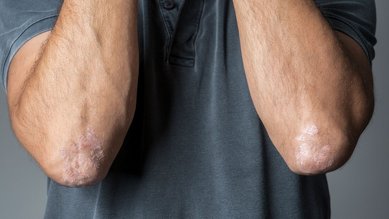
Conditions Dry skin
ICD codes: L85.3 What are ICD codes?
Dry skin not only affects many people’s wellbeing – it can also act as a port of entry for more serious conditions. Numerous factors influence the skin’s condition. Changes in behavior and appropriate care often help, but sometimes medical advice is also needed.
At a glance
- If the skin is too dry, its protective barrier function is disrupted. Damaging influences are then more difficult to ward off.
- Dry skin contains too few hygroscopic (i.e., moisture-retaining) factors and fats.
- A feeling of tightness, flaking, cracks and redness are all signs of dry skin.
- Numerous external and internal factors influence the skin’s condition.
- Making small changes in behavior and personal care often helps make the skin softer and more supple.
- Dry skin can also be a symptom of other conditions, and medical advice should be sought in this case.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What does it mean to have dry skin?
Dry skin develops when the skin does not produce enough fats and hygroscopic (moisture-retaining) substances. This makes the skin tight, chapped and sensitive. It may flake, form wrinkles, turn red and become inflamed. A number of different things can cause dry skin. It may be hereditary, caused by external factors, the result of other conditions or a side effect of medication.
What functions does healthy skin perform?
The skin is the largest organ of the body. It forms a protective barrier between the body and the outside world and has many functions:
- As a mechanical barrier, the skin provides protection from contact with harmful substances and germs.
- It regulates body temperature by increasing or decreasing blood flow and producing more or less sweat.
- Varying amounts of fluid can evaporate through the skin. Since salts dissolved in the fluid are released at the same time, the skin influences the body’s water and electrolyte balance.
- There are many sensory cells in the skin that measure touch, pressure, temperature and pain, and so it provides important information about the environment.
A healthy stratum corneum (the outermost “horny” layer of the skin) is particularly important for a functioning barrier between the skin and the environment. Various factors have to come together to achieve this:
- The skin must produce enough hygroscopic factors for moisture to be bound in the horny cells.
- The fatty layer between the horny cells must be intact and have the right composition so that only a small amount of water evaporates and no water and no irritants can penetrate from outside.
- Sebaceous glands produce what is known as sebum or sebaceous matter – a mixture of fats, proteins and hydrocarbons. It is released on the surface of the skin and supports the barrier function.
- The horny cells must be well connected so that there are no “holes” in the horny layer.
- The skin also has a protective acid mantle consisting of a thin film of fats, shed horny cells and sweat. The acid milieu offers the ideal environment for the body’s own bacterial flora that protect the skin from disease pathogens.
- The skin’s metabolic enzymes that regularly renew the horny layer and produce fats (lipids) in the skin work best in an acidic environment.
Important: An optimal composition of the fatty layer and sufficient production of hygroscopic factors are especially important for the skin’s barrier function. Age, heredity, the body’s own hormones, diet and seasonal changes play an important role in this regard.
What does dry skin look like?
Typical signs of dry skin are:
- tightness
- roughness, flaking
- redness
- fine cracks
- itching, pain
Some regions of the body are particularly prone to dry skin, i.e., the face, hands, forearms and elbows and shin bones and feet. Dry skin is thin and easily irritated.
What causes dry skin?
Dry skin is mainly a problem of the top layer of the skin, known as the stratum corneum or horny layer. There are numerous external and internal factors, as well as some health conditions and medication that can lead to dry skin.
External factors
- Environmental factors such as cold, wind, low humidity, dry heating air in the winter and strong sunlight can easily dry out the skin.
- Jobs or hobbies where the skin often comes into contact with moist or skin-damaging substances take their toll on the skin. This affects hairdressers, construction workers, nursing staff, cleaning staff and swimmers, for example.
- Unusual washing behavior, such as long, hot showers or very frequent baths, can be harmful to the skin. The use of alkaline soap, disinfectants with high alcohol content and detergents can also lead to dry skin.
Internal factors
- Older age, hereditary factors and changes in hormone balance, such as those that occur during menopause for example, influence the skin’s condition and often lead to dry skin.
- Diet-related causes, such as malnutrition or dehydration (which can develop due to insufficient fluid intake as well as excessive sweating) also play a role.
- Smoking damages the skin by impairing blood circulation, meaning that the skin receives too few nutrients to form a healthy barrier against the outside world.
- Psychological and emotional stress can also have a negative effect on the structure and thus the protective function of the individual skin layers.
Conditions
- Skin conditions, such as neurodermatitis, allergic contact eczema, psoriasis, erysipelas, hereditary keratosis and fungal, parasitic or bacterial infections, are associated with dry skin. After an acute inflammation, flaking is part of the healing process of the skin.
- Dry skin can appear as an accompanying symptom of internal conditions such as diabetes, diseases affecting the kidneys, liver, gallbladder, intestines and thyroid and cancer.
- Psychiatric conditions such as obsessive compulsive disorder can involve a compulsion to wash hands, thereby disrupting the skin’s barrier function. Anorexia and other addictive disorders can lead to a lack of nutrients.
Medication
- Dry skin can be a side effect of certain types of medication, such as cortisone, diuretic drugs, cholesterol-lowering drugs, hormonal contraceptives and some chemotherapy drugs.
How common is dry skin?
It is estimated that dry skin affects around 10 million people in Germany every year. About one in three working adults suffer from dry skin, with women and men being affected to roughly the same extent.
The risk of dry skin increases with age. Almost all older people and people in need of care have dry skin.
What can be done to treat dry skin?
Since dry skin leads to barrier disruption, this also makes other skin conditions more likely to develop. This is why good skin care is important. For example, it can prevent bedsores or skin ulcers, especially for older people and those in need of care.
Those affected with dry skin should take the following measures:
- Suitable care products include mild, non-alkaline soaps and lipid-replenishing baths, shampoos and creams – ideally without allergens and perfumes.
- A full bath should not last longer than 5 minutes. Showers that are too frequent, too long and too hot damage the skin. Afterwards, the skin should be re-moisturized and replenished.
- The skin’s condition can also be improved by following a balanced diet and staying hydrated. Those affected should avoid nicotine and alcohol.
- Loose clothing, if possible made of cotton, is gentle on irritated skin. If the skin on the person’s hands is irritated, they can use protective gloves with cotton lining.
- The skin needs protection from dry, hot or very cold climates. Those affected should avoid large temperature fluctuations and strong sunlight.
- Relaxation also helps, as excitement and stress can have a negative impact on the skin.
- If a person has dry skin, they should dry themselves well after getting wet. This is because the evaporation of residual moisture also dries out the skin.
When should people see a doctor?
People should seek medical help if:
- the skin continues to dry out despite appropriate care measures
- the skin flakes a lot and there is severe itching or even pain
- there are inflamed, weeping areas of the skin, crusts that don’t heal, or a skin rash develops
- additional signs of illness, such as hair loss, headache, dizziness, weight loss, significant thirst, frequent urination or fever, are present
- the dry skin occurred shortly after taking a new medication
What do doctors do?
Doctors will first ask when and in what context the dry skin developed and what factors improve the skin’s condition or make it worse. Next, they will take a close look at the affected areas of skin. At this point, they can usually make a diagnosis. If they assume that another underlying condition is present, appropriate testing (for example, a blood test) will be carried out.
What does medical treatment involve?
Dry skin disrupts the skin’s barrier function, resulting in allergens, pollutants and pathogens such as bacteria, viruses and fungi penetrating the skin and possibly leading to serious complications. This is why it is important to medically treat dry skin if its condition is not improved by following general recommendations.
Depending on the skin’s condition, doctors choose the appropriate primary treatment, consisting of varying proportions of re-moisturizing and lipid-replenishing ingredients:
- Re-moisturizing ingredients include, for example, glycerine or urea. They increase the quantity of moisturizing factors that bind moisture in the top layer of the skin.
- Lipid-replenishing substances, such as ceramides, cholesterol, free fatty acids and components of natural oils, can replenish the fatty layer between the horny cells.
- Filmogenic (i.e., film-forming) substances, such as oils, fats and waxes based on mineral or silicone oil, are not absorbed into the skin, but form a protective film on the skin, thereby supporting its barrier function. Filmogenic substances based on mineral oil also increase the skin’s water content.
Ingredients that calm the irritated skin and itching can also be added to the primary treatment:
- Skin-soothing substances include, for example, licochalcone A, dexpanthenol, oat extract and bisabolol.
- Antipruritic (itch-relieving) ingredients include, for example, polidocanol, substances that activate the cold receptors in the skin (e.g., menthol) and N-Palmitoylethanolamide.
Those affected should also consider their personal preferences when making their choices to ensure that they will actually use the products. These preferences include, for example, scent, how easy the product is to apply to the skin and how the skin feels after the product has been absorbed.
- Augustin M, Wilsmann-Theis D, Körber A, Kerscher M, Itschert G, Dippel M, Staubach P. Positionspapier der Deutschen Dermatologischen Gesellschaft: Diagnostik und Therapie der Xerosis cutis. J Dtsch Dermatol Ges 2018. 16(S4). Aufgerufen am 19.11.2020.
- Peters EM. Stressed skin?--a molecular psychosomatic update on stress-causes and effects in dermatologic diseases. J Dtsch Dermatol Ges. 2016 Mar;14(3):233-52. Aufgerufen am 21.12.2020.
- Tončić RJ, Kezić S, Hadžavdi SL, Marinović B. Skin barrier and dry skin in the mature patient. Clin Dermatol 2018. 36(2): 109-115. Aufgerufen am 19.11.2020.
Reviewed by the German Dermatological Society (Deutsche Dermatologische Gesellschaft e.V.).
As at: