Conditions Gout
ICD codes: M10 What are ICD codes?
Gout is a metabolic disorder that inflames the joints. When an attack occurs, the joints swell up within a few hours and become extremely tender. Tiny, needle-shaped crystals made from uric acid, which tend to be deposited in the joints, trigger the inflammation.
At a glance
- Gout is a metabolic disorder that inflames the joints.
- Gout is the most common inflammatory joint disease (arthritis) in Germany.
- When an attack occurs, certain joints swell up within a few hours and become extremely tender.
- Tiny, needle-shaped crystals made from uric acid, which tend to be deposited in the joints, trigger the inflammation.
- The inflammation usually dies away completely, by itself, within one to two weeks.
- Medication can alleviate the pain.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
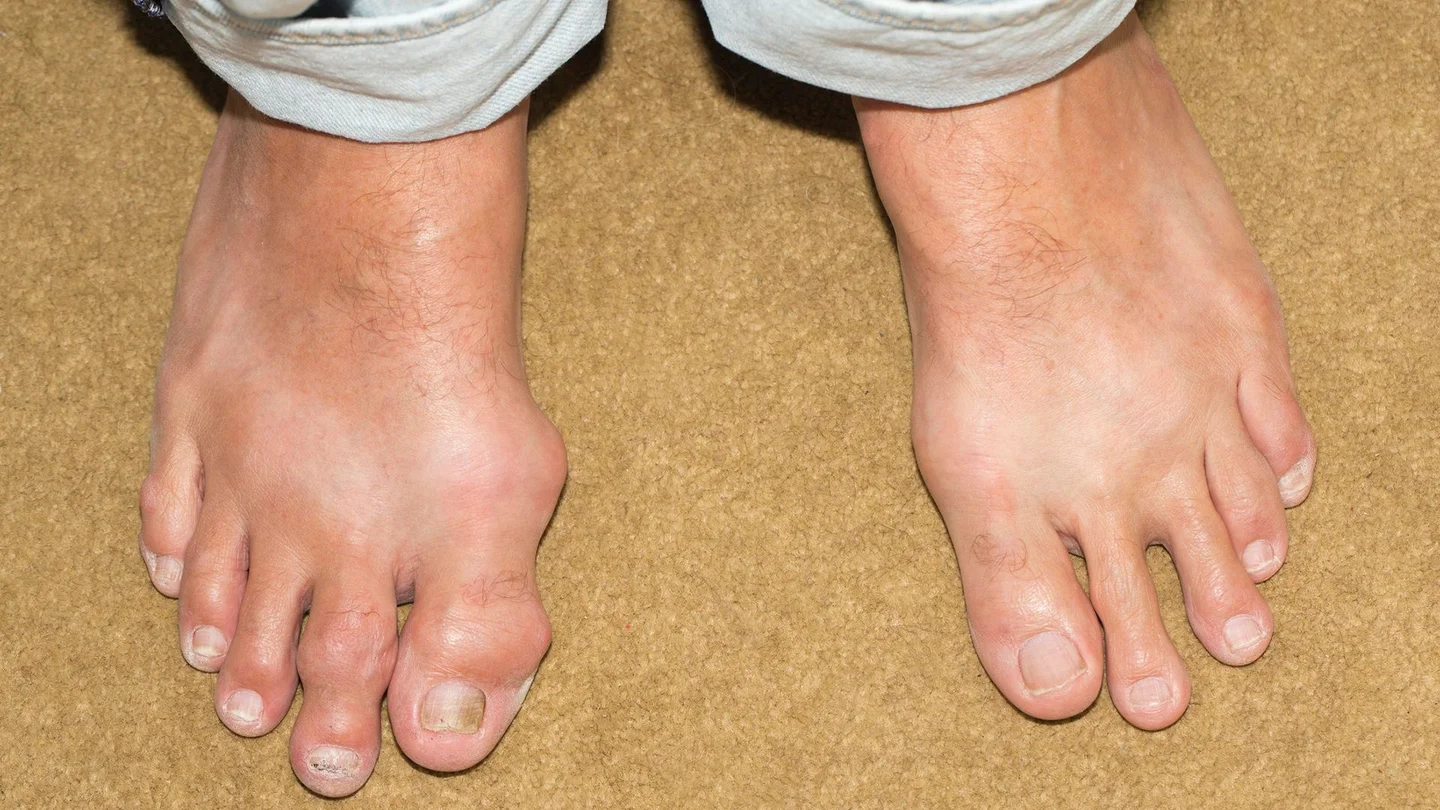
What is gout?
Gout is a metabolic disorder that inflames the joints. When a gout attack occurs certain joints swell up within a few hours and become extremely tender.
Tiny, needle-shaped crystals made from uric acid, which tend to be deposited in the joints, trigger the inflammation. These crystals can form when there is too much uric acid in the body.
The inflammation usually dies away completely, by itself, within one to two weeks. Medication can alleviate the pain.
Most people with gout suffer acute attacks once in a while. There may be months or even years between them. However, they can occur more frequently, too.
There are various ways of preventing attacks. For example, some people cut out particular foods and other potential triggers.
Others take medication that lowers the uric acid level over the long term. This option is of particular interest when gout attacks are frequent, but also in the case of complications such as chalkstones or kidney stones.
Many people have high uric acid levels but no pain. There is debate as to whether these levels mean anything for one’s health. They do not need any treatment.
What are the signs of gout?
Gout attacks often occur at night or early in the morning. The joints suddenly swell up very painfully. The inflamed joints are then tender, hot to the touch and reddened.
The swellings and pain is usually worst after six to twelve hours. The joints are often so sensitive that even the pressure from bedclothes is almost unbearable.
If the swelling goes down after a few days the skin can become slightly flaky in that area.
The first gout attack often only affects one joint, usually the lower joint of the big toe. The metatarsus and ankles, hand and finger joints, knee and elbow can also become inflamed.
Gout attacks in the shoulders and hips are rare.
With chronic gout, the joints are slightly inflamed on a permanent basis. Over time, the joints may become deformed and mobility can become restricted.
What are the causes of gout?
Gout can occur when the blood contains too much uric acid.
Hyperuricemia, i.e., an elevated level of uric acid, is defined as a blood uric acid level of 6.8 milligrams per deciliter (mg/dL) or higher. However, according to estimates, only about one third of all those with a high uric acid level suffer from gout.
Uric acid is formed during the breakdown of purines, a component of DNA. DNA stores genetic information and is found in every cell of the body. Some of the uric acid is normally excreted with urine.
As some people’s kidneys do not excrete enough uric acid, the blood uric acid level increases. If a certain threshold is crossed, the uric acid can form crystals that are deposited in the body’s tissues. The crystals usually accumulate in the joints and can then trigger a gout attack.
Certain illnesses can also contribute to raising uric acid levels, for example, blood disorders or cancers such as leukemia.
In rare cases, gout occurs because the body produces too much uric acid. This may be due to a hereditary disease in which the function of certain proteins (enzymes) that are related to uric acid metabolism is faulty.
Other factors apart from the uric acid level play a role in gout. For example, if the joint tissue contains too little fluid, uric acid crystals tend to form. The acidity level (pH value) of the joint fluid and the joint temperature also affect the illness.
What increases the risk of suffering from gout?
Gout is fostered by any factor that increases the uric acid level. In people who already suffer from gout, they increase the risk of further attacks.
Scientifically proven risk factors for gout include:
- medication that increases the level of uric acid in the blood – in particular, diuretic drugs (diuretics), acetylsalicylic acid (ASA), certain drugs used after an organ transplant, Levodopa (used to treat Parkinson’s disease), and cancer drugs
- meat, fish and seafood: these foods contain lots of purine. When eaten in large quantities they slightly increase the risk of suffering from gout. In studies, purine-rich plant-based foods showed no impact on the occurrence of gout.
- Alcohol: alcoholic drinks promote the formation of uric acid and act as diuretics. Moreover, when alcohol is consumed, the kidneys excrete less uric acid. Beer, in particular, also contains a relatively large amount of purine. Studies show that beer and high-percentage alcohol increase the risk of gout. Wine drunk in moderation does not appear to have any effect.
- Sugary drinks: drinks containing a lot of (fruit) sugar can also slightly increase the risk of gout. This applies in particular to colas and possibly also fruit juices. Artificially sweetened drinks have no effect on gout.
- Being overweight: excess weight increases the risk of gout. The risk rises in tandem with an increase in the body mass index (BMI).
While certain foods and other factors can slightly increase the risk of developing gout or gout attacks, it is particularly important that the kidneys continue to function well and are able to reliably excrete an excess of uric acid.
How common is gout?
Gout is the most common type of inflammatory joint disease (arthritis) in many industrialized countries, including Germany.
According to estimates, one to two percent of the population have gout.
Men suffer around five times more than women, and usually earlier.
In men, gout usually occurs from the age of 40 onwards, while in women it is only after the menopause. This is due to hormonal influences on the kidneys.
How does gout develop?
The joint usually recovers by itself from an attack of gout within one to two weeks. Most people who have had a gout attack suffer another one within a period of six months to two years afterwards. Repeated attacks can affect multiple joints and last somewhat longer.
After about twelve years, gout may become chronic and damage the joints. However, acute gout does not always become chronic. The risk of chronic gout depends, for instance, on how elevated the uric acid level is.
Over time, chalkstones may form. These are uric acid deposits in the soft tissues. These develop over a period of years. Chalkstones are not usually painful. They are particularly likely to occur in the toe and finger joints, the elbow, the Achilles tendons and on the ears.
What are the long-term effects of gout?
If gout becomes chronic and the joints are damaged, this restricts mobility. It can also weaken the muscles.
In rare cases, uric acid crystals are deposited in atypical parts of the body. For example, if chalkstones form in the spinal cord area, they can press on the nerves and cause signs of paralysis. If chalkstones develop in the carpal tunnel in the hand joint, carpal tunnel syndrome may develop.
Gout patients also have an increased risk of kidney stones. Kidney stones can be painful and make urinary tract infections more likely. On average, just under one man in every 100 who suffer from gout will develop kidney stones within a year.
How is gout diagnosed?
Doctors can often detect an acute case of gout from the risk factors and typical symptoms. A relatively reliable indication of gout is, in particular, a painful, reddened swelling on the lower or end joint of the big toe.
Gout is unequivocally proven by a joint puncture. This involves using a fine hollow needle to extract fluid from the joint and examine it in a laboratory. When uric acid crystals are found in the joint fluid, “gout” is diagnosed.
A joint puncture is done if the symptoms are ambiguous or to exclude other potential causes. These mainly include joints infected by bacteria, which may occur due to injury, for example. This type of infection should be treated rapidly.
Determining the uric acid level in the blood is of limited use because the level often drops to within the normal range during a gout attack.
How is gout treated?
Gout treatment has various goals:
- In the short term, it aims to alleviate pain when a gout attack occurs.
- In the long term, it aims to prevent attacks and to reduce the risk of chronic inflammations and joint damage.
Short-term gout treatment
Gout attacks are treated with anti-inflammatory drugs. These include the following:
- non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, indometacin and naproxen
- cortisone products: usually tablets with the active ingredient prednisolone
- the gout drug colchicine is no longer used as often as in the past because it is slow-acting and can have side effects
If pain medication is not enough to alleviate the pain, more than one active ingredient can be used in combination to treat the condition.
Cooling the affected joints is also likely to be beneficial. At the very least, it provides short-term relief.
Long-term gout treatment
Long-term gout treatment aims to prevent gout attacks and complications by reducing the uric acid level. This may be done as follows:
- changes in diet, especially reducing consumption of meat, fish and seafood and drinking less alcohol
- taking medication that reduces uric acid levels – usually allopurinol
Not every person with gout needs medication to reduce uric acid. These products are usually not needed after the first gout attack, in particular. This is because some patients experience few problems or none at all for years afterwards.
Medication to reduce uric acid is considered if dietary changes alone are insufficient. It is used in particular for frequent or especially painful gout attacks. These products are also useful when there are complications such as chalkstones and kidney stones, or when kidney functionality is limited.
For more detailed information about pain treatment during an acute attack of gout and about the role of diet in the condition, see gesundheitsinformation.de.
What is life like with gout?
When a person has a gout attack, the pain can be very debilitating and make many everyday activities impossible. Walking, cycling, putting shoes on or gripping and holding things may become a challenge.
Over time, some patients develop the ability to sense when a new gout attack is about to occur.
But gout attacks do not just impose physical limitations. They can also affect sleep and harm the patient’s mood. It is not normally possible for patients to go to work or do household chores.
It may be helpful to explain to friends and family members how painful the illness is. This will help them understand why the person needs to look after themselves and why they need to rest.
People with gout should not feel guilty because they cannot work or are less available to partners and family.
Gout attacks can change one’s own body image. In particular, it can be difficult for young people to have an illness which tends to be viewed as an older person’s illness.
The gesundheitsinformation.de website has reports from four people with experience of gout.
- Ayoub-Charette S, Liu Q, Khan TA et al. Important food sources of fructose-containing sugars and incident gout: a systematic review and meta-analysis of prospective cohort studies. BMJ Open 2019; 9(5): e024171. doi: 10.1136/bmjopen-2018-024171.
- Harrold LR, Mazor KM, Velten S et al. Patients and providers view gout differently: a qualitative study. Chronic Illn 2010; 6(4): 263-271. doi: 10.1177/1742395310378761.
- Jamnik J, Rehman S, Blanco Mejia S et al. Fructose intake and risk of gout and hyperuricemia: a systematic review and meta-analysis of prospective cohort studies. BMJ Open 2016; 6(10): e013191. doi: 10.1136/bmjopen-2016-013191.
- Li X, Meng X, Timofeeva M et al. Serum uric acid levels and multiple health outcomes: umbrella review of evidence from observational studies, randomised controlled trials, and Mendelian randomisation studies. BMJ 2017; 357: j2376. doi: 10.1136/bmj.j2376.
- Martini N, Bryant L, Te Karu L et al. Living With Gout in New Zealand: Living With Gout in New Zealand. An Exploratory Study Into People's Knowledge About the Disease and Its Treatment. J Clin Rheumatol 2012; 18(3): 125-129. doi: 10.1097/RHU.0b013e31824e1f6f.
- Newberry SJ, FitzGerald JD, Motala A et al. Diagnosis of Gout: A Systematic Review in Support of an American College of Physicians Clinical Practice Guideline. Ann Intern Med 2017; 166(1): 27-36. doi: 10.7326/M16-0462.
- Qaseem A, Harris RP, Forciea MA. Management of Acute and Recurrent Gout: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med 2017; 166(1): 58-68. doi: 10.7326/M16-0570.
- Qaseem A, McLean RM, Starkey M et al. Diagnosis of Acute Gout: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med 2017; 166(1): 52-57. doi: 10.7326/M16-0569.
- Richette P, Bardin T. Gout. Lancet 2010; 375(9711): 318-328. doi: 10.1016/S0140-6736(09)60883-7.
- Roddy E, Mallen CD, Doherty M. Gout. BMJ 2013; 347: f5648. doi: 10.1136/bmj.f5648
- Shekelle PG, FitzGerald J, Newberry SJ, et al. Management of Gout. Comparative Effectiveness Reviews. No. 176. Agency for Healthcare Research and Quality (AHRQ). 2016.
- Tausche AK, Jansen TL, Schröder HE et al. Gout. Current diagnosis and treatment. Dtsch Arztebl Int 2009; 106(34-35): 549-555. doi: 10.3238/arztebl.2009.0549.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen) (IQWiG).
As at:


