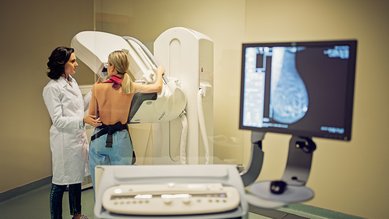
Conditions Lung cancer
ICD codes: C34 What are ICD codes?
57,000 people get lung cancer every year in Germany. It is the second most common type of cancer in men, and the third most common in women. This article provides an overview of the risk factors, diagnostic and therapy options for lung cancer.
At a glance
- Lung cancer is also known as bronchial carcinoma or lung carcinoma.
- In its early stages, lung cancer is only rarely accompanied by specific symptoms.
- Smoking is the main risk factor for the occurrence of lung cancer.
- With lung cancer, medical practitioners differentiate between non-small cell and small cell tumors.
- Depending on the stage, there are various treatment options available for non-small cell tumors.
- The most important part of the treatment for small cell tumors is usually chemotherapy combined with other therapies.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.
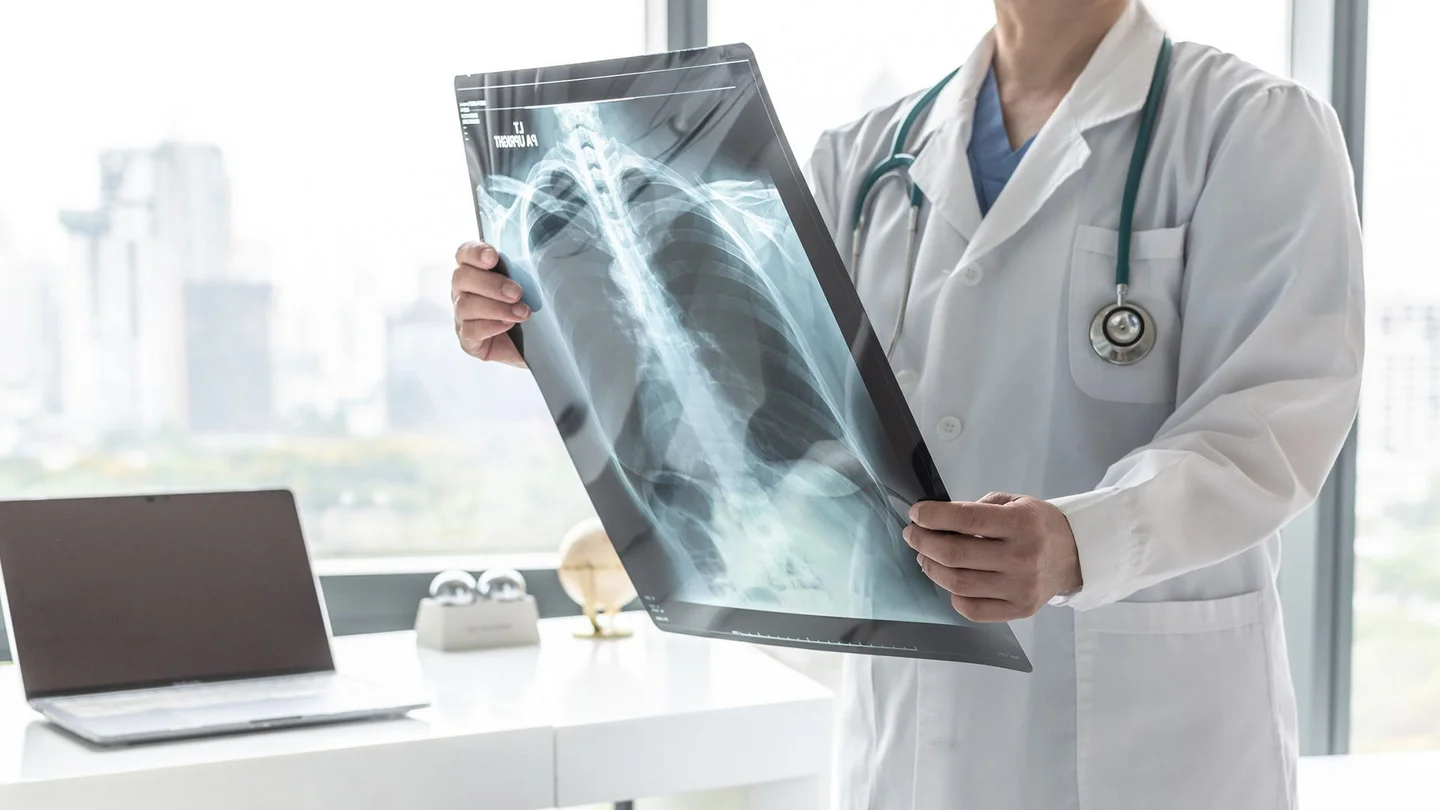
What is lung cancer?
Lung cancer, lung carcinoma and bronchial carcinoma are the terms medical practitioners use to refer to malignant tumors created from lung tissue cells. Bronchial carcinomas are divided into two large groups: non-small cell tumors and small cell tumors.
Which symptoms can occur with lung cancer?
57,000 people get lung cancer every year in Germany. In most patients, the disease is only identified when it is at an advanced stage. There are two main reasons for this: firstly, lung cancer often only reveals itself through symptoms at a late stage. Secondly, these signs of illness are usually non-specific. This means that symptoms such as coughing and abnormal fatigue may also be caused by another illness such as bronchitis (inflammation of the bronchia).
The symptoms of lung cancer can include:
- persistent coughing
- shortness of breath, breathing difficulties through to breathlessness
- phlegm and/or bloody sputum
- pain in the lung and chest area
- general weakness and fatigue
- weight loss
- bone pain
- high temperature
- neurological symptoms such as headaches
Symptoms such as coughing or abnormal fatigue do not only occur with lung cancer, but often also with benign conditions. If these symptoms persist over several weeks and if there are typical risk factors for lung cancer, a visit to the doctor is recommended. General Practitioners can already narrow down what is causing the symptoms and, if necessary, initiate further diagnostic steps with specialists.
Lung cancer: what are the causes and risk factors?
There has long been no doubt that smoking is a very crucial risk factor for the occurrence of lung carcinomas. Amongst lung cancer patients, around 9 out of 10 men and 8 out of 10 women have probably become ill due to years of smoking. The reason: tobacco smoke contains a large amount of carcinogens – these are agents that are classified as causing cancer. The longer and more intensively these carcinogens are breathed in, the more the risk of lung cancer increases. On the other hand, a person can get a bronchial carcinoma without having smoked.
Not only tobacco smoke, but also certain types of radiation and harmful substances in the workplace or everyday life can damage the lungs. Unfortunately, not all of these risk factors can be eliminated – particularly fine dust. However, someone who gives up smoking now can significantly reduce their risk of getting ill within a few years.
Video Stopping smoking – when does the body recover?
How quickly does the body recover when you stop smoking? The video below provides information on this.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What can a person do to prevent lung cancer?
Someone who does not smoke, or who gives up smoking now, has already taken the main measure to prevent lung cancer. Even for non-smokers, if a person is often exposed to tobacco smoke, their risk of getting ill increases.
The risk of lung cancer increases:
- the longer a person smokes.
- the earlier a person starts to smoke.
- the more cigarettes (or cigars or pipe tobacco) a person smokes.
- the more often a person passive-smokes.
Moreover, a healthy lifestyle in general helps prevent cancer – not only lung cancer. Key habits are a balanced diet and sufficient activity: at least 150 minutes light exercise per week.
Is lung cancer screening available in Germany?
With a common type of cancer such as lung cancer, the question naturally arises as to whether screening is a good idea. Up to now, however, there is no suitable, low-risk, reliable test method for everyone.
Specialists and legislators are currently working on the introduction of lung cancer screening for heavy, long-term smokers aged between 50 and 75. This should be performed using low-dose computed tomography. It may still take several more months for all requirements to be fulfilled though.
Heavy smokers are only classed as people who:
- have been smoking for at least 25 years and
- have stopped smoking for less than 10 years within this time and
- have smoked for at least 15 pack years. This is calculated by multiplying the number of packs of cigarettes smoked per day by the number of years for which the person has been smoking.
Would you like to know more about current lung cancer screening options? You can find information about these on the website of the Cancer Information Service of the German Cancer Research Center (in German).
Which tests does a lung cancer diagnosis involve?
If lung cancer is suspected, doctors can use a range of complementary diagnostic methods.
To start with, there is always the basic diagnosis, which consists of the following elements:
- taking the patient’s case history, asking about pre-existing conditions, symptoms and risk factors
- physical examination
- laboratory tests
- x-rays and computed tomography of the chest
- bronchoscopy
General practitioners can take the first steps of a basic diagnosis themselves. Radiologists and lung specialists, for example, are responsible for subsequent steps. Specialist outpatient clinics have trained staff and the medical equipment required.
When a bronchoscopy is done, tissue samples can be taken from the lung. Doctors use these to confirm their diagnosis. If a tumor is found, laboratory staff can use the sample to determine its type. They can also determine whether the tumor cells have particular molecular biological features. Both factors are decisive for the choice of treatment.
If a lung cancer diagnosis is corroborated or confirmed, various imaging methods are used to find out whether and to what extent the cancer has spread through the body.
Do you want to know what other tests are done when the diagnosis of lung cancer is confirmed? You can find out more about testing methods on the website of the Cancer Information Service of the German Cancer Research Center (in German).
How is lung cancer treated?
When selecting the best treatment option for lung cancer, doctors primarily take the following factors into account:
- The stage of the disease (how advanced is the lung cancer?)
- The type of tumor (non-small cell or small cell tumor?)
- The properties of the tumor (does the tumor have special molecular biological properties?)
- The patient’s general health (do any other conditions need to be taken into account when planning the treatment?)
- The patient’s wishes
Non-small cell lung cancer can primarily be operated on in the early stages of the disease – with the aim of fully removing the tumor. Depending on the spread of the tumor, surgery can be combined with other treatment types. If surgery is not an option, it may be possible to use targeted radiotherapy on its own in very early stages. Because small cell tumors form metastases more quickly than non-small cell tumors, an operation is rarely suitable for small-cell lung cancer.
In any case, an operation is only considered if the patient’s condition in general is stable enough. For example, an existing condition such as cardiac insufficiency may constitute a risk that is too great for a surgical intervention. As the average age for getting lung cancer is around 70, many lung cancer patients are affected by other, age-related conditions.
Usually, though, lung cancer is only detected at an advanced stage when it has already spread and there are metastases. At this point, the tumor can no longer be completely removed by surgery or radiotherapy. Drug therapies are the primary choice for patients. These aim to slow the progress of the disease and alleviate the symptoms caused by the tumor or metastases.
Around 85% of patients with lung cancer in Germany have non-small cell lung cancer whilst approximately 15% have small cell lung cancer.
The types of treatment possible in the case of metastatic non-small cell lung cancer are as follows:
- Chemotherapy: this halts the cell growth and inhibits cell division.
- So-called targeted therapies: drugs are used to attack surface features of cancer cells. Healthy cells have little or none of these features.
- Immunotherapy: drugs stimulate certain of the body’s own defense cells to fight the cancer cells themselves.
- Supportive treatments: treatments for alleviating symptoms and improving quality of life. This can include radiotherapy, for example. This aims to use high-energy radiation to damage tumor cells while protecting the surrounding tissue as much as possible.
If small cell lung cancer has produced metastases, patients generally receive a combination of chemotherapy and immunotherapy.
Video What are targeted cancer therapies?
The video below explains when targeted cancer therapies are used. How are these drugs used and how do they work?
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
Would you like to know how therapy options differ for non-small cell and small cell lung cancer? And which treatment options there are if the lung cancer can no longer be cured? Detailed descriptions of the therapy methods can be found on the website of the Cancer Information Service (in German).
After lung cancer therapy: what does rehabilitation involve?
Cancer treatment can be both mentally and physically exhausting. Medical rehabilitation (rehab) after cancer therapy aims to help patients regain their strength. It also aims to help them deal with the consequences of the disease and its treatment in the best possible way. Medical rehab programs are therefore based on patients’ personal medical history and physical limitations.
A medical rehab program after lung cancer therapy may include:
- breathing training to reduce breathlessness after a lung cancer operation
- psychological support
- dietary advice
- physiotherapy and sport
- smoking cessation
What’s next? Lung cancer aftercare and checkups
Lung cancer aftercare is intended to detect any recurrence at an early stage as well as any delayed effects of the treatment. Once treatment has been completed, patients are examined regularly, initially at short intervals, then at longer ones. To that end, they will receive an aftercare plan tailored to their personal situation. However, if patients have any problems they can also visit their doctor more often.
During the follow-up examination, doctors ask about symptoms, examine the body and check the lung function. Computed tomography of the chest or an MRI scan of the brain may be possible.
If the cancer is incurable, regular checkups help to identify adverse symptoms at an early stage. The aim is to maintain the patient’s quality of life for as long as possible.
What is life like with lung cancer?
Many lung cancer patients want to take an active part in order to affect their illness positively. There are a number of ways they can do this. What can help them to cope better with the disease and the consequences of treatment depends on the individual situation:
- Exercise can help overcome tiredness and weakness. It should be adapted to the patient’s physical ability.
- A balanced, healthy diet or nutritional therapy can prevent or treat malnourishment.
- Psycho-oncological counseling can help if worry and anxiety become overwhelming.
If it is no longer possible to cure the cancer and it is becoming more advanced, good medical and nursing care are very important. Adverse symptoms such as coughing and breathlessness can be alleviated. And psychosocial support can help maintain quality of life for as long as possible.
What are suitable points of contact regarding lung cancer?
Doctors with different specializations work closely together to treat lung cancer. Hospitals that are particularly experienced in treating patients with lung cancer can get certification to prove this. The German Cancer Society (Deutsche Krebsgesellschaft) regularly checks their compliance with the relevant professional requirements.
You can find the addresses of the certified centers on the OncoMAP website.
The German Society for Thoracic Surgery (Deutsche Gesellschaft für Thoraxchirurgie – DGT) centers are certified by the independent body Doc-Cert AG.
Do you have any questions about everyday life with lung cancer and other support options? The website of the Cancer Information Service of the German Cancer Research Center provides a wide range of information (in German).
If you have any questions about lung cancer you can also make personal contact with the Cancer Information Service by dialing the freephone number 0800 - 420 30 40 or writing an email to krebsinformationsdienst@dkfz.de.
- Arbeitsgemeinschaft der Wissenschaftlichen Medizinischen Fachgesellschaften e.V. (AWMF), Deutschen Krebsgesellschaft e.V. (DKG) und Deutschen Krebshilfe (DKH). Prävention, Diagnostik, Therapie und Nachsorge des Lungenkarzinoms. S3-Leitlinie. Langversion 2.2. AWMF- Registernummer 020-007OL. 07/2023.
- Zentrum für Krebsregisterdaten des Robert Koch-Instituts (RKI). Lungenkrebs (Bronchialkarzinom). Aufgerufen am 12.08.2024.
In cooperation with the Cancer Information Service of the German Cancer Research Center (Krebsinformationsdienst des Deutschen Krebsforschungszentrums).
As at: