Conditions Seborrheic dermatitis
ICD codes: L21 What are ICD codes?
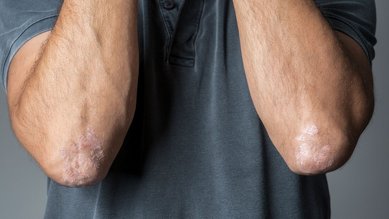
Red patches of skin with oily flakes on the scalp and face are typical of seborrheic dermatitis. The severity of these symptoms can vary during each recurrence. Men are more often affected by this condition than women. Seborrheic dermatitis is a non-contagious inflammation of the skin. Special creams and shampoos are available to relieve the symptoms.
At a glance
- Seborrheic dermatitis is a non-contagious inflammation of the skin.
- It is considered a chronic form of eczema.
- It causes red patches with oily flakes to form on the face and scalp in particular. These patches are rarely itchy.
- Medical practitioners assume that this type of eczema is caused by factors such as seborrhea, i.e., increased production of sebum (skin oil), microorganisms on the skin (e.g., fungi), or a weakened immune system.
- If an individual develops seborrheic dermatitis for the first time during puberty or as an adult, it usually becomes a recurring condition.
- In many cases, it is helpful to apply anti-fungal agents or creams containing cortisone to the affected skin areas.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is seborrheic dermatitis?
Seborrheic dermatitis is sometimes also called seborrheic eczema or seborrheic psoriasis. This non-contagious skin inflammation causes the formation of red patches of skin with oily flakes, especially on the scalp and face. These patches are not normally itchy. Medical practitioners assume that, in addition to seborrhea, i.e., increased production of sebum (skin oil), this type of eczema is also caused by factors such as microorganisms on the skin (e.g., fungi) or a weakened immune system.
People who develop the flaky rash for the first time as an adolescent or adult usually experience later recurrences of the condition. It is often helpful to treat the affected skin areas with anti-fungal agents or creams containing cortisone. On the other hand, if the eczema develops during the first few months of life, it usually disappears by itself within a year and doesn’t recur.
What are the symptoms of seborrheic dermatitis?
Skin patches covered in yellowish, shiny, oily flakes are typical of seborrheic dermatitis. The patches appear red on paler skin. On darker skin, the flaky areas appear as lighter patches. Itching is rare with this condition.
These patches develop in particular on areas of the skin that have a large number of sebaceous (oil-producing) glands, such as:
- the scalp and hairline
- on and between the eyebrows
- on the cheeks, especially in the folds of skin between the sides of the nose and the corners of the mouth
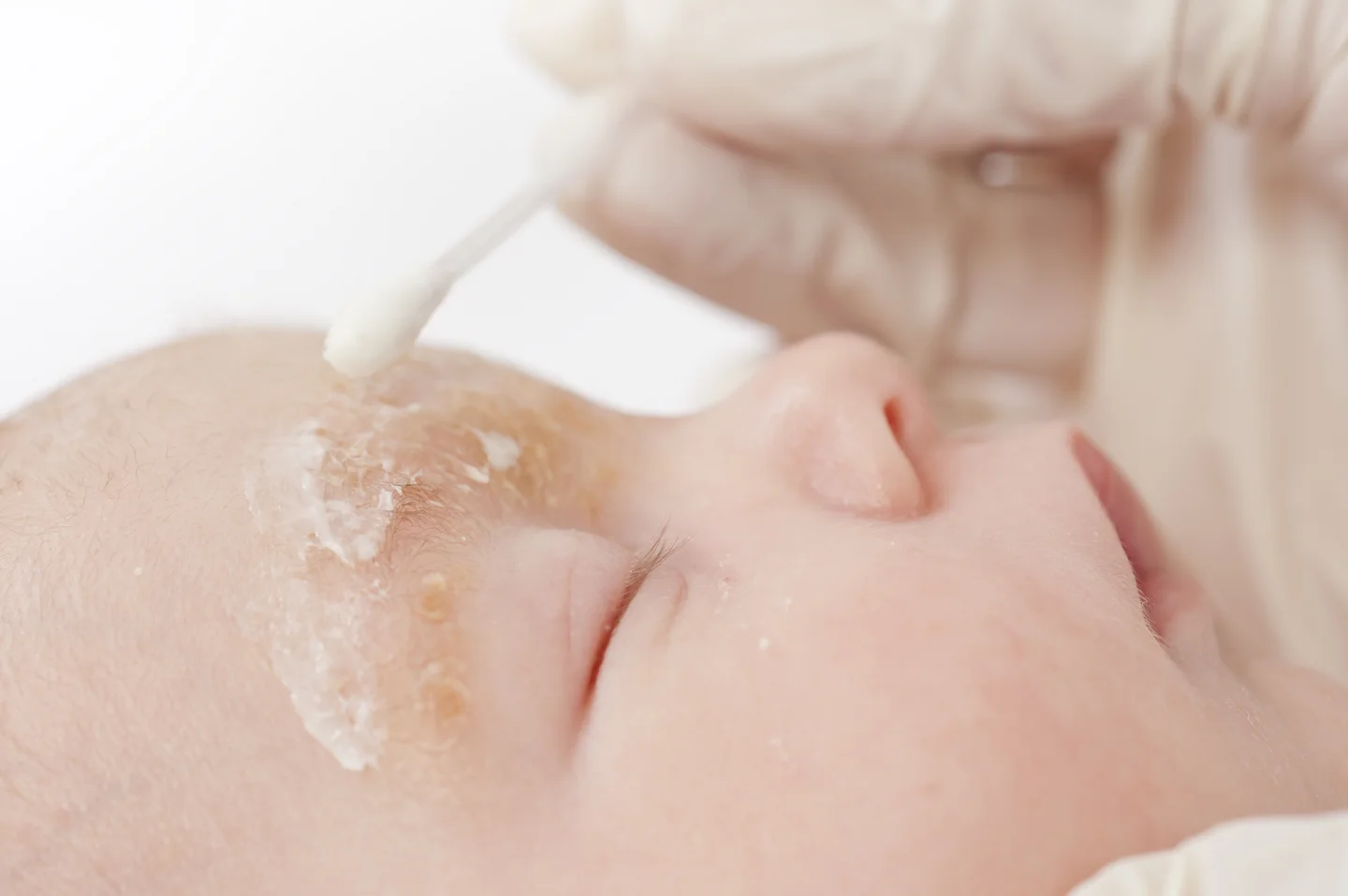
However, the rash may also spread to other parts of the body. In such cases, it most commonly develops above the breastbone and on the back close to the thoracic spine. It can also affect skin folds, for example, under the breasts, in the armpits, or in the groin. In men, the patches occasionally occur in the genital area. In infants and babies, the head is usually affected.
What causes seborrheic dermatitis?
Seborrheic dermatitis is likely to be caused by multiple factors. These include increased production of sebum (skin oil) by the sebaceous glands and growth of a normally harmless yeast called Malassezia furfur on the skin.
Other possible factors include bacteria, stress, genetic predisposition, and hormones. Nervous system disorders such as Parkinson’s disease and a weakened immune system may also play a role. People with a weakened immune system are also at a higher risk of developing a more severe form of seborrheic dermatitis, in which the skin on the entire body is affected. This form is harder to treat.
How common is seborrheic dermatitis?
Seborrheic dermatitis is common, affecting between 3% and 10% of the population. Men are more commonly affected than women. In most people, the flaky rash occurs for the first time when they are young adults or after the age of 50.
The condition is chronic for adolescents and adults. The severity of the symptoms varies with each recurrence. The skin changes may also clear up entirely for a certain period. This is often the case in summer. However, it eventually returns – for example, in winter or during a period of stress.
How is seborrheic dermatitis diagnosed?
A doctor can usually diagnose this condition without difficultly if flaky, red patches that don’t itch appear on the typical sites on the body. In this case, a diagnosis is usually reached after taking the patient’s medical history and performing a physical examination. The doctor will first seek to exclude any other skin illnesses with similar symptoms to seborrheic dermatitis, such as neurodermatitis (atopic dermatitis) or psoriasis. However, these conditions usually cause skin changes in other parts of the body. With neurodermatitis, the inflamed areas are itchy. On pale skin, the red patches also have no clearly defined edges and occasionally have small blisters. On darker skin, the areas affected by neurodermatitis appear even darker than the surrounding skin. In addition, small firm bumps (papules) develop instead of blisters.
Further testing is only rarely necessary. For example, a swab can be taken and sent to a lab to determine whether the patient has a bacterial skin infection such as impetigo. It is not normally necessary to take a biopsy (a sample of tissue).
How is seborrheic dermatitis treated?
Adolescents and adults can apply medicated treatments to the affected areas of the skin. The following are some examples of treatments to relieve the symptoms:
- shampoos containing tar
- creams containing salicylic acid
- anti-fungal creams or shampoos
- anti-inflammatory creams or gels containing cortisone
It is not usually necessary to take any oral medication. Some people with seborrheic dermatitis try phototherapy with UVB light, as sunlight can relieve the symptoms.
To date, no treatment to permanently cure seborrheic dermatitis has been found.
Most infants and babies require no treatment, as the condition tends to resolve by itself.
What is it like to live with seborrheic dermatitis?
Although seborrheic dermatitis is harmless, adolescents and adults may find it difficult to live with. It often causes flaky patches to appear on the face, where they are visible to others. In addition, seborrheic dermatitis can be a life-long condition. People who find it very distressing to live with seborrheic dermatitis can ask their doctor for advice about how to deal better with their condition and reduce their stress, e.g., by attending behavioral therapy.
It is not advisable to try to hide the inflamed areas of skin under a thick layer of make-up, as this causes the pores to become clogged. However, wearing some light make-up now and again won’t do any harm. Mild, non-greasy skin-care products are most suitable for people with this skin condition.
No special sun protection is required – it’s sufficient to use regular, appropriate UV protection based on skin type. Symptoms may also be relieved by exposing the skin to sunlight and fresh air. Non-greasy sunscreen is best.
- Elgash M, Dlova N, Ogunleye T et al. Seborrheic Dermatitis in Skin of Color: Clinical Considerations. J Drugs Dermatol 2019; 18(1): 24-27. Aufgerufen am 14.03.2024.
- Kastarinen H, Oksanen T, Okokon EO, Kiviniemi VV, Airola K, Jyrkkä J et al. Topical anti-inflammatory agents for seborrhoeic dermatitis of the face or scalp. Cochrane Database Syst Rev 2014; (5): CD009446. Aufgerufen am 14.03.2024.
- Moll I. Duale Reihe Dermatologie. Stuttgart: Thieme; 2016.
Naldi L, Diphoorn J. Seborrhoeic dermatitis of the scalp. BMJ Clin Evid 2015: 1713. Aufgerufen am 14.03.2024. - Okokon EO, Verbeek JH, Ruotsalainen JH, Ojo OA, Bakhoya VN. Topical antifungals for seborrhoeic dermatitis. Cochrane Database Syst Rev 2015; (5): CD008138. Aufgerufen 14.03.2024.
- Pschyrembel online. 2023.
- Victoire A, Magin P, Coughlan J et al. Interventions for infantile seborrhoeic dermatitis (including cradle cap). Cochrane Database Syst Rev 2019; (3): CD011380. Aufgerufen am 14.03.2024.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at: