Conditions Acne inversa
ICD codes: L73.2 What are ICD codes?
Acne inversa (hidradenitis suppurativa) is a chronic inflammatory skin condition. It causes issues such as painful nodules, pustules and abscesses. However, extensive skin damage can also occur. The condition often has a significant psychological impact. Its causes are unclear.
At a glance
- Acne inversa is a chronic inflammatory skin condition.
- It primarily affects the armpits, groin and anal and genital areas.
- The inflamed areas of skin are usually very painful and weep.
- The precise causes of acne inversa are unknown.
- At present, there is no cure for acne inversa. However, the symptoms can be alleviated and the progress slowed.
- The type of treatment depends on the severity of the condition.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.

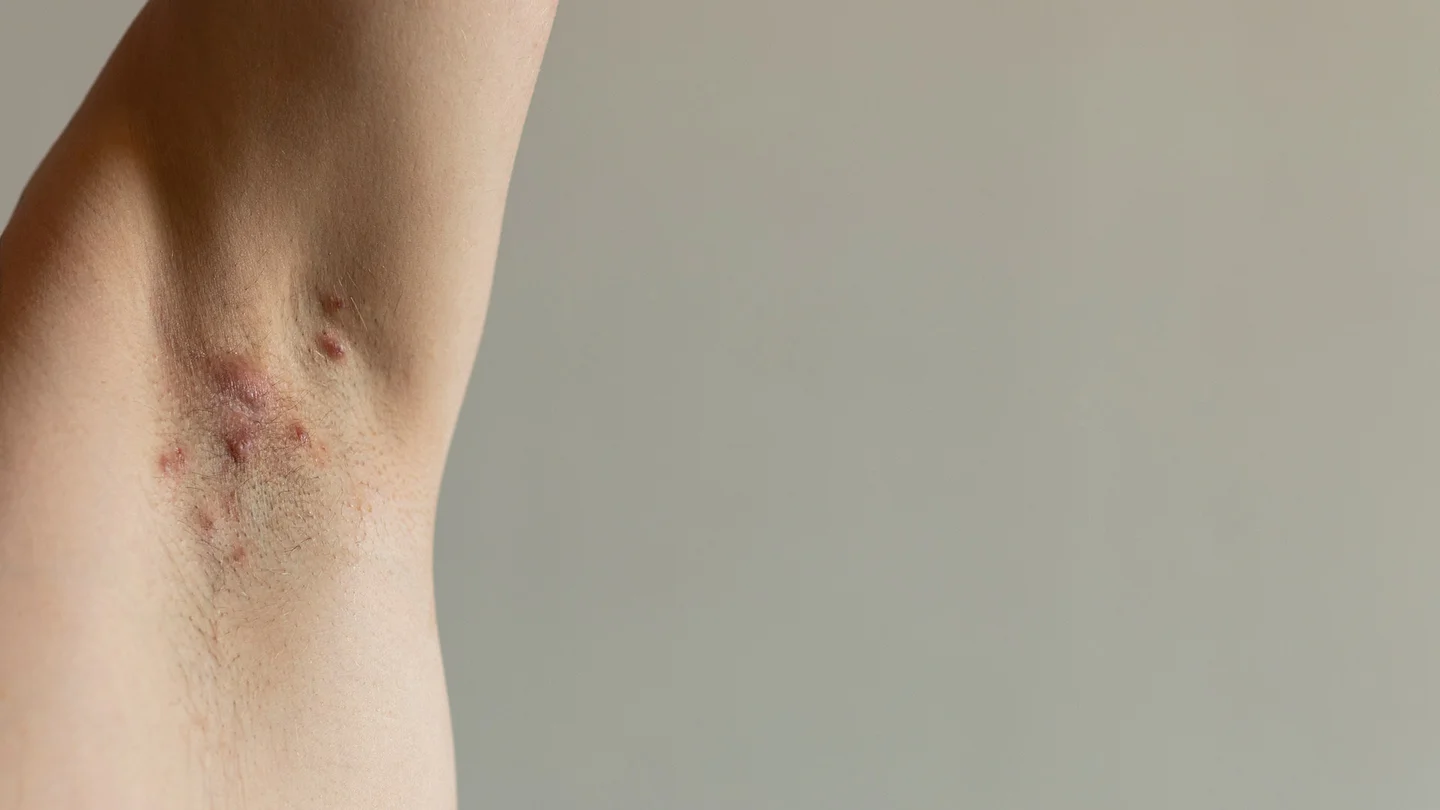
What is acne inversa?
Acne inversa – also known as hidradenitis suppurativa – is a chronic inflammatory hair follicle condition. Hair follicles are the structures that surround the hair roots. They consist of connective and skin tissue.
In the case of acute acne inversa, the inflammation of hair follicles results in recurrent nodules, abscesses and even cavities under the skin known as fistula tracts. This severely damages the skin and often causes scarring.
Acne inversa not only causes physical symptoms but can also result in psychological stress. Some people withdraw from their social environment or develop depression.
Several treatment methods can help to alleviate the symptoms and slow the condition’s progress. To date, however, there is no known cure.
Important: Acne inversa is not caused by poor hygiene and is not contagious.
What are the symptoms of acne inversa?
With acne inversa, the hair follicles regularly become inflamed. This results in the formation of:
- blackheads and pustules
- deep-seated nodules of half to two centimeters in diameter
- cysts (cavities in the tissue)
- encapsulated collections of pus (abscesses)
- channel-like cavities (fistulas)
- later, also scarring
The inflamed areas are usually very painful and can persist for months. They generally release pus and unpleasant smelling fluid if they are pressed or rupture.
About half of people with acne inversa find that the affected area of skin burns, becomes painful, itches or feels warm some 12 to 48 hours before new inflammation occurs.
Inflammation primarily occurs in the armpits and groin area as well as in the anal and genital areas. However, it can also occur on the buttocks and upper body, especially in the stomach and breast folds.
What causes acne inversa?
Acne inversa starts with hair follicle inflammation. This leads to the follicles becoming clogged and being no longer able to externally release the sebum that they produce. If they ultimately rupture under the skin, the accumulated content enters the surrounding tissue. The inflammation spreads. Skin structures such as sweat glands and connective tissue can also be damaged. Abscesses and fistula tracts can subsequently form.
It is not known why the hair follicles become inflamed.
The following are thought to play a role:
- Genetic predisposition: in about 40 percent of people with acne inversa, there is a family history of the condition. Certain genes can increase the risk of the condition’s development.
- Influence of hormones: it is believed that certain hormones promote the condition as acne inversa is far more common in women than men. Furthermore, the condition in women occurs between puberty and menopause.
- Impaired immune system: disorders that affect the body’s own defense system are also suspected to trigger the condition.
Research to date has shown that the condition is not caused by bacteria.
What are the risk factors for acne inversa?
The precise causes of acne inversa are unknown. However, it is known that the risk is higher in children if a parent already has a history of the condition. This indicates a family predisposition.
How common is acne inversa?
According to estimates, up to 4 percent of people worldwide have acne inversa. The condition usually manifests itself between the ages of 11 and 50. It is three times as common in women as in men.
What long-term effects are possible with acne inversa?
Acne inversa can have both physical and mental long-term effects – especially if not treated early.
The changes and damage to the skin can cause chronic pain and restrict mobility. Anemia, high protein levels in the blood and joint disorders are also possible.
In the long term, acne inversa can also increase the risk of a certain form of non-melanoma skin cancer. However, this is very rare.
The chronic pain, the unpleasant odor and the skin’s appearance can severely impair people’s quality of life and affect their mental health. Some people with severe acne inversa develop depression among other conditions.
How is acne inversa diagnosed?
In the initial stage, acne inversa is often mistaken for other conditions. As a result, it can often take several years to obtain a diagnosis.
There are no tests or examination methods that enable a clear diagnosis. A detailed medical consultation and an examination of the skin are therefore essential.
The doctor will ask:
- when the symptoms first appeared and how long they have persisted;
- whether the pain temporarily goes away and later returns;
- whether there is a family history of acne inversa.
The appearance of the affected areas of skin will subsequently be examined to see if the inflammation is deep-seated, painful or has caused scarring.
Depending on the appearance, acne inversa is divided into three stages:
- Stage 1 (mild): single abscesses without fistula tracts and scarring
- Stage 2 (moderate): one or more recurrent abscesses with fistula tracts and scarring
- Stage 3 (severe): interconnecting abscesses with several fistula tracts and scarring, widespread area of skin affected
How can acne inversa be treated?
Medication can help to alleviate the symptoms of acne inversa, extend the intervals between episodes and prevent the condition from progressing. To this end, it is important to consult a doctor about new inflammation as soon as possible. The type of treatment depends on the severity of the condition. There is no cure for acne inversa.
Doctors use painkillers in the form of ointments or tablets to treat the pain. Antibacterial and anti-inflammatory ointments or tablets are also prescribed, especially for mild and moderate cases. A further option is hormone therapy, for example in the form of the birth control pill for women. The inflamed areas sometimes need to be surgically removed.
There are also other treatment options such as laser therapy. In many cases, multiple treatment methods are combined.
What is the best way to deal with acne inversa on an everyday basis?
For people with acne inversa, it helps to maintain a healthy diet and a normal body weight. It is also beneficial to give up smoking. Loose, skin-friendly clothing can furthermore prevent irritated skin.
Although the condition is not caused by poor personal hygiene, it could still be useful to use a disinfectant, antiseptic body wash for the areas of the body most at risk.
Acne inversa can severely affect people’s quality of life. Many people experience severe pain or feel ashamed of their skin. Psychological treatment can be important for helping prevent additional medical conditions such as depression.
If people regularly feel low due to the condition, they can obtain psychotherapeutic support or attend a self-help group and talk to others with acne inversa.
Information about psychotherapy and how to find a therapy place can be found at gesundheitsinformation.de.
- Ballard K, Shuman VL. Hidradenitis Suppurativa. [Updated Aug 11 2021]. In: StatPearls [Internet]. Treasure Island (FL). StatPearls Publishing; 2021 Jan-. Aufgerufen am 11.03.2021.
- DynaMed (Internet), Ipswich (MA). Hidradenitis Suppurativa. EBSCO Information Services. Record No. T115217. 2018 (1995). Aufgerufen am 11.03.2021.
- Ingram JR, Collier F et al. British Association of Dermatologists guidelines for the management of hidradenitis suppurativa (acne inversa) 2018. Br J Dermatol. 2019 May;180(5):1009-1017. doi: 10.1111/bjd.17537. Epub 2019 Mar 11. PMID: 30552762.
- UpToDate (Internet). Hidradenitis suppurativa: Management. Wolters Kluwer 2021. Aufgerufen am 11.03.2021.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: