Conditions Neurodermatitis
ICD codes: L20 What are ICD codes?
People with neurodermatitis keep getting a rash that usually itches badly. This chronic skin condition often occurs in children, but often fades away after a couple of years. It is rare in adults. Find more here about the causes, risk factors, and treatment options.
At a glance
- Neurodermatitis is a chronic, non-infectious skin condition.
- The rashes itch badly and usually occur episodically.
- Neurodermatitis often occurs in children and often improves over the years.
- A little over one-third of people with neurodermatitis have an allergic form of the condition.
- Acute symptoms can be treated successfully with cortisone ointments and creams.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is neurodermatitis?
Neurodermatitis is a chronic inflammatory skin condition. It usually occurs episodically. Typical symptoms are a rash and severe itching. Neurodermatitis is particularly common in children and is non-infectious. The allergic form is referred to as “atopic dermatitis” or “atopic eczema”.
Symptoms often improve over the years, or sometimes disappear completely. Careful skincare, medication and avoidance of irritating materials and allergy triggers can usually alleviate the symptoms so that people affected can live a largely normal life.
However, acute symptoms can severely impair the quality of life. The itching often makes it very difficult for people with neurodermatitis to sleep, and impairs their ability to concentrate. Some people are also ashamed because of the rash.
Video What is neurodermatitis and what treatment is available?
The video below shows the signs of neurodermatitis and what can be done to mitigate it.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
How can neurodermatitis be identified?
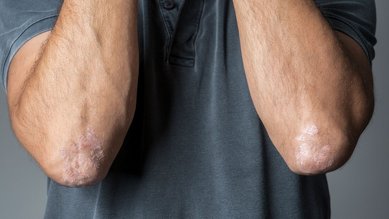
The main characteristic of neurodermatitis is the nagging itching. When the symptoms are acute, the skin becomes red and itchy. Sometimes blisters form that can easily expand and then weep.
Over the longer term the skin dries up, and becomes cracked and thicker at the sites affected. Various rashes and skin changes can also occur simultaneously.
Neurodermatitis normally occurs episodically. This means that sometimes less severe or scarcely any symptoms occur, while in other phases the symptoms are severe. The skin is only rarely inflamed over the long term.
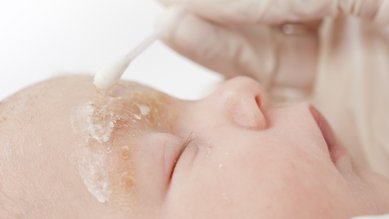
In babies it is mainly the cheeks and the outside of the arms and legs that are affected – they get neurodermatitis on their back, stomach and chest more rarely.
In children, adolescents and adults, neurodermatitis occurs mainly in the hollows of the knee, the inside of the elbow, and on the neck. But the surfaces of the hands and the soles of the feet also often show the typical signs of inflammation. There is rarely a rash on the face.
What are the causes of neurodermatitis?
Many factors play a part in neurodermatitis occurring.
With neurodermatitis, the natural skin barrier is damaged by inflammatory reactions in the skin. As a result, the outer layer of the skin’s protection, the horny layer, is unable to sufficiently protect the body.
Changes to the skin flora can also cause neurodermatitis to develop. But heredity also plays a part: an altered gene blocks production of filaggrin, a protein that plays an important role in forming the epidermis. Because it lacks filaggrin, the skin loses moisture and dries out. The damaged skin then provides poorer protection against irritants, substances that trigger allergies (allergens), and germs, and it gets inflamed more quickly. But how the various factors interact is still unclear.
Important: Around 30 to 40 percent of cases of neurodermatitis are allergy-related. Sufferers then also often have more severe skin conditions or hay fever and allergic asthma at the same time. The triggers (allergens) include, for example, house dust mites, pollen, and foods such as milk, eggs, nuts, or fish.
But non-allergenic substances and certain environmental conditions can also irritate the skin. These include, for example: extreme heat or cold, coarse textiles made from rough wool, or cigarette smoke.
What are risk factors for neurodermatitis?
A predisposition within the family substantially increases the risk of neurodermatitis. But there are other factors that contribute to neurodermatitis occurring. As the condition has become more common in recent decades, other risk factors apart from heredity are presumed.
Both environmental pollution and excessive hygiene could be reasons behind an increase in neurodermatitis. The hygiene theory is based on the observation that children with a lot of brothers and sisters get neurodermatitis less frequently, as do those who attended a kindergarten as a baby or who grew up with a dog. These children come into contact with germs at an earlier age and more frequently, so their immune system is better trained.
How common is neurodermatitis?
Around 15 percent of children get neurodermatitis. In adults the figure is only 2 to 5 percent. However, adults often have a more severe form of the condition.
How does neurodermatitis develop?
In most children, neurodermatitis begins within their first two years, typically between their third and sixth months. There are also children who only develop neurodermatitis later. It is rare for the condition to begin after the age of five.
How the neurodermatitis evolves depends, among other factors, on the person’s age. Only 50 percent of children who have the condition within their first year still have neurodermatitis after 3 years.
In children who develop neurodermatitis between the ages of 2 and 5, it usually lasts longer. According to estimates, though, in over 80 percent of all children it has disappeared or become far less severe around 10 years after it first appeared.
In some people, the neurodermatitis reappears when they are an adult. Then it is often mainly the hands that are affected. With adults, the neurodermatitis is usually chronic. Phases with more and less severe symptoms alternate.
It is rare that a person first gets the condition as an adult.
Can neurodermatitis be prevented?
As yet there are no measures that could give proven protection against neurodermatitis. While it is true that the risk of neurodermatitis is largely hereditary, it is impossible to say exactly when someone will and will not get neurodermatitis. Because many factors interact to cause it.
To date, there have only been some weak indications of a preventive effect for food supplements with probiotic bacteria.
If babies are breast-fed, their risk of getting the condition might be reduced. However, the results of research into this are not definitive. It is not yet known why children get neurodermatitis. It is only clear that different mechanisms are involved.
As yet it has not been proven whether omitting certain foods alleviates the symptoms in children without a proven food allergy. And there has been very little research into whether elimination diets help with neurodermatitis in adults. Neither has any evidence been produced that the preventive use of skincare products in the first year of life prevents neurodermatitis.
However, getting a child who has neurodermatitis vaccinated is a good idea, because illnesses such as chickenpox can be more severe for neurodermatitis sufferers.
If someone has neurodermatitis, can it help to eliminate certain foods? Find out more at gesundheitsinformation.de.
How is neurodermatitis diagnosed?
There are other skin conditions that can cause similar symptoms to neurodermatitis. Doctors only diagnose it if a severe, itchy rash lasts for months or keeps recurring. The symptoms need to appear at the sites in the body that are typical for the person’s age.
At the same time, other conditions such as psoriasis are ruled out. In babies in particular, neurodermatitis is easily confused with seborrheic dermatitis. Compared with neurodermatitis, this skin disease hardly itches and disappears on its own after a few weeks or months.
Allergy tests have only limited effect when attempting to diagnose neurodermatitis. So if there is no real suspicion, testing on a wide range of substances is not very useful.
How is neurodermatitis treated?
Neurodermatitis is a chronic skin condition, so it cannot be completely cured. However, sound treatment with regular skincare and medication can often effectively alleviate symptoms such as itching and rashes.


The main therapies include:
- Basic care: using oil-replenishing and hygroscopic care products (emollients) will prevent the skin from drying out. This should soothe the itching, protect the skin from germs and irritants, and prevent new outbreaks. The care should be applied twice per day at least.
- Avoiding irritants: many common soaps and products such as shampoos or shower gels contain substances that can dry out the skin. It is worth trying special cleaning products that do not contain these substances. However, basic care using emollients can also compensate for the loss of moisture caused by conventional soaps. The skin may also be irritated by coarse clothing, contact allergens, and extreme cold and heat.
- Cortisone ointments: acute outbreaks are often treated with cortisone ointments (glucocorticoids). They can very effectively alleviate the itching and inflammation. To prevent outbreaks, so-called proactive treatments or interval therapy are also options. In this case, cortisone ointments are applied on 2 days in the week in addition to the basic care. This results in people with neurodermatitis having far fewer outbreaks of acute rashes.
- Pimecrolimus and tacrolimus: these two anti-neurodermatitis agents are applied to the skin as a cream or ointment. They can be used if cortisone is not tolerated or if cortisone treatment has not led to any improvement. Both products can be used, for example, as long-term treatment for sensitive skin in the face and neck area.
Important: Other therapy methods include moist compresses, UV light and drugs that suppress certain reactions in the immune system. These agents are used when other treatments do not help and when the neurodermatitis is very severe or widespread.
Allergy medication (antihistamines) is also used sometimes. This aims to soothe the itching. However, studies have shown that these medications do not help against the neurodermatitis symptoms.
Herbal products or food supplements are also often tried, for example evening primrose oil, dill oil (borage oil), various vitamins and zinc. However, products like these have also shown no effect in studies.
Many other treatments have not yet been researched sufficiently. These include methods such as laser therapies and desensitization. As a result, medical associations do not recommend them.
For more detailed information, for example on skincare and neurodermatitis, go to gesundheitsinformation.de.
What is everyday life with neurodermatitis like?
The extent to which neurodermatitis can make life difficult is often underestimated, including by doctors. A great deal of patience is required to live with the condition and try to find the right treatment. However, over time, most people manage to get on top of their neurodermatitis, both physically and mentally.
Neurodermatitis can also make things very difficult for children. Some days, normal life quickly becomes stressful for both child and parents. However, phases with severe symptoms are usually followed by periods with fewer symptoms – and the neurodermatitis often disappears, or at least improves, as the child grows.
Parents of a child with neurodermatitis can quickly feel overwhelmed or helpless. Special neurodermatitis training courses have been developed to support families. With cases of severe neurodermatitis, outpatient or inpatient rehabilitation may also be an option.
What else should I know?
There is more information on neurodermatitis at allergieinformationsdienst.de (in German).
- Chalmers JR, Haines RH, Bradshaw LE et al. Daily emollient during infancy for prevention of eczema: the BEEP randomised controlled trial. Lancet. 2020 Mar 21;395(10228):962-972. doi: 10.1016/S0140-6736(19)32984-8. Epub 2020 Feb 19. PMID: 32087126; PMCID: PMC7086156.
- Evans I, Thornton H, Chalmers I et al. Wo ist der Beweis? Plädoyer für eine evidenzbasierte Medizin. Hans Huber: Bern 2013.
- Garcia-Larsen V, Ierodiakonou D, Jarrold K et al. Diet during pregnancy and infancy and risk of allergic or autoimmune disease: A systematic review and meta-analysis. PLoS Med. 2018 Feb 28;15(2):e1002507. doi: 10.1371/journal.pmed.1002507. PMID: 29489823; PMCID: PMC5830033.
- Kim JP, Chao LX, Simpson EL et al. Persistence of atopic dermatitis (AD): A systematic review and meta-analysis. J Am Acad Dermatol. 2016 Oct;75(4):681-687.e11. doi: 10.1016/j.jaad.2016.05.028. Epub 2016 Aug 17. PMID: 27544489; PMCID: PMC5216177.
- Langan SM, Irvine AD, Weidinger S. Atopic dermatitis. Lancet. 2020 Aug 1;396(10247):345-360. doi: 10.1016/S0140-6736(20)31286-1. Erratum in: Lancet. 2020 Sep 12;396(10253):758. PMID: 32738956.
- Lu CL, Liu XH, Stub T, Kristoffersen AE et al. Complementary and alternative medicine for treatment of atopic eczema in children under 14 years old: a systematic review and meta-analysis of randomized controlled trials. BMC Complement Altern Med. 2018 Sep 26;18(1):260. doi: 10.1186/s12906-018-2306-6. Erratum in: BMC Complement Altern Med. 2019 Jan 14;19(1):16. Araek T [corrected to Alræk. T]. PMID: 30257693; PMCID: PMC6158902.
- Matterne U, Böhmer MM, Weisshaar E, Jupiter A, Carter B, Apfelbacher CJ. Oral H1 antihistamines as 'add-on' therapy to topical treatment for eczema. Cochrane Database Syst Rev. 2019 Jan 22;1(1):CD012167. doi: 10.1002/14651858.CD012167.pub2. PMID: 30666626; PMCID: PMC6360926.
- Schindler T, Sinn JK, Osborn DA. Polyunsaturated fatty acid supplementation in infancy for the prevention of allergy. Cochrane Database Syst Rev. 2016 Oct 28;10(10):CD010112. doi: 10.1002/14651858.CD010112.pub2. PMID: 27788565; PMCID: PMC6464137.
- Skjerven HO, Rehbinder EM, Vettukattil R et al. Skin emollient and early complementary feeding to prevent infant atopic dermatitis (PreventADALL): a factorial, multicentre, cluster-randomised trial. Lancet. 2020 Mar 21;395(10228):951-961. doi: 10.1016/S0140-6736(19)32983-6. Epub 2020 Feb 19. Erratum in: Lancet. 2020 Mar 21;395(10228):e53. PMID: 32087121.
- Van Zuuren EJ, Fedorowicz Z, Christensen R et al. Emollients and moisturisers for eczema. Cochrane Database Syst Rev 2017; (2): CD012119.
- Williams HC, Chalmers J. Prevention of Atopic Dermatitis. Acta Derm Venereol. 2020 Jun 9;100(12):adv00166. doi: 10.2340/00015555-3516. PMID: 32419030.
- Zhang Y, Lin J, Zhou R, Zheng X, Dai J. Effect of omega-3 fatty acids supplementation during childhood in preventing allergic disease: a systematic review and Meta-Analysis. J Asthma. 2020 Jan 10:1-14. doi: 10.1080/02770903.2019.1709866. Epub ahead of print. PMID: 31880179.
- Zhu Z, Yang Z, Wang C, Liu H. Assessment of the Effectiveness of Vitamin Supplement in Treating Eczema: A Systematic Review and Meta-Analysis. Evid Based Complement Alternat Med. 2019 Oct 31;2019:6956034. doi: 10.1155/2019/6956034. PMID: 31781276; PMCID: PMC6875217.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at: