Healthy living Stem cell donation: from the search for a donor to healing
A stem cell donation can save the lives of people with blood-forming diseases or congenital immunodeficiencies. However, it is sometimes difficult to find a suitable donor. Nearly all healthy people aged 18 to 55 can register in a donor database.
At a glance
- Stem cell transplants are used for malignant blood diseases or congenital immunodeficiencies.
- Voluntary stem cell donors are registered in the Central Bone Marrow Donor Registry (in German: Zentrale Knochenmarkspender-Datei, or ZKRD).
- For a successful transplantation, the tissue characteristics of the donor and recipient must match as closely as possible. Typing is done with a swab of the oral mucosa or a blood sample.
- Stem cells are usually taken from the blood, but more rarely bone marrow may be taken from the pelvis.
- The chances for a transplant’s success are about 50%.
What is a stem cell donation?
Various types of cells can mature from stem cells. The blood-forming stem cells are located in the bone marrow and can evolve into different blood cells with various functions. These blood cells then enter the bloodstream.
In a stem cell donation, people with particular diseases of the hematopoietic (blood-forming) system receive healthy stem cells from voluntary donors. A stem cell donation gives people with malignant blood diseases like leukemia the chance to heal.
Because these stem cells usually come from other people, the term allogenic (originating “from elsewhere”) stem cell donation is used. With certain diseases, the body’s own hematopoietic stem cells can also be used. This is called autologous (“originating from oneself”) hematopoietic stem cell transplant.
When is a stem cell donation necessary?
A stem cell donation is used to treat hematopoietic diseases or disorders of the immune system for which other therapies have not been successful on a long-term basis. These include:
- blood cancer, e.g. acute leukemia
- hematopoietic disorders such as aplastic anemia
- congenital hematopoietic and immune defects
- lymphomas, for example Non-Hodgkin lymphoma
- lymphatic diseases like lymph node cancer
With some of these diseases, normal blood formation is disrupted because the white blood cells are multiplying uncontrollably. As a result, the body is no longer able to fight infections, transport enough oxygen or stop bleeding. A stem cell transplant is usually considered when earlier therapies have not shown any satisfactory effect or do not look as though they will be successful.
How many people need a stem cell donation?
In Germany, more than 11,000 people become ill every year with leukemia or another hematopoietic disorder. Some of them need a stem cell donation to make a cure possible. About 3,500 stem cell transplantations are performed in Germany each year.
20 to 30% of patients in need of a blood stem cell donation find a donor within their family. All others rely on unrelated donors. In Germany, there is a matching donor for 9 out of 10 sick people.
Who may donate stem cells?
Any healthy person aged 18 to 60 who weighs at least 50 kg can be a stem cell donor. The registration must be made up to the age of 55. After the donor turns 61, their data is automatically deleted from the registry.
With certain diseases, a stem cell donation is not possible as it may pose a risk to the donor or recipient. These include:
- cancer
- insulin-dependent diabetes mellitus
- diseases of the blood or blood vessels
- infections with HIV, hepatitis B or hepatitis C
- autoimmune diseases like Crohn’s disease, rheumatoid arthritis, multiple sclerosis, lupus erythematosus
Existing allergies or high blood pressure should be individually cleared with the particular donor database. After, for instance, surgeries or biopsies, a pregnancy or various infectious diseases, a stem cell donation may have to be temporarily postponed.
How can people register for a stem cell donation?
To register as a stem cell donor, a swab of the oral mucosa or a blood test is required. The registration needs a declaration of consent and analysis of the tissue characteristics:
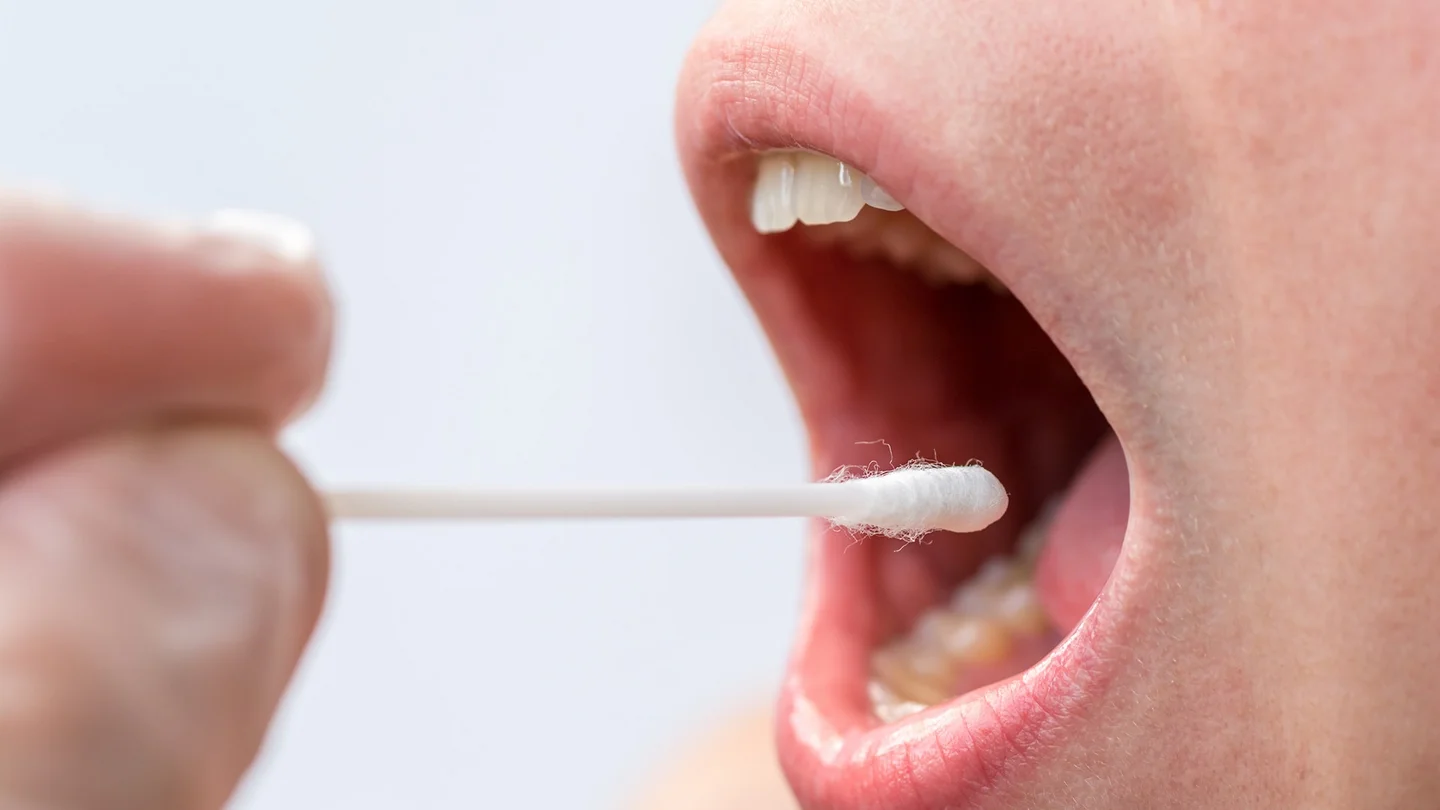
- by a swab of the oral mucosa (home typing set)
- as part of a blood donation
- by submitting a blood sample to a GP
- during a typing campaign
Various organizations offer a set for typing. This makes it possible to independently extract some cells from the oral mucosa with the aid of a cotton swab and send them back to the organization for assessment. A more precise typing with a blood sample is required in case a donor is chosen for a transplant.
Typing sets are available from all German donor databases. There is an overview of all German donor databases available from the Central Bone Marrow Donor Registry (ZKRD) at www.zkrd.de.
Relatives or friends of sick people who require a stem cell donation sometimes organize local typing campaigns. However, it is not possible to only donate stem cells specifically for one particular person. In addition, the data collected from typing campaigns is stored in the central registry and is thus available for all data matches with potential stem cell recipients.
Can a donor who registered at one time withdraw?
Voluntary donors can withdraw their consent at any time without giving reasons. As soon as a sick person is prepared for a stem cell transplant however, a cancellation is no longer possible – dropping out would be life-threatening for the recipient.
How is a suitable stem cell donor found?
After a donor has been registered, the extracted blood sample or submitted oral mucosa swab is assessed in a laboratory. The tissue data is then provided to the Central Bone Marrow Donor Registry from the particular donor database. A match of stem cell donors and potential recipients is done here. The aim is to find a “genetic twin”. The higher the match of tissue characteristics is, the greater the likelihood is that the stem cell transplantation will proceed successfully.
How is a match between donor and recipient established?
The unique genetic characteristics of a person are called “HLA markers”. The abbreviation stands for human leukocyte antigens. They are also called tissue characteristics. HLA markers are structures on the surfaces of body cells. They can occur in the most varied combinations. The immune system uses them to recognize whether the cells are the body’s own or foreign ones.
To prevent undesirable immune responses, it is important for the HLA markers of the stem cell donor and recipient to match as closely as possible. If it is not possible to find a donor that is a 100% match, then depending on the patient’s risk of disease, a stem cell donation with HLA markers that do not fully match the recipient’s markers can also be chosen.
What is the Central Bone Marrow Donor Registry’s job?
The saved data of all registered donors in Germany is transferred from the particular donor database and foundations to the Central Bone Marrow Donor Registry (ZKRD). More than 7 million people are registered in that, according to the data of the German Stem Cell Donor Registry.
Furthermore, the ZKRD is linked to other registries in Europe and the wider world. All data converges in the “Bone Marrow Donors Worldwide” database. This stores the tissue characteristics of all available stem cell donors throughout the world. Thanks to this networking, the data of people who need a stem cell donation can be matched with around 29 million potential donors from all over the world.
What is the procedure for stem cell harvesting?
The type of stem cell harvesting is based on the patient’s medical requirements such as their age or how quickly the donation is needed. The harvesting type is suggested by the transplant center. Possible methods of stem cell harvesting are:
- peripheral stem cell harvesting (stem cells from venous blood)
- harvesting of stem cells from the bone marrow of the pelvis
- using stem cells from umbilical cord blood
80% of stem cell donations are done via blood withdrawal. This method is called “peripheral stem cell harvesting”. Much more rarely, stem cells are extracted directly from the bone marrow of the pelvis. Contrary to a common misconception, stem cells are never harvested from the spinal cord. Until now, stem cells from umbilical cord blood have seldom been used, because only a few parents are aware that they can donate umbilical cord blood of their child.
What is the procedure for a peripheral stem cell donation?
With this method, the stem cells are harvested from the venous blood of the donor. A preliminary medical examination is carried out in the harvesting center 2 to 4 weeks before the donation. For preparation, the number of stem cells in the donor’s blood is initially increased. This is achieved by administering the messenger G-CSF. The abbreviation stands for “granulocyte colony-stimulating factor”. The drug is injected under the skin twice a day 4 or 5 days before the donation.
Stem cell harvesting is an outpatient procedure that takes place in a harvesting center on 1 to 2 days. It always takes 4 to 5 hours. Anesthesia is not required. The procedure is called stem cell apheresis. In the course of this, the donor blood is initially guided from the arm vein into a cell separator in which the stem cells are harvested. The blood is subsequently restored again via a second intravenous access. The body regenerates the stem cells within 2 weeks.
How are stem cells harvested from the bone marrow?
With this method also, a preliminary medical examination is carried out in the harvesting center 2 to 4 weeks before the donation. During a bone marrow donation, the stem cells are harvested from the bone marrow of the pelvic bone with a puncture needle. The operation takes about 60 minutes and is performed under general anesthetic. For bone marrow harvesting, donors remain in hospital for 3 days altogether. They are often subsequently on sick leave for several days. The missing bone marrow regenerates within 2 to 4 weeks.
How are stem cells harvested from umbilical cord blood?
After the birth of a child, the blood of the umbilical cord can be donated on the parents’ request. This does not cause any adverse effects whatsoever for mother or child. The stem cells can be harvested from the umbilical cord blood and provided to other people who need a stem cell transplantation. Umbilical cord blood is considered high-quality, because it contains many still very immature blood-forming stem cells. As a result, they adapt well to the new body after a transplant. Rejection reactions of the immune system can thus be prevented as far as possible. However, these cells are not normally suitable for an autologous transplant, because the stem cells of people with blood cancer may already contain the disease-causing genetic defect.
Important: According to current knowledge, storing umbilical cord blood in case one’s own child requires stem cells later on is not a good idea. Consequently, the costs of that are not borne by health insurance providers.
Who bears the costs of a stem cell donation?
The required examinations and treatments in the course of a stem cell donation are paid for by the recipient’s health insurance provider. It also accepts the costs for travel to and from the harvesting center or hospital, a possible loss of earnings and other expenditure. The costs for the registration and typing of potential stem cell donors are borne by the foundations and donor databases performing these tasks. These organizations therefore often ask for donations.
What are the risks and side effects of a stem cell donation?
During stem cell harvesting from the pelvic bone or the blood and the prior G-CSF treatment, side effects – usually slight – may develop. These include:
- flu-like symptoms such as headaches, muscle aches or bone pain (peripheral stem cell harvesting)
- tingling in or around the mouth (peripheral stem cell harvesting)
- nausea and vomiting (after anesthesia during stem cell harvesting from the pelvic bone)
- pain and minor bruising at the puncture or harvesting site
- dizziness
- in rare cases, allergic reactions
All these symptoms are temporary. When necessary, pain can be treated with painkillers. The risks are thus low for healthy donors.
Important: A stem cell donation does not lead to permanent loss of stem cells. The body regenerates them within a few weeks.
How are stem cells transplanted?
Treatment of the stem cell recipient begins with what is known as conditioning therapy. In the course of this, the patient is treated with high-dose chemotherapy or radiotherapy. The goal of these is to destroy as many cancer cells in the body as possible. At the same time, the immune defense is suppressed by drugs so that the new stem cells will not be rejected or fought against by the recipient’s immune system, if possible.
How does the stem cell transplant proceed?
After harvesting, the stem cells are immediately brought to the hospital in which the transplant is to be carried out. There, they enter the recipient’s bloodstream via an infusion. The donated stem cells then settle independently in the bone marrow and start to multiply.
Due to the pre-treatment, the recipient’s immune system is severely weakened. The body is thus highly susceptible to infections with pathogens. To reduce the risk of infection, patients spend the first few days or even weeks after a stem cell transplant in special wards with high hygiene standards. They should moreover follow particular hygiene and nutrition recommendations in the initial months after the transplant.
What are the chances for success?
The donated stem cells migrate to the bone marrow via the blood and form new blood cells there. This process takes about 2 to 3 weeks.
Among the biggest risks after the stem cell transplantation is a rejection reaction of the immune system, reactions to the earlier chemotherapy or radiation and a recurrence of the original illness.
A patient is considered cured if there is no relapse within 5 years after the transplant. According to the German Registry for Stem Cell Transplantation, the national 5-year survival rate is about 40 to 50%.
In the event of insufficient success or a recurrence of the illness, a stem cell transplantation can be repeated after an extended period.
Can donors and recipients meet?
For reasons of data and privacy protection, recipients and donors of stem cells initially remain anonymous. 3 months at the earliest after a stem cell donation, a query can be made about the patient’s state of health and the donor informed if interested. If they wish, donors and recipients may contact each other anonymously later on. The German guidelines only allow a face-to-face meeting 2 years after a successful stem cell transplantation provided both parties agree. Other rules may apply for donations outside Germany, or made to Germany from other countries.
- Bundesärztekammer. Richtlinie zur Herstellung und Anwendung von hämatopoetischen Stammzellzubereitungen – Erste Fortschreibung. Deutsches Ärzteblatt 2019. doi: 10.3238/arztebl.2019.rl_haematop_sz02
- Bundeszentrale für gesundheitliche Aufklärung (BZgA). Die Stammzellspende und Transplantation bei schwerwiegenden Erkrankungen des Blutes. Aufgerufen am 01.03.2021.
- Deutsche Gesellschaft für Hämatologie und Medizinische Onkologie e.V. Spenderauswahl Allogene Stammzelltransplantation. Onkopedia Leitlinien. 01.2021.
- Deutsche Knochenmarkspenderdatei (DKMS). Grundlegende Informationen. Aufgerufen am 01.03.2021.
- Deutsches Register für Stammzelltransplantationen (DRST). Jahresbericht 2019. 10.2020.
- Deutsche Stammzellenbank. Vorsorge durch Stammzellen aus Nabelschnurblut. Aufgerufen am 03.03.2021.
- Deutsche Stammzellspenderdatei. Stammzell- und Knochenmarkspende. Aufgerufen am 01.03.2021.
- Gragert L, Eapen M, Williams E et al. HLA match likelihoods for hematopoietic stem-cell grafts in the U.S. registry. N Engl J Med. 2014 Jul 24;371(4):339-48. doi: 10.1056/NEJMsa1311707. PMID: 25054717; PMCID: PMC5965695.
- Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen (IQWiG). Stammzelltransplantation bei Krebs. In: Gesundheitsinformation.de. Aufgerufen am 03.03.2021.
- Klingebiel T. The price of hope: is autologous cord blood storage necessary and useful? Dtsch Arztebl Int. 2009 Dec;106(50):829-30. doi: 10.3238/arztebl.2009.0829. Epub 2009 Dec 11. PMID: 20049093; PMCID: PMC2801067.
- Stiftung Knochenmark- und Stammzellspende Deutschland (SKD). Stammzellen spenden – Informationen für Spender. Aufgerufen am 01.03.2021.
Reviewed by the German Society of Hematology and Medical Oncology (Deutsche Gesellschaft für Hämatologie und Medizinische Onkologie e.V.) (DGHO).
As at:


