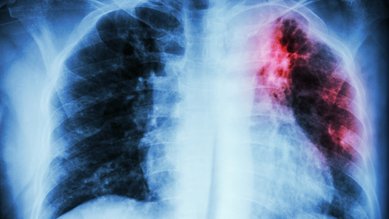
Conditions Leprosy
ICD codes: A30 What are ICD codes?
Leprosy is a chronic infectious disease that can cause skin changes and nerve damage. It primarily occurs in South East Asia, South America, and Africa. Although leprosy can be cured, severe cases still occur.
At a glance
- Leprosy is a chronic infectious disease caused by bacteria called Mycobacterium leprae.
- The disease occurs primarily in certain regions of South East Asia, South America, and Africa.
- It can cause skin changes and nerve damage.
- Leprosy is treated with a combination of different antibiotics, so it can be cured.
- Early treatment is important in preventing leprosy from causing disabilities.
- In many societies, people with leprosy experience social exclusion.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
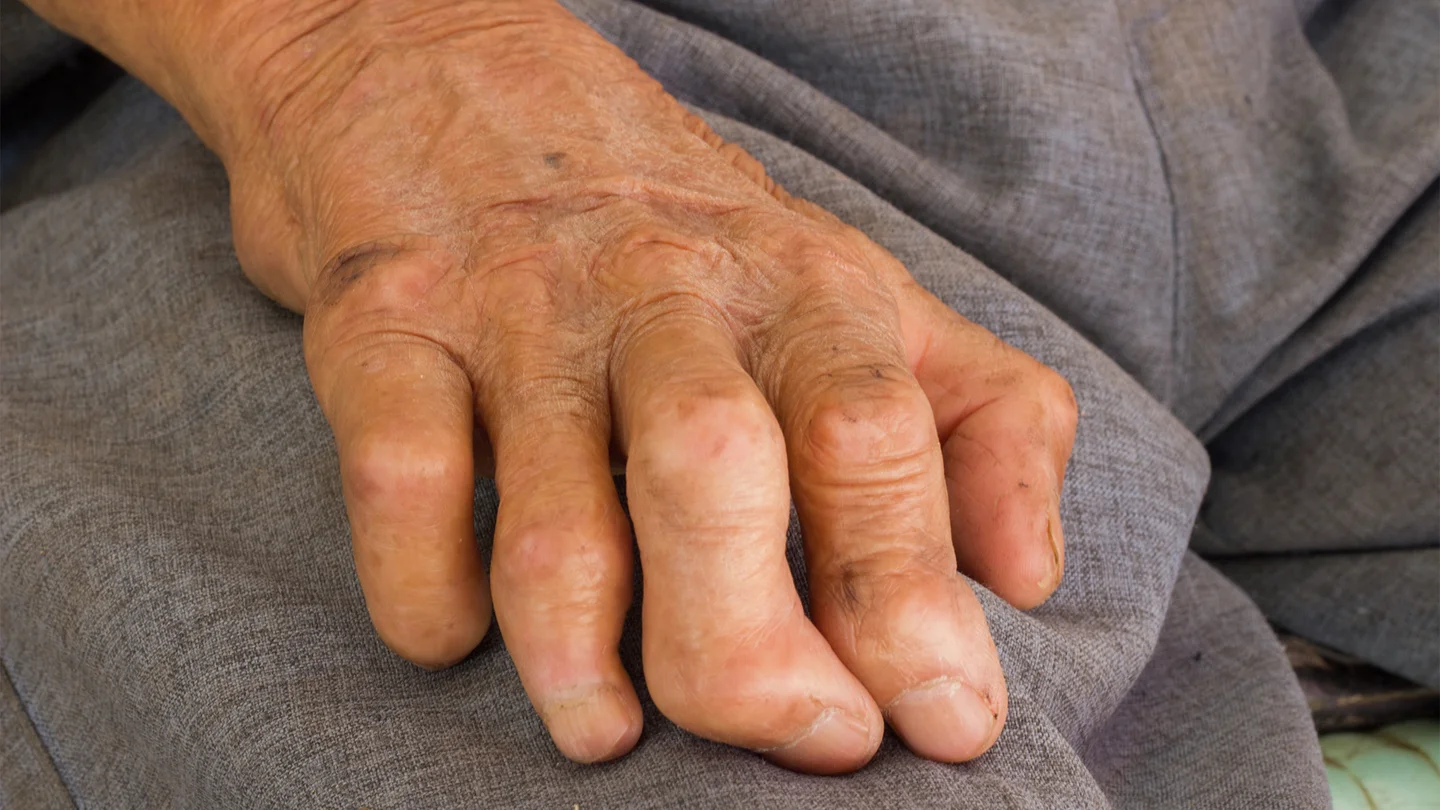
What is leprosy?
Leprosy is a chronic infectious disease caused by bacteria called Mycobacterium leprae. The disease is particularly common in some countries of South East Asia, South America, and Africa. It is very rare for cases of leprosy to be “imported” into Germany by foreign travelers.
Leprosy is typically associated with changes to the skin. Another characteristic symptom is nerve damage, which can cause paralysis and sensory disorders.
The disease can be treated with a combination of various drugs. If treatment is started at an early stage, disabilities caused by leprosy can usually be prevented.
What are the symptoms of leprosy?
Leprosy causes visible changes to the skin and damage to the nerves, impairing sensitivity to touch, pain, and temperature. Mucous membranes, airways, and eyes can also be affected.
Following contact with the Mycobacterium leprae pathogen, only 5% of people develop symptoms. After contracting the disease, it may take between 3 months and 40 years for the first symptoms to appear, with the average being 2 to 4 years.
Early symptoms include small, isolated, uncharacteristic skin changes, appearing as reddish patches on pale skin and as pale patches on dark skin. The skin patches are commonly referred to as skin lesions. In around three-quarters of people infected, the skin changes heal spontaneously. For the remaining quarter, the disease develops in one of the ways described below. The severity of the disease depends on the individual’s immune defenses.
Limited inflammation
This limited form occurs if the immune system is functioning as normal, as the body’s defenses are able to actively fight the pathogens. A few asymmetrical, sharply defined skin lesions occur, often with a raised border. On darker skin, the skin lesions are paler than the surrounding skin. They sometimes appear reddish, especially on pale skin. The lesions are accompanied by nerve swellings and damage to the peripheral and autonomous nervous systems. Sensitivity to pain and temperature as well as sweat production may be severely impaired as a result.
Severe form
When there is no immune response, i.e. the body’s defenses are not working effectively, symmetrically distributed skin lesions form all over the body. These may appear pale on dark skin or reddish on pale skin. As the disease progresses, deeper layers of the skin are also affected, in particular on the face. The eyebrows may also be lost. Over time, swellings and nodules can give the face the appearance of a lion (a condition known as leonine facies).
Nerve damage causes pronounced sensory disorders, including loss of sensitivity to pain and temperature. Due to this impaired sensitivity, injuries are more likely to occur that are not or barely noticed by the individual affected. Open sores can become inflamed when they are attacked by more bacteria. Paralysis occurs as a result of damage to the nerves that control the muscles. Persistent inflammations and injuries that go unnoticed can lead to deformed or shortened limbs.
Transitional forms
Along the spectrum ranging from limited inflammation to the most severe form of leprosy, several other stages and mixed forms are defined.
What causes leprosy?
Leprosy is transmitted from person to person by means of droplet infection. This means that the infectious agents are spread in tiny respiratory droplets that are released into the air when talking or sneezing. Leprosy is not highly contagious – only prolonged, close contact can cause an infection that leads to illness. Once treatment with medication has begun, a person infected with leprosy is no longer contagious.
What are the known risk factors for leprosy?
As leprosy is only a moderately contagious infectious disease, the living conditions and general health play an important role in infection. The risk of infection is increased in particular through prolonged, close contact with an infected person and through a weakened immune system. Hereditary factors also appear to influence whether an individual becomes ill following contact with an infected person.
Video What are infectious diseases?
The video below looks at when doctors talk about an infectious disease, which pathogens trigger infectious diseases, and how they are transmitted.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
Where and how frequently does leprosy occur?
Every year, over 200,000 people worldwide become ill with leprosy. The disease occurs in particular in certain parts of South-East Asia, Africa, and South America.
In Germany, an average of 1 case of leprosy was reported annually over the last 10 years. It can be assumed that these cases were brought into the country as a result of foreign travel.
How does leprosy progress?
There are mild, but also very severe forms. The weaker a person’s immune defenses, the more easily the pathogens can grow in the body, making the disease develop into a severe form.
If left untreated, the severe form of leprosy can result in unnoticed injuries and the inflammation of open wounds, ultimately leading to deformities of the hands and feet. Severe inflammation of the eyes, which can ultimately lead to blindness, is also possible.
How can leprosy be prevented?
Close contact with infected individuals over an extended period should be avoided to prevent the spread of leprosy. Anyone who has had contact with someone infected with leprosy should be examined by a doctor. To avoid developing leprosy at a later stage, it is recommended that the antibiotic rifampicin be administered as a one-time treatment in such cases.
Early diagnosis based on screening in at-risk areas and early treatment are important ways of preventing further spread of the disease.
There is no approved vaccine against leprosy. However, there is an immunological similarity between the pathogens that cause leprosy and those that cause tuberculosis. As a result, vaccination against tuberculosis offers a certain degree of protection against leprosy.
How is leprosy diagnosed?
Cases of leprosy are normally identified on the basis of the typical symptoms that occur. These consist of pale or reddish patches on the skin with a simultaneous loss of sensitivity in those areas. Other typical symptoms include thickening of the nerves with impaired sensitivity and muscle weakness.
If there are only mild symptoms or none at all, laboratory analysis may be required to verify the presence of the disease. With the skin smear method, the skin is scored with a scalpel in certain places to obtain a small volume of lymph fluid. The lymph fluid can then be tested for the presence of the bacteria that cause leprosy. In most patients, however, this does not provide definitive evidence of the disease. A more reliable diagnostic method is to take a tissue sample for analysis.
How is leprosy treated?
Leprosy can be cured. Early treatment is important in preventing leprosy from causing disabilities. The disease is treated with multiple drugs (antibiotics) simultaneously. These drugs are called dapsone, rifampicin and clofazimine, and are taken for a period of 6 to 12 months. The severity of the disease dictates how long the patient must continue to take the medication. The symptoms of leprosy should also be treated and alleviated, e.g., by means of wound care, skin care, exercise therapy where there are signs of paralysis, and eye care.
Inflammatory reactions occasionally occur during treatment with drugs. For this reason, treatment should take place in specialized centers so that doctors can respond without delay to any complications that may arise.
- Deximed. Lepra. Aufgerufen am 10.12.2024.
- Robert Koch-Institut (RKI). Epidemiologisches Bulletin 5/2007: Lepra – die neue globale Strategie. Aufgerufen am 10.12.2024.
- Robert Koch-Institut (RKI). Epidemiologisches Bulletin 5/2024: Welt-Lepra-Tag 2024. Aufgerufen am 10.12.2024.
- Robert Koch-Institut (RKI). Epidemiologisches Bulletin 45/2024: Importierte Infektionskrankheiten 2023. Aufgerufen am 10.12.2024.
- Robert-Koch-Institut (RKI). Steckbriefe seltener und importierter Infektionskrankheiten. Aufgerufen am 10.12.2024.
- World Health Organization (WHO). Guidelines for the diagnosis, treatment and prevention of leprosy. 2018. Aufgerufen am 10.12.2024.
- World Health Organization (WHO). Leprosy. Aufgerufen am 10.12.2024.
Reviewed by the German Brain Foundation (Deutsche Hirnstiftung e.V. – DHS)
As at: