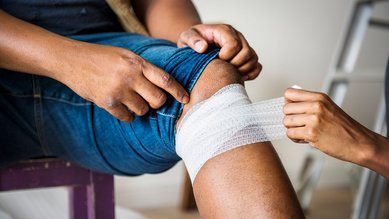
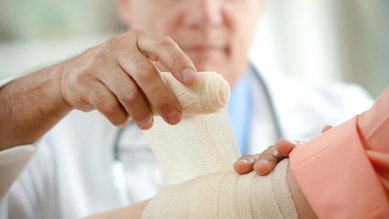
Conditions Erysipelas and cellulitis
ICD codes: A46 L03 What are ICD codes?
Bacteria can penetrate injured skin and cause an infection. While erysipelas usually only affects the upper layers of skin, cellulitis goes deeper into the tissue. A complete recovery without any complications is usually possible for both types of infection, provided that they are treated as soon as possible.
At a glance
- When the skin is injured, an infection may occur due to the entry of bacteria.
- Erysipelas usually only occurs in the upper skin layers.
- In contrast, cellulitis goes deeper into the tissue.
- With both infections, the skin becomes swollen, red, and painful.
- With prompt treatment, a complete recovery without any complications is usually possible.
- The feet and lower legs are the areas most commonly affected.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is erysipelas and what is cellulitis?
Both erysipelas and cellulitis can occur if bacteria break through the skin barrier due to an injury. The skin becomes swollen, red, and painful. If only the upper layers of the skin are affected, this is generally due to erysipelas, which is sometimes called “St. Anthony’s fire”. In contrast, cellulitis – sometimes also referred to as a phlegmonous infection or simply as “phlegmons” – usually goes deeper into the tissue. With proper treatment administered as soon as possible, a complete recovery from both types of infection is almost always possible without any complications. However, severe complications can arise if they are left untreated.
Erysipelas and cellulitis are the two medical terms used to describe bacterial skin infections. It should be noted that the term cellulitis has nothing to do with cellulite, a harmless condition also known as “orange peel skin”.
What are the symptoms of a bacterial skin infection?
The following infections are caused by bacteria penetrating the skin and soft tissues:
- erysipelas
- cellulitis
These infections occur most frequently in the feet and lower legs but they may also occur in other areas of the body. Facial erysipelas is erysipelas that occurs on the face, for example. Cellulitis can occur on the palm of the hand, where it spreads in a V-shape in the synovial tendon sheaths between the thumb, wrist, and little finger.
With erysipelas in the upper skin layers, a painful, light red, shiny swelling is typical. The boundaries of the inflammation are relatively clearly defined. Red streaks leading from the area indicate that the infection is spreading along the lymph vessels. Blisters may also form in severe cases. Nearby lymph nodes are sometimes also affected. If this occurs, they become swollen and sensitive to pressure. In most cases, fever and a general feeling of being unwell occurs as soon as the skin starts to become red.
In cases of cellulitis, the infection usually penetrates deeper layers of the skin and the underlying tissue. As a result, the infection can spread along the tendons and muscles, in some cases causing pus to form.
Both types of infection are usually painful and cause swelling of the inflamed skin and connective tissue. Fever and a general feeling of being unwell are typical of erysipelas, but may also occur in severe cases of cellulitis.
What causes erysipelas and cellulitis?
Erysipelas is frequently caused by streptococcus bacteria, while cellulitis is usually caused by staphylococcus bacteria. However, both groups of bacteria can be involved in both types of infections.
It is easier for bacteria to penetrate the skin if the skin is already damaged. Because of this, skin disorders such as neurodermatitis, impetigo, fungal infections like athlete’s foot, or wounds and ulcers all increase the risk of an infection. Erysipelas and cellulitis can also develop after injuries, needle punctures, and insect or animal bites. Surgery also increases the risk of germs entering the wound.
The risk of infection is especially high if the immune system is weakened. This can occur, for example, due to certain medications, such as cortisone, some cancer drugs, and medication used following an organ transplant.
In addition, the risk is increased in people who have diabetes, are overweight, suffer with lymph drainage or circulatory disorders, or have venous insufficiency. A previous erysipelas or cellulitis infection is another risk factor.
How can erysipelas and cellulitis be prevented?
With both erysipelas and cellulitis, a recurrence of the infection often occurs, even if the initial treatment was completely successful. Approximately one-third of people experience re-infection.
There are various ways to prevent this from happening. If the infection is caused by a skin disorder such as athlete’s foot or neurodermatitis, treating these issues will reduce the risk of recurring infections. In cases where the risk of infection is higher due to diabetes or circulatory disorders, good foot care and foot hygiene is essential.
Doctors may consider preventive treatment with antibiotics in the case of recurring bacterial skin infections. These need to be taken daily over a period of several months.
For more detailed information about preventing erysipelas and cellulitis (for example, determining whether antibiotics can help), visit gesundheitsinformation.de.
How are erysipelas and cellulitis diagnosed?
Erysipelas and cellulitis can normally be diagnosed based on the typical symptoms and the appearance of the skin. The patient’s medical history and details of prior injuries will also help in the diagnosis.
Further testing is not usually required. However, this may be useful if the doctor suspects that a specific pathogen (germ) has triggered the inflammation, for example, after a dog bite.
How are erysipelas and cellulitis treated?
Antibiotics are used to treat erysipelas and cellulitis. In mild infections, these can be taken in tablet form but, in more severe cases, they are delivered directly into the vein using a drip. If hospitalization is required, patients usually stay for about a week.
The precise antibiotic used depends on a number of factors, including the specific pathogen that is suspected of triggering the inflammation. To track the progress of the treatment and determine whether the infection and reddening is reducing, the infected area of skin is outlined with a pen.
To relieve the symptoms, it is recommended that the swelling be kept cool and that moistened antiseptic wipes be applied. Anti-inflammatory painkillers, such as ibuprofen, are effective in treating pain and fever.
- Dalal A, Eskin-Schwartz M, Mimouni D et al. Interventions for the prevention of recurrent erysipelas and cellulitis. Cochrane Database Syst Rev 2017; (6): CD009758. doi: 10.1002/14651858.CD009758.pub2. PMID: 28631307; PMCID: PMC6481501.
- Kilburn SA, Featherstone P, Higgins B et al. Interventions for cellulitis and erysipelas. Cochrane Database Syst Rev 2010; (6): CD004299. doi: 10.1002/14651858.CD004299.pub2. PMID: 20556757; PMCID: PMC8693180.
- Moll I. Duale Reihe Dermatologie. Stuttgart: Thieme; 2016.
- Oh CC. Cellulitis and erysipelas: prevention. BMJ Clin Evid. 2015 Nov 18;2015:1708. PMID: 26580894; PMCID: PMC4651026.
- Oh CC, Ko HC, Lee HY et al. Antibiotic prophylaxis for preventing recurrent cellulitis: a systematic review and meta-analysis. J Infect 2014; 69(1): 26-34. doi: 10.1016/j.jinf.2014.02.011. Epub 2014 Feb 24. PMID: 24576824.
- Phoenix G, Das S, Joshi M. Diagnosis and management of cellulitis. BMJ 2012; 345: e4955. doi: 10.1136/bmj.e4955. PMID: 22872711.
- Quirke M, Ayoub F, McCabe A et al. Risk factors for nonpurulent leg cellulitis: a systematic review and meta-analysis. Br J Dermatol 2017; 177(2): 382-394. doi: 10.1111/bjd.15186. Epub 2017 Jul 25. PMID: 27864837.
- Stevens DL, Bisno AL, Chambers HF et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014; 59(2): e10-52. doi: 10.1093/cid/ciu444. Erratum in: Clin Infect Dis. 2015 May 1;60(9):1448. Dosage error in article text. PMID: 24973422.
- Stevens DL, Bryant AE. Impetigo, Erysipelas and Cellulitis. Oklahoma City (OK): NIH; 2016.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: