Conditions Sepsis
ICD codes: R57.2 A41 What are ICD codes?
Sepsis, also known as blood poisoning, always follows an infection that the body’s own defense system can no longer hold off. Infectious agents and the body’s own inflammatory messengers then flood the organism and damage critical organs. Sepsis is a life-threatening complication and it is always an emergency.
At a glance
- With sepsis, the body’s own response to an infection gets out of control and damages the organs.
- Multiple vital organs can fail.
- Approximately one third of the people in Germany who get a sepsis or a septic shock die from it each year.
- Sepsis is more common than a stroke, breast cancer or bowel cancer.
- A case of sepsis is always an emergency.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is sepsis?
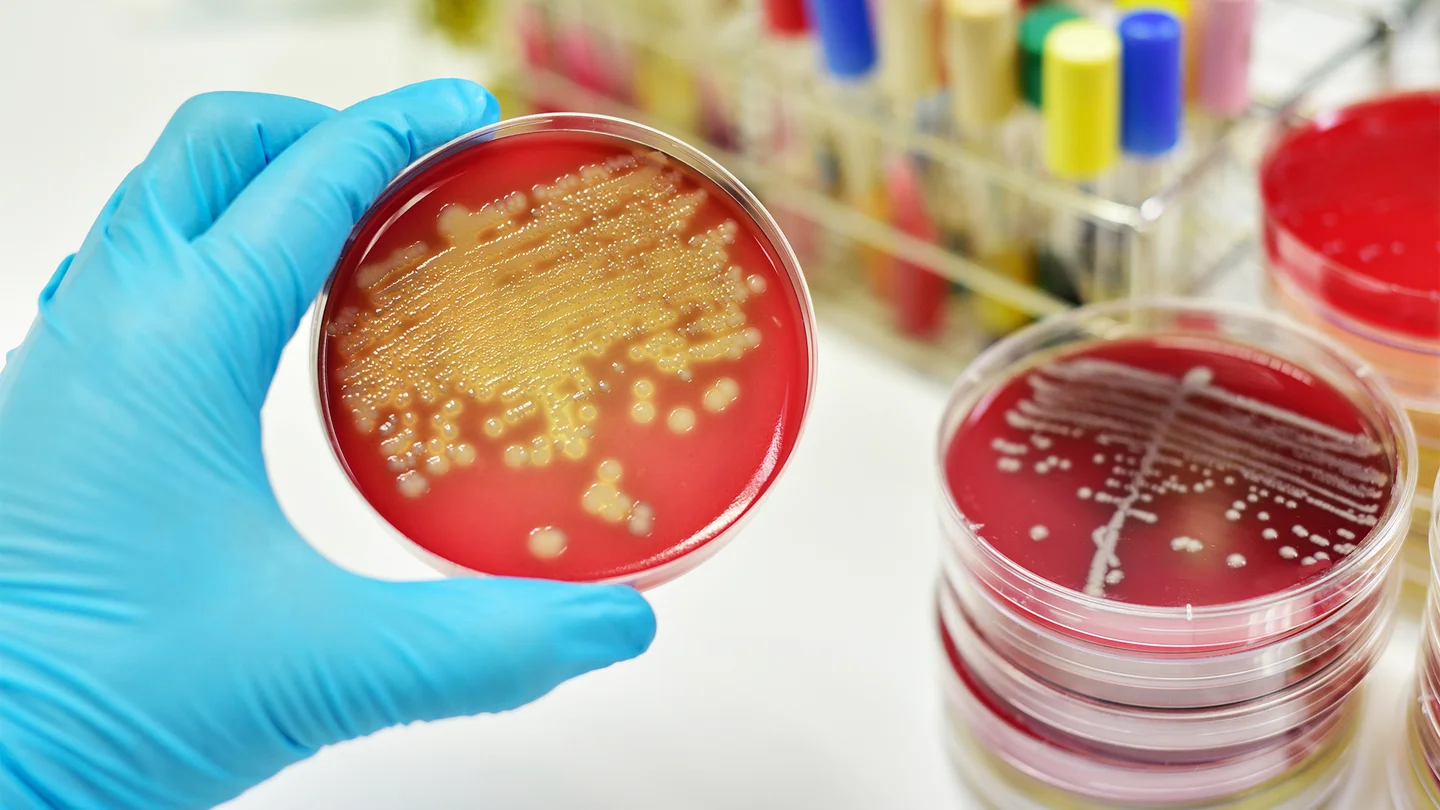
Sepsis always stems from a local, limited infection. The infection is usually caused by bacteria, but viruses, fungi and parasites can also cause sepsis. Sepsis is also known as blood poisoning, but it has nothing to do with poisoning in the usual sense. Rather, it is a runaway defense response of the body to the infectious agents. Pathogens and inflammatory messengers spread throughout the body and damage vital organs.
What are the symptoms of sepsis?
When an infection spreads through the body, there are initially non-specific symptoms that resemble those that occur with a common cold or flu.
These may include:
- temperature above 38 degrees or body temperature below 36 degrees
- shivering
- accelerated pulse
- generally feeling very ill
- aches
The following warning signs may indicate sepsis:
- sudden disorientation
- low blood pressure: systolic below 100 mmHg
- rapid breathing: over 22 breaths per minute
If at least one of these three indicators is present, you should get medical help immediately. A case of sepsis is always an emergency.
Important: Systolic blood pressure specifies the pressure with which the heart is pumping blood in the body. It is the first of the two blood pressure values to be measured and is normally between 110 and 130 mmHg. A value below 100 mmHg is regarded as critical in older people in particular.
A red streak slowly spreading on the arm also supposedly indicates sepsis. But most patients do not have this symptom. The red streak occurs if a lymph channel is inflamed, for example due to an infected wound. This can cause sepsis, but it does not necessarily do so.
What causes sepsis?
Sepsis is always caused by an infection. The infection is usually bacterial, but viruses, fungi and parasites can also cause sepsis. As long as the body can keep the infection local, sepsis does not occur. It is only when it breaks through that pathogens and inflammatory messengers flood the entire body. This can cause damage to organs and circulatory collapse.
Any type of infection can cause sepsis: purulent, inflamed wounds to the skin or mosquito bites, inflamed teeth, infected prostheses, pneumonia, meningitis, urinary tract infections, diarrhea, and many other infectious conditions. Sepsis is the final common pathway if the body’s own defense system can no longer hold back the infection.
Video What is sepsis?
The video below explains how sepsis is triggered. What are the symptoms and how can they be treated?
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
How does sepsis progress?
Sepsis can quickly become life-threatening, but it does not always need to become serious. Doctors differentiate between two phases:
Sepsis
Sepsis is referred to when the inflammatory response to the infectious agents causes damage to the body. Immune cells and inflammatory messengers then attack vital organs and restrict their function. It usually affects the lungs, heart, liver and kidneys.
Septic shock
Septic shock involves the cardiovascular function collapsing so that the organs no longer receive an adequate supply of blood. Sometimes multiple organs fail. Many patients die from this type of septic shock.
How can sepsis be prevented?
There is no protection against sepsis itself, but infections that can cause sepsis can be prevented. The following general measures help to avoid infections, which reduces the risk of sepsis:
- Hygiene: wash hands regularly and thoroughly.
- Take good care of wounds and inflamed areas of skin. You should not scratch, and you should keep wounds clean and disinfect them.
- Possibly get a medical opinion if infected.
- If your doctor prescribes an antibiotic, take it as prescribed and for the length of time indicated.
- Chronic conditions such as rheumatism and diabetes can weaken the body’s defenses, and they should be treated properly.
- Lead a healthy lifestyle to strengthen your immune system.
- Vaccinations help to avoid certain infectious diseases.
How is sepsis diagnosed?
Doctors diagnose sepsis based on the symptoms and the case history. They then take several blood samples to check how the organs are functioning and to provide evidence of possible infectious agents in the blood.
How is sepsis treated?
Sepsis must be treated in hospital, as it is always an emergency. The quicker medical practitioners start treatment, the better the chances of recovery, and the milder the potential damage.
Before hospital treatment begins, doctors take several blood samples. On the one hand, this enables the pathogens to be identified and suitable drugs to be chosen. On the other, blood values are measured to show whether and which organs are already being damaged.
Even before the blood test results are in, the patient is given an antibiotic that acts against the most common sepsis pathogens. They are also given intravenous fluids to stabilize the circulation. Once the blood test results are in, doctors can switch to the most effective drug.
If blood pressure values drop dramatically and there is too little oxygen in the blood, the patient must be treated in intensive care. If it is not clear where the pathogens are coming from, doctors need to do more tests to identify the source of the infection so that they can treat it.
Where can I get everyday support?
Patients that have had severe sepsis very often suffer mental and physical complications. Top-class aftercare is not always possible, however, for example due to a lack of rehab places. Organizations like Deutsche Sepsis-Hilfe e.V. offer those affected and their relatives a platform for getting information, finding the help that is available, and for sharing experiences with others who have been affected.
Go to the Deutsche Sepsis-Hilfe e.V. website
What other useful information is there?
There is a World Sepsis Day every year on September 13th. This aims to draw attention to the high rates of illness and fatality, and to help change this through early detection and better treatment methods.
- Brunckhorst FM, Gastmeier P, Abu Sin M. Aktuelle Aspekte zur Definition und Diagnostik der Sepsis und Antibiotikaresistenz. Bundesgesundheitsblatt – Gesundheitsforschung – Gesundheitsschutz 2018. 61: 562–571. Aufgerufen am 11.11.2020.
- Deutsche Sepsis-Gesellschaft e.V. Sepsis – Prävention, Diagnose, Therapie und Nachsorge. S3-Leitlinie. AWMF-Registernummer 079-001. 12.2018. Aufgerufen am 11.11.2020.
- Engel C et al. Epidemiology of sepsis in Germany: results from a national prospective multicenter study. Intensive Care Med 2007. 33(4): 606–618. Aufgerufen am 11.11.2020.
- Robert Koch-Institut (RKI). Infektionskrankheiten A–Z: Sepsis. Aufgerufen am 03.11.2020.
- Sepsis-Stiftung. Gemeinsam gegen Sepsis – Früherkennung rettet Leben. Aufgerufen am 03.11.2020.
- Singer M et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016. 315(8): 801-810. Aufgerufen am 03.11.2020.
- Weltgesundheitsorganisation (WHO). Improving the prevention, diagnosis and clinical management of sepsis. Aufgerufen am 03.11.2020.
Reviewed by the German Sepsis Society (Deutsche Sepsis-Gesellschaft e.V.).
As at: