Conditions Anthrax
ICD codes: A22 What are ICD codes?
Anthrax is a dangerous infectious disease transmitted by bacteria from animals to humans. Occupational groups in agriculture and forestry, for example, are at some risk of infection if they come into contact with infected animals.
At a glance
- Anthrax is a rare infectious disease caused by bacteria.
- The anthrax pathogen is transmitted from animals to humans.
- People who come into close contact with livestock or wildlife are at increased risk.
- If left untreated, some forms of anthrax can quickly become fatal. Cutaneous anthrax is the most common form and resolves without treatment in 80 percent of cases. However, it should still be treated in order to avoid complications.
- Anthrax is treated with antibiotics and, in severe cases, with antibodies also.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is anthrax?
Anthrax is a rare but dangerous infectious disease caused by bacteria. In the past, it was known by several different names, including splenic fever, malignant edema and woolsorters’ disease. The disease is called “anthrax” since the pathogen is called Bacillus anthracis. This name comes from the Greek and means “coal”. This refers to the black skin lesions that occur with cutaneous anthrax.
Depending on the part of the body where anthrax occurs, there are four different variants:
- cutaneous anthrax
- pulmonary anthrax
- gastrointestinal anthrax
- injection anthrax
Cutaneous anthrax is the most common form of the disease (95 percent of cases); the other three variants are very rare.
What are the symptoms of anthrax?
Anthrax causes different symptoms that depend on the affected organ.
Cutaneous anthrax
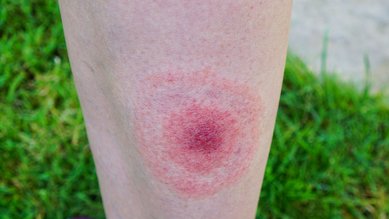
In cutaneous anthrax, pea-sized bumps form at the infection sites, mainly affecting the hands, arms, neck and face. The bumps turn first into fluid-filled blisters and then into an ulcer covered with black scabs (anthrax carbuncles). The skin lesions are not painful.
Pulmonary anthrax
The symptoms of pulmonary anthrax initially resemble those of a cold. However, the toxins released by the bacteria then cause severe symptoms that include a high fever within one to three days. This can develop into blood poisoning (sepsis) along with lung and cardiovascular failure.
Gastrointestinal anthrax
Gastrointestinal anthrax initially manifests as an upset stomach, with abdominal pain, nausea, vomiting, loss of appetite, fever, bloating and flatulence. The toxins produced by the bacteria subsequently cause bloody diarrhea and peritonitis.
Injection anthrax
The symptoms of injection anthrax first become noticeable as swelling around the injection site. The initial stage of the disease may or may not be accompanied by slight pain. As the disease progresses, it causes widespread swelling due to water retention, as well as extensive inflammation of the skin and underlying tissues. The nervous system and gastrointestinal tract may also be affected.
Anthrax meningitis
All of the aforementioned forms can develop into meningitis as a complication. Symptoms such as headache, high fever, confusion, tremors, and muscle pain then suddenly appear. Patients get worse very quickly as the disease progresses. The meningitis it causes is almost always fatal.
What are the causes of anthrax?
All four types of anthrax are caused by the same bacterial pathogen. Bacillus anthracis is a type of bacteria that spreads in the form of spores. The spores are highly resistant and can survive in the ground for long periods. External events, such as floods or landslides, may bring the spores to the surface, where they are typically ingested by grazing animals. Cattle, horses, sheep, and goats are the most likely to be infected. The bacteria are transmitted to humans from animals or through animal products. Once it enters the body, the pathogen produces various toxins that cause symptoms.
The anthrax pathogen can be transmitted in several ways.
Cutaneous anthrax
Cutaneous anthrax is transmitted through direct contact with animals infected with anthrax bacteria. The pathogens enter the body through tiny breaks in the skin. Therefore, people who process animal hides and skins, animal bones and bone products, and other animal tissues are at some risk. Likewise, people working in veterinary medicine and in agriculture, forestry, and hunting can become infected from infected animals. Following infection, it may take up to 6 days for symptoms to develop.
Pulmonary anthrax
Pulmonary anthrax is caused by inhalation of the spores of the anthrax pathogen. This is most likely to happen when spores are intentionally released for this purpose, for example as a biological weapon. It usually takes 4 to 6 days but can take up to 2 months for symptoms to appear.
Gastrointestinal anthrax
The digestive tract becomes infected with the pathogen when someone has eaten the meat of a diseased animal. Symptoms develop around 1 to 3 days after the food is consumed.
Injection anthrax
Transmission occurs when a substance contaminated with anthrax spores is injected. This can happen, for example, during drug use with, e.g., contaminated heroin. Infection via contaminated syringes is also possible. The symptoms usually appear around 1 to 3 days following injection.
Helpful information for drug users is provided by the German AIDS Federation (Deutsche Aidshilfe).
How common is anthrax?
Anthrax is an infectious disease that only occurs rarely in modern, industrialized countries. The most recent case of cutaneous anthrax to be reported in Germany was in 1994. Since 2000, there have been several cases of anthrax among drug users in Europe. In 2012, the disease was also found in four German heroin users.
The last outbreak of anthrax in cattle occurred in Germany in 2014. In contrast, the disease occurs more frequently in southern Europe, Central Asia and southern regions of Africa.
Video What are infectious diseases?
The video below looks at when doctors talk about an infectious disease, which pathogens trigger infectious diseases, and how they are transmitted.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
How can people at risk protect themselves?
Unprotected contact with diseased animals or animal products should be avoided.
A vaccination is also available for certain groups of people who are at high risk of coming into contact with the anthrax pathogen. In Germany, a vaccine for active immunization of adults has been approved since 2013. However, procuring this vaccine is quite complicated because it is not currently sold in the European Union.
How is anthrax diagnosed?
Diagnosis can be difficult because more common infectious diseases cause similar symptoms. A few examples show other possible causes that doctors must consider. In the case of cutaneous anthrax, these include bacterial skin disorders. However, unlike cutaneous anthrax, these are usually painful. In the case of pulmonary anthrax, these include respiratory diseases caused by bacteria, fungi and viruses. For gastrointestinal anthrax, these are very common gastrointestinal infections caused by viruses or bacteria. And for injection anthrax, they include abscesses or diseases in which skin, connective, and muscle tissues die (necrosis).
Depending on symptoms, blood samples, swabs, or tissue samples are taken from the skin, stool, or sputum for a direct diagnosis of anthrax bacteria.
How is anthrax treated?
Various antibiotics are available for treating anthrax, depending on the symptoms and severity of the disease. Even before the laboratory result is available, doctors should start treatment immediately if anthrax is suspected, as the disease can be fatal within a short time if left untreated. In contrast, an early start of antibiotic therapy usually leads to rapid improvement.
There are many antibiotics that are effective against the anthrax pathogen. They are usually given as infusions and sometimes also combined. Depending on the severity of the course of the disease, supporting treatment in the intensive care unit may be necessary. If the course of the disease has already progressed to the point where the bacteria have been able to produce numerous toxins, antibiotic therapy is usually no longer successful.
In order to prevent or slow down the progression of the disease, antibodies against the bacterial toxins can be used to supplement antibiotic therapy in cases of pulmonary anthrax.
Injection anthrax can cause death of the affected skin and underlying tissue. The tissue in the area must then be surgically removed, sometimes several times.
What protective measures can be taken during contact with an infected person?
Although the risk of contracting the infection from an infected person is extremely low, infection is possible if contact is made with contaminated clothing or wound fluid. The following measures, which reduce the risk of infection, apply primarily to hospital personnel:
- Wear protective gloves, protective gowns, mouth-nose protection, eye protection.
- Disinfect hands and surfaces with special agents that combat the spores, for example products made from peracetic acid.
- Place patients in a room by themselves, if possible.
Contacts or people who may possibly have been infected are not required to self-isolate. However, they should be monitored closely to identify possible symptoms immediately. They may also take antibiotics as a precautionary measure (prophylaxis).
Important: Anthrax is a disease that must be reported. If bioterrorism is suspected (the pathogen has also been used as a biological weapon in the past), the responsible health department will initiate all further necessary steps.
- Deutsche Gesellschaft für Infektiologie (DGI) e.V. und Deutsche Gesellschaft für Hygiene und Mikrobiologie (DGHM) e.V. Injektions-Anthrax (Milzbrand). Stand 03.09.2012.
- European Medicines Agency. Guidance document on use of medicinal products for the treatment and prophylaxis in case of exposure to biological agents that might be used as weapons of terrorism, crime or warfare. 07/2024.
- Robert Koch-Institut (RKI). RKI-Ratgeber: Milzbrand (Anthrax). Aufgerufen am 07.03.2025.
- Robert Koch-Institut (RKI). Infektionsepidemiologisches Jahrbuch meldepflichtiger Krankheiten für 2022.
- Weltgesundheitsorganisation (WHO). Anthrax in humans and animals. 4. Auflage 2008.
Reviewed by the Robert Koch Institute.
As at: