Conditions Acute middle ear infection
ICD codes: H65.0 H65.1 H66.0 What are ICD codes?
Acute middle ear infections (referred to in medical terminology as acute otitis media or AOM) are one of the most common illnesses among babies and small children. In most cases, the infection and pain subside on their own within two to three days. Serious complications are rare.
At a glance
- Around 80 percent of children experience a middle ear infection in the first three years of life.
- These infections are usually impossible to avoid.
- Children with an infection have pain and fever, cry frequently, and are unable to sleep at night.
- An acute middle ear infection usually clears up on its own within two to three days.
- Recovery can be assisted by treatment to relieve the pain and reduce fever, as well as by giving the child plenty of care and attention.
- Antibiotics are only prescribed if the infection is bacterial.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
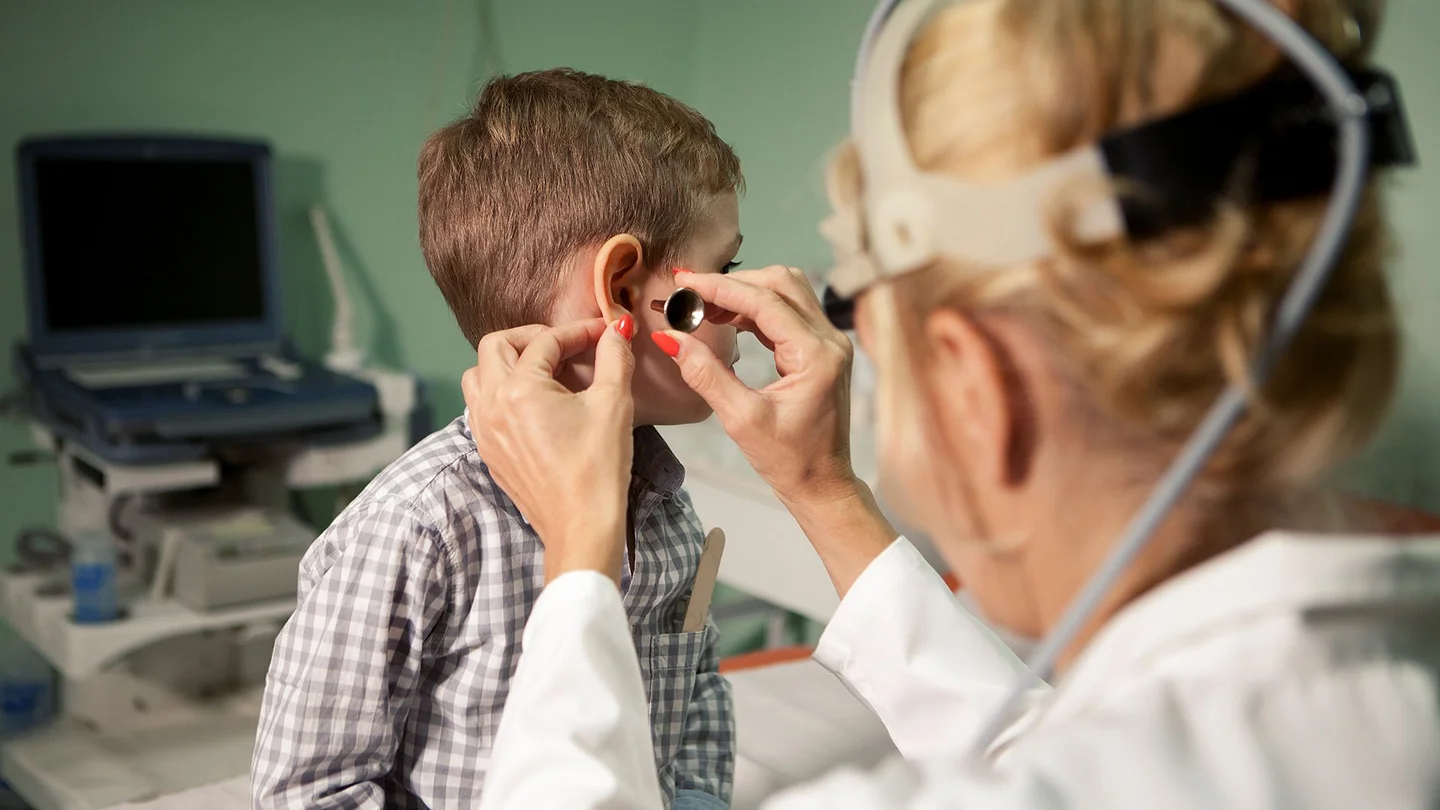
What is a middle ear infection?
Most babies and small children experience at least one acute middle ear infection (acute otitis media) in the first three years of life. Children with an infection have pain and fever, cry frequently, and are unable to sleep at night. Although an acute middle ear infection can mean sleepless nights and worry for parents, it usually clears up on its own within two to three days. Serious complications are very rare.
In most cases, the only treatment needed is to give the child medication to relieve pain and reduce the fever, as well as to give them plenty of care and attention. However, parents should still monitor the course of the infection closely and ask for medical advice in case of doubt. More severe and longer-lasting symptoms may require further treatment.
What are the signs of a middle ear infection?
The typical symptoms of an acute middle ear infection in a small child are:
- severe earache
- fever over 38 °C
- difficulty hearing because fluid has accumulated in the middle ear
The infection occurs very suddenly, sometimes accompanied by vomiting. As small children are often unable to pinpoint sources of pain, they may complain of a sore stomach rather than an earache. In particular if the child is still very young, it can be difficult for parents to assess the severity of the pain. They should check to see if the child frequently shakes his/her head or touches/rubs the ears. These may all indicate an infection.
What happens during a middle ear infection?
When the middle ear becomes acutely inflamed, this is usually accompanied by a viral or bacterial infection such as the common cold, flu, or sore throat.
- With a respiratory infection, viruses or bacteria enter the throat. This causes inflammation of the mucus membranes, and increased production of secretions.
- The infection also causes swellings of the mucus membranes in the ear and in the Eustachian (or auditory) tube, i.e., the tube connecting the middle ear and throat.
- As a result, secretions can no longer drain out of this tube or the middle ear, and so these become blocked. This in turn causes pressure on the eardrum, so that the child experiences pain and difficulty hearing.
In babies and small children, germs can easily spread from the nose and throat to the middle ear because the tube connecting the two areas is still very short and narrow. Once children reach the age of seven, this tube and the immune system are more developed and middle ear infections occur less frequently.
In addition, enlarged adenoids (also known as polyps) can interfere with ventilation of the middle ear and make an infection more likely. Allergic reactions or sinus infections can also cause swelling of the tube and inflammation of the middle ear.
The following factors increase the likelihood of children getting a middle ear infection:
- using pacifiers
- close contact with other children, e.g. in childcare settings
- bottle feeding rather than breast feeding
- frequent exposure to tobacco smoke (passive smoking)
How common are middle ear infections?
Middle ear infections are one of the most common reasons for babies and small children to visit the doctor. Around 80 percent of all children will have had one by the time they are three years old. Up to one third of these children will have recurring infections.
How does the condition develop?
An acute middle ear infection usually clears up on its own and without any complications within two to three days. If an excessive volume of secretions has built up and puts pressure on the eardrum, the eardrum may rupture (burst). If this happens, the pain will subside and a thick fluid, possibly mixed with mucus and blood, flows out into the ear canal.
This ear discharge, known as otorrhea, may continue for several days or weeks. Over this period, the tear in the eardrum – which is usually very small – normally heals by itself.
With a chronic middle ear infection (chronic otitis media), the pain and fever resolve but the fluid buildup in the middle ear persists for weeks and fluid mixed with pus may continue to be discharged from the ear.
These longer-lasting infections can permanently damage the child’s hearing. Parents should seek medical advice if they notice that their child’s hearing is impaired after a middle ear infection.
Can a middle ear infection be prevented?
While middle ear infections cannot normally be prevented, there are certain methods and measures that may serve to reduce the risk to some extent. For example, parents can reduce the amount of time that their child uses a pacifier. Above all, a smoke-free environment is very important for children, as passive smoking increases the risk of infections in the airways, nose, and throat, while also weakening the immune system.
For information about preventing middle ear infections, including recurring infections, visit gesundheitsinformation.de.
How is a middle ear infection diagnosed?


The doctor will begin by asking about the acute symptoms and any prior history of the illness.
This is followed by an examination of both ears, the neck, and throat. An instrument called an otoscope (auriscope) is used to examine the eardrum. This instrument has a magnifying glass and a lamp, which allow the doctor to see inside the ear canal. A tympanometer can be used to test the patient’s hearing. This instrument can generate and record sounds. It can also alter the air pressure to detect whether the ear drum is able to move freely. Body temperature is also measured.
It is not always easy to diagnose an acute middle ear infection with certainty. The following are some of the signs that point to this diagnosis:
- sudden onset of the illness with severe ear pain, fever, and general weakness
- a red eardrum
- an eardrum that appears swollen, is rigid, and is not transparent – suggesting that there could be a buildup of fluid behind the eardrum
How is a middle ear infection treated?
The main focus is usually on treating the severe earache as quickly as possible. Drugs like paracetamol or ibuprofen are suitable for relieving pain and reducing fever – these are available as suppositories or in liquid form. The symptoms often subside after these have been administered, so that further treatment is not required.
Antibiotics are only effective if the inflammation is caused by a bacterial (rather than viral) infection. A bacterial infection is indicated by a discharge from the ear that is mixed with pus. In children under two years of age, inflammation in both ears is indicative of a bacterial infection.
To improve ventilation of the middle ear, nose drops to reduce swelling are often recommended, but in all likelihood, they do not have any effect on the course of the illness or its symptoms. They may simply relieve a blocked nose for a couple of hours, but they should not be used for more than a few days.
The effectiveness of home remedies such as leg compresses for fever or onion poultices for earache has not been sufficiently demonstrated. The same applies to herbal remedies. Homeopathic remedies are not effective.
For more detailed information about acute middle ear infections and what parents can do, visit gesundheitsinformation.de.
- Bhutta MF, Head K, Chong LY et al. Aural toilet (ear cleaning) for chronic suppurative otitis media. Cochrane Database Syst Rev 2020; (9): CD013057.
- Coleman C, Moore M. Decongestants and antihistamines for acute otitis media in children. Cochrane Database Syst Rev 2008; (3): CD001727.
- Jones LL, Hassanien A, Cook DG, Britton J, Leonardi-Bee J. Parental smoking and the risk of middle ear disease in children: a systematic review and meta-analysis. Arch Pediatr Adolesc Med 2012; 166(1): 18-27.
- National Institute for Health and Care Excellence (NICE). Otitis media (acute): antimicrobial prescribing. NICE guideline (NG91). Evidence review 03.2018.
- Nelson AM. A comprehensive review of evidence and current recommendations related to pacifier usage. J Pediatr Nurs 2012; 27(6): 690-699.
- Ranakusuma RW, Pitoyo Y, Safitri ED, Thorning S, Beller EM, Sastroasmoro S et al. Systemic corticosteroids for acute otitis media in children. Cochrane Database Syst Rev 2018; (3): CD012289.
- Russel D, Luthra M, Wright J, Golby M. A qualitative investigation of parents' concerns, experiences and expectations in managing otitis media in children: implications for general practitioners. Primary Health Care Research and Development 2003; 4(1): 85-93.
- Sjoukes A, Venekamp RP, van de Pol AC, Hay AD, Little P, Schilder AG et al. Paracetamol (acetaminophen) or non-steroidal anti-inflammatory drugs, alone or combined, for pain relief in acute otitis media in children. Cochrane Database Syst Rev 2016; (12): CD011534.
- Son MJ, Choi S, Kim YE, Kim YH. Herbal medicines for the treatment of otitis media with effusion: a systematic review of randomised controlled trials. BMJ Open 2016; 6(11): e011250.
- Son MJ, Kim YE, Song YI et al. Herbal medicines for treating acute otitis media: A systematic review of randomised controlled trials. Complement Ther Med 2017; 35: 133-139.
- Venekamp RP, Damoiseaux RA, Schilder AG. Acute otitis media in children. BMJ Clin Evid 2014: pii: 0301.
- Venekamp RP, Sanders SL, Glasziou PP, Del Mar CB, Rovers MM. Antibiotics for acute otitis media in children. Cochrane Database Syst Rev 2015; (6): CD000219.
In cooperation with the Institute for Quality and Efficiency in Health Care (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG).
As at: