Conditions Thyroid cancer
ICD codes: C73 What are ICD codes?
Thyroid carcinomas are rare and can occur at any age. Most forms are slow growing, with few symptoms in the initial stages. The primary treatment is surgery. This article will give you more information about the diagnosis and treatment options.
At a glance
- Benign nodules (lumps) in the thyroid gland are common, but thyroid cancer is rare.
- There are different forms of thyroid cancer. Some occur in family “clusters”.
- The primary treatment option is surgery, usually followed by radioactive iodine therapy.
- Chemotherapy is not normally used.
- Targeted therapy is used in advanced or aggressive forms of the disease.
- After surgery people have to take thyroid hormone tablets for the rest of their life.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is thyroid cancer?
The thyroid gland is located in the front of the neck and produces thyroid hormones, chemical messengers that are vital for body functions. The specialist term for thyroid gland is glandula thyreoidea. Thyroid cancer is sometimes referred to as a thyroid carcinoma. It is a rare disease.
The cancer can start in a number of different types of thyroid cells. The World Health Organization (WHO) has identified four main types of thyroid cancer:
- papillary thyroid carcinoma (most common type)
- follicular thyroid carcinoma
- anaplastic thyroid carcinoma and
- medullary thyroid carcinoma (also C-cell carcinoma)
In papillary and follicular thyroid carcinomas, the cancer cells have the same appearance as normal thyroid cells under the microscope. Experts refer to well-differentiated thyroid carcinomas.
In anaplastic carcinomas, the cancer cells no longer have the same properties as normal thyroid cells. These cancers are therefore referred to as undifferentiated thyroid carcinomas.
Medullary thyroid carcinomas start in the C cells. These are located in the thyroid gland and produce a hormone that is important for calcium metabolism. Medullary carcinomas can occur in family “clusters”.
The thyroid gland produces chemical messengers (hormones). It is part of the body’s endocrine system. So thyroid carcinomas are also classed as endocrine cancers.
What are the symptoms of thyroid cancer?
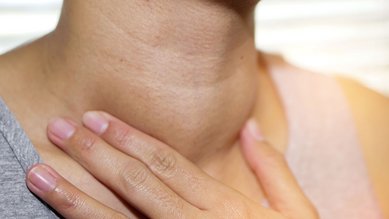
Possible symptoms of thyroid cancer arise from its position at the front of the neck. The thyroid gland is very close to the windpipe and esophagus as well as the nerves of the inner larynx muscles.
Thyroid cancer can cause the following symptoms:
- hoarseness or other persistent changes in speech
- difficulty swallowing
- respiratory problems
- chronic coughing with no other sign of infection such as rhinitis or phlegm
- a nodule (lump) or swelling on the front of the neck (near the Adam’s apple)
- enlarged lymph nodes on the neck
- pain in the neck that may radiate to the ears
These symptoms can also be caused by other conditions such as infections. So it is important to see a doctor for further clarification.
Thyroid cancer: what are the causes and risk factors?
It is still unclear what causes thyroid cancer. The only definite, environmental risk factor is contact with ionizing radiation. This type of contact is relatively rare. Examples include, for example, exposure of the neck to radiation, or reactor accidents that release 131 iodine, as happened in Chernobyl and Fukushima.
Many patients have a history of thyroid conditions such as an enlarged thyroid (goiter) or benign tumors (adenomas). These pre-existing conditions increase the risk of thyroid carcinomas. This risk is still small in Germany.
There are also subtypes of thyroid cancer based on genetic predisposition. The main subtype is the rare medullary thyroid carcinoma (MTC). It is also known as C-cell carcinoma.
There is currently no reliable evidence on the significance of other dietary or life-style-related risk factors or environmental risks. It is also unclear why women are more often affected than men.
How common is thyroid cancer?
There are around 5,700 new cases of thyroid cancer a year in Germany. Women are more often affected than men.
What examinations are conducted for a diagnosis of thyroid cancer?
The doctor starts by asking the patient about potential risk factors and symptoms. He or she then palpates the thyroid gland and adjacent lymph nodes.
Blood is tested for the following markers: thyroid-stimulating hormone (TSH) and calcitonin. For TSH, further names exist: thyrotropin, or hTSH (for human TSH).
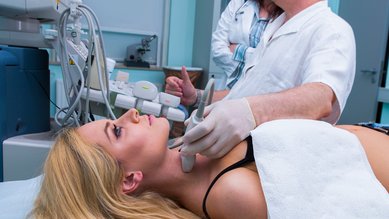
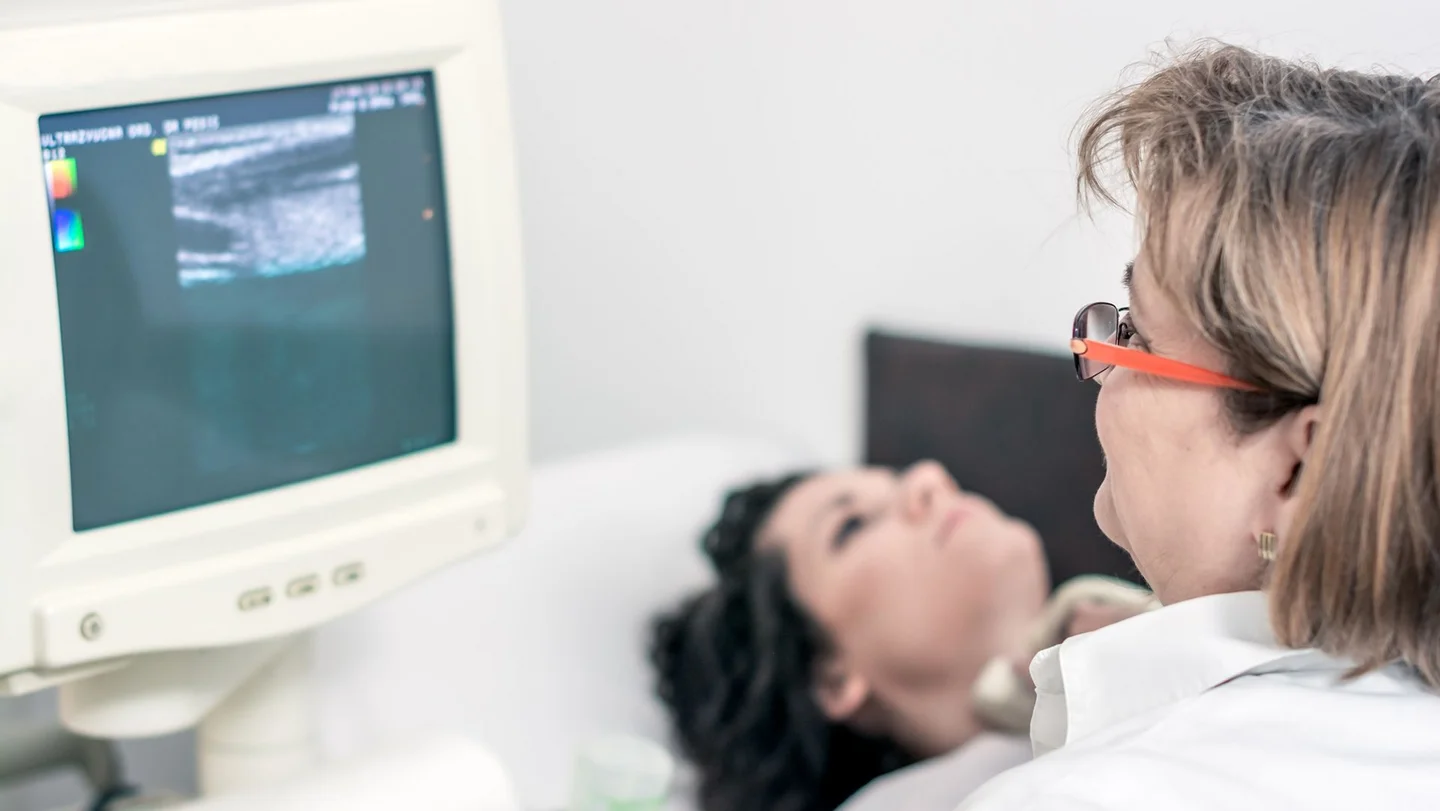
The ultrasound scan (sonography) is the most important examination in suspected cases of thyroid cancer. It reveals the size and composition of the thyroid gland and adjacent lymph nodes. It also allows doctors to identify the location, composition and size of any thyroid nodule.
Nuclear medicine scans (scintigraphy) of the thyroid gland are only needed if any of the following occur:
- There is a nodule that is more than one centimeter in diameter.
- TSH levels are low.
Nuclear medicine scans (scintigraphy) of the thyroid gland provide information about the metabolism of a suspected thyroid nodule and gives pointers on whether a nodule could be thyroid cancer.
To establish or rule out a diagnosis of thyroid carcinoma the doctor removes a sample of tissue from the suspicious site in the thyroid gland. The doctor punctures the lump with a very thin needle in a process known as fine needle aspiration biopsy. Individual cells are removed by suction (“aspiration”) and then examined under a microscope.
If this examination confirms that thyroid cancer is present it is followed by further steps needed to establish a diagnosis. The task then is to find out how far the tumor has grown (determination of cancer spread). The following examinations are recommended for the most common differentiated thyroid cancers:
- ultrasound scan of cervical lymph nodes
- chest X-ray
- laryngoscopy to assess vocal cord movement
How is thyroid cancer treated?
Treatment will depend on the histology of the tumor and on the spread of the disease.
Video How is cancer treated?
The video below explains how cancer can be treated.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
The primary treatment is surgery. This involves a doctor removing part or all of the thyroid gland (subtotal or total thyroidectomy). If it is suspected that the cancer has spread to the lymph nodes, these are also removed during surgery.
Depending on the results of the surgery, doctors will decide whether to follow up with radioactive iodine (I-131) therapy. This is a specialized form of internal radiation. Radioactive iodine is absorbed by targeted cancer cells but also healthy thyroid cells. The goal of treatment is to remove any remaining cancer cells as far as possible.
If the thyroid gland is removed completely and radioactive iodine therapy is applied, there is no longer any functioning thyroid tissue. This means that thyroid hormones need to be administered externally. In other words, patients have to take thyroid hormone tablets (L-thyroxine) for the rest of their life.
If the cancer has spread to other organs and formed distant metastases, various treatment options can be considered depending on the location and number of metastases. The main purpose of these is to improve the patient’s quality of life and slow down the progression of the disease. Complete recovery is only rarely possible if the disease has reached this stage.
New therapies such as targeted therapies are also already being used for thyroid cancer in certain situations. New drugs are being tested in clinical trials, mostly to improve treatment of aggressive or advanced thyroid carcinomas.
Anaplastic thyroid carcinoma
The procedure is rather different for anaplastic thyroid carcinomas. Here too, the tumor should be removed surgically if at all possible. Since anaplastic carcinomas do not store iodine, radioactive iodine therapy is ineffective against this form of thyroid cancer. Post-operative treatment may thus entail a combination of radiation and chemotherapy, referred to as radiochemotherapy. Doctors may also use this approach if surgery is not possible.
Important: Anaplastic thyroid carcinomas progress rapidly. So rapid treatment is required at a center with experience of this rare form of cancer.
Would you like to know more about the treatment of thyroid cancer? What the potential side effects are, what should be considered in relation to radioactive iodine therapy and what treatment options are available for advanced stages of the cancer?
The Cancer Information Service of the German Cancer Research Center can provide information free of charge by phone or e-mail.
What’s next? Aftercare for thyroid cancer
Aftercare is intended to ensure early detection of any relapse and any long-term effects of treatment. People with thyroid cancer are regularly examined after the therapy has ended. Aftercare appointments are made at shorter or longer intervals based on how high the doctors think the risk of relapse is.
Important: If patients experience any symptoms, they should consult their doctor regardless of their aftercare appointments.
At the aftercare appointments doctors ask about symptoms and examine the body. The thyroid hormone levels in the blood are measured to determine whether the right amount of the thyroid hormone L-thyroxine is being administered.
What examinations will be required later on depends on how high the doctors think the risk of a relapse is and what type of thyroid cancer is present.
The following examinations are used in particular during the aftercare period:
- ultrasound scan of the neck
- blood test for the tumor marker thyroglobulin (especially if the thyroid gland has been entirely removed)
- nuclear medicine scan with radioactive iodine injection (depending on risk of relapse)
If there is reason to suspect that the cancer has returned or metastases have formed, further examinations will be used, such as computed tomography, X-ray, ultrasound scans of the abdomen or chest, as well as positron emission tomography (PET). A PET scan can, in particular, make metabolically active cells – such as tumor cells – visible in the body.
Thyroid cancer: what is everyday life like?
How thyroid cancer affects people’s lives depends on the precise consequences of treatment.
Complete removal of the thyroid gland (thyroidectomy), in particular, affects people’s everyday lives.
This is particularly the case if it is followed by radioactive iodine therapy. This leaves the body with no functioning thyroid tissue and patients have to take thyroid hormone tablets for the rest of their lives.
This hormone therapy is generally well tolerated. But there are a few things to watch out for in terms of follow-up checks, side effects, interactions and accompanying illnesses.
Removal of the thyroid gland may also have damaged the adrenal gland. If this is the case it will disrupt the body’s calcium metabolism. Those affected can take a calcium product to restore calcium levels.
Another potential side effect of surgery is vocal cord paralysis. This paralysis mostly clears up after some time but can also be permanent.
Consequences of radioactive iodine therapy can also affect people’s lives in the longer term. The risk of a secondary cancer unrelated to the thyroid carcinoma is slightly increased by radioactive iodine therapy.
Men should consider whether their family planning is complete before embarking on radioactive iodine therapy. If radioactive iodine therapy involves a high therapeutic dose of iodine-131 it can result in azoospermia, where sperm cells do not reach maturity. Cryopreservation (freezing) of sperm can help them to have a child later despite receiving radioactive iodine therapy.
Depending on the total therapeutic dose of iodine-131, radioactive iodine therapy can accelerate onset of the menopause in women.
Psycho-social and psycho-oncological support can also be helpful. Counseling by trained experts is often provided to patients while they are still in hospital. Other supports for patients and their families include psycho-social cancer counseling centers and registered psycho-oncologists. Self-help organizations provide patients with important support in dealing with a range of issues and with information from other people in a similar situation.
Are you looking for the addresses of cancer counseling centers or psycho-oncologists working in psychotherapy? Enter your search term and a radius on the website of the Cancer Information Service of the German Cancer Research Center to find addresses where you live or nearby.
Key points of contact and more information on thyroid cancer
There are currently no oncology centers certified by the German Cancer Society (DKG) for the treatment of thyroid cancer.
Interdisciplinary cooperation between all specialties involved (surgery, internal oncology, radiotherapy, nuclear medicine, endocrinology and ear, nose and throat medicine) is important for the diagnosis and treatment of thyroid carcinomas, as well as clinical experience of diagnosing and treating thyroid carcinomas. So it is recommended that you use clinics or treatment centers that meet the relevant requirements.
You can find information on how to find the right clinic on the website of the Cancer Information Service of the German Cancer Research Center (in German).
Among the oncology centers certified by the German Cancer Society (Deutsche Krebsgesellschaft, DKG) are some that fulfill the special requirements for the treatment of “endocrine malignancies” such as thyroid cancer. These can be found on the OncoMap website.
There are also centers for thyroid and adrenal gland surgery/endocrine surgery certified by the German Society for General and Visceral Surgery (DGAV).
The European Neuroendocrine Tumor Society (ENETS) has certified several German centers as centers of excellence. An overview is provided on the website of the Neuroendocrine Tumors Network self-help organization (Netzwerk Neuroendokrine Tumoren e.V).
Do you have further questions about dealing with the condition in everyday life and additional support options? You can find information about this on the website of the Cancer Information Service of the German Cancer Research Center (in German).
For all questions about thyroid cancer, you can also make direct contact with Cancer Information Service doctors by dialing the freephone number (0800) 420 30 40 or by sending an e-mail to krebsinformationsdienst@dkfz.de.
- Haugen BR, Alexander EK, Bible KC et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid 2016. 26(1): 1-133. Aufgerufen am 22.12.2023.
- Smallridge RC, Ain KB, Asa SL et al. American Thyroid Association Guidelines for Management of Patients with Anaplastic Thyroid Cancer. Thyroid 2012. 22(11): 1104-1139. Aufgerufen am 22.12.2023.
- Wells SA, Asa SL, Dralle H et al. Revised American Thyroid Association Guidelines for the Management of Medullary Thyroid Carcinoma prepared by the American Thyroid Association Guidelines Task Force on Medullary Thyroid Carcinoma. Thyroid 2015. 25(6): 567–610. Aufgerufen am 22.12.2023.
- Zentrum für Krebsregisterdaten (ZfKD) des Robert Koch-Instituts (RKI). Schilddrüsenkrebs. Aufgerufen am 22.12.2023.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at: