Conditions Clostridioides (formerly Clostridium) difficile infection
ICD codes: A04.7 What are ICD codes?
Clostridioides (formerly: Clostridium) difficile are bacteria that colonize the intestines. This usually go unnoticed. However, if the balance of intestinal flora is disrupted, the bacteria can trigger intestinal inflammation and diarrhea.
At a glance
- Clostridioides difficile (formerly called Clostridium difficile) is a type of intestinal bacteria that produce toxins. If the bacteria multiply significantly, the intestines can become inflamed.
- The main symptom of infection is usually sudden, watery diarrhea with a distinctive smell.
- Severe cases can lead to life-threatening complications such as intestinal rupture.
- People with an infection can pass it on to others via tiny, usually invisible fecal particles on their hands or clothing.
- Thorough hand washing is essential to prevent infection.
- The condition of a person’s intestinal flora also determines whether they will contract an infection. Most cases of Clostridioides difficile are due to the person taking antibiotics.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
What is a Clostridioides difficile infection?
Clostridioides (formerly: Clostridium) difficile is a type of bacteria that live in the environment as well as in animals’ and people’s intestines. Almost 5 percent of adults have these bacteria in their intestines but they only cause problems in a very small number of cases.
Under certain circumstances, the bacteria can multiple, for example, if the natural balance of a person’s intestinal flora is disrupted by the use of antibiotics. The toxins released by the bacteria can also damage the intestinal cells and trigger severe diarrhea. This is known as a Clostridioides difficile (C. difficile) infection. Doctors also use the term enterocolitis or enteritis due to C. difficile to describe this condition.
What are the symptoms of a Clostridioides difficile infection?
A Clostridioides difficile (C. difficile) infection typically causes watery diarrhea that has a distinctive smell. It is very rare for diarrhea not to occur. Blood is usually only found in the feces in extremely severe cases.
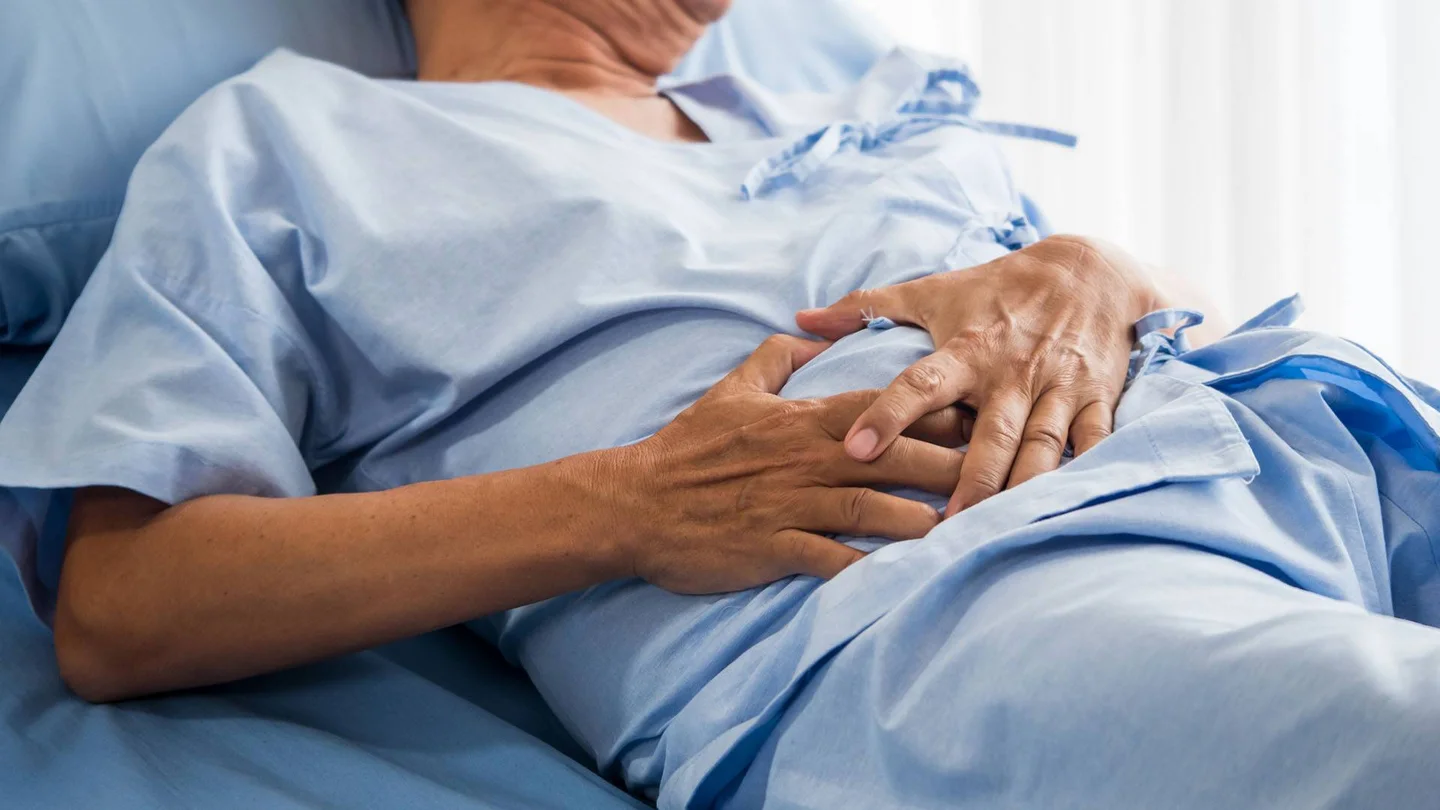
A further typical symptom is a high temperature, which is experienced by almost a third of patients. About a fifth experience pain in the lower abdomen. Loss of appetite, nausea and vomiting are also potential indications of a C. difficile infection.
What causes a Clostridioides difficile infection?
Healthy people with a good immune system and intact intestinal flora can have Clostridioides difficile (C. difficile) bacteria living in their intestines without necessarily becoming ill. However, if the intestinal flora is out of balance (for example, due to taking antibiotics), this can result in an overgrowth of C. difficile bacteria, causing the person to become ill.
C. difficile can produce poisonous substances known as toxins. These toxins damage the intestinal mucosa, leading to intestinal inflammation. The result is sometimes very severe diarrhea.
If the infection has been triggered by antibiotics, symptoms usually begin within a few days after the person has finished the medication. Sometimes, diarrhea may occur while they are still taking the antibiotics but it can also take weeks or even months for symptoms to appear.
Important: Antibiotics do not only combat the bacteria that make people ill, but also the useful bacteria found in the intestines and on the skin. These are part of the human microbiome – a community of microorganisms that performs important tasks such as protecting the body against infections caused by pathogens.
Video What is the microbiome?
Watch this video to find out more about the microbiome and its functions in the human body.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
C. difficile bacteria form resistant spores that can survive on surfaces for a very long time. People who are ill with an infection usually shed large number of these spores in their feces. The spores can spread C. difficile to other people, for example, when shaking hands, grasping door handles or sharing toilets.
Which factors increase the risk of a Clostridioides difficile infection?
The greatest risk factor in association with a Clostridioides difficile (C. difficile) infection is taking antibiotics.
This is because antibiotics can affect the body’s natural bacterial balance. The community of bacteria and other microorganisms that live in the intestines are known as the intestinal flora. The intestinal flora is particularly susceptible to damage from taking antibiotics. An imbalance of the intestinal flora makes it easier for pathogens such as C. difficile to colonize and multiply in large numbers.
Other risk factors for a C. difficile infection are:
- older age
- underlying gastrointestinal tract disorders
- chronic liver and kidney disease
- taking medication that suppresses the immune system
- taking medication that inhibits the production of stomach acid
- a long hospital stay
- an infection with C. difficile in the past
How many people have Clostridioides difficile in their intestines?
Up to 80 percent of all small children have Clostridioides difficile (C. difficile) in their intestines, but most do not notice this.
Among the adult population, up to 5 percent of people have this type of bacteria living in their intestines. Most of them have no symptoms.
C. difficile is responsible for about 15 to 20 percent of all antibiotic-related cases of diarrhea. An average of 1 in 100 people who take antibiotics develop a C. difficile infection.
What is the outlook for a Clostridioides difficile infection?
Clostridioides difficile (C. difficile) does not always cause intestinal inflammation: some people have no symptoms at all; others develop minor intestinal inflammation. On the other hand, some people develop an extremely severe form of intestinal inflammation, known in medical terms as pseudomembranous enterocolitis.
Severe cases can also lead to the dangerous enlargement of the large intestine (toxic megacolon), intestinal obstruction (ileus) or blood poisoning (sepsis).
Up to 5 percent of patients die from the infection, especially older people and those with pre-existing health conditions. Complications vastly increase the risk of the condition being fatal.
Recurrence after treatment is rather common. Up to 10 to 20 percent of patients experience intestinal inflammation again at a later date.
How can a Clostridioides difficile infection be prevented?
Health problems due to Clostridioides difficile (C. difficile) often occur in people who are taking or have taken antibiotics. Therefore, antibiotics should only be used if medically essential. In addition, antibiotic drugs should always be used to treat specific infections and pathogens in as targeted a way as possible. This also helps curb the spread of antibiotic resistance.
The spread of C. difficile can be reduced – especially in medical and care institutions – by quickly identifying, isolating and treating people with an infection.
In the event of contact with people who are infected, it is also important to observe strict hygiene measures. These include wearing protective clothing such as gloves and gowns, for example.
Good hand hygiene is particularly important – not just in medical institutions but during everyday life. By carefully washing the hands with soap every time they go to the toilet and before meals, people can protect themselves and others against infection. This does not just apply to people with an infection, but to everyone.
How do doctors detect Clostridioides difficile?
To definitively diagnose a Clostridioides difficile (C. difficile) infection, a stool sample from the patient is usually examined in a laboratory. There, several tests can be used to prove the presence of either the bacteria themselves or their toxins and other bacterial components.
Sometimes, treatment is begun before the lab results are available, for example, in the case of a very severe infection. In some cases, a colonoscopy can also help to detect the illness.
How is a Clostridioides difficile infection treated?
If a person develops a Clostridioides difficile (C. difficile) infection, any antibiotic medication they are taking for other reasons should be stopped, provided that this is medically reasonable. Certain antibiotics can still be used to treat the infection itself. These include vancomycin and fidaxomicin. Doctors choose the antibiotic based on the severity of the condition and existing risk factors, such as the patient’s age. In severe cases with complications such as intestinal penetration or toxic megacolon, surgery may be necessary.
Important: Treatment is only required in the event of symptoms. Asymptomatic C. difficile infections do not need to be treated.
There are also several other treatment options, such as:
- Infusion with the antibody bezlotoxumab, a drug that binds to the bacterial toxins and renders them harmless. However, these antibodies have not be available in Germany since 1 January 2024 (based on the latest information in 2025).
- Fecal microbiota transplant (stool transplant): The stool from a healthy donor is transferred into the patient’s intestines, for example, in the form of capsules that are taken orally. However, the transfer carries the risk of transmitting other pathogens or triggering undesired processes in the recipient’s body.
Interesting fact: A fecal microbiota transplant is a highly effective treatment method for recurrent C. difficile infections. It is successful in up to 90 percent of patients.
Where can I find more information about Clostridioides difficile?
The infektionsschutz.de website provides more information about C. difficile.
- Bundesinstitut für Arzneimittel und Medizinprodukte (BfArM). Fäkale Mikrobiota-Transplantation (FMT, Stuhltransplantation): Risiko für die Übertragung von multiresistenten Erregern. Aufgerufen am 03.02.2025.
- Czepiel J, Dróżdż M, Pituch H et al. Clostridium difficile infection: review. Eur J Clin Microbiol Infect Dis. 2019;38(7):1211-1221. doi:10.1007/s10096-019-03539-6.
- Deutsche Gesellschaft für Gastroenterologie, Verdauungs- und Stoffwechselkrankheiten (DGVS). S2k-Leitlinie Gastrointestinale Infektionen. AWMF-Registernummer 021-024.11.2023. Aufgerufen am 03.02.2025
- Mada PK, Alam MU. Clostridioides Difficile. [Updated 20241 April 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan.
- Robert Koch-Institut (RKI). Clostridioides (früher Clostridium) difficile. RKI-Ratgeber [Stand 22.01.2025]. Aufgerufen am 03.02.2025.



