Conditions Varicose veins
ICD codes: I83 What are ICD codes?
About one in every five adults has varicose veins. The uneven bluish veins are a cosmetic problem in particular for most people. However, they can sometimes also lead to complications. Find out more about causes and therapies.
At a glance
- Varicose veins are uneven bluish veins that are permanently enlarged.
- Varicose veins develop most commonly on the calves or insides of the thighs if blood accumulates in the superficial leg veins.
- The bluish veins directly under the skin are only a cosmetic problem for many of those affected, but they can also cause symptoms such as heavy legs or calf cramps.
- With severe symptoms or for cosmetic reasons, varicose veins can be surgically removed, sealed by heat or chemically shrunk.
- A less distinctive form of varicose veins is spider veins. These are fine reddish or bluish branches under the skin.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.

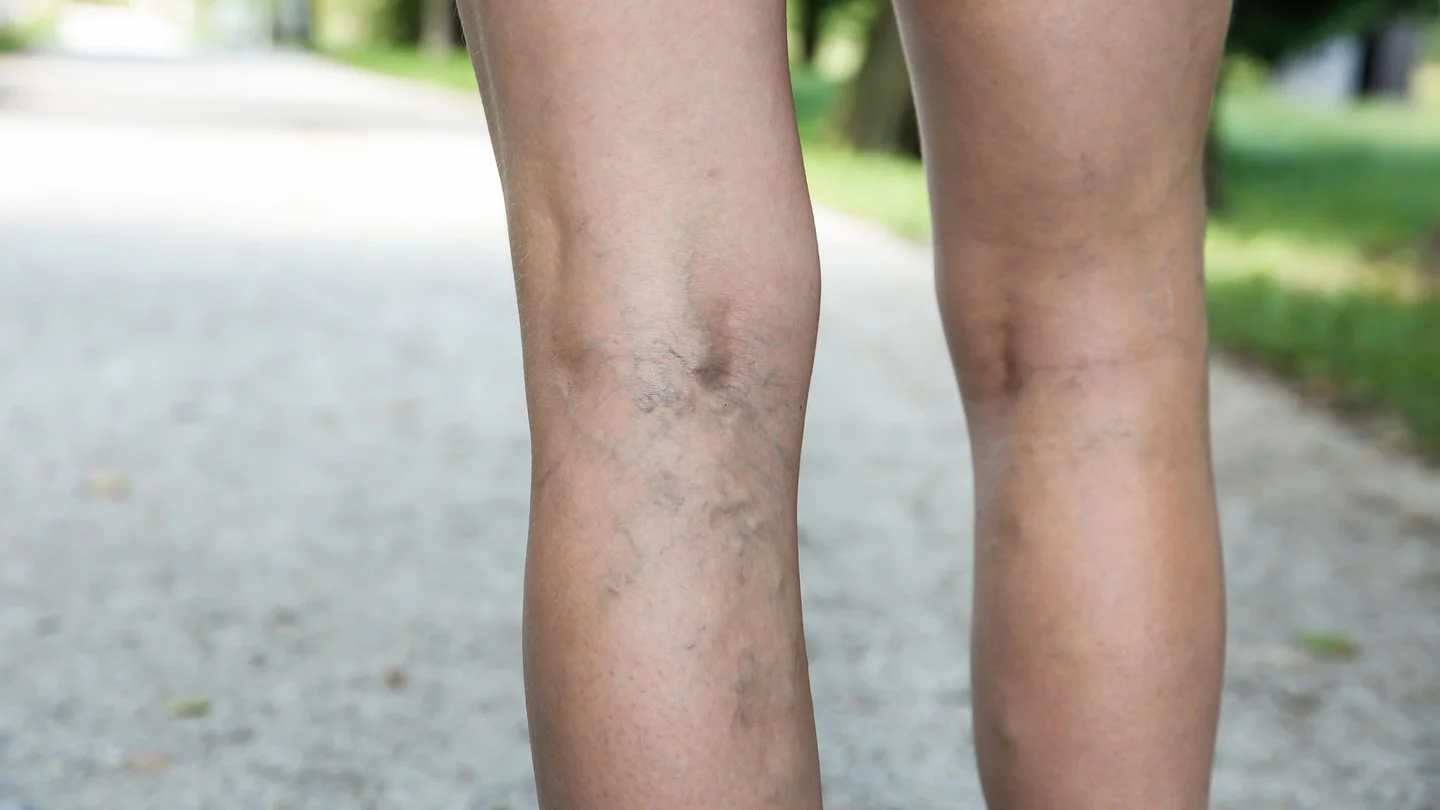
What are varicose veins?
Varicose veins (varices) are enlarged veins that often have a purple or bluish luster through the skin. For many people, they are an esthetic problem in particular. However, they can also lead to symptoms like heavy legs or calf cramps.
The bluish veins most commonly appear on the calves or insides of the legs. Varicose veins develop when blood accumulates in the superficial leg veins. Ordinarily, the veins swell up and then protrude outward – in doing so, they look bluish through the skin.
So-called spider veins are a less distinctive form of varicose veins. These are fine reddish or bluish branches under the skin. Visually, they thus often resemble spider legs, hence the name. Spider veins also frequently occur on the legs, and sometimes they also appear on the face. Spider veins are widespread and harmless.
What are the symptoms of varicose veins?
Varicose veins most commonly develop on the calves or insides of the thighs – they can cause the legs to feel heavy and swell up, especially on the ankles. The skin can moreover stretch or itch. The discomfort commonly increases around the end of the day – especially with prolonged sitting or standing. Varicose veins can sometimes also cause calf cramps or pain in the night. The problems often get worse in warm weather.
The appearance of the legs can also be very debilitating for many people. They then avoid showing their legs in public. In that case, it is typical for instance to only wear long trousers or avoid going to a swimming pool. If the quality of life is so severely limited by varicose veins, a therapy can be useful even without severe symptoms.
The form of the varicose veins does not necessarily reveal anything about the severity of the symptoms. Barely noticeable varicose veins can cause severe impairments, whereas large, knotty and thickened varicose veins can cause no problems at all.
What are the causes of varicose veins?
There are deep and superficial veins in the legs. All veins are equipped with valves that ensure the blood does not regurgitate. Varicose veins can develop when the blood in the superficial veins backs up. That occurs when the vein walls and venous valves are weak or do not exert enough pressure on the veins. That can be the case for example if someone stands often on one spot for a long time without the leg muscles (the “muscle pump”) being activated.
What favors the development of varicose veins?
Various factors can favor the formation of varicose veins:
- advancing age
- family history
- severe obesity
- professions involving long periods standing up
- vascular diseases such as deep vein thrombosis of the leg
In women, varicose veins develop for the first time during pregnancy, because the blood flow out of the leg veins is worse. That is due to hormonal changes to the body tissue and the extra weight. But these varicose veins often form again in the months after childbirth.
How common are varicose veins?
Around 20% of adults will develop varicose veins at some point. The prevalence increases with age. Women are affected more often than men.
Which complications can occur with varicose veins?
Leg ulcers are the most common complication of varicose veins. An open sore develops in 3% to 6% of those affected if varicose veins remain untreated. Other possible complications include phlebitis, thromboses or bleeding, but they are rare.
If the following indications occur, seek medical advice quickly as they may indicate complications:
- sores or open wounds around the ankle that are not the result of an injury or have not healed after 2 weeks
- severe leg swelling
- reddened veins that feel warm and are painful
- bleeding from or near the varicose veins
- a skin rash in the area of the varicose veins
While bleeding is very rare with varicose veins, it can still be dangerous and requires immediate medical assistance. As a first-aid measure, the leg should be elevated and pressure applied to the site of the bleeding.
How are varicose veins diagnosed?
Varicose veins can be easily recognized by their typical appearance. During diagnosis, a Duplex ultrasound, also known as a Doppler, gives information about the blood flow in the veins and venous valves that do not close tightly. This method moreover helps assess the veins before a surgical procedure.
How are varicose veins treated?
The following measures can help relieve symptoms:
- avoiding prolonged standing and sitting
- plenty of exercise – as often as possible, even in the daily routine
- elevating the legs when sitting
- not crossing legs when sitting
- if overweight, losing some weight
Important: Support stockings (compression stockings) exert pressure on the veins – this should assist the blood flow. However, it is still unclear whether and how well they actually help with discomfort caused by varicose veins. The same also applies to weight loss. The effectiveness of creams, ointments, tablets and food supplements acquired to treat vein problems also remains unproven. These remedies contain, for example, horse chestnut or red vine leaf extracts.
Various interventions are possible in the case of severe symptoms or for cosmetic reasons. The varicose veins can be surgically removed, sealed by heat or chemically shrunk.
The following two methods are the most common for operations:
- Vein stripping: 2 incisions are made on the leg and the vein is fully extracted via an incision in the groin or the back of the knee.
- Phlebectomy: With this, various small incisions of a few millimeters are made along the affected vein, which is removed in multiple sections. This method is used especially for smaller veins.
Nowadays, varicose veins are often sealed by heat as well. This procedure is more rarely associated with complications than surgery. There are 2 options to choose from:
- Radiofrequency ablation: a thin tube (catheter) is pushed into the vein through a small skin incision, after which a probe that emits electromagnetic waves is inserted into the catheter. The vein is sealed by the heat release.
- Endovenous laser therapy: with this method, the vein is also sealed from within by heat, but laser beams are used instead of radio waves.
Another option is sclerotherapy: a liquid or foam is injected into the affected vein. This damages the vein so severely that it is converted into connective tissue and thereby sealed. Possible side effects can be brownish skin discolorations on the injection sites – however, they usually disappear again within a few weeks or months.
Because not all health insurance funds pay for every therapy, it is a good idea to find out beforehand which costs will be accepted.
More detailed information about when an operation for varicose veins is a good idea can be found at gesundheitsinformation.de.
- De Avila Oliveira R, Riera R, Vasconcelos V et al. Injection sclerotherapy for varicose veins. Cochrane Database Syst Rev 2021; (12): CD001732.
- Knight Nee Shingler SL, Robertson L, Stewart M. Graduated compression stockings for the initial treatment of varicose veins in people without venous ulceration. Cochrane Database Syst Rev 2021; (7): CD008819.
- Paravastu SC, Horne M, Dodd PD. Endovenous ablation therapy (laser or radiofrequency) or foam sclerotherapy versus conventional surgical repair for short saphenous varicose veins. Cochrane Database Syst Rev 2016; (11): CD010878.
- Robert Koch-Institut (RKI), Statistisches Bundesamt (Destatis). Venenerkrankungen der Beine (Gesundheitsberichterstattung des Bundes; Band 44). Berlin: RKI; 2009.
- Vemulapalli S, Parikh K, Coeytaux R et al. Systematic review and meta-analysis of endovascular and surgical revascularization for patients with chronic lower extremity venous insufficiency and varicose veins. Am Heart J 2018; 196: 131-143.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at:
