Conditions Polio (poliomyelitis)
ICD codes: A80 B91 G14 What are ICD codes?
Polio is a highly contagious viral disease that can cause permanent paralysis. The disease was common among children in the past. Today, infection can be prevented thanks to vaccines. As a result, polio viruses only occur in a small number of countries. Unvaccinated children and adults can contract the disease.
At a glance
- Polio is a highly contagious viral disease.
- It only occurs in a small number of countries, in particular where hygiene conditions are poor.
- In most cases, there are only mild symptoms or none at all.
- In rare cases, however, the infection can cause permanent paralysis. Polio can cause death if the muscles used in breathing are affected.
- Both children and adults who have not been vaccinated against polio or have not previously had a polio infection can contract the disease.
- There is no treatment for polio. However, vaccination prevents infection. Only inactivated polio vaccines are used in Germany.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
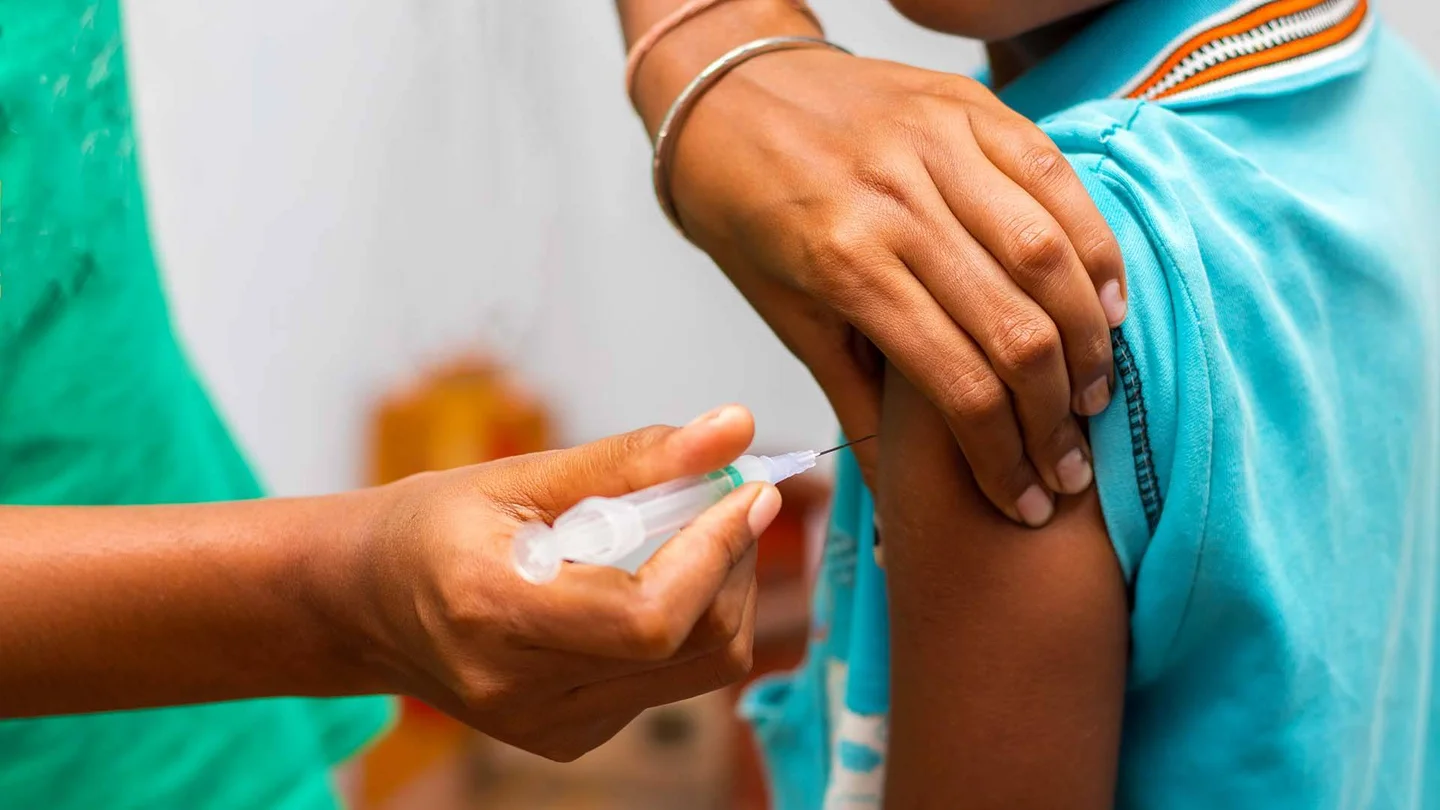
What is polio?
Polio (short for poliomyelitis), which was previously also known as infantile paralysis, is a highly contagious infectious disease. There were many cases of polio and deaths from the disease between 1900 and 1950. The name poliomyelitis is derived from the Latin word for the part of the spinal cord that can be affected by the disease.
Today, polio has been almost completely eradicated across the world thanks to global vaccination campaigns. However, it still occurs in a small number of countries and, with foreign travel, could be carried by people traveling from there to Germany. The risk of infection is particularly high when hygiene conditions are poor. A preventive vaccine will be given to children until the disease is completely eradicated.
Most people who are infected with polio viruses have either mild symptoms or no symptoms at all. However, around 1 in every 200 people infected will suffer from paralysis that does not completely clear up following the infection. If the muscles involved in breathing are affected, this may cause life-threatening respiratory paralysis. Both children and adults who have no immunity can contract the disease.
What are the symptoms of polio?
In over 95 percent of people infected with a polio viruses, there are no symptoms of disease.
If symptoms do occur, there are three different types, which occur in the following sequence:
- Abortive poliomyelitis: this is a mild form that does not involve the nervous system.
- Non-paralytic poliomyelitis: the nervous system is involved but there is no paralysis.
- Paralytic poliomyelitis: the nervous system is involved and paralysis occurs.
Polio not affecting the nervous system
This mild form affects 4 to 8 percent of those infected and is characterized by general symptoms such as nausea, vomiting, diarrhea, high temperature, sore throat, muscle aches and headache.
Polio affecting the nervous system but without paralysis
This occurs in 2 to 4 percent of people infected and its symptoms appear about 3 to 7 days after the mild form begins. The symptoms are high temperature, stiff neck, back ache and muscle cramps.
Polio affecting the nervous system with paralysis
This occurs in 0.1 to 1 percent of people infected and its symptoms appear about 2 to 3 days after the non-paralytic form begins. It causes a renewed increase in temperature and severe pains in the back, neck and muscles. It also causes paralysis. Various leg muscles are often paralyzed. However, muscles in the arms, stomach and eyes and those involved in breathing may also be affected.
What causes polio?
Polio is an infectious disease caused by polio viruses. Polio viruses are enteroviruses that live exclusively in the gastrointestinal tract of humans.
Infection occurs due to fecal contamination – for example, the virus may be contained in fecal particles that are passed from unwashed hands to the mouth. At the start of the infection, the virus multiplies in the throat and can be spread to others in the tiny droplets that are released into the air with a sneeze or cough.
The first symptoms of the disease appear after 3 to 35 days following infection. After an infection, the virus may continue to be present in the stool (feces) for up to 6 weeks. The risk of infection is particularly high in unsanitary conditions. Regular cleaning products are unable to render polio viruses harmless.
How common is polio?
In the past, polio was common worldwide. As children came into contact with these viruses at a very early age, polio was considered a childhood disease. Thanks to vaccines, the virus has been almost entirely wiped out everywhere. Today, the virus is only found in the “wild” in Pakistan and Afghanistan. The last case of infection with a “wild” polio virus in Germany occurred in 1990.
The first polio vaccines used weakened living viruses that provided a good level of immunity. The vaccine was either swallowed directly or taken in a sugar cube. This type of vaccine is called an oral vaccine. The disadvantage of using this type of vaccine with a live virus was that, in rare cases, it could cause vaccine-associated polio. In Germany, there were 1 or 2 cases of vaccine-associated polio each year.
Today, inactivated polio vaccines are used, which also provide a good level of immunity but do not cause any vaccine-associated illness. Only inactivated vaccines have been used in Germany since 1998. In some other countries, the weakened live virus is still used in vaccines, which means that vaccine-associated polio may still occur there and be transmitted to others. In many crisis regions, only a small number of people are fully vaccinated. As a result, larger-scale polio outbreaks can still occur there.
Video How do vaccinations work?
The video below explains how a vaccination works.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What is the outlook for polio?
The mild, non-paralytic form of polio, which does not cause paralysis, can clear up on its own without any lasting effects.
With the paralytic form of polio, the paralysis typically only clears up partially – in other words, the person will not make a full recovery. This form can be fatal if the brain stem – with its vital control centers – or the muscles used in breathing are affected.
For years and even decades after a polio infection, 30 to 40 percent of people suffer muscle wasting with progressive paralysis. Doctors refer to this as post-polio syndrome (PPS).
It is suspected that healthy nerves take over some of the function of the nerves that are damaged by the initial polio virus, so that these originally healthy nerves become overloaded. Chronic overloading then causes further damage and loss of function.
How can polio be prevented?
There is no specific treatment for polio viruses, the pathogens that cause polio. This is why the preventive polio vaccine is so important.
Polio only occurs in a very small number of places in the world today. However, travelers or migrants from these regions may carry polio viruses to other countries with them. The World Health Organization (WHO) aims to wipe out this disease across the globe. Vaccination will be required until polio infections no longer occur.
Germany only uses inactivated viruses in vaccines. These are not capable of causing vaccine-associated polio. The polio vaccine is usually part of the 5-in-1 or 6-in-1 vaccine recommended for infants. Primary vaccination is usually administered via muscle injection at the age of 2, 4 and 11 months. A person is considered fully immunized after receiving a booster vaccine between the ages of 9 and 16. People who receive their primary vaccine in adulthood should receive a booster vaccine after 10 years.
No further polio vaccines are then required. However, an additional booster vaccine may be a good idea before traveling to a region where there is a high risk of infection.
How is polio diagnosed?
Doctors can often recognize polio by the asymmetrical way in which it affects the limbs. In other words, both sides of the body are not equally affected by paralysis.
For a clear diagnosis, however, the polio virus must be detected. This can only be done by testing a stool sample in the lab. Doctors sometimes also take a throat swab or a sample of cerebrospinal fluid (liquor) – the fluid surrounding the spinal cord in the spine.
How is polio treated?
There is no effective medication for an infection with polio viruses. Treatment of polio is limited to supportive measures to relieve the symptoms. In the acute phase of the disease, these include medications to reduce temperature and relieve pain. If the muscles used in breathing are affected by paralysis, mechanical respiratory support will be required.
People with lasting paralysis often receive additional and usually long-term treatments from orthopedic specialists and physiotherapists. The aim is to enable them to walk independently despite their paralysis. The treatment aims to avoid muscle imbalance and joint stiffness.
If a person is suffering from post-polio syndrome (PPS) – a very common complication of a polio infection – endurance training and pain control are other important components of life-long treatment.
- Robert Koch-Institut (RKI). Schutzimpfung gegen Poliomyelitis: Häufig gestellte Fragen und Antworten. Aufgerufen am 10.11.2021.
- Robert Koch-Institut (RKI). RKI-Ratgeber: Poliomyelitis. Aufgerufen am 10.11.2021.
- Wolbert JG, Higginbotham K. Poliomyelitis. [Updated July 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. 2021 Jan-. Aufgerufen am 10.11.2021.
Reviewed by the German Society for Pediatric Infectiology (Deutsche Gesellschaft für Pädiatrische Infektiologie e.V., DGPI).
As at: