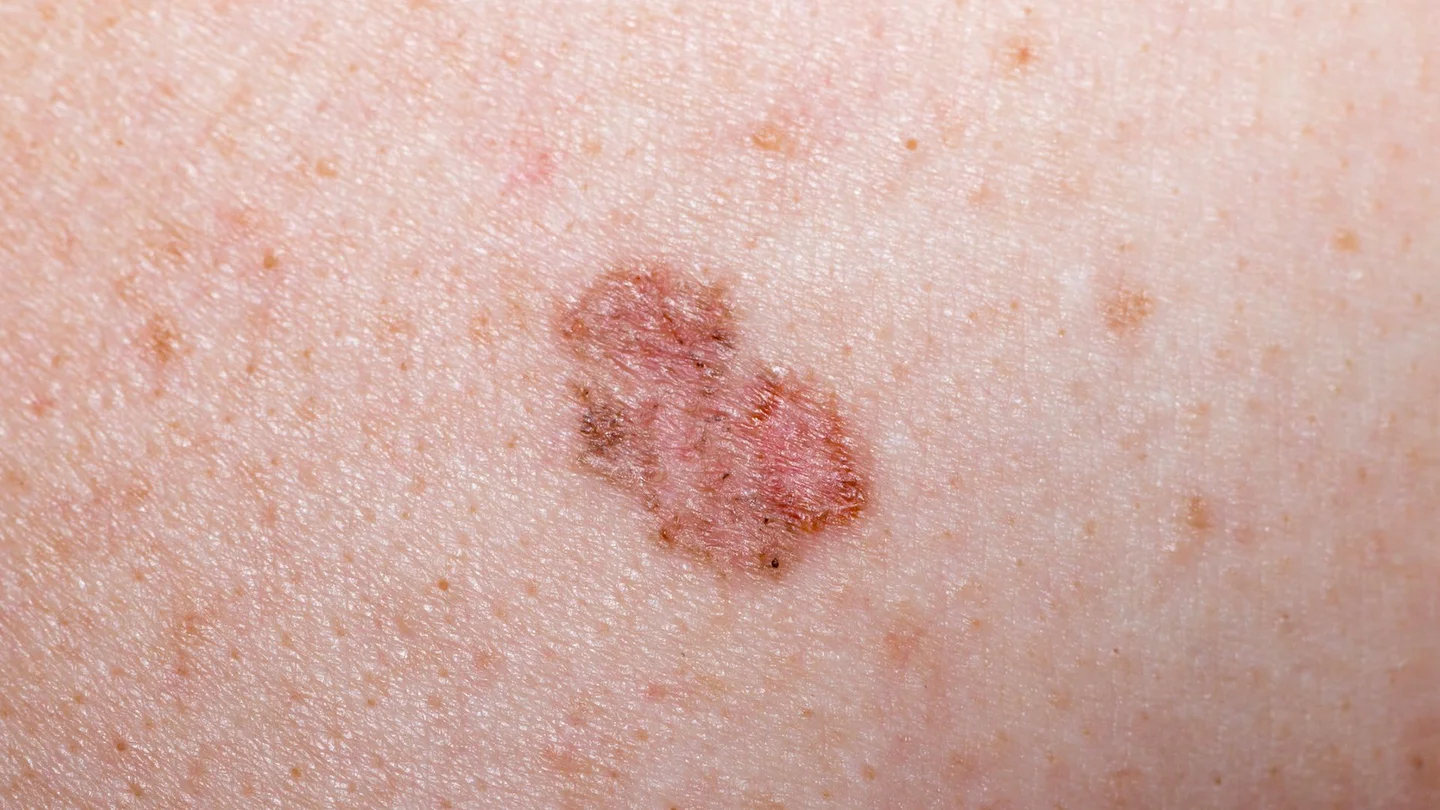
Where on the body does non-melanoma skin cancer develop and what does it look like?
Non-melanoma skin cancer occurs most frequently on the areas of the body that are most exposed to sunlight. These include the face and ears, as well as any parts of the scalp that are not covered by hair.
However, basal cell carcinoma can also occur on parts of the body that are not overly exposed to the sun, such as the torso (upper body).
Both BCC and SCC can vary greatly in their appearance. Sometimes, it is even difficult for doctors to distinguish between different types of non-melanoma skin cancer when looking at them with the naked eye.
Appearance of basal cell carcinoma
BCC most commonly appears as a
- small, translucent, pearly-white or pinkish bump with tiny blood vessels and that is sunken in the middle.
- Later, a tumor develops with an elevated, ridge-like border comprising several small bumps that appear like a string of pearls.
In rarer cases, BCC may appear as
- whitish, scar-like, flat areas or
- flat, scaly, reddish patches.
In very rare cases, BCC can also develop as dark patches on the skin, which are similar in appearance to melanoma skin cancer.
Oozing skin defects and open sores can develop if BCC is not detected and treated in good time.
Appearance of squamous cell carcinoma
SCC may appear as:
- a hardened, horn-like patch of skin
- a flat open sore with a raised, ridge-like border
- a hardened bump, with or without an open sore
Other signs of SCC include:
- rapid growth
- crusting
- hardened tissue
- bleeding
- redness
- flaking
What causes non-melanoma skin cancer?
In most cases, non-melanoma skin cancer occurs because the skin has been exposed to excessive amounts of ultraviolet (UV) radiation. This radiation may come from sunlight, tanning lamps and tanning beds, or other artificial sources of UV light.
The risk of developing squamous cell carcinoma and basal cell carcinoma increases in proportion to the amount of UV radiation people have been exposed to over their lifetime. The risk of basal cell carcinoma also increases as a result of repeated intense UV exposure. This includes sunburn during childhood and adolescence, for example.
Other causes of non-melanoma skin cancer
Contact with poisonous substances such as arsenic or coal tar can also trigger non-melanoma skin cancer. Exposure to X-ray radiation can also increase the risk of developing non-melanoma skin cancer.
Who is at a particularly high risk of developing non-melanoma skin cancer?
Fair complexion: people with a fair complexion are at particular risk of developing non-melanoma skin cancer. Their skin is particularly sensitive to UV radiation.
In addition, some pre-existing conditions also put people at a higher risk of non-melanoma skin cancer:
- Inherited skin disorders: patients with inherited skin disorders associated with light sensitivity are more likely to develop basal cell carcinoma and squamous cell carcinoma.
- Immune suppression: patients whose immune systems have been suppressed by medication (e.g. following an organ transplant) or are not functioning normally due to illness (e.g. as a result of an HIV infection) are also at a higher risk of developing non-melanoma skin cancer.
- Actinic keratoses: an actinic keratosis is a pre-cancerous skin growth, which can develop into squamous cell carcinoma. People with one or more actinic keratoses (sometimes also called solar keratoses) are at a higher risk of developing squamous cell carcinoma.
- A history of non-melanoma skin cancer: if an individual has already had non-melanoma skin cancer, the risk of developing another skin tumor is higher.
How common is non-melanoma skin cancer?
Non-melanoma skin cancer is the most common type of cancer in Germany, with almost 200,000 new cases reported in 2018. However, very few patients die as a result of non-melanoma skin cancer. In 2018, this was just under 1,000 people.
Non-melanoma skin cancer is most common among older adults.
How does non-melanoma skin cancer progress?
Basal cell carcinoma: BCC is usually slow-growing and remains limited to the area of the skin in which it initially develops. It does not normally metastasize, i.e. spread to other parts of the body. However, if BCC is not treated, it can continue to grow and gradually destroy the surrounding tissue structures.
Squamous cell carcinoma: SCC also tends to only grow at its site of origin. However, it is somewhat more aggressive than BCC. In around 4 percent of patients, SCC will spread to other parts of the body (metastasize).
Left untreated, non-melanoma skin cancer can expand into the surrounding tissue structures and destroy them.
Cancer precursors of non-melanoma skin cancer
BCC, unlike SCC, develops without a pre-cancerous form. SCC, meanwhile, frequently develops from pre-cancerous growths, actinic keratoses, actinic cheilitis on the lips or Bowen’s disease.
How can non-melanoma skin cancer be prevented?
Most cases of non-melanoma skin cancer are caused by overexposure to ultraviolet (UV) radiation. Therefore, it is very important to ensure adequate protection against overexposure to the sun and UV radiation. This includes avoiding use of tanning beds.
Consistent sun protection can reduce the risk of developing non-melanoma skin cancer. However, there is no fail-safe method of preventing it.
The following measures help to protect you against excessive UV radiation:
- During the summer in particular, avoid strong sunlight between the hours of 11 am and 3 pm.
- Move into the shade or under a parasol, especially around midday. Note: even in the shade, the skin is still exposed to a small amount of UV radiation.
- Wear UV-protective clothing and sunglasses as well as a hat.
- Use plenty of sunscreen on any uncovered areas of the body.
- Do not use solariums.
Parents should take care to protect their children particularly well. Furthermore, people who work outdoors should follow their company’s sun protection measures.
The Federal Office for Radiation Protection (Bundesamt für Strahlenschutz) provides a forecast of the intensity of the UV radiation to be expected from the sun in Germany over the coming days.
Would you like to know more about UV rays and how to protect yourself from them? You can find detailed information about UV radiation and sun protection on the website of the Cancer Information Service of the German Cancer Research Center (in German).
What screening options are available?
In Germany, anyone aged 35 and over and covered by statutory health insurance is entitled to a skin cancer screening every 2 years. This skin cancer screening is part of the statutory cancer screening program.
During the screening, a specially trained doctor examines all of the individual’s skin and mucous membranes.
You should also check your skin regularly and have any suspicious changes checked by a dermatologist.
How is non-melanoma skin cancer detected?
In most cases, doctors detect non-melanoma skin cancer based on the external appearance of the skin when examined with the naked eye. Sometimes, a reflected-light microscope (dermatoscope) can help to examine the affected area of the skin in greater detail and, for example, to exclude other types of skin cancer or skin diseases.
If basal cell carcinoma or squamous cell carcinoma is suspected, the doctor can take a tissue sample (biopsy). However, the tumor can also be surgically removed immediately (without a biopsy) and examined under the microscope.
Further tests, e.g. ultrasound or computed tomography (CT) scans, are rarely necessary. They are only used if the tumor is growing into the deeper levels of the skin or if it is suspected that the cancer has spread.
How can non-melanoma skin cancer be treated?
With non-melanoma skin cancer, the main objective of treatment is to remove the tumor entirely. For this purpose, the doctor will normally excise (surgically remove) the skin cancer. A microscope will be used to ensure that the tumor has been removed in its entirety.
If surgery is not possible or if the patient does not want to have this procedure done, other types of treatment can be considered. This may be the case, for example, if the tumor has developed on a very visible part of the face and surgery would leave scars. Treatment options include:
- radiation
- special light therapy (photodynamic therapy)
- freezing of the tumor (cryotherapy)
- laser treatment
- medicated creams applied locally to the skin
Factors that will determine which type of treatment is best suited in each case include:
- the type of skin cancer involved
- the size of the tumor
- the location of the tumor
- how advanced the skin cancer is (has it metastasized?)
- the patient’s general health
If the cancer is already at an advanced stage, special medication may be administered. This is the case, for example, if the tumor is growing into and destroying the deeper skin levels or has already spread to other organs. Medication can suppress and halt the progress of the cancer – at least for a certain amount of time.
Targeted therapy drugs are available for advanced basal cell carcinoma. These suppress the growth of tumor cells and can prevent the disease from progressing further.
Patients with advanced squamous cell carcinoma can be treated with a type of immunotherapy known as immune checkpoint inhibitors. These substances bind to specific docking sites on the body’s own defense cells and stimulate these to fight the cancer cells directly.
Video How is cancer treated?
The video below explains how cancer can be treated.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
Would you like more detailed information about the various types of treatment available? You will find detailed descriptions of many of the treatment options mentioned here on the website of the Cancer Information Service of the German Cancer Research Center (in German).
What happens after treatment?
Treatment of non-melanoma skin cancer is followed by a program of aftercare. This is used to ensure that any recurring tumors in the same or a different site on the skin are detected at an early stage.
Once treatment is completed, the patient will be examined by a doctor at regular intervals. The length of these intervals will be determined by the individual risk of relapse in each case. Patients who are at a higher risk of further tumors occurring will be screened more frequently than those at a lower risk.
What does aftercare involve?
The doctor will examine every part of the patient’s skin at the follow-up appointment. Patients who have had squamous cell carcinoma may also have an ultrasound scan to examine the lymph nodes. Other scanning methods, such as computed tomography (CT) or magnetic resonance imaging (MRI), are only used if the doctor detects any relevant signs of disease and wants to exclude the possibility that the cancer is progressing.
Those who have recovered from non-melanoma skin cancer should also examine themselves regularly to ensure that any further tumors which may occur are detected and treated at an early stage.
Would you like to know more about testing methods like ultrasound or computed tomography? You will find detailed descriptions of these and other methods on the website of the Cancer Information Service of the German Cancer Research Center (in German).
Living with non-melanoma skin cancer
For most patients with non-melanoma skin cancer, their tumor responds well to treatment and their life expectancy is not affected. Advanced, life-threatening basal cell carcinoma or squamous cell carcinoma are very rare.
Those who have recovered from non-melanoma skin cancer should protect themselves from overexposure to the sun and examine themselves regularly.
Points of contact for more information about non-melanoma skin cancer
Hospitals that are particularly experienced in treating patients with skin cancer can demonstrate this through certification. The German Cancer Society (DKG) regularly checks their compliance with certain professional requirements.
You can find the addresses of the certified centers on the OncoMAP website.
You can also search for dermatology clinics in Germany on the homepage of the German Dermatological Society.
Do you have further questions about dealing with the condition in everyday life and additional support options? More information is provided on the website of the Cancer Information Service of the German Cancer Research Center (in German).
You can also contact the Cancer Information Service directly with any questions about non-melanoma skin cancer on freephone 0800 420 30 40 or by e-mail at krebsinformationsdienst@dkfz.de.
- Arbeitsgemeinschaft Dermatologische Onkologie (ADO). Basalzellkarzinom der Haut. S2k-Leitlinie. AWMF-Registernummer 032 – 021. 06.2018.
- Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF. Aktinische Keratose und Plattenepithelkarzinom der Haut. Langversion 2.0. S3-Leitlinie. Leitlinienprogramm Onkologie. AWMF-Registernummer 032/022OL. 12.2022.
- Deutsche Krebsgesellschaft, Deutsche Krebshilfe, AWMF. Prävention von Hautkrebs. Langversion 2.0. S3-Leitlinie. Leitlinienprogramm Onkologie. AWMF-Registernummer 032/052OL. 03.2021.
- Zentrum für Krebsregisterdaten (ZfKD) des Robert-Koch-Instituts (RKI). Nicht-melanotischer Hautkrebs (heller Hautkrebs). Aufgerufen am 29.03.2023.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at:

