Conditions Inflammation of the inner lining of the heart (endocarditis)
If the lining of the heart becomes inflamed, this is known as endocarditis. It can be caused by pathogens or, more rarely, occur as the result of a pre-existing condition. Severe progression of the condition and complications can often be avoided with early treatment of the inflammation.
At a glance
- Endocarditis is an inflammation of the inner lining of the heart (the endocardium).
- Endocarditis is caused by pathogens in most cases.
- In very rare cases, endocarditis occurs as part of an autoimmune disorder or cancer.
- Most of the symptoms are not specific to this condition. However, endocarditis caused by bacteria is usually accompanied by a high temperature.
- Early treatment is important to avoid life-threatening complications.
- Depending on the cause and the severity of the condition, antibiotics or heart surgery can be used as treatment.
Note: The information in this article cannot and should not replace a medical consultation and must not be used for self-diagnosis or treatment.


What is endocarditis?
Endocarditis is the inflammation of the endocardium. The endocardium is the thin membrane that lines the inside of the heart. It is sometimes referred to as the lining of the heart. The endocardium also forms the valves of the heart. Endocarditis therefore usually also affects the heart valves.
Most cases of endocarditis are caused by a pathogen, such as bacteria or fungi. In rare cases, endocarditis has other causes, such as serious illnesses like cancer or autoimmune disorders.
Severe progression and complications can often be avoided with early diagnosis and treatment.
Video How does the heart function?
This video provides more information about the function and role of the heart.
This and other videos can also be found on YouTube
Watch nowThe privacy policy indicated there applies.
What are the symptoms of endocarditis?
Acute endocarditis caused by a pathogen is often accompanied by a high temperature and chills. However, the inflammation can also develop gradually, causing a slight fever over an extended period.
Other possible symptoms include:
- weakness
- headache
- joint and muscle pain
- loss of appetite, weight loss, nausea and vomiting
The person may also experience symptoms that indicate a problem with the heart. These include:
- chest pain
- shortness of breath
- abnormal sounds when a doctor listens to the heart (murmurs)
- an accelerated heartbeat
- fluid retention
Endocarditis can also cause a stroke and neurological symptoms may occur, including:
- impaired sensitivity
- visual impairment
- hemiplegia (paralysis on one side of the body)
- difficulty speaking
- severe headache
If the inflammation progresses, symptoms include the following distinctive skin changes:
- Osler nodes: painful, bluish-red nodules about the size of a lentil, which occur on the fingers and/or toes
- Janeway lesions: painless, very small red lesions on the hands and feet
- Petechiae (blood spots): red dots the size of a pinhead, which usually occur in one part of the body
Important: Various symptoms may occur when endocarditis is not directly caused by a pathogen. For example, deposits may form on the heart valves, break off and get into the bloodstream, where they can block the blood vessels. This can then cause symptoms of a stroke.
What causes endocarditis?
Endocarditis is almost always caused by bacteria – mainly staphylococcal, streptococcal and enterococcal bacteria. The most common type of bacteria to cause endocarditis is Staphylococcus aureus.
In very rare cases, fungi such as candida and aspergillus can cause inflammation of the endocardium.
Also in very rare cases, endocarditis may occur when blood platelets (thrombocytes), proteins or immune cells may be deposited on the endocardium and the heart valves. This can occur as a result of other serious illnesses, such as cancer or autoimmune disorders. A blood clotting disorder can also make these kinds of deposits more likely to develop, especially if the person has a pre-existing heart valve disorder.
What factors increase the risk of developing endocarditis?
Several factors and pre-existing conditions can increase the risk of developing endocarditis. Risk factors for endocarditis caused by a pathogen include:
- congenital or acquired heart conditions, such as hypertrophic cardiomyopathy
- an artificial heart valve, pacemaker or other artificial material in the heart
- long-term dialysis therapy
- diabetes mellitus
- a weakened immune system, for example, due to medication or HIV/AIDS
- injecting drugs into the veins using unsterile equipment
- poor oral and dental hygiene
People with a blood clotting disorder are particularly vulnerable to endocarditis that is not caused directly by a pathogen. This can also occur as part of other health conditions, such as:
- cancer and autoimmune disorders
- hereditary clotting disorders
- blood poisoning (sepsis)
- severe burns
How common is endocarditis?
Endocarditis is rare. Every year in developed countries, it is estimated that between 3 and 10 people in every 100,000 develop endocarditis due to infection with a pathogen. Men are twice as likely as women to be affected.
What is the outlook for someone with endocarditis?
With acute endocarditis, the patient’s condition deteriorates rapidly. The milder form that begins more gradually (subacute endocarditis) often goes unnoticed for a long time.
If endocarditis is not detected and treated in good time, serious complications and long-term effects can occur – including death of the patient. Almost 25 percent of adults who require hospital treatment for infective endocarditis will die either during treatment or later due to long-term effects.
The mortality rate for endocarditis is lower in children. Between 5 percent and 10 percent of children who are treated in hospital for infective endocarditis will die.
Possible complications and long-term effects include:
How is endocarditis diagnosed?
Endocarditis is not always easily diagnosed as it has a wide range of symptoms, some of which can also occur with other conditions.
During a consultation, a doctor will determine potential risk factors for endocarditis when taking a detailed medical history. These include, for example, an artificial heart valve or a congenital heart disease.
Other possible indicators are recent surgeries or dental treatments, during which pathogens may have entered the body.
Further indications of endocarditis may be discovered during a physical examination. These include unusual heart sounds when the doctor listens to the heart, or changes visible on the skin and nails.
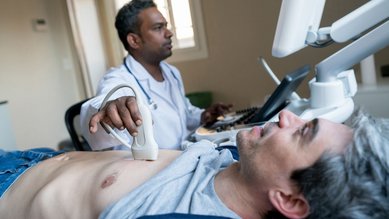
If endocarditis is suspected, an echocardiogram and blood tests will usually be performed.
An echocardiogram or “echo” is an ultrasound scan of the heart. It allows doctors to check the structure and movement of the organ.
Blood tests are performed to check for the presence of pathogens. Blood cultures, in which bacteria and fungi in the blood can grow, are created in a lab.
Further indications of an inflammation can also be found by measuring inflammatory markers and the level of white corpuscles (also known as white blood cells or leukocytes) in the blood.
Certain antibodies and clotting factors in the blood may also help narrow down the cause of endocarditis.
If doctors are still unable to make a definitive diagnosis following these tests, additional imaging techniques may be used, such as X-ray, computed tomography (CT), or magnetic resonance imaging (MRI).
How is endocarditis treated?
Antibiotics are used to treat endocarditis caused by bacteria.
Antimycotics (anti-fungals), i.e., drugs that specifically target fungi, are used if the cause is a fungal infection. Antibiotics or antimycotics are usually administered over several weeks via an infusion into the bloodstream.
In many cases, treatment with medication alone is not sufficient to treat endocarditis – for example, if the heart valves are already seriously damaged by the inflammation and are no longer fully functional.
Surgery is then often required to prevent heart failure and other complications. The operation involves the surgeon removing the inflamed tissue. In most cases, the affected heart valve is replaced with an artificial heart valve.
In people with endocarditis caused by another illness, the pre-existing condition is treated first. The treatment may also aim to prevent the formation of blood clots. In most cases, the patient will need to take anticoagulants (anti-clotting medication) such as heparin on a long-term basis. Under certain circumstances, such as acute heart failure, surgery may also be required.
What aftercare is required for endocarditis?
Following treatment, doctors will check the patient’s heart using an ultrasound scan (echocardiogram). This scan determines the condition and functioning of the heart.
Blood tests are performed again to check certain blood values and levels of white corpuscles in the blood. This indicates whether the inflammation has reduced. Regular check-ups are an important element of aftercare for endocarditis.
People who have survived endocarditis or who are at an increased risk of developing endocarditis, e.g., following surgical procedures on the heart valves, are advised to observe good skin and dental hygiene. They should also attend preventive dental check-ups on a regular basis. In advance of certain surgical procedures and dental treatments, it is recommended – in consultation with a doctor – to take an antibiotic on a preventive basis to avoid developing endocarditis again. If anyone at an increased risk of developing endocarditis notice any sign of infection (e.g., high temperature or lethargy), they should always consult a doctor.
Important: As a general rule, antibiotics should not be taken on a preventive basis, as taking these drugs without good reason can promote the development of antibiotic resistance.
- Delgado V, Marsan NA, de Waha S, et al. 2023. ESC Guidelines for the management of endocarditis: Developed by the task force on the management of endocarditis of the European Society of Cardiology (ESC). Endorsed by the European Association for Cardio-Thoracic Surgery (EACTS) and the European Association of Nuclear Medicine (EANM), European Heart Journal, Volume 44, Issue 39, 14 October 2023, Pages 3948–4042
- Deutsche Gesellschaft für Pädiatrische Kardiologie und angeborene Herzfehler e.V. Infektiöse Endokarditis und Endokarditisprophylaxe. S2k Leitlinie. 09/2022.
- Deutsche Herzstiftung. Ursachen einer Endokarditis. Aufgerufen am 18.03.2025.
- DynaMed (Internet), Ipswich (MA). Infective Endocarditis in Adults. EBSCO Information Services. Aufgerufen am 12.03.2025.
- DynaMed (Internet), Ipswich (MA). Nonbacterial Thrombotic Endocarditis (NBTE). EBSCO Information Services. Aufgerufen am 12.03.2025.
- Gupta A, Mendez MD. Endocarditis. [Updated 2023 July 17]. In: StatPearls (Internet). Treasure Island (FL): Statpearls Publishing. 2025 Jan-. Aufgerufen am 12.03.2025.
- Yallowitz AW, Decker LC. Infectious Endocarditis [Updated 2023 April 24]. In: StatPearls (Internet). Treasure Island (FL): Statpearls Publishing. 2025 Jan-. Aufgerufen am 12.03.2025.
Reviewed by the German Cardiac Society (Deutsche Gesellschaft für Kardiologie – Herz- und Kreislaufforschung e.V., DGK).
As at: